Ear infections Flashcards
(15 cards)
most common causes of hearing loss
ear wax, otitis media and otitis externa.
Acute otitis media
risk factors (6) and causes
- Lack of breast feeding as a baby (formula fed)
- FHx
- passive smoking
- downs sydrome
- Cystic fibrosis
- attend daycare or nursery
Cx:>>URTI causes inflammed upper airways and swelling will block ET
Viral: RSC, Rhinovirus, enterovirus
Bacterial: strep pneumonia, H.influenza, Morexella Catarrhalis
lally’s tip: the middle ear is respiratory epthelium or pseudostratified, which is why the organisms r similar pathogens to the resp ones!
OME
causes
what do u think if it occured to an adult?
due to ET dysfunction
in kids its smaller and more horizontal, also more prone to having enlarged tonsils blocking ET.
- Downs sydrome, CF–>thick mucus
- Primary ciliary dyskinesia
- Smoking exposure–>thick mucus
- facial anomilies–>cleft palate,
- Allergic Rhinitis
- Bottle feeding — feeding with unventilated, or underventilated bottles can generate negative pressure in the middle ear.
IN ADULTS DANGEROUS–>Nasopharyngeal TUMORS blocking ET
Symptoms OM and OME
Signs on Otoscope
OM: otalgia (baby tugs on ear), fever, vommitting
Signs: bulging red TM,
OME: Hearing loss (most common Cx of deafness in kids), learning difficulties, behavioral problems
Signs: dull, straw coloured, retracted TM, loss of light reflex, Air bubbles
Tx
OM vs OME
- when do u give antibiotics in OM? (3)*
- which antibiotic?*
- when do u refer to ENT in OME*
OM:
- Conservative – analgesia (paracetamol & ibuprofen)
- Medical – In severe or persistent cases oral antibiotics may be required
- Surgery – Recurrent AOM may be helped by grommet
Give antibiotics if:
- Ptx who r systemically very unwell.
- Ptx who have symptoms and signs of a more serious illness or condition.
- People who have a high risk of complications.
5–7 day course of _AMOXICILLIN_ recommended first-line.
OME: –> maku salfa antiobiotics!
- watch and wait–> 50% resolve spontaneously w/in 3 mnths
- During checkups check hearing via 2 hearing tests using PTA at least 3 months apart as well as tympanometry.
- refer ENT if above shows bad hearing loss or delay in developmental milestones!
nonsurgical:
- Active observation (every 3 mnths)
- Hearing aids (if Sx is contraindicated)
- Autoinflation–> involves blowing up a balloon via the nostril 2-3 x day, thus ventilating the middle ear–> equilibrating pressure, and allowing some drainage of fluid.

What are the surgical options for children with OME?
Myringotomy + insertion of grommets (ventilation tubes) +- adenoidectomy.
Grommets fall out in 9-10 mnths & most kids will need reinsertion within 5 years.
Management of persistent AOM involves (3)
- Reassessing the person.
- Considering the need for paediatric or ENT referral or admission, depending on the clinical situation.
- Considering a first-line antibiotic (if not already prescribed) or a second-line antibiotic if the initial treatment was ineffective.(co-amoxivlav)
prevention of recurrent AOM include:
In children —
- avoiding exposure to passive smoking,
- use of dummies, and flat, supine feeding
- ensuring children have had a complete course of pneumococcal vaccinations as part of the routine childhood immunization schedule.
In adults — avoiding smoking and/or passive smoking.
Ix: OME (2)
- Tympanometry assesses the ability of the eardrum to react to sound–> will show FLAT trace due toreduced compliance of TM
- PTA –> reveal conductive hearing loss
IN ADULT with unilateral ear effusion–> flexible nasal endoscopy to rule out TUMOR!

who should be screened in OME?
Children with Down’s syndrome or cleft palate should be regularly assessed (every 3–6 months) for OME by ENT specialist
Complx of Grommets (6)
- Otorrhoea (ear discharge) — most common
- Tympanosclerosis
- Infection
- Fibrosis.
- Cholesteatoma.
- Bleeding.

OE
acute vs chronic
Cx (3) &Precipitating factors(3)
symptoms (4) & signs
Complications
- Acute: <3 mnths
- chronic: >3mnths
Causes: Pseudomonas aeruginosa, S aureus, S epidermis
Precipitating factors: ear trauma, excessive moisture, dermatitis.
Symptoms: otalgia, itching, otorrhea,hearing loss
otoscopy: red, swollen, or eczematous canal, unabke to see TM
Complications: abscess, inflammation TM, and malignant otitis.
Management of otitis externa?
when to refer to ENT?
- Offer Analgesia: paracetamol or ibuprofen (plus codeine for severe pain).
- Topical antibiotic (or COMBINED topical antibiotic + steroid) if TM is perforated aminoglycosides are not used*
- Providing appropriate self-care advice
- consider ear swab (if symptoms persist for ages)
- If there is canal debris then consider removal
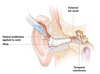
- if the canal is extensively swollen then an ear wick is sometimes inserted
If a patient fails to respond to topical antibiotics –> referred to ENT.
what is this?
who gets this?
what causes it?
Key features in history? (5)
Dx?
Tx?

Malignant otitis externa (necrotising)
- aggressive infection where infection spreads from the soft tissue of the ear canal into the bone
- found in immunocompromised individuals! DIABETES
- most commonly caused by Pseudomonas aeruginosa
Hx key features
- Diabetes (90%)
- deep seated severe ear pain at NIGHT
- Temporal headaches
- chronic ear discharge despite treatment
- Possibly dysphagia, hoarseness, and/or facial nerve Palsy
Tx
- aggressive treatment with IV antibiotics CIPRFLOXACIN as well as topical treatment for an extended period of time to eradicate infection
(ii) Chronic Otitis Media


