Chemical Mediators of Inflammation II Flashcards
(12 cards)
What connects the coagulation system with the inflammatory response system?
Factor XII: Hageman Factor. IT is associated with coagulation, with anti-microbial actions, and with inflammation.

How does Factor XII act in coagulation?
Factor XII is activated by vascular damage which increases vascular permeability, causes endothelial damage, and exposes extracellular collagen, activating platelets. Factor XII changes to XIIa which is the start of the coat. pathway that includes thrombin and fibrin. This promotes the production of prostaglandins, cytokines, PAF, and nitric oxide.
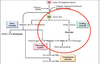
How does Factor XII lead to anaphylaxis?
Either through the Kallikrein pathway or the Fibrinolytic pathway. Pre-Kallikrein -> kallikrein -> Bradykinin -> C5a (compliment protein C5 product) which is an anaphylatoxin. Fibrinolytic pathway: Plasminogen -> Plasmin -> Fibrin -> C3a an anaphylatoxin

What are some functions of complement?
Anaphylaxis (C3a, C5a), inflammation (C3a, C5a), phagocytosis (C3b, iC3b), cell lysis. Complement is inactivated by C1 esterase inhibitor (C1-inh).
What is kinin/bradykinin and how does its system work?
Kinin is a protein derived from kininogens, activated by kallikrein proteases. It functions in vasodilation, increases vascular permeability, and causes bronchial smooth muscle contraction and pain.
What is required for to produce anaphylatoxins?
Factor XII is activated, leading to the activation of the kinin system, that then leads to the cleavage of complement proteins C3 and C5, producing the anaphylatoxins C3a and C5a.

What is the overall process of inflammatory response?
Injury -> vascular damage -> edema -> PMN/neutrophil invasion -> macrophage.
What is the process of PMNs responding to injury?
No neutrophils in tissue, must cross from blood stream - endothelial cell activation -> P, E selectins -> slowing and binding of neutrophils -> diapedesis through vascular wall. PMN mediation through inflammatory mediators, expressed by endothelia
What is the process of macrophages responding to injury?
Macrophages are already present in the tissues. Require inflammatory mediators to activate their processes.
Summarize the inflammatory mediators
Chemical mediators create a complex interplay of various microbial/tissue based content and specific chemicals/mediators in inflammation. They can be produced locally at the site of inflammation or systemically (by the liver). Their effects are to promote and modulate inflammation, promote repair, alert body to the problem and cause the acute phase response.
How is the liver signalled to create systemic inflammatory mediators?
PMNs and macrophages at the site of the inflammation secrete IL-1, IL-6, TNF-a, IFN-g, TGF-b which trigger the liver to produce its systemic mediators.

What is one goal of the systemic response chemical mediators during the acute phase reaction?
Stimulation of white blood cell creation. These signals include GM-CSF (granulocyte/macrophage colony stimulating factor) interleukins, stem cell factors, stromal cell derived factor. Overall effect is to increase WBC count.



