10/21- Liver failure and portal HTN Flashcards
(82 cards)
What is seen here?

Normal liver (left) vs. cirrhosis (right)
Non-invasive alternatives to liver biopsies?
- Fibroscan
- Magnetic Resonance Elastography (MRE)
Describe Fibroscan
- Pros/cons
Fibroscan
- Works best on thin patients
- Tells you how stiff/soft the liver is (stiffness can indicated cirrhosis)
What do these fibroscan results show?

- Not as steep slope on left (stiffer?)
- Steep slope on right (softer?)
How do liver diseases compare on fibroscan results (grades of stiffness)?
Different diseases cause different fibrotic patterns and different densities. Also happen at different times

Describe Magnetic Resonance Elastography (MRE)
Again, indicates stiffness (blue -> red scale)
- Newer technique
- Good for saying yes/no to cirrhosis

What are the 3 types of liver decompensation?
- Synthetic failure
- Portal HTN
- Hepatocellular Carcinoma (HCC)
What are markers of synthetic failure in terms of liver disease (what symptoms do you see)?
Synthetic Failure
- Jaundice
- Prolonged INR (low clotting factors)
- Hypoalbuminemia
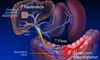
What are signs/symptoms of portal hypertension?
Portal vein entering the base of the liver; dilates; 3x increase in pressure (4->12 mmHg)
- Hypersplenism
- Fluid retention
- Ascites and peripheral edema
- Varices
- With/without bleeding
- Encephalopathy
What are the cardinal signs of liver failure?
If you have any of these, you have liver failure.
Mortality goes up significantly once any of these happen
- Jaundice
- Ascites
- May include SBP
- May include peripheral edema
- Variceal bleed
- Encephalopathy
- Clinical or subclinical
Other signs of liver failure?
- Spider angiomata
- Fed from the middle (blanching)
- Surprisingly common in people with cirrhosis (especially alcoholic)
- Palmar erythema
- Dupuytren contracture
Describe bilirubin synthesis
- RBCs -> hemoglobin -> globin + heme
- Heme is degraded into bilirubin (unconjugated); carried with albumin to liver
- Bilirubin transported into hepatocyte and binds Ligandin
- Glucuronidation -> conjugated bilirubin
- Bilirubin conjugation actually involves clevage site, heme oxygenase conversion into Biliverdin, and then conjugated bilirubin
- Bile excreted into bile duct In the intestine:
- Bilirubin glucuronide (conjugated) converted back into bilirubin (unconjugated) by gut bacteria
- Bilirubin converted into urobilinogen/urobilin
- Urobilin should be reabsorbed and sent to kidney (yellow color of urine)
- Urobilinogen converted to stercobilin and excreted by gut (brown color of stool)
**There is no bilirubin in urine or stool!
What are causes of high unconjugated (indirect) bilirubin?
Excess bilirubin production
- Hemolysis
Failure of conjugation (typ hereditary)
- Gilbert syndrome
- Neonatal jaundice
- Crigler-Najjar
(Other lecture also mentioned decreased uptake such as with Rifampin)
What are causes of high conjugated (direct) bilirubin?
- Biliary obstruction
- Liver damage
- Failed excretion
- Dubin-Johnson
- Rotor
(Other lecture separated this into main liver disease or obstructive causes; important here to also add failed excretion)
How is clinical testing for direct vs. indirect bilirubin done?
Uses a color assay (diazo)
- Conjugated bilirubin is soluble and direct-reacting
- Unconjugated bilirubin is not soluble and only reacts after alcohol is added
After initial and then alcohol stages, the total amount has reacted
- Indirect is calculated by subtracting direct from total
- A small amount of unconjugated reacts without alcohol (5-10% of total), so direct levels might be a tad high
- Normal unconjugated levels are 0, but will get a low amount using this assay
What is cholestasis?
Failure of bile excretion
What are effects of cholestasis?
- Bile contents in the circulation
- Bilirubin -> jaundice
- Bile salts -> pruritis
- Hepatocyte effects
- Obstruction -> alkaline phosphatase
- Damage -> ALT and AST
- Malabsorption of fats and fat-soluble vitamins
- Absence of stercobilin in stool (clay-colored) and urobilin in urine (colored instead by bilirubin, darker?)
Look at these pictures of dilated bile ducts due to obstruction

What is shown here?

ERCP
- Large duct obstruction
- Can see stone and dilated duct leading into liver
What is seen here? Main features?

Normal liver histology
- Portal tract (triad)
- Terminal hepatic venule
- Zones 1-2-3 moving from tract -> venule

What are diseases of small duct obstruction
- Primary biliary cirrhosis (aka non-suppurative
- Primary sclerosing cholangitis
What happens in primary biliary cirrhosis?
- PBC – cells and lymphocytes destroy bile duct
- Granulomas
What happens in primary sclerosing cholangitis?
- Primary sclerosing cholangitis
- Bead signs (dilated and strictured areas
- Thick onion-skin appearance of fibrous tissue obstruction the duct
What is seen here?

Primary biliary cirrhosis
- PBC – cells and lymphocytes destroy bile duct
- Granulomas