What is aneurysm disease?
Dilation of all layers of the aorta leading to an increase in diameter of >50% (abdominal aorta > 3.5cm)
What is dilation of all layers of the aorta leading to an increase in diameter of >50% (abdominal aorta > 3.5cm) called?
Aneurysm
What is the aetiology of aneurysm disease?
Degenerative disease
Connective tissue disease (such as Marfan’s disease)
Infection (such as mycotic aneurism)
What are some risk factors for degenerative abdominal aortic aneurism?
Male sex
Age
Smoking
Hypertension
Family history
What is the prevalence of abdominal aneurysm in the UK?
3%
What can be said about abdominal aneurysm always presenting with symptoms?
It often does not have any presentations and so is asymptomatic
What is used to detect dangerous swelling of the aorta?
Abdominal aortic aneurysm screening
When are men invited to abdominal aortic aneurysm screening?
When they turn 65
What is the criteria for screening to be used in general?
Definable disease
Prevalance
Severity of disease
Natural history
Reliable detection
Early detection confers advantage
Treatment options are available
Cost
Feasibility
Acceptability
What are the potential outcomes for screening?
Normal aorta (discharged)
Small abdominal aortic aneurysm, 3-4.4cm (invited for annual ultrasound)
Medium abdominal aortic aneurysm,4.5-5.5cm (incited for 3 monthly ultrasound scan)
Large abdominal aortic aneurysm, >5.5cm
What is classified as a small abdominal aortic aneurysm?
3-4.4cm
How often do people with a small abdominal aortic aneurysm getting an ultrasound?
Once a year
What is classified as a medium abdominal aortic aneurysm?
4.5-5.5cm
How often do people with a medium abdominal aortic aneurysm get an ultrasound?
Once every 3 months
What is classified as a large abdominal aortic aneurysm?
More than 5.5cm
What is the presentation of abdominal aortic aneurysm when it is impending rupture?
Increasing backpain
Tender abdominal aorta
What is the presentation of abdominal aortic aneurysm once it has ruptured?
Abdominal/back/flank pain
Painful pulsatile mass
Haemodynamic instability
Hypoperfusion
What are some unusual presentations of abdominal aortic aneurysm?
Distal embolism
Aortocaval fistula
Aortoenteric fistula
Ureteric occlusion
Duodenal obstruction
What are questions to ask when deciding how to manage an asymptomatic patient?
Is the aneurysm a size to consider repair?
Is the patient a candidate for repair?
Is the aneurysm suitble for endovascular or open repair?
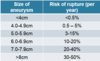
How does the risk of rupture change with aneurysm size?
It increases
What is patient fitness determined by?
Full history and examination
Bloods
ECG
ECHO
Pulmonary function tests (PFT)
Myocardial perfusion scan (MPS)
Cardiopulmonary exercise testing
End of the bad test
Patient preferance
What does ECHO stand for?
Echocardiogram
What is an echocardiogram (ECHO)?
Ultrasound used to make pctures of heart valves and chambers
What is an ultrasound used to make pctures of heart valves and chambers called?
Echocardiogram
What does PFTs stand for?
Pulmonary function tests
What are pulmonary function tests?
Non-invasive tests that show how well the lungs are working
What are non-invasive tests that show how well the lungs are working called?
Pulmonary function tests
What does MPS stand for?
Myocardial perfusion scan
What is a myocardial perfusion scan?
Uses radioactive substance to show blood flow to the heart
What uses radioactive substance to show blood flow to the heart?
Myocardial perfusion test
What does CPEX stand for?
Cardiopulmonary exercise testing
What is cardiopulmonary exercise testing?
Tests the function of the heart and lungs as a combined unit
What tests the function of the heart and lungs as a combined unit?
Cardiopulmonary exercise testing
What is used to determine if the aneurysm is suitible for endovascular or open repair?
Ultrasound
CT/MRI
What are the advantages of ultrasound?
No radiation
No contrast
Cheap
What are the disadvantages of ultrasound?
Operator dependent
Inadequate for surgical planning
What are the advantages of CT/MRI?
Quick
Not operator dependent
Necessary for surgical planning (shows detailed anatomy)
What are the disadvantages of CT/MRI?
Contrast
Radiation
What are the treatment options of abdominal aortic aneurysm?
Conservative
Endovascular repair
Open repair
What is endovascular repair?
Using a small graft guided by an X-ray
What is open repair?
Large incision and then graft inserted
What are some potential consequences of open repair?
Wound infection
Bleeding
Pain
Scar
Damage to veins or nerves
What are some potential consequences of endovascular repair?
Wound infection
Bleeding
Pain
Scar
Contrast
Radiation
Endoleak
What is endoleak?
Persistant blood flow outside of the lumen of an endoluminal graft but within the aneurysm sac, caused by an incomplete seal of the aneurysm sac

Compare open vs vascular repair?
3 fold reduction in operative mortality for endovascular vs open
Improved quality of life initially with endovascular
Quality of life improvements lost with increase reintervention and surveillance for endovascular repair
No difference in overall mortality
What is the process of managing someone who is symptomatic?
ABCDE (first aid)
History, check records
Examination
Maybe coronary CT angiography
What does CTA stand up for?
CT angiography
What is a CT angiography?
CT along with intravenous contrast to obtain 3D pictures of the moving heart and great vessels
What can occur after a CTA in an emergency?
Emergency open repair or emergency endovascular repair
What should be remembered about exposure to abdominal aortic aneurysm patients?
It will be as an incidental finding through screening or sympomatic
What is the treatment as the aneurysm gets bigger?
Always curveillance until the abdominal aorta reaches 5.5 cm, then assess the patient for surgery and decide if open repair or endovascular repair
What is carotid disease?
Plaque builds up in the carotid arteries
What is atherosclerosis of the carotid arteries associated with?
Transient ischaemic attacks and ischaemic stroke
Who are the symptoms of stroke managed by?
Stroke teams
Who is involved with the management of carotid disease other than stroke teams?
Vascular surgeons to prevent further events
What does TIA stand for?
Transient ischaemic attacks
What is a transient ischaemic attack?
Focal CNS disturbance caused by vascular events such as microemboli and occlusion, leading to cerebral ischaemia, symptoms are less than 24 hours and there is no permanent neurological damage
What is focal CNS disturbance caused by vascular events such as microemboli and occlusion, leading to cerebral ischaemia, symptoms are less than 24 hours and there is no permanent neurological damage called?
Transient ischaemic attack
What is a stroke?
Clinical syndrome consisting of rapidly developing clinical signs of focal or global disturbance of cerebral function, symptoms lasting more than 24 hours or leading to death, with no apparent origin other than vascular
What is clinical syndrome consisting of rapidly developing clinical signs of focal or global disturbance of cerebral function, symptoms lasting more than 24 hours or leading to death, with no apparent origin other than vascular called?
Stroke
What are possible causes of stroke?
Cerebral infarction (84%)
Primary intracerebral haemorrhage (10%)
Subarachnoid haemorrhage (6%)
What can cause cerebral infarction?
Atrial fibrillation
Carotid atherosclerotic plaque rupture/thrombosis
Endocarditis
Myocardial infarction
Carotid artery trauma/dissection
Drug abuse
Haemotological disorder
What are some risk factors for carotid artery atherosclerosis?
Smoking
Diabetes
Family history
Male sex
Previous deep vein thrombosis
Hypertension
Hyperlipidaemia/hypercholesterolaemia
Obesity
Age
Are females or males more susceptible to carotid artery atherosclerosis?
Males
What does the diagnosis of carotid plaque involve?
History
Examination:
neurological
cardiac
auscultate carotids
Investigations
CT
carotid ultrasound scan
What investigations are used to diagnose carotid plaque?
CT
Carotid ultrasound scan
How does the velocity of blood change as the radius of a vessel changes?
As the radius decreases the velocity increases

What is the velocity of blood through the carotid at <50% stenosis?
<125cm/s
What is the velocity of blood at 50-69% stenosis?
>125 cm/s
What is the velocity of blood as 70-79% stenosis?
>270cm/s
What is the end diastolic velocity of blood at 80-99% stenosis?
End diastolic velocity
What does the mangement of carotid plaques involve?
Medical therapy
Carotid doppler
What does the medical therapy for carotid plaque involve?
Smoking cessation
Control of hypertension
Antiplatelet
Statin
Diabetic control
What is carotid doppler?
Imaging test that uses ultrasound to examine the carotid arteries
How is the brain still perfused even if the carotid arteries are blocked?
Circle of Willis

When the carotid arteries are blocked, what is the further risk of stroke?
Emboli being showered from high velocity causing distal ischaemia
What is performed if the occlusion of the carotid artery is severe enough?
Carotid endarterectomy

What is an endarterectomy?
Surgical procedure to removed the atheromatous plaque material, or blockage in the lining of an artery
What is a surgical procedure to removed the atheromatous plaque material, or blockage in the lining of an artery?
Endarterectomy
What are some potential complications of endarterectomy?
General (wound infection, bleeding, scar, anaesthetic risks)
Nerve damage
Perioperative stroke
What is a treatment option for carotid plaques other than endarterectomy?
Stenting
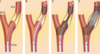
What is stenting?
Insertion of a small mesh tube to treat weak arteries and restored blood flow through a narrow or blocked artery
What is insertion of a small mesh tube to treat weak arteries and restored blood flow through a narrow or blocked artery called?
Stenting
What is NNT?
Number of patietns needed to treat to prevent 1 additional bad outcome
How does the NNT for stenting change with time?
Increases exponentially (is 5 for within 2 weeks but 125 for longer than 12 weeks)

What does CEA stand for?
Carotid andarterectomy
What is the management for asymptomatic patients with carotid plaque?
CEA should be considered when high grade stenosis
CEA may be of more benefit for males patients <70 years
CEA should only be performed by operators with a low (<3%) perioperative stroke or death rate
When should carotid surgery be offered to all symptomatic patients?
When stenosis is >70%

