CVS S7 - The ECG Flashcards
(38 cards)
Describe the spread of excitation through the heart
You should be able to draw a diagram of this
Activity starts at the SAN and depolarisation spreads over the walls of the atria to the AVN
At the AVN there is a 120ms delay
Excitation then spreads down the septum through the bundle of His and the left and right bundle branches then out over the ventricular myocardium
Excitation through the myocardium progresses from the endocardial to epicardial surface, at this point, the entire ventricle is depolarised
There is a delay before ventricular repolarisation of 280ms
Repolarisation spreads in the opposite direction to depolarisation, from epicardial to endocardial surface
What would an extracellular electrode placed near a myocardial cell see during each contraction?
Why does this differ from what an intracellular electrode sees?
Sees only two signals for each action potential/systole:
- One for depolarisation
- One for repolarisation
Electrodes outside the cell only record CHANGES in membrane potential
How does what an electrode see depend on the direction of depolarisation and repolarisation?
If depolarisation is spreading:
- Toward electrode then upward signal
- Away from electrode then downward signal
If repolarisation is spreading:
- Toward electrode then downward signal
- Away from electrode then upward signal
What determines amplitude of signal seen by an extracellular electrode?
Amplitude is larger when:
- There is more muscle depolarisaing/repolarising
- The spread is at a smaller angle to the electrode view (largest when directly towards/away)
What are the different waves found on an ECG and what electrical events do they correspond to?
P wave - Atrial depolarisation
Q wave - Septal depolarisation spreading to ventricles
R wave - Main ventricular depolarisation
S wave - End ventricular depolarisation
T wave - Ventricular repolarisation
Describe how the P wave’s form is produced
What happens following the P wave?
Atrial depolarisation produces a small upward deflection
Small and upward because it’s moving toward the electrode, but not directly
Following the P wave:
- 120ms delay before QRS complex
Describe how the Q wave’s form is produced
Depolarisation spreads down the septum then out across the axis of the heart, producing a small downward deflection
Small and downward because it’s away from the electrode, but not directly
Describe how the R wave’s form is produced
Depolarisation spreads thorough the ventricular muscle along an axis slightly left of the septum producing a large upward deflection
Large and upward as there’s lots of muscle and depolarisation is moving directly toward the electrode
Describe how the S wave’s form is produced
What happens directly after the S wave?
Depolarisation spreads up the ventricles towards the atria producing a small downward deflection
Small and downwards as it’s moving away from the electrode, but not directly
Afterwards, there is a delay of 280ms before the T wave
Describe how the T wave’s form is produced
Repolarisation spreads from epicardial to endocardial surfaces producing a medium upward deflection
Upward because repolarisation is moving away
Medium sized because repolarisation timing in different cells is dispersed
Label each of the black boxes
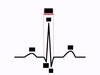
From left to right
P wave
Q wave
R wave
S wave
T wave
At the top:
QRS complex
Where is atrial repolarisation on an ECG trace?
It can’t be seen as it gets lost in the QRS complex
Describe how the R wave would change if an electrode is moved around the heart
Viewing directly in line with the cardiac axis results in a large upward deflection
Viewed at a 90 degree angle to the cardiac axis there is no signal
Viewed at a 180 degree angle sees a large downward deflection
Varies predictably between these points
How many electrode comprise are involved in a normal ECG reading?
How many are recording?
Where are these electrodes? (In the broadest of terms)
10 electrodes in a 12 lead ECG
9 recording, right lower limb is neutral
4 Limbs
6 Chest
Where are each of the limb electrodes placed?
Red - Right upper limb
Yellow - Left upper limb
Green - Left lower limb
Blue - Right lower limb
What are all the limb leads called?
State the equivalent single electrode views of all the leads
All veiwing the heart in the coronal plane, all angles given relative to Lead I, which views the heart directly from the left
Lead I - 0 degrees
Lead II at +60 degrees
Lead III at +120 degrees
aVL at -30 degrees
aVR at -150 degrees
aVF at +90 degrees
What are the limits of the normal cardiac axis?
Between aVL and aVF ( -30 to +90 degrees)
Describe the placement of each of the chest electrodes
V1 - Right 4th intercostal space next to the sternum
V2 - Left 4th intercostal space next to the sternum
V3 - Directly between V2 and V4
V4 - 5th intercostal space along the left midclavicular line
V5 - Level with V4 at the left anterior axillary line
V6 Level with V5 along the left midaxillary line (directly under the midpoint of the armpit)
What leads correspond the the chest electrodes?
What views do they provide?
Leads correspond to each electrode (V1, 2, 3, 4, 5, 6)
They provide horizontal views of the heart
Describe how leads are amplified
One electrode is used as positive
One is negative (can be directly opposing positive or offset)
Negative signal is inverted and the signals are combined
The signal is then amplified further
If the negative as opposing positive, we get an amplified view directly from the positive (E.g. Lead I)
If the negative was offset we get and amplified view from between the positive and equivalent positive of the negative (directly opposite the negative) (E.g. Lead II and III)
Label each of the black boxes with the corresponding limb lead, include degrees offset from Lead I

Starting from the lead directly to the left and going clockwise
Lead I at 0 degrees
Lead II at +60 degrees
aVF at +90 degrees
Lead III at +120 degrees
aVR at -150 degrees
aVL at -30 degrees
How do you calculate a regular heart rate from an ECG?
Where do you read this rate from?
All ECG machines run at a standard rate of 300 small squares per minute
To find the rate, divide 300 by the number of squares in the R -R interval.
The rate is commonly read from the ‘rhthym strip’ but can be read from any lead
How would you calculate an irregular rhythym from an ECG?
A larger interval is used than a single R- R interval
For example, multiply the number of beats in 10 seconds by 6
What are ventricular ectopic beats and how do they present in an ECG?
Ventricular cells that gain pacemaker capability can cause ventricular contraction before underlying rhythym depolarises the ventricles, the ectopic beat
The resultant ECG often appears wider and taller than the underlying rhthym
May occur every other beat, every third beat, every fourth beat etc. or in couplets or triplets.


