What is the definition of Intramural Hematoma
an aortic dissection without an intimal flap.
what is the radiographic definition of an intramural hematoma?
regional thickening of the aortic wall, >7mm in circular or crescent shape without intimal flap and without enhancement s/p contrast injection
what is the underlying pathophysiology of intramural hematoma (2)
1) spontaneous rupture of vasa vasorum –> aortic wall disintegration –> dissection +/- tear **OR** 2) intimal fracture of atherosclerotic plaque –> allows blood to propogate in the aortic media
what is the initial management of intramural hematoma
aggressive BP control in the ICU
what anatomic involvement is associated with highest involvement with intramural hematoma
ascending aortic arch and/or coexisting aneurysm –> warrant aggressive approach
how can intramural hematoma exist on a spectrum of disease with aortic dissections?
intramural hematoma and intact intima (like an acute aortic dissection with thrombosed lumen) –> full blown aortic dissection
what is the early mortality of acute aortic dissection per hour?
1-2% per hour; therefore misdiagnosis causing a delay in treatment –> catastrophe
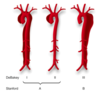
define a DeBakey Type I dissection
involving ascending, arch, and descending aorta
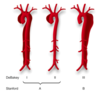
define a DeBakey Type II dissection
involves only ascending aorta
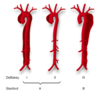
Define a DeBakey Type III dissection
originates and propagates distal to the left SCA

Distinguish a DeBakey Type IIIa and IIIb dissections
Type IIIa: descending thoracic aorta; Type IIIb: extends beyond diaphragm
Define a Stanford Type A dissection
positive ascending aortic involvement

Define a Stanford Type B disection
no ascending aortic involvement (therefore arch and/or descending involvement)
What is the relative duration of acute, subacute, and chronic dissections?
<2 weeks: acute; 2-6 weeks subacute; > 6 weeks, chronic
What percent of all dissections are acute Stanford A and how are they managed?
60%, surgical emergency, needs immediate OR
what is the difference between “complicated” and “uncomplicated” Stanford Type B dissections in presentation and management? What are their relative frequencies?
Complicated (20%) rupture/impending rupture; malperfusion; refractory pain/HTN –> needs open or endovascular repair. Uncomplicated (80%) manage with aggressive medical therapy
What percent of patients with clinical picture of acute aortic dissection actually have intramural hematoma?
10-20% have IMH –> incorrectly referred to as dissection with thrombosed false lumen. Have clinical picture but no blood flow to false lumen or identifiable lesions
name three underlying causes of possible intramural hematoma
microscopic intimal tear; penetrating aortic ulcer; vaso vasorum hemorrhage
what disease process is intramural hematoma managed like?
managed like acute aortic dissection
what is the classic presentation of acute aortic dissection? (5 S/Sx)
10/10 ripping chest or back pain; asymmetric pulses; differing BP in extremities +/- S/Sx of malperfusion (pulseless extremities, new neuro deficit); new diastolic murmur 2/2 retrograde dissection into coronary arteries / aortic valve
What underlying process should you suspect in an aortic dissection patient with hypotension and shock?
tamponade; cardiac dysfunction; ongoing hemorrhage
what is the gold standard study for acute aortic dissection and its associated sens/spec? what are its limitations?
CTA: sens/specificity is 90-100%. Scans limited to the thoracic aorta can confirm diagnosis, scanning the entire aorta helps with surgical planning and assessnig for subclinical disease
What are the three diagnostic benefits of TEE?
rapid assessment for tamponade; valve dysfunction; and cardiac wall motion alone
what are the BP meds of choice and BP goals for acute aortic dissection patients
- hemodynamic monitoring with arterial line; - start beta blockade with goal SBP 100-110 and goal HR 60-70; add vasodilators prn (nitroprusside / hydralazine)
why shouldn’t you initiate BP control for aortic dissection patients with vasodilators?
increases left ventricular contractility (dp/dT) = increased aortic shear = increased rupture risk
What subtype of aortic dissections should not be managed with beta blockers and why?
Acute Stanford Type A with either a diastolic murmur or TEE evidence of significant aortic regurgitation should not be managed with beta blockers because they increase the risk of worsening CHF (reduced HR leads to increased diastole leads to increased congestion?)
why should patients with acute Type A dissections undergo central repair in the setting of cerebral / renal / visceral malperfusion?
central aortic reconstruction will correct malperfusion
What is the goal of surgery for acute Type A dissection?
prevents imminent death from : aortic rupture –> exsanguination / tamponade; acute aortic insufficiency; malperfusion of coronary / cerebral / systemic ciruclation. Accomplished with tube interposition graft and reestablishing true lumen blood flow
What should be monitored during anesthesia for ascending aortic dissection repair?
arterial line for invasive BP; CVP monitoring; TEE; temperature of bladder/venous/arterial (ensures uniform cooling); EEG; cerebral oximetry
is CPB required for ascending aortic replacement?
Yes
Name three possible sites for arterial cannulation for CPB for ascending aortic dissection repair and associated pros/cons
1) CFA - easily accessible and familiar. 2) right axillary/SCA with 8-10mm Dacron graft anastomosed end-to-side to axillary artery –> allows for antegrade systemic perfusion –> selective antegrade cerebral perfusion. 3) direct central ascending aortic cannulation with TEE (TEE to guide to true lumen), difficult but lifesaving in unstable patients

What is the incision for ascending aortic dissection repair?
median sternotomy to expose heart and ascending aorta
what is cannulated for CPB venous drainage for ascending aortic repair?
right atrium can be easily cannulated
what is the next step if the patient on CPB develops aortic insufficiency or coronary malperfusion?
vent the left ventricle on bypass; protect myocardium with direct antegrade coronary ostial / retrogradecoronary sinus cardioplegia strategies
What is the optimal temperature for profound hypothermia prior to cardioplegia?
18 degrees celsius in the nasopharynx before turning off circulation, be sure hypothermia occurs uniformly (perfusion and cooling)
What are the steps to reconstruct the ascending aorta with acute aortic dissection
patient in Trendelenberg; resect entire ascending aorta - sinotubular junction –> innominate artery; evaluate dissection flap –> make sure that brachiocephalic branches arise from true lumen; reconstruct all layers of the proximal aortic arch –> obliterate false lumen
Describe two techniques to reconstruct the proximal aortic arch with ascending aortic dissection
1) reconstructive aortic wall between two Teflon felt strips; anastomose Dacron graft to aorto-felt “sandwich”; 2) insert Teflon into false lumen –> obliterates false lumen –> sew Dacron graft to reconstituted aorta buttressed with strip of Dacron around adventitia (creates “neo-media”)

Why is it advised to avoid glue during ascending aortic dissection repair?
although they allow for easier tissue handling, can increase risk of pseudoaneurysm
what step should be completed after the distal anastomosis of ascending aortic dissection repair?
-“deair” the aortic arch; -clamp proximal graft; -CPB resumed through Dacron graft –> promote true lumen flow
When should aortic arch replacement be considered for acute aortic dissections? (3 scenarios)
- complex intimal disruptions in the arch; - arch aneurysm > 5cm; - connective tissue syndromes (Marfan’s, Loeys-Dietz, Ehler-Danlos)
What step should be performed with arch replacements that is a/w improved neuro outcomes?
antegrade cerebral perfusion
Describe two methods for constructing the proximal aortic anastomosis in ascending aortic dissection repair
b/c aortic root is usually uninvolved in the dissection, can do “sandwich” technique (reconstitute aortic wall between two teflon felt strips and anastomose dacron graft to aorto-felt sandwich) or “neomedia” technique if dissection extends to the root (insert Teflon into false lumen –> obliterates false lumen, sew Dacron graft to reconstituted aorta buttressed with strip of Dacron aroudn adventitia (“neomedia”)
What is the most common cardiac complication a/w acute Type A aortic dissection?
aortic regurgitation
Describe three mechanisms of Type A dissection –> aortic regurgitation
1) acute dilatation of sinotubular junction 2/2 expanding false lumen = incomplete coaptation of valve cusps; 2) dissect through aortic root –> disrupts commisurial posts –> prolapse of valve cusps; 3) aortic flap prolapses through valve during diastole, thereby preventing appropriate valve function
Name four scenarios where you should consider composite aortic root replacement with coronary button reimplantation
aortic root aneurysms > 5 cm; complex aortic valve pathology; dissection approaching coronary ostia; connective tissue syndromes
What is the overall mortality of acute type A dissections? How is this affected by preop instability? Name 8 causes of preop instability.
Approx 25% mortality, if unstable preop = 31% mortality. Tamponade, shock, CHF, stroke, coma, MI, ARF, and mesenteric ischemia are all causes of preop instability.
Name 7 early postop complications after treatment of acute type A aortic dissection requiring ICU care
transient neuro dysfunction; CVA/TIA; acute lung injury; refractory hypotension; new malperfusion syndromes; renal insufficiency; multisystem organ failure
What is the preferred management of Acute Type B dissection?
Medical management with BP control
What is the mortality of uncomplicated Type B dissection?
< 10%
What percent of acute type B aortic dissections are “complicated”? Name 5 S/Sx of “complicated” Type B.
~25% complicated. S/Sx: refractory HTN (to three different drug classes); malperfusion syndromes; increasing periaortic hematoma; bloody pleural effusions; shock
What is the preferred surgical management of complicated Type B dissection? What is its associated 5-year survival and how does this compare to medical management?
TEVAR has a 5-year survival of 60-80%, preferred for complicated patients. Has not yet been compared to medical management in uncomplicated patients.
