Spot diagnosis:
Picture and info from Dermnet

Psoriasis.
Psoriasis is a group of common, chronic, scaly rashes that affect people of all ages (about 2% of the population). There is a genetic predisposition to psoriasis i.e. it tends to run in families. Psoriasis is also influenced by many environmental factors. It is not contagious and is not due to an allergy.
The most common ages for psoriasis to first appear are in the late teens and in the 50s. It affects men and women equally, although in children, girls are more commonly affected than boys.
Psoriasis is often so mild it is barely noticed by the affected person, but it can occasionally so severe the patient must be admitted to hospital for treatment. It may or may not be itchy.
About 5% of those with psoriasis will also develop joint pains (psoriatic arthritis), which may involve one or more joints. This can be very debilitating. The arthritis runs an independent course to the skin disease.
Spot diagnosis:
Dermnet

Lipodermatoscleroris
Lipodermatosclerosis refers to a skin change of the lower legs that often occurs in patients who have venous insufficiency. It is a type of panniculitis(inflammation of subcutaneous fat). Two-thirds of affected patients are obese. Affected legs typically have the following characteristics:
- Skin induration (hardening)
- Increased pigmentation
- Swelling
- Redness
- “Inverted champagne bottle” or “bowling pin” appearance
Lipodermatosclerosis has also been called hypodermitis sclerodermiformis and sclerosing panniculitis.
Spot diagnosis
Dermnet

Venous eczema
Venous eczema is a common form of eczema / dermatitis that affects one or both lower legs in association with venous insufficiency. It is also called gravitational dermatitis.
Venous eczema appears to be due to fluid collecting in the tissues and activation of the innate immune response.
Normally during walking the leg muscles pump blood upwards and valves in the veins prevent pooling. A clot in the deep leg veins (deep venous thrombosis or DVT) or varicose veins may damage the valves. As a result back pressure develops and fluid collects in the tissues. An inflammatory reaction occurs.
Venous eczema is most often seen in middle-aged and elderly patients—it is reported to affect 20% of those over 70 years. It is associated with:
History of deep venous thrombosis in affected limb
History of cellulitis in affected limb
Chronic swelling of lower leg, aggravated by hot weather and prolonged standing
Varicose veins
Venous leg ulcers
Spot diagnosis (Dermnet)

Pityriasis rosea is a viral rash which lasts about 6–12 weeks. It is characterised by a herald patch followed by similar, smaller oval red patches that are located mainly on the chest and back.
Pityriasis rosea most often affects teenagers and young adults. However, it can affect males and females of any age.
Systemic symptoms
Many people with pityriasis rosea have no other symptoms, but the rash sometimes follows a few days after a upper respiratory viral infection (cough, cold, sore throat or similar).
The herald patch
The herald patch is a single plaque that appears 1–20 days before the generalised rash of pityriasis rosea. It is an oval pink or red plaque 2–5 cm in diameter, with a scale trailing just inside the edge of the lesion like a collaret.
Secondary rash
A few days after the appearance of the herald patch, more scaly patches (flat lesions) or plaques (thickened lesions) appear on the chest and back. A few plaques may also appear on the thighs, upper arms and neck but are uncommon on the face or scalp. These secondary lesions of pityriasis rosea tend to be smaller than the herald patch. They are also oval in shape with a dry surface. Like the herald patch, they may have an inner collaret of scaling. Some plaques may be annular (ring-shaped).
Pityriasis rosea plaques usually follow the relaxed skin tension or cleavage lines (Langers lines) on both sides of the upper trunk. The rash has been described as looking like a fir tree. It does not involve the face, scalp, palms or soles.
Pityriasis rosea may be very itchy, but in most cases it doesn’t itch at all.
Spot diagnosis (dermnet)

Pityriasis versicolor
Pityriasis versicolor is a common yeast infection of the skin, in which flaky discoloured patches appear on the chest and back.
The term pityriasis is used to describe skin conditions in which the scale appears similar to bran. The multiple colours of pityriasis versicolor give rise to the second part of the name, versicolor. Pityriasis versicolor is sometimes called tinea versicolor, although the term tinea should strictly be used fordermatophyte fungus infection.
Spot diagnosis (Dermnet)

Lichen planus
Lichen planus is an uncommon skin complaint. It is thought to be due to an abnormal immune reaction provoked by a viral infection (such as hepatitis C) or a drug. Inflammatory cells seem to mistake the skin cells as foreign and attack them.
Lichen planus may cause a small number of skin lesions or less often affect a wide area of the skin and mucous membranes. In 85% of cases it clears from skin surfaces within 18 months but it may persist longer especially when affecting the mouth or genitals.
Classical lichen planus is characterised by shiny, flat-topped, firm papules (bumps) varying from pin point size (‘guttate’) to larger than a centimetre. They are a purple colour and often are crossed by fine white lines (called ‘Wickham’s striae’). They may be close together or widespread, or grouped in lines (linear lichen planus) or rings (annular lichen planus). Linear lichen planus can be the result of scratching or injuring the skin. Although sometimes there are no symptoms, it is often very itchy.
Lichen planus may affect any area, but is most often seen on the front of the wrists, lower back, and ankles. On the palms and soles the papules are firm and yellow. Very thick scaly patches are particularly itchy and are most likely to arise around the ankles (hypertrophic lichen planus).
New lesions may appear while others are clearing. As the lichen planus papules clear they are often replaced by areas of greyish-brown discolouration, especially in darker skinned people. This is called postinflammatory hyperpigmentation and can persist for months.
Spot diagnosis (Dermnet)

Dermatomyositis
Dermatomyositis is a rare acquired muscle disease that is accompanied by a skin rash. It is just one of a group of muscle diseases called inflammatory myopathies.
Dermatomyositis may affect people of any race, age or sex, although it is twice as common in women than in men. The onset of the disease is most common in those aged 50 to 70.
In many patients the first sign of dermatomyositis is the presence of a symptomless, itchy or burning rash.
Reddish or bluish-purple patches, mostly on sun exposed areas
Purple eyelids, which are described as heliotrope, as they resemble the heliotrope flower, e.g., Heliotropium peruvianum, which has small purple petals.
Purple spots on bony prominences, especially the knuckles, which are known as Gottron’s papules
Ragged cuticles and prominent blood vessels on nail folds
The rash may also affect cheeks, nose, shoulders, upper chest and elbows
A scaly scalp and thinned out hair may occur
Less commonly there is poikiloderma i.e. the skin is atrophic (pale, thin skin), red (dilated blood vessels) & brown (post-inflammatory pigmentation)
Image = Gottron’s papules

Spot diagnosis (dermnet)

Ringworm
Tinea corporis (ringworm) is the name used for infection of the trunk, legs or arms with a dermatophyte fungus.
In different parts of the world, different species cause tinea corporis. In New Zealand, Trichophyton rubrum (T. rubrum) is the most common cause. Infection often comes from the feet (tinea pedis) or nails (tinea unguium) originally. Microsporum canis (M. canis) from cats and dogs, and T. verrucosum, from farm cattle, are also common.
Spot diagnosis (dermnet)

Actinic keratosis
Rough scaly spots on sun-damaged skin are called actinic keratoses. They are also known as solar keratoses. They should be distinguished from other kinds of keratosis (scaly spot) such as seborrhoeic keratosis, porokeratosis and keratosis pilaris.
Actinic keratoses are a reflection of abnormal skin cell development due to exposure to ultraviolet radiation. They are considered precancerous or an early form of squamous cell carcinoma.
They appear as multiple flat or thickened, scaly or warty, skin coloured or reddened lesions. A keratosis may develop into a cutaneous horn.
Actinic keratoses are very common on sites repeatedly exposed to the sun especially the backs of the hands and the face, most often affecting the nose, cheeks, upper lip, temples and forehead. On the lips they are often called actinic or solar cheilitis. They are especially common in fair-skinned persons or those who have worked outdoors for long periods without skin protection. Sun-damaged skin is also dry, discoloured and wrinkled.
Spot diagnosis (dermnet)

Nodular melanoma
Malignant melanoma is a potentially serious type of skin cancer. It is due to uncontrolled growth of pigment cells, called melanocytes.
Normal melanocytes are found in the basal layer of the epidermis, i.e. the bottom part of the outer layer of the skin. The melanocytes produce a protein called melanin, which protects the skin by absorbing ultraviolet (UV) radiation. Melanocytes are found in equal numbers in black and in white skin, but the melanocytes in black skin produce much more melanin. People with dark brown or black skin are very much less likely to be damaged by UV radiation than those with white skin.
Nodular melanoma appears to be invasive from the beginning, and has little or no relationship to sun exposure.
Spot diagnosis (dermnet)

Superficial spreading melanoma
Superficial spreading melanoma is the most common type of melanoma, a potentially serious skin cancer that arises from pigment cells (melanocytes).
Superficial spreading melanoma is a form of melanoma in which the malignant cells tend to stay within the tissue of origin, the epidermis, in an ‘in-situ’ phase for a prolonged period (months to decades). At first, superficial spreading melanoma grows horizontally on the skin surface – this is known as the radial growth phase. The lesion presents as a slowly-enlarging flat area of discoloured skin.
An unknown proportion of superficial spreading melanoma become invasive, i.e. the melanoma cells cross the basement membrane of the epidermis and malignant cells enter the dermis. A rapidly-growing nodular melanoma can arise within superficial spreading melanoma and start to proliferate more deeply within the skin.
Superficial spreading melanoma is due to the development of malignant pigment cells (melanocytes) along the basal layer of the epidermis. The majority arise in previously normal-appearing skin. About 25% arise within an existing melanocytic naevus (mole), which can be a common or normal naevus, anatypical or dysplastic naevus or a congenital naevus.
What triggers the melanocytes to become malignant is not fully known. Specific gene mutations such as BRAFV600E have been detected in many superficial spreading melanomas and these mutations may change as the disease advances.
Damage by ultraviolet radiation results in a degree of immune tolerance, allowing abnormal cells to grow unchecked. This can occur from exposure to natural sunlight, particularly if sunburn has occurred, and artificial sources of ultraviolet radiation from sun beds / solaria.
Spot diagnosis (dermnet)

Squamous cell carcinoma (SCC) is a common type of skin cancer. It is derived from squamous cells, the flat cells that make up the outside layers of the skin, the epidermis. These cells are keratinising i.e., they produce keratin, the horny protein that makes up skin, hair and nails.
Invasive SCC refers to cancer cells that have grown into the deeper layers of the skin, the dermis. Invasive SCC can rarely metastasize (spread to distant tissues) and may prove fatal.
Invasive SCCs are usually slowly-growing, tender, scaly or crusted lumps. The lesions may develop sores or ulcers that fail to heal.
Most SCCs are found on sun-exposed sites, particularly the face, lips, ears, hands, forearms and lower legs.
They vary in size from a few millimetres to several centimetres in diameter. Sometimes they grow to the size of a pea or larger in a few weeks, though more commonly they grow slowly over months or years.
Spot diagnosis (dermnet)

Basal cell carcinoma
BCC typically affects adults of fair complexion who have had a lot of sun exposure, or repeated episodes of sunburn. Although more common in the elderly, sun-loving New Zealanders frequently develop them in their early 40s and sometimes younger.
The tendency to develop BCC may be inherited. BCC is a particular problem for families with basal cell naevus syndrome (Gorlin syndrome), Bazex-Dupré-Christol syndrome, Rombo syndrome, Oley syndrome and xeroderma pigmentosum. Recent research has detected genetic defects in common BCCs as well as in patients with these syndromes.
Spot diagnosis (dermnet)

Molluscum contagiosum
Molluscum contagiosum is a common viral skin infection. It most often affects infants and young children but adults may also be infected.
Molluscum contagiosum presents as clusters of small round bumps (papules) especially in the warm moist places such as the armpit, groin or behind the knees. They range in size from 1 to 6 mm and may be white, pink or brown. They often have a waxy, pinkish look with a small central pit (umbilicated). As they resolve, they may become inflamed, crusted or scabby. There may be few or hundreds of spots on one individual.
Molluscum contagiosum is a harmless virus but it may persist for months or occasionally for a couple of years. Molluscum contagiosum may rarely leave tiny pit-like scars.
Molluscum frequently induces dermatitis in the affected areas, which are dry, pink and itchy. An itchy rash may sometimes appear on distant sites and represents an immunological reaction or ‘id’ to the virus.
Molluscum contagiosum can be spread from person to person (especially children) by direct skin contact. This appears to be more likely in wet conditions, such as when children bathe or swim together. Sexual transmission is possible in adults.
Lesions tend to be more numerous and last longer in children who also have atopic eczema. It can be very extensive and troublesome in patients with human immunodeficiency virus infection.
Molluscum contagiosum may arise in areas that have been injured, often because they’ve been scratched. The papules form a row; this is known as koebnerised molluscum.
Spot diagnosis (dermnet)

Herpes
Spot diagnosis (dermnet)

Scabies
Scabies is an itchy rash caused by a little mite that burrows in the skin surface. The human scabies mite’s scientific name is Sarcoptes scabiei var. hominis.
Scabies is nearly always acquired by skin-to-skin contact with someone else with scabies. The contact may be quite brief such as holding hands. Frequently it is acquired from children, and sometimes it is sexually transmitted. Occasionally scabies is acquired via bedding or furnishings, as the mite can survive for a few days off its human host.
Scabies is not due to poor hygiene. Nor is it due to animal mites, which do not infest humans. However animal mites can be responsible for bites on exposed sites, usually the forearms.
Typically, an affected host is infested by about 10 -12 adult mites. After mating, the male dies. The female scabies mite burrows into the outside layers of the skin where she lays up to 3 eggs each day for her lifetime of one to two months. The development from egg to adult scabies mite requires 10 to 14 days.

A gentleman with a solitary painless ulcer on his penis also presents with this skin condition.
Spot diagnosis (dermnet)

Secondary syphilis
Syphilis is a complex sexually transmitted infection (STI) caused by the bacteria Treponema pallidum. Episodes of active disease occur, followed by latent periods, when the person remains infected but there are no signs or symptoms.
Initially syphilis appears as a painless sore (ulcer) where the infection entered (usually around the genitals) and may go unnoticed. The sore is known as a chancre and this phase is known as primary syphilis.
Widespread rash and ‘flu-like symptoms appear next (secondary syphilis).
If left untreated, tertiary syphilis may develop years later and cause a variety of problems affecting the heart, eyes, brain & bones.
Secondary syphilis
If left untreated or treatment has failed, about 3 weeks to 3 months after the 1st stage, a widespread skin rash occurs.
Rash may be subtle or appear as rough, red or reddish brown spots. Occur anywhere on the body but frequently affects palms and soles. May be mistaken for other conditions.
Patchy hair loss.
Raw and red mucosal surfaces such as inside the mouth, throat, genital area, vagina and anus (mucous patches).
Greyish-white moist raised patches in the groin, inner thighs, armpits, or under breasts (condyloma latum).
Other symptoms include fever, tiredness, muscle and joint pains, headache and swollen lymph glands.
Other affected organs may include liver, kidneys, central nervous system (CNS), joints and eyes.
What are the 5 main conditions that undergo the Koebner phenomenon?
Psoriarsis
Lichen Planus
Vitiligo
Viral Warts
Molluscum contagiousum.
A 19 year old Irish girl, who complains of abdominal pain especially after eating bread presents with this skin condition:
(dermnet)
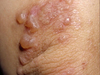
Dermatitis herpetiformis
Dermatitis herpetiformis (also known as ‘DH’ or Duhring disease) is a rare but persistent blistering skin condition related to coeliac disease.
Dermatitis herpetiformis is an ‘immunobullous’ condition, which means it is a blistering condition caused by an abnormal immunological reaction. Like other forms of coeliac disease, it involves IgA antibodies and intolerance to the gliaden fraction of gluten found in wheat, rye and barley.
Dermatitis herpetiformis often affects young adults; two thirds of patients are male. There is a genetic predisposition; there are associations with human leukocyte antigens (HLAs) DQ2 DQ8.
Eighty percent of patients with dermatitis herpetiformis also have gluten enteropathy, the most common form of coeliac disease. Some patients have personal or family history of other autoimmune disorders.
Dermatitis herpetiformis is unrelated to other forms of dermatitis such as atopic eczema, but these are common so may co-exist.
Dermatitis herpetiformis is characterised by extremely itchy bumps (prurigo papules) and blisters (vesicles), which arise on normal or reddened skin. They tend to be distributed symmetrically and are most often found on the scalp, shoulders, buttocks, elbows and knees.
As the blisters are so itchy, they are often immediately scratched, resulting in erosions and crusting. Older lesions may leave pale or dark marks (hypopigmentation and hyperpigmentation). Flat red patches, thickened plaques and raised wheals may arise, resembling dermatitis, scabies and other skin conditions.
Dermatitis herpetiformis may present initially as digital petechiae, which are small bleeding spots on fingers.
Treatment:
The medication of choice is dapsone, which considerably reduces the itch within a day or two. The dose required varies from 50 mg to 300 mg daily; refer to DermNet’s page about dapsone for potential side effects and monitoring requirements.
For those intolerant or allergic to dapsone, the following may be useful:
- Ultrapotent topical steroids
- Systemic steroids
- Sulfapyridine (not available in New Zealand).
A strict gluten-free diet is strongly recommended.
- It reduces the requirement for dapsone
- It improves associated gluten enteropathy
- It enhances nutrition and bone density
- It may reduce the risk of developing other autoimmune conditions
- It probably reduces the risk of intestinal lymphoma.
Spot diagnosis (dermnet)

Discoid lupus (a form of cutaneous lupus erythematosus)
Discoid LE: unsightly red scaly patches develop which leave postinflammatory pigmentation and white scars. It may be localised or widespread.
Discoid LE predominantly affects the cheeks, nose and ears, but sometimes involves the upper back, V of neck, and backs of hands.
Hypertrophic LE results in thickened and warty skin resembling viral warts or skin cancers.
Rarely, discoid LE occurs on the palms and/or soles (palmoplantar LE).
If the hair follicles are involved, they are first plugged with adherent scale and then bald areas can develop. If the follicles are destroyed, the bald patches are permanent (scarring alopecia).
Discoid LE may affect the lips and inside the mouth, causing ulcers and scaling. These lesions may predispose to squamous cell carcinoma.
Spot diagnosis (dermnet)

Subacute cutaneous lupus erythematous
In subacute LE, a non-itchy dry rash appears on the upper back and chest, often following sun exposure. Subacute LE does not scar. It includes the following clinical types:
Annular or polycyclic (ring-shaped)
Papulosquamous (scaly bumps)
Vasculitis (purple spots)
Nodular (lumps)
Significant internal (systemic) disease is uncommon with subacute LE.
Spot diagnosis (dermnet)
Patient also presents with abdominal pain, diarrhoea and occassional PR bleeding.

Pyoderma gangrenosum
Pyoderma gangrenosum is an uncommon cause of very painful skin ulceration. It may affect any part of the skin, but the lower legs are the most common site. Pyoderma gangrenosum is classified as a neutrophilic dermatosis and is considered a reaction to an internal disease or condition. It affects males and females of any age, but is more common in those aged over 50 years.
The name pyoderma gangrenosum is historical. The condition is not an infection (pyoderma), nor does it cause gangrene.
Pyoderma gangrenosum often affects a person with an underlying internal disease such as:
- Inflammatory bowel diseases (ulcerative colitis and Crohn disease)
- Rheumatoid arthritis
- Myeloid blood dyscrasias
- Chronic active hepatitis.
- Wegener granulomatosis
- PAPA syndrome
- Miscellaneous less common associations.
However, about 50% of those affected by pyoderma gangrenosum have none of the associated risk factors.
Clinical features:
Pyoderma gangrenosum usually starts quite suddenly, often at the site of a minor injury. It may start as a small pustule, red bump or blood-blister. The skin then breaks down resulting in an ulcer. The ulcer can deepen and widen rapidly. Characteristically, the edge of the ulcer is purple and undermined as it enlarges. It is usually very painful. Several ulcers may develop at the same time.
Untreated, the ulcers may continue to enlarge, persist unchanged or may slowly heal. Treatment is usually successful in arresting the process, but complete healing may take months. This is particularly true if there is underlying venous disease, another reason for leg ulcers.
Deep ulcers heal with scarring and this is sometimes with a characteristic cribriform or criss-cross pattern. A rare superficial bullous variant of pyoderma gangrenosum may heal without leaving a scar.
Treatment
Treatment is non-surgical. The necrotic tissue should be gently removed. Wide surgical debridement should be avoided because it may result in enlargement of the ulcer.
Often conventional antibiotics such as flucloxacillin are prescribed prior to making the correct diagnosis. These may be continued if bacteria are cultured in the wound (secondary infection) or there is surrounding cellulitis (red hot painful skin), but they are not helpful for uncomplicated pyoderma gangrenosum.
Small ulcers are best treated with:
- Potent topical steroid creams
- Intralesional steroid injections
- Special dressings eg. silver sulfadiazine cream or hydrocolloids.
- Oral anti-inflammatory antibiotics such as dapsone or minocycline.
- If tolerated, careful compression bandaging for swollen legs
- Potassium iodide solution
- Short-term nicotine as 0.5% in cetomacrogol cream, gum, patches, snuff
More severe disease requires immunosuppressive therapy:
- Tacrolimus ointment
- Oral steroids.
- Ciclosporin. .
- Methotrexate.
- Cyclophosphamide .
- Mycophenolate mofetil.
- Intravenous immunoglobulins and plasmapheresis
Treatment with the biological agent infliximab has also been reported to be effective in a small clinical trial of patients with pyoderma gangrenosum.
Outlook or prognosis for pyoderma gangrenosum is unpredictable.
Spot diagnosis (dermnet)

Acanthosis nigricans
Acanthosis nigricans (AN) is a skin disorder characterised by hyperpigmentation and hyperkeratosis of the skin, occurring mainly in the folds of the skin in the axilla, groin and back of the neck.
Acanthosis nigricans is not a skin disease per se but a cutaneous sign of an underlying condition or disease.
There are two important types of acanthosis: benign and malignant. Although classically described as a sign of internal malignancy, this is very rare. Benign types, sometimes described as ‘pseudoacanthosis nigricans’ are much more common.
Thickened brown velvety textured patches of skin that may occur in any location but most commonly appear in the folds of the skin in the armpit, groin and back of the neck.
- Papillomatosis (multiple finger-like growths) is common on cutaneous and mucosal surfaces.
- Skin tags often found in and around affected areas.
- Pruritus may be present.
- AN lesions may also appear on the mucous membranes of the oral cavity, nasal and laryngeal mucosa and oesophagus.
- Lesions involving the mucosa, palms and soles tends to be more extensive and more severe in malignant AN.
- Patients with malignant AN tend to be middle-aged, not obese and lesions develop abruptly.
Spot diagnosis (dermnet)

Pemphigus vulgaris
Pemphigus vulgaris is a rare autoimmune disease that is characterised by blisters and erosions on the skin and mucous membranes, most commonly inside the mouth. It is the most common subtype of pemphigus, accounting for 70% of all pemphigus cases worldwide although it is extremely rare in New Zealand (about one case per million). The other two main subtypes of pemphigus are pemphigus foliaceus and paraneoplastic pemphigus.
The building block cells of the epidermis are called keratinocytes. These cells are cemented together at special sticky spots called desmosomes. In pemphigus vulgaris immunoglobulin type G (IgG) autoantibodies bind to a protein called desmoglein 3, which is found in desmosomes in the keratinocytes near the bottom of the epidermis. The result is the keratinocytes separate from each other, and are replaced by fluid, the blister.
Diagnosis generally requires a skin biopsy, which shows typical features of rounded-up separated keratinocytes (called acantholytic cells) within the blisters just above the basal layer of the epidermis. Suprabasal clefting may be reported.
In most cases, circulating antibodies can be detected by a blood test (indirect immunofluorescence test). The level of antibodies fluctuates and may reflect the effectiveness of treatment.Pemphigus is confirmed by direct immunofluorescence staining of the skin biopsy sections to reveal antibodies.
Treatment
The primary aim of treatment is to decrease blister formation, prevent infections and promote healing of blisters and erosions. Oral corticosteroids are the mainstay of medical treatment for controlling the disease. Since their use, many deaths from pemphigus vulgaris have been prevented (mortality rate dropped from 99% to 5-15%). They are not a cure for the disease but improve the patient’s quality of life by reducing disease activity. Unfortunately higher doses of corticosteroids may result in serious side effects and risks. Other immune suppressive drugs are used to minimise steroid use.
Spot diagnosis (dermnet)

Bullous pemphigoid
Bullous pemphigoid is a blistering skin disease which usually affects middle aged or elderly persons. It is an immunobullous disease, i.e. the blisters are due an immune reaction within the skin.
Bullous pemphigoid results in crops of tense, fluid-filled, itchy bullae (large blisters). The blisters may be filled with clear, cloudy or blood-stained fluid. They may arise from normal-looking or inflamed skin.
A nonspecific red, itchy rash may be present for several weeks or months before blisters appear. The rash may be thought to be due to dermatitis or urticaria. The early plaques may resolve temporarily or persist, with or without treatment. They may have a smooth or dry surface and are often ring-shaped (annular).
Bullous pemphigoid may be localized to one area, or widespread on the trunk and proximal limbs. Frequently it affects the skin around skin folds. In severe cases, there may be blisters over the entire skin surface as well as blisters inside the mouth.
When the blisters heal up, they may leave brown marks (postinflammatory pigmentation) and/or tiny cysts called milia but these usually disappear within a few months. Direct immunofluorescence staining highlights antibodies along the basement membrane that lies between the epidermis and dermis. Indirect immunofluorescence test on blood serum may find circulating pemphigoid antibodies.
In most cases the diagnosis will be confirmed by a skin biopsy of a typical blister. Under the microscope, the pathologist can see a split between the outside layer of the skin, the epidermis, and the inside layer, the dermis.
If the pemphigoid is very widespread, hospital admission may be advised so the blisters and raw areas can be expertly dressed. Antibiotics may be required for secondary bacterial infection.
Most patients with bullous pemphigoid are treated with steroid tablets, usually prednisone. The dose is adjusted until the blisters have stopped appearing, which usually takes several weeks. The dose of prednisone is then slowly reduced over many months or years. As systemic steroids have many undesirable side effects, other medications are added to ensure the lowest possible dose (aiming for 5 to 10mg prednisone daily).
Spot diagnosis (dermnet)
Patient presents with this nail abnormality. Also has ash leaf macula, angiofibromas, and a Shagreen patch on his lower back.

Tuberous sclerosis
The nail change is a periungal fibroma.
Tuberous sclerosis or tuberous sclerosis complex is a genetic disorder that is characterised by hamartomas in many organs, but particularly the skin, brain, eye, kidney and heart. Hamartomas are non-cancerous malformations composed of overgrowth of the cells and tissues that normally occur in the affected area and include naevi (birthmarks). It is also known as epiloia.
Skin lesions, epileptic seizures and developmental delay/behavioural problems are the main features of tuberous sclerosis complex. However, individuals with the condition may be affected in many different ways and with differing degrees of severity. Some patients may have very few or no symptoms at all, whilst others may be severely affected with a multitude of symptoms.
About one third of all cases of tuberous sclerosis are inherited from an affected parent. All other cases are due to sporadic new mutations of the tuberin protein gene occurring in the early stages of life.
Skin lesions are found in 60-70% of cases of tuberous sclerosis. Characteristically, ash leaf macula, angiofibroma, a Shagreen patch (see pic) as well as peri-ungal fibromas.
Epilepsy is present in about 70% of patients with tuberous sclerosis.
Usually begins in infancy or early childhood and may precede appearance of skin lesions by years
The greater the number of tumours (cortical tubers) in the brain, the greater the severity of seizures.
Developmental delay and behavioural problems may also occur. Symptoms include mild to severe mental retardation, autism, attention deficit disorder (ADD), anxiety, depression, paranoia and schizophrenia.
Other signs and symptoms of tuberous sclerosis include:
Eye involvement: white spots on the iris and white lumps on the retina
Heart, gastrointestinal and kidney tumours
Lung changes

Spot diagnosis (Dermnet)
Patient presents with multiple lesions as pictured. Also had axillary freckling and some abnormal lesions in their iris.

Neurofibromatosis
Neurofibromatosis (NF) is a genetic disorder that affects the bone, soft tissue, skin and nervous system. It is classified into 2 distinct types, neurofibromatosis 1 (NF1) and neurofibromatosis 2 (NF2). NF1 occurs in about 1 in 3000 births whilst NF2 only occurs in about 1 in 50,000 births.
NF1, also known as von Recklinghausen disease, is characterised by the presence of:
- 6 or more café-au-lait spots (defined oval-shaped light brown patches greater than 0.5cm in diameter)
- Multiple neurofibromas (tumours on, under, or hanging off the skin)
- Freckling (under the armpits and areas of skin folds such as the groin)
- Lisch nodules (tiny tumours on the iris of the eye)
NF2, also known as bilateral acoustic neurofibromatosis, is characterised by multiple tumours and lesions on the brain and spinal cord. Tumours growing on the auditory nerves that lead to hearing loss is usually the first symptom of the disease. Often this is not apparent until the late teens or early 20’s.
NF1 and NF2 occur as a result of defects in different genes . NF1 is caused by a mutation on a gene located on chromosome 17 and NF2 on chromosome 22. The mutated gene can be inherited from a parent who has NF or in some cases you could be the founder of a spontaneously mutated gene. A parent with NF has a 50% chance of passing the gene on to each of their children.
Treatment
There is no cure for NF. The main goal of treatment is to monitor its development and intervene when necessary. Healthy children with NF should be followed-up and examined every 6-12 months by a paediatrician.
Neurofibromas that become large and painful can be cut out to reduce the risk of malignancy and other complications.
Genetic counselling and education about NF is important. One concern that should not be overlooked is the risk of isolation or loneliness in people with NF. People with NF are often anxious about future complications and sometimes disfiguring lesions can lead to withdrawal from society.
Targeted molecular therapies show promise for the future treatment of neurofibromatosis.
Spot diagnosis (dermnet)
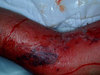
Necrotizing fasciitis
Necrotising fasciitis is a very serious bacterial infection of the soft tissue and fascia (a sheath of tissue covering the muscle). The bacteria multiply and release toxins and enzymes that result in thrombosis (clotting) in the blood vessels. The result is destruction of the soft tissues and fascia.
There are three main types of necrotising fasciitis:
- Type I (polymicrobial i.e. more than one bacteria involved). Bacteria causing type 1 necrotising fasciitis include Staphylococcus aureus, Haemophilus, Vibrio and several other aerobic and anaerobic strains. It usually follows significant injury or surgery.
- Type II (due to haemolytic group A streptococcus)
- Type III (gas gangrene) - Clostridia perfringens
Once the diagnosis of necrotising fasciitis is confirmed, treatment should be initiated without delay. Patients must be hospitalised, the causative organism(s) identified and treated with high dose intravenous antibiotics, often in an intensive care unit.
It is absolutely vital than an experienced surgeon urgently removes all dead tissue.
Treatment to raise blood pressure, hyperbaric oxygen, and intravenous immunoglobulin may also be necessary.
If diagnosed and treated early, most patients will survive with minimal scarring. However if there is significant tissue loss, later skin grafting will be necessary and in some patients amputation of limbs is required to prevent death. Up to 25% of patients will die from the disease and complications such as renal failure and septicaemia (blood poisoning) increase the likelihood of death.
Prompt diagnosis and treatment is essential to reducing the risk of death and disfigurement from necrotising fasciitis.
What is the Auspitz sign in psoriasis?
Scraping of psoriatic scale leads to pinpoint bleeding.
Koebner phenomenon occurs in which 5 conditions
- Psoriasis
- Lichen Planus
- Molluscum contagiousum
- Vitiligo
- Sarcoid
First line managment of lichen planus
Topical steroids

