Male reproductive endocrinology Flashcards
(29 cards)
State the two main functions of the testis
- Secrete testosterone
- Production of sperm by the process of spermatogenesis.
Spermatogenesis takes place in what structure of the testis?
Semiferous tubules
What is the passage of sperm from testis to outside the body?
Seminiferous tubules
Rete Testis
Efferent ductules
Epididymis (where final maturation of sperm formation occurs)
Vas Deferens
Ampulla
Ejaculoatory duct
Urethra
The testis is surrounded by the tunica ??? and the tunica ???. It is divided into ???? lobules. Lobules contain the ???? tubules.
The testis is surrounded by the tunica albuginea and the tunica vaginalis . It is divided into 200-300 lobules. Lobules contain the seminiferous tubules.

Define spermatogenesis
Where does it take place?
How many sperm do men make per day? How long does it take to make a mature sperm?
They are prodcued from ????, rather than being born with them like women. Production continues through to death.
Process by which immature stem cells (spermatogonia) proliferate and differentiate into mature sperm.
In the seminiferous tubules
100 million per day - takes 64 days to make a mature sperm
Puberty
There are 2 major compartments in the seminiferous tubules. What are they?
The lumen of tubules and the interstitium
Germ cells around found throughtout the wall of the seminiferous tubules. The most mature germ cells are found towards the ?? of the tubule, with the least mature being found ?? to the lumen.
The area between the tubules is called the ??, and this is where you will primarily find ??? cells.
Germ cells around found throughtout the wall of the seminiferous tubules. The most mature germ cells are found towards the lumen of the tubule, with the least mature being found distal to the lumen.
The area between the tubules is called the interstitum, and this is where you will primarily find leydig cells.
SE = Seminferous tubule
I = interstitum
C = capillaries

What other cells aside from the germ cells around within the seminiferous tubules? What is another name for this cell (knowing this will help to explain it’s function later)
Sertoli cell - Nurse cell

Sertoli cellls are the columnar epithelial supporting cells of the ???. They have a large ??? . which spans from the basement membrane to the lumen. They are derived from the ?? of the developing testis.
The sertoli cells surrond the proliferating and differentiating germ cells, forming pockets around these cells, providing ???. They will ??? excess spermatid cytoplasm.
They are connected to other by ?????, that seal the tubule into two compartments, the?? and ??compartment. This is creating a division between cells that have and have not undergone meiosis. This is important, as haploid cells can potentially be recognised as foreign.
Large molecules cannot pass between the ? and ? compartments - this is called the ???
Sertoli cells (nurse cells) are the epithelial supporting cells of the seminiferous tubules. They have a large cytoplasm. which spans from the basement membrane to the lumen.They are derived from the sex cords of the developing testis.
The sertoli cells surrond the proliferating and differentiating germ cells, forming pockets around these cells, providing nutrition. They will phagocytose excess spermatid cytoplasm.
They are connected to other by tight junctions, that seal the tubule into two compartments, the basal and adluminal compartment. This is creating a division between cells that have and have not undergone meiosis. This is important, as haploid cells can potentially be recognised as foreign.
Large molecules cannot pass between the basal and adluminal compartments - this is called the blood-testis barrier.

The process of spermatogenesis involves 3 main cell types, going from most immature, to most mature.
Spetmatogonia, Spermatocytes, Spermatids
Furthermore, it can be considered that there are 3 stages; Mitotic proliferation, meiotic division (important to half the chromosome number) and differentiation.
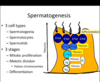
The spermatogonia reside on the basal compartment of the seminferous tubules. Begining at puberty, they divide by ???? - they are diploid.
There are two subtypes of spermatogonia, type A and type B.
Type A can be further divided into ? and ? types - named according to how their cytoplasms appear.
The dark (Ad) are the “reserve populatiom”. They will turn over and keep the spermatogonia going.
The pale spermatogonia are more for going down the pathway to produce ???. They divide by ??, to give???
Then, ??? divide by ??? to give ???.
The spermatogonia reside on the basal compartment of the seminferous tubules. Begining at puberty, they divide by mitosis - they are diploid.
There are two subtypes of spermatogonia, type A and type B.
Type A can be further divided into dark(blue on diagram) and pale types - named according to how their cytoplasms appear.
The dark (Ad) are the “reserve population”. They will turn over by mitosis and keep the spermatogonia going.
The pale type A spermatogonia are more for going down the pathway to produce sperm. They divide by mitosis, to give Type B spermatogonia.
Then, Type B spermatogonia divide by mitosis to give Primary spermatocytes.

Once we have our primary spermatocyte, it will then undergo ???. This division produces ???. ???? then enter ????, and produce ????. ???? can then differentiate to give ?????.
Once we have our primary spermatocyte, it will then undergo meosis I. This division produces secondary spermatocytes. Secondary spermatocytes then enter meiosis 2, and produce spermatids. ???? can then differentiate to give mature sperm.

What is the process of differentiation called by which spermatids differentiate into mature sperm?
Spermiogenesis
Spermiogenesis does NOT involve further ????. The spermatid begins to reorganise it’s internal structure going from rounded and elongated, including the formation of the propulsive structure, the ???. This is accompanied by lots of cytoplasmic remodelling as well as ??? of the nucleus. As cytoplasm is reduced as the spermatid matures, parts of the cytoplasm get pushed to one side. of the spermatid, forming a residual body of cytoplasm. This excess cytoplasm can be phagocytosed by ??? cells.
Another important area that is developed between the head and the tail of the sperm, which is called the ????. This section contains lots of ????, that are arranged as spirals around a filamentous core. The filamentous core forms a drive shaft connection to the ???. Energy for sperm motility comes from the metabolism of ??? in the seminal fluid.
Another important structure that forms is called the acrosome, which lies in the anterior thirds of the sperm nucleus. The acrosome is a large secretory vesicle, originating from the golgi complex in the spermatid, and contains many ???? that will factilitate pentetration of the ??.

Spermiogenesis does NOT involve further division. The spermatid begins to reorganise it’s internal structure going from rounded and elongated, including the formation of the proprolsive structure, the flagellum. This is accompanied by lots of cytoplasmic remodelling as well as compaction of the nucleus. As cytoplasm is reduced as the spermatid matures, parts of the cytoplasm get pushed to one side. of the spermatid, forming a residual body of cytoplasm. This excess cytoplasm can be phagocytosed by Sertoli cells.
Another important area that is developed between the head and the tail of the sperm, which is called the Midpiece. This section contains lots of mitochondria that are arranged as spirals around a filamentous core. The filamentous core forms a drive shaft connection to the flagellum. Energy for sperm motility comes from the metabolism of fructose, in the seminal fluid.
Another important structure that forms is called the acrosome, which lies in the anterior thirds of the sperm nucleus. The acrosome is a large secretory vesicle, originating from the golgi complex in the spermatid, and contains many enzymes that will factilitate pentetration of the ovum.

Label the structures of the sperm


What are the 3 main somatic cell types that make are found in and around the testis?
Sertoli cells
leydig cells
Peritubular myoid cells
Leydig cells are found in the ?? around the seminiferous tubules. The cytoplasm of these cells is very ???, because they contain many cholesterol-lipid droplets.
They make and secreteion ????, in response to ???? from the pituitary.
Leydig cells are found in the interstituim around the seminiferous tubules. The cytoplasm of these cells is very pale, because they contain many cholesterol-lipid droplets.
They make and secrete testosterone, in response to Lutenizing hormone from the pituitary.
Sertoli cells also produce ????, which is important in masculisation of genital structures during development (also allowing for degenration of the paramesenphric duct).
FSH stimulates the sertoli cells to secrete ????, into the lumen of the ????. Whilst this is occuring, you obviously have the testosterone moving into the lumen as well after it’s production by the leydig cells. This testosterone binds to the ???, concentrating it in the seminferous tubules. This gives the spermatoogonia a much needed supply of testosterone.
Sertoli cells also produce anti-mullarian hormone , which is important in masculisation of genital structures during development (also allowing for degenration of the paramesenphric duct).
FSH stimulates the sertoli cells to secrete androgen binding protein, into the lumen of the seminiferous tubules. Whilst this is occuring, you obviously have the testosterone moving into the lumen as well after it’s production by the leydig cells. This testosterone binds to the androgen binding protein,concentrating it in the seminferous tubules. This gives thespermatoogonia a much needed supply of testosterone.
The 3rd main somatic cell is the peritubular myoid cell, which surrounds the ??? of the seminiferous tubule. These are squamous contractile cells. However, the main role, in promoting renewal and maintenance of the ????? cell population. They also have been shown to signal to ?? cells.
The 3rd main somatic cell is the peritubular myoid cell, which surrounds the basement memrbane of the seminiferous tubule. These are squamous contractile cells. However, the main role, in promoting renewal and maintenance of the Type A spermatogonial stem cell population. They also have been shown to signal to sertoli cells.
One important point to note, is that the germ cells do not have receptors for FSH, LH or Testosterone (Although they do have oestroegn receptors), emphasising the importance of Sertoli, Leydig and peritubular myoid cells.
For example, Sertoli cells, aside from Androgen binding proteins, also produce ?? and ??.
?? are essential for support of spermatgenesis and for initiation of meiosis, whilst ?? are responsible for exerting negative feedback on the GnRH axis that acts to inibit FSH secrrtion.
Furthermore, whilst leydig cells make testosterone, receptors can be found on ?? cells.
Sertoli cells also have the enzyme ??, which coverts testosterone to oestrogen.
One important point to note, is that the germ cells do not have receptors for FSH, LH or Testosterone (Although they do have oestroegn receptors), emphasising the importance of Sertoli, Leydig and peritubular myoid cells.
For example, Sertoli cells, aside from Androgen binding proteins, also produce growth factors and inhibins.
Growth factors are essential for support of spermatgenesis and for initiation of meiosis, whilst inhibins are responsible for exerting negative feedback on the GnRH axis that acts to inibit FSH secrrtion.
Furthermore, whilst leydig cells make testosterone, receptors can be found on sertoli cells cells.
Sertoli cells also have the enzyme aromatase, which coverts testosterone to oestrogen.

Let’s think the overall regulation of all of the hormone release and gametogenesis. The onset of puberty can be thought of when GnRH is released from the hypothalamus acts on the ?? pituitary causing release of ?? and ??. These of course can enter the testis. FSH acts on the ?? cells to begin the facilitation of ????. LH will act on the ??? cells to make and release ?? into both the systemic circulation and the testes. Testosterone is also responsible for the development of ??? characteristics.
Let’s think the overall regulation of all of the hormone release and gametogenesis. The onset of puberty can be thought of when GnRH is released from the hypothalamus acts on the anterior pituitary causing release of FSH and LH These of course can enter the testis. FSH acts on the sertoli cells to begin the facilitation of spermatogenesis. LH will act on the leydig cells to make and release testosterone into both the systemic circulation and the testes. Testosterone is also responsible for the development of secondary sexual characteristics.
LOOK AT MIND MAP FOR ALL OF THE REGULATOIN OF SPERMATOGENESIS STUFF :)
Define endocrine disruptors
- Exogenous substance the disurpts the body’s endocrine system and produce developmental, reproductive, neurological and immune effects in both humans and wildlife.
- Can decrease, or increase endocrine functions
- Can affect a specific endocrine organ, but can also go onto to effect other tissues
- Can affect a hormone or a receptor for that hormone
- Can be natural or man made
There are many possible sources for endocrine disruptors. Natural hormones may be released into the environemnt - i.e. sewage by humans. This sewage might get spread onto fields where animals are grazing - these animals migtht be destined for the ?? chain.
There are also natural chemicals produced by ???/???, such as ???. This can also enter the food chain.
They can also be synthetically produced. Exxamples include the contraceptive pill, or patients who are taking hormone treatments for cancer.
They can also be made made, such as food ??? such as ???, as well as plastic additives.
There are many possible sources for endocrine disruptors. Natural hormones may be released into the environemnt - i.e. sewage by humans. This sewage might get spread onto fields where animals are grazing - these animals migtht be destined for the food chain.
There are also natural chemicals produced by plants/fungi, such as Phytoestrogens. This can also enter the food chain.
They can also be synthetically produced. Exxamples include the contraceptive pill, or patients who are taking hormone treatments for cancer.
They can also be made made, such as food additives such as DDT, as well as plastic additives.


