Dermatopathology Flashcards
(146 cards)
What is the difference between a vesicle and a bulla?
A vesicle is <1cm and a bulla is >1 cm.
What pathological processes are usually involved when you see vesicles or bullas?
degeneration/necrosis or inflammation and repair.
What causes vesicles/bullas to form?
keratinocytes break apart and allow fluid to build. Can usually be caused by auto-immune dermatoses, viral infections, chemical irritants, and burns.
What is the difference between a pustule and a veiscle or bulla?
a pustule is a palpable elevation filled with pus.
What pathological processes would be involved in pustule formation?
inflammation and repair.
dried exudate, serum, blood, and scale adhered to the skin surface is referred to as what?
Crust
What would cause pustules to form?
leukocyte infiltrate
What causes could be involved in the formation of crust?
Severe disorders of keratinazation or severe pustular dermatitis. Crust formation can also be secondary to ulcers.
What pathological processes could be involved in the formation of crust?
degeneration/necrosis, inflammation and repair, or disorders of growth.
Can a vesicle turn into a pustule?
Yes, if it becomes infected.
Are papules fluid filled?
No. They are solid elevated masses, less than 1cm in diameter. (i.e. mosquito bite)
When would you refer to a papule as a nodule?
When it is greater than 1 cm in diameter and deeper.
What are plaques?
Coalesced papules, raised epidermis with a flat surface.
What pathological processes could be involved in the formation of papules?
inflammation and repair, disorders of growth, or deposits and pigmentation.
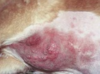
What is this a picture of?

Ulcers.
Loss of epidermis with exposure of dermis.
What pathological processes can cause ulcers?
Degeneration/necrosis, inflammation and repair, circulatory disorders, or disorders of growth
Ulcers can be caused by
epidermal necrosis, inflammation (really severe), infarction, or neoplasia.
This is an example of ____.

Scale, also known as dandruff.
What is scale? What is the most common cause of it?
Scale is an accumilation of loose keratinized cells. Chronic dermatitis is the most common cause.
What is this a picture of? What causes them to occur?

Epidermal collarettes. They are a circular rim of scale that occurs secondary to the rupture of a vesicle, pustule, or papule.
What is this? What causes it?

Thickening and hardening of the skin, also known as lichenification. Caused by chronic irritation/inflammation.
What are some things you should when collecting a skin biopsy?
Collect it early, before treatment
Be gentle
Collect multiple samples, range of changes
Include crusts!
Should you surgically prep the site before collecting a skin biopsy?
No!
What does St. John’s Wort cause?
Type I photosensitization