What is the pattern of events of immediate innate immunity?
- Lasts up to 4 hours
1. Infection.
2. Recognition by performed, nonspecific effectors.
3. Removal of infectious agent.
Give a sequence of events of innate early induced response.
- Response time: 4-96 hours.
1. Infection.
2. Recognition of microbial-associated molecular patterns.
3. Inflammation and recruitment and activation of effector cells.
4. Removal of infectious agent.
Give an overview of the sequence of events of the adaptive immune response.
Lasts over 96 hours.
- Infection.
- Transport of antigen to lymphoid organs.
- Recognition by naieve B and T cells.
- Clonal expansion and differentiation to effector cells.
- Removal of infectious agent.
What are the non-immunological barriers to infection?
Mechanical: epithelial cells, longitudinal flow of air.
Chemical: fatty acids, low pH, enzymes (pepsin), salivary enzymes (lysozyme).
Microbiological: normal flora
What is the complement system?
- It is an important set of preformed molecules found in blood plasma and interstitial fluids.
- They have the capacity to recognise & kill foreign microbes, and to recruit and activate the immune system to combat those microbes.
In the complement system, what is the alternative pathway?
- Driven solely by the interaction of complement with microorganisms.

In the complement system, what is the lectin pathway?
Slightly more restricted, but also driven by interaction with pathogens directly.
In the complement system, what is the classical pathway?
- Requires antibodies.
- Antibodies are the products of the acquired immune response (bit of an evolutionary advantage).
- C3a has a function to do with inflammation & recruitment of cells.
- C3b has function to do with making cells interact better with bacteria.
C5a also helps with inflammation and recruitment.
C5b starts a cascade to c6, 7, 8, 9 which generates a membrane attack complex (MAC)

What are the functional protein classes in the complement system?

Bacteria gets into finger. What does complement system do?
- Bacteria can be reccognised by c3 - will activate the alternative pathway.
- It will generate c3 fragment products - c3a and c3b.
- c3b still stick to the surface of the bacterium and help it to be recognised by phagocytes that are in the tissue at the time.
- Then the other fragment, C5a comes in, and they have the ability to recruit and drive inflammation - they don’t do this directly, but do it through the activation of mast cells.
- Mast cells have a lot of vasoactive products, such as histamine.
- So what happens is C3a and C5a hit the mast cell, degranulation of the mast cell causing histamine release, then the histamine works on the blood vessel vasculature to make them more permeable.
- And because they are more permeable, fluid can get in across the barrier (interstitial space) but also allows cells (WBC) to get across the barrier.
- Similarly, how do these cells realise that they can now come out of the vasculature? The complement proteins also provide a ‘follow me’ signal - this process is called exudation.

How is the membrane attack complex created?

There are many different receptors that different things bind to. Give such examples.
1. LPS - gram negative bacteria.
2. Fungal infection - recognised by glucan receptor.
- Receptor for complement C3b
4. TLR4 - gram negative bacteria.
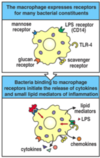
What do gram +ve bacteria express on their cell wall which can be detected by host cells?

Pattern recognition receptors (PRR) identify the class of pathogen by identifying the pathogen associated molecular patterns (PAMPs). Give some examples.

Outline the steps of phagocytosis.

Give an example of a potent antimicrobial mechanism during phagocytosis.
- Activation of NADPH oxidase occurs during the ‘respiratory burst’ and releases toxic oxygen radicals (superoxide and hydrogen peroxide).
- Oxygen radicals may directly damage microbial membrane and/or activate microbial enzymes found in granules.
What roles does the phagosome play in immunity?

What are the microbicidal mechanisms of phagocytes?

What percentage of leukocytes are formed by monocytes?
2-10%

How do neutrophils catch bacteria?
They catch bacteria using ‘neutrophil extracellular traps’ or NETs.
- NETs contain chromatin and granule proteins (including enzymes to degrade pathogen virulence factors).
Can blood monocytes give rise to tissue macrophages?
Yes, but most tissue macrophages arise from non-hematopoietic precursors.
What are Kupffer cells?
They are stellate macrophages located in the liver.
- They constitute 80-90% of tissue macrophages in the body.
- Exposed to gut microbacteria, endotoxins etc.
What is so special about dendritic cells?
- They are specialised for interacting with lymphocytes.
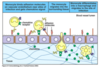
Cytokines are produced by macrophages. What do they do?
- They cause dilation of local small blood vessels.
- Leukocytes move to periphery of blood vessel as a result of increased expression of adhesion molecules.
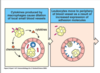
How does a monocyte differentiate into a macrophage and migrate to the site of infection?
What are cytokines and chemokines?
- The hormones of the immune system.
- Allow communication between a variety of immune and non-immune cells.
- Approximately 30 identified, with specific but overlapping functions.
- Mostly referred to as ‘interleukens’
- A further heterogeneous and complex family of small molecular weight chemotactic cytokines are known as chemokines (approximately 30 of them also).
How are cytokines and chemokines regulated?
- Mostly short acting ‘hormones’ but can have systemic effects e.g. shock
- May be released in a polar fashion at ‘synapses’
- Recognised on target cells by specific receptors (with some redundancy).
- Receptor expression is highly regulated to control the targets and duration of response.
- Subsets of cytokines/chemokines may be selectively co-regulated and help define cell subsets e.g. Th1 and Th2 CD4+ lymphocytes.
Link up the modules of innate immunity with their respective cytokines.

What are the opposing effects of cytokines on macrophage function?

What is the function of natural killer cells?

Why is innate cytokine production essential for host survival after infection with gram- bacteria?

How do steroids affect the immune system?

