Describe glucose homeostasis in terms of its regulators
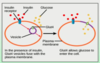
Glucose is in homeostasis at a concentration of 90mg/100ml and when that rises, beta crlls of the pancreas release insulin and when it lowers, alpha cells release glucagon to cause glycogenolysis and glucose to be released from the liver
What is the difference between the secretions of the pancreas and endocrine secretions?
The pancreas is composed of ducts and therefore releases its hormones in an exocrine fashion directly into the GI BUT 1-2% of the pancreas are occupied by the Islets of Langerhan which perform the endocrine function of the pancreas

What are the main cells of the pancreatic islets?
B cells which secrete insulin,
alpha cells which secrete glucagon,
somatostatin delta cells which are inhibitory of both
PP-cells secrete pancreatic polypeptide (few in number) which inhibit intestinal motility

How are the cells of the pancreatic islets arranged?
B cells (pink) are centrally located while a-cells (brown) and D-cells (blue) are at the periphery of B-cell clusters

Describe the blood supply of the pancreas
The inlet is via the splenic artery, superior mesenteric artery, and the inferior pancreaticoduodenal artery and the outlet is via the portal vein.
Keep in mind that although the islets comprise only 1-2% of the pancreatic tissue, it receives 10-15% of blood flow
What is the significance of the portal vein being the outlet of the pancreas?
The pancreatic hormones will reach the liver first where the bulk of their actions occur
How is insulin made?
Insulin is a peptide hormone so transcription produces, Preproinsulin which is transformed into proinsulin which has a-chains on the C-terminal and beta-chains on the N-terminal linked by C peptides/disulfide bonds. Proinsulin is then acted upon by endopeptidases which cleaves C peptides to produce insulin and C peptides where are then packaged into secretory vesicles.
NOTE: There are two types of secretory granules, ready releasable pool (5%) and reserve pool (95%)
How is insulin released?
It is a biphasic phenomenom that is characterized by a burst followed by a sustained released of insulin

How does insulin secretion patterns differ in fasting vs post-meal states?
In post-meal states, insulin is relased more frequently and in larger amounts
How does insulin circulate? Half-life? Degradation? Whta about C peptide?
Circulates in free form (peptide hormone) and have a half life of 3-8 minutes until they are degraded by the liver (50% in first pass) and secondarily by target tissues via endocytosis of the receptor-boudn hormone followed by proteolytic degradation
NOTE: C peptide has a half-life of 35 min and is slowly degraded by the liver?
Since insulin has a short half life and is rapidly cleared from the circulation, how can one determine the secretory capacity of the endocrine pancreas?
measure C peptide
How is insulin regulated?
B cells integrate many signals to stimulate insulin release but the main inducer is glucose entering the cell via low-conducting GLUT-2 channels. Glucose is manipulated and via the Krebs cycle ATP is generated. A rise in the ratio of ATP:ADP leads to deactivation/closure of membrane ATP-sensitive K+ channels to help stop efflux of K+ causing membrane depolarization. Depolarization leads to opening of voltage-dependent Ca2+ channels which causes Ca2+ influx into the cell which stimulates insulin preprohormone production and release.
NOTE: The rise of Ca works in complex with many other signals
What are the effects of insulin?
Immediately it promotes cellular uptake of K+ and AAs and begins lowering glucose uptake. Then it manipulates metabolic enzyme activity, enzyme synthesis, and finally, affects growth and cell differentiation
NOTE: Insulin DOES NOT cross the placenta unlike glucose
What are the main effects of insulin?
It lowers BG levels by transporting it into adipose and muscle and increasing glycogen synthesis
It lowers plasma fatty acid levels and increases fat deposition and protein production
promotes K+ and AA cellular uptake
promotes Na+ retention in the kidneys
GLUT transporters are responsible for cellular glucose uptake. Where is GLUT1 expressed and what is its function?
Ubiquitous (primarily in RBCs and brain vascular endothelial cells and some in skeletal muscle and fat, placenta and cornea) and functions to increase glucose uptake by skeletal muscle and fat under basal conditions
NOTE: RBCs need GLUT1 because they dont have mitochondria
NOTE2: The brain uses glucose for energy under normal states and ketone bodies in times of starvation
Where is GLUT2 expressed and what is its function?
Low-affinity transporter common in B cells, liver, intestine, and kidney and acts as a glucose sensor system (limits glucose uptake by B-cells and hepatocytes to only when glucose levels are high)
Where is GLUT3 expressed and what is its function?
Primarily in neurons (and placenta) and are crucial in allowing glucose to cross the BBB and enter neurons
Where is GLUT4 expressed and what is its function?
Primarily in striated muscle and adipose and is sequestered in specialized storage vesicles that remain within the cell’s interior under basal conditions
Where is GLUT5 expressed and what is its function?
Spermatozoa and small intestine and is predominantly a fructose transporter
How does GLUT4 work? What are the insulin-independent glucose uptake organs?
Sequestered inside the cell in vesicles. When insulin increases and binds to its membrane receptor, GLUT4 is transported to the membrane where it starts to transport glucose (aka insulin responsive transporter)
NOTE: The insulin-independent glucose uptake organs are BRICK-L (brain, RBCs, intestine, cornea, kidneys, and liver)
What is the role of glucagon?
Counteracts insulin by promoting glucose mobilization in the liver through glycogenolysis and gluconeogenesis (as well as lipolysis and ketone production)
How is glucagon made?
Proglucagon is manipulated to produce glucagon in the pancreas and GLPs (aka incretins) in the intestine. These are very sensitive to glucose levels
How is glucagon production inhibited?
Insulin acts on the alpha cells to decrease glucagon secretion when BG is high. Somatostatin can also inhibit glucagon
How can glucagon production be stimulated?
1) hypoglycemia
2) high amino acid levels following a meal
3) Epinephrine via B2 adrenergic mechanisms
4) Vagal stimulation
How does glucagon work?
via a Gs protein (cAMP process)
Why would a patient with insulin deficiency present with fruity smelling breath?
The icnreased amount of glucagon produces more acetone which is deposited into the fat of the lungs and breathed out
Describe somatostatin
a 14 AA peptide hormone produced by Delta cells of the pancreas in response to high-fat, high-carb, and protein-rich diet and has a generalized inhibitory effect on insulin, glucagon, TSH, and GH
What inhibits somatostatin?
insulin
Describe Pancreatic polypeptide
A 36 AA peptide hormone produced by F cells located in the periphery of the pancreas released after a meal, exercise and vagal stimulation
What is the role of pancreatic polypeptide?
Inhibits pancreatic exocrine secretion, gallbladder contraction, modulation of gastric acid secretion, and GI motility
