57 Principles of Wound Healing Flashcards
(23 cards)
What are the layers of skin?
What are the layers of skin?
The epidermis and dermis are the two main layers of skin. The epidermis is further separated into the stratum corneum, stratum lucidum, stratum granulosum, stratum spinosum, and stratum basale (from superficial to deep). The layers of the dermis include the papillary and reticular dermis.
What is a scar?
What is a scar?
A scar is an area of fibrosis that replaces normal skin after injury. A scar always forms after an injury, as it is the product of a normal wound healing process. Scars can be made less visible with various surgical and nonsurgical techniques.
What is healing by primary intention?
What is healing by primary intention?
Healing by primary intention healing occurs when the edges of the wound are brought together in direct contact, which may involve sutures, staples or other closure methods. This is the most commonly used method of wound closure and results in a minimally visible surgical scar.
What is healing by secondary intention?
What is healing by secondary intention?
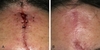
Healing by secondary intention occurs when wound edges are not approximated, leaving an area of exposed subcutaneous tissue. This may result in greater wound contracture than seen in primary closure. This type of healing works best in concavities (e.g., temporal fossa, medial canthus, alar groove). It can be useful in scalp and forehead wounds. Advantages include low risk of infection, high rate of healing, acceptable cosmesis, and surveillance in cases where cancer may be incompletely excised.
FIgure: A, B. Healing by secondary intention of a forehead wound.
What is healing by tertiary intention?
What is healing by tertiary intention?
Healing by tertiary intention is delayed primary closure. Wound edges are not closed immediately, but the defect is allowed to undergo the acute inflammatory phase in which phagocytosis of contaminated tissue occurs and the microbial count decreases. The wound edges are then brought together and closed.
What are the three phases of surgical wound healing?
What are the three phases of surgical wound healing?
- Inflammatory Phase (injury to approximately 1 week)
- Proliferative Phase (30 minutes to approximately 1 month)
- Remodeling Phase (3 weeks to approximately 1 year)
What occurs in a wound during the inflammatory phase?
What occurs in a wound during the inflammatory phase?
Local vasoconstriction occurs within the first 5 to 10 minutes; then the coagulation cascade proceeds and a fibrin clot is formed. Activated platelets release several chemotactic factors that affect vascular tone. Vasodilation subsequently ensues secondary to histamine release. Next, the cellular response begins. Macrophage, neutrophil, and lymphocyte infiltration occurs, hallmarking the inflammatory phase. Importantly, only when inflammation subsides, does collagen deposition begin. Therefore, wounds with excess nonviable debris will experience a prolonged inflammatory phase.
What is the proliferative phase?
What is the proliferative phase?
The proliferative phase begins with re-epithelialization of the wound. This process begins at the time of the injury, and in primary closure is completed in 24 hours. Collagen synthesis begins on day 2. Fibroblasts proliferate and produce type III collagen, elastin, and extracellular matrix. The final component of the proliferative phase is wound contraction, which is mediated by myofibroblasts. This contraction is centripetal and is maximal at 10 to 15 days. Contraction may be severe in inflamed wounds.
What is the remodeling phase?
What is the remodeling phase?
Collagen remodeling and vascular maturation occur in the remodeling phase. Scars become pale, soft, and less protruding. Type III collagen initially deposited in the proliferative phase is converted into type I collagen. Collagen fibers become more organized into parallel bundles. Completion of remodeling may take 12 to 18 months and, even then, scars achieve only 70% to 80% of the tensile strength of normal skin.
What four local factors influence wound healing?
What four local factors influence wound healing?
- Oxygenation
- Infection
- Foreign bodies
- Venous sufficiency
What chemotactic and proliferative factors are released during wound healing?
What chemotactic and proliferative factors are released during wound healing?
- Growth Hormone (GH): Produced by the pituitary gland; promotes fibroblast proliferation
- Epidermal Growth Factor (EGF): Produced by platelets; promotes epithelial cell and fibroblast proliferation and migration; activates fibroblast and vascular formation
- Platelet Derived Growth Factor (PDGF): Produced by platelets, macrophages, endothelial cells and keratinocytes; functions as chemoattractant for neutrophils, macrophages, and fibroblasts. Also works as mitogenic agent for fibroblasts, inducing production of collagen and hyaluronic acid.
- Fibroblast Growth Factor (FGF): Produced by macrophages, mast cells, lymphocytes, endothelial cells, and fibroblasts; promotes proliferation of vascular endothelial cells; also mitogenic for keratinocytes and fibroblasts
- Transforming Growth Factor (TGF): Produced by platelets, fibroblasts, neutrophils, macrophages, and lymphocytes; promotes proliferation of epithelial cell and fibroblasts
- Insulin-like Growth Factor (IGF-1): Produced by liver, plasma, and fibroblasts; promotes fibroblast proliferation and synthesis of extracellular matrix
- Tumor Necrosis Factor (TNF): Produced by macrophages, mast cells, and lymphocytes; promotes fibroblast proliferation
What are the tenets of Halstead?
What are the tenets of Halstead?
These tenets address gentle handling of tissue, aseptic technique, sharp anatomic dissection, obliteration of dead space, careful hemostasis, and avoidance of wound tension. These principles are highly important to surgical wound healing.
How does wound desiccation affect healing?
How does wound desiccation affect healing?
A moist environment is essential for wound healing, particularly in re-epithelialization. Dry, scabbed wounds heal more slowly than wounds with adequate humidity. Desiccation increases the energy expenditure of epithelial cells in wound closure, thereby lengthening wound healing time.
How are wound healing phases affected by oxygen?
How are wound healing phases affected by oxygen?
Initial hypoxia by vasoconstriction and vascular disruption actuates the early phases of wound healing by activating platelets and endothelium. However, recovery of tissue oxygenation is required for adequate healing, and chronic hypoxia can disrupt all aspects of wound healing.
What are relaxed skin tension lines (RSTLs)?
What are relaxed skin tension lines (RSTLs)?
These are lines of tension that are intrinsic to the skin and determined largely by the underlying collagen matrix. RSTLs typically lie parallel to wrinkles. Incisions made at 90-degree angles to RSTLs will gape open widely, while those lying parallel will close with minimal tension.
Describe the differences and similarities between hypertrophic scars and keloids.
Describe the differences and similarities between hypertrophic scars and keloids.
Hypertrophic scars:
- Remain within the boundaries of original tissue injury.
- Tend to regress with time.
- Contain collagen fibers in a wavy, randomly organized pattern, parallel to the epithelial surface.
Keloids:
- Tend to overgrow the boundaries of the initial tissue injury.
- May continue to enlarge with time.
- Can be treated with intralesional corticosteroids, interferons, or radiation.
- Contain thick collagen fibers, closely packed together, haphazardly oriented to the epithelial surface.
Figure: A, A profound keloid scar stemming from ear piercings. B, A hypertrophic scar of a neck apron incision following thyroidectomy.

How do vitamin deficiencies affect wound healing?
How do vitamin deficiencies affect wound healing?
Vitamin A is important in epithelialization, collagen synthesis, and cross-linking. Vitamin C is an important cofactor in lysine and proline hydroxylation in collagen synthesis. It is also important to neutrophil function and serves as a reductant in free radical formation (“antioxidant”). Vitamin E reduces collagen production, thereby decreasing wound tensile strength. Vitamin K is important to the production of clotting factors II, VII, IX, and X. Zinc is important to wound healing by promoting cell differentiation and fibroplasia.
Which lifestyle factors affect wound healing?
Which lifestyle factors affect wound healing?
Smoking, through the effects of nicotine, leads to vascular compromise and causes wound tissue ischemia and delayed healing. Alcoholism is associated with global malnutrition, which is detrimental to the wound healing process.
What is the ideal dressing for a surgical wound?
What is the ideal dressing for a surgical wound?
An ideal dressing for a surgical wound would have the following characteristics: maintains a moist wound environment, absorbs exudate, and keeps the surgical site protected.
What are the types of collagen?
What are the types of collagen?
Type I collagen: Found in skin, bone, and tendons and supports connective tissue
Type II collagen: Found in cartilage, corneal stroma, and vitreous humor; promotes shock absorption and joint mobility
Type III collagen: Ubiquitous; promotes formation of fibrous elements
Type IV collagen: Found in basement membranes; forms a scaffold for filtration
Type V collagen: Ubiquitous; forms cytoskeleton around cells
How does radiation affect wound healing?
How does radiation affect wound healing?
Radiation leads to diminished fibroblast, myofibroblast, and endothelial cell proliferation. There is also considerable ischemia of tissue due to hyalinization and sclerosis of blood vessels. This leads to overall delay and poor wound healing in radiated patients.
What is the role of vacuum-assisted closure in otolaryngology?
What is the role of vacuum-assisted closure in otolaryngology?
Vacuum-assisted closure may be used in skin grafts to remove fluid secretions that prevent revascularization and imbibition of the graft. They are also used to promote granulation in infected wounds that are healing by secondary intention. Vacuum-assisted devices must not be used in nasal, oral, tracheal, blood vessels or neoplastic sites.
What is the role of autologous platelet rich plasma in wound healing?
What is the role of autologous platelet rich plasma in wound healing?
Controversial
The theoretical principle of the use of platelet rich plasma (PRP) in wound healing is that platelets are a potent source of growth factors and a concentrate of these growth factors potentially improves healing. Clinical reports studying the efficacy of PRP in reducing ecchymosis and edema have been mixed and its use remains controversial.


