women visit Flashcards
age 13-18 (screening)
ACOG recommends initial Ob/Gyn visit at what age?
what 4 things to look for in hx?
what are the 3 periodic labs to check if sexually active?
13-15
menstrual, family medical hx, drugs (alcohol and tobacco), sexual abuse
labs periodic of chlamydia, gonorrhea (urine screening) and HIV
-sexually active
13-18 (evaluation and counseling)
immunization:
evaluation and counseling: sexually transmitted disease prevention-barrier, sexual abuse, tobacco, alcohol
immunization
Tdap (diphtheria and reduced tetanus toxoids and acellular pertussis
Hep B (1 series if not immunized before)
HPV (9-45)
-protect against anogenital cancer (cervical, vaginal, penile, anal) oropharygneal cancer
–cervarix (16 & 18)
–Gardasil (11, 6, 16, 18)
–Gardasil 9
influenza vaccine annually
MMR if needed
varcella vaccine if needed
19-39
hx
PE
lab
screening
Hx:
FM hx, tobacco, alcohol, sexual practices: vaginal, anal, oral sex
PE: breast (q 1-3 years beginning at age 20), pelvic exam: 19-20 if needed or 21 or older
labs
cervical cytology
age 21-29 (q 3 years with cytology)
age 30 or older (q 3 years w/ cytology) Co test with cytology and HPV testing (q 5 years)
chlamydia and gonorrhea testing
if 25 or younger if sexually acitve, 26 or older at high risk should be screen rountinely
HIV
19-39
evaulation and counseling
sexuality and reproductive planning
psychosocial evaulation
health risk assessment
drugs
immunization
sexuality and reproductive planning: discussion of reproductive health plan, preconception and genetic counseling, STD prevention
psychosocial: intimate partner violence and acquaintance rape prevention
health risk assessment: breast self-awareness
drugs: tobacco and alcohol
immunization
Tdap: booster q 10 years
HPV (9-45)
influenza vaccine annually
MMR and varcella vaccine is needed
40-64 years
screening
hx
PE
labs
screening
hx
FMhx, tobacco, alcohol, pevic prolapse, menopausal sx
PE: breast (yearly clinical breast exam)
Lab:
cervical cytology
-screen q 3 years w/ cyptology alone or co test with cyptology and HPV testing q 5 years
colorectal cancer screening ( beginning at 50 years)
- ACG recommend starting at 45 y/o
- colonoscopy q 10 years
others
- fecal occult blood testing (requires 2-3 samples of stool at home and return for analysis) yearly
- flex sigmoidoscopy q 5 years
- double contrast barium enema q 5 years
- CT colonography (virtual colonoscopy) q 5 years
HIV
lipid profile assessment q 5 years beginning at 45 yo
mammography yearly after 40 yo
diabetes testing q 3 years 45 yo
age 40-64
Evaulation and counseling
sexuality and reproductive planning
psyhosocial evaluation
drugs
health risk
immunization
sexuality and reproductive planning
genetic counseling
STD prevention
psychosocial evaluation: initmate partner violence, advance directives
drugs: tobacco, alcohol
health risk assessment: breast self-awareness
immunization
Tdap
HPV
MMR
varicella vaccine
varicella zoster vaccintion in 60 and older
65 and older
screening
hx
PE
labs
screening
Hx: FMHx, tobaaco, alochol, pelvic prolapse, menopausal symptoms
PE: breasts (yearly clinical breast exam)
Lab
cervical cytology: can discontinue in women with no history of CIN 2 or higher (3 consective negative prior cyptology results or 2 consectuve negative co-test within the previous 10 years
-if has a hx of CIN2 or CIN 3- need to continue pap x 20 years after even if it extends > 65 yo
colorectal cancer screening
bone mineral density screening - in absence of new risk factors do NOT screen more frequently then q 2 years
lipid profile and mammography
65 years and older
evaluation and counseling
sexuality and reproductive planning
psychosocial evaluation
healthy risk assessment
immunization
evaluation and counsel is the same as all the other ages
immunization
add in pneumococcal vaccine: once at 65 yo or older
describe a breast exam in upright position and supine position

patient in an upright sitting position- palpate all quadrants of the breasy systematically, pushing gently, but firmly towards the chest
inspect both breast and compare size, symmetry, contour, venous pattern, skin and or nipple abnormalities
patient in supine position- have the patient raise their arms behind the head which allow breast tissue to spread more evenly over the chest wall and can allow deeper palpation
if mass if felt, document its location, size, shape, mobility and retraction
palpate the nipple: compress the nipple between thumb and index finer and inspect for discharge
palpate the tail of spence
methods of palpation: back and forth, concentric circles, wedge technique
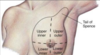
what are the signs of breast cancer?
skin dimpling, flattening of nipple

