what is the initial injury that triggers the immune response in a transplant?
ischemia-reperfusion injury
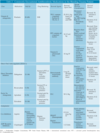
Describe the mechanism of ischemia-reperfusion injury
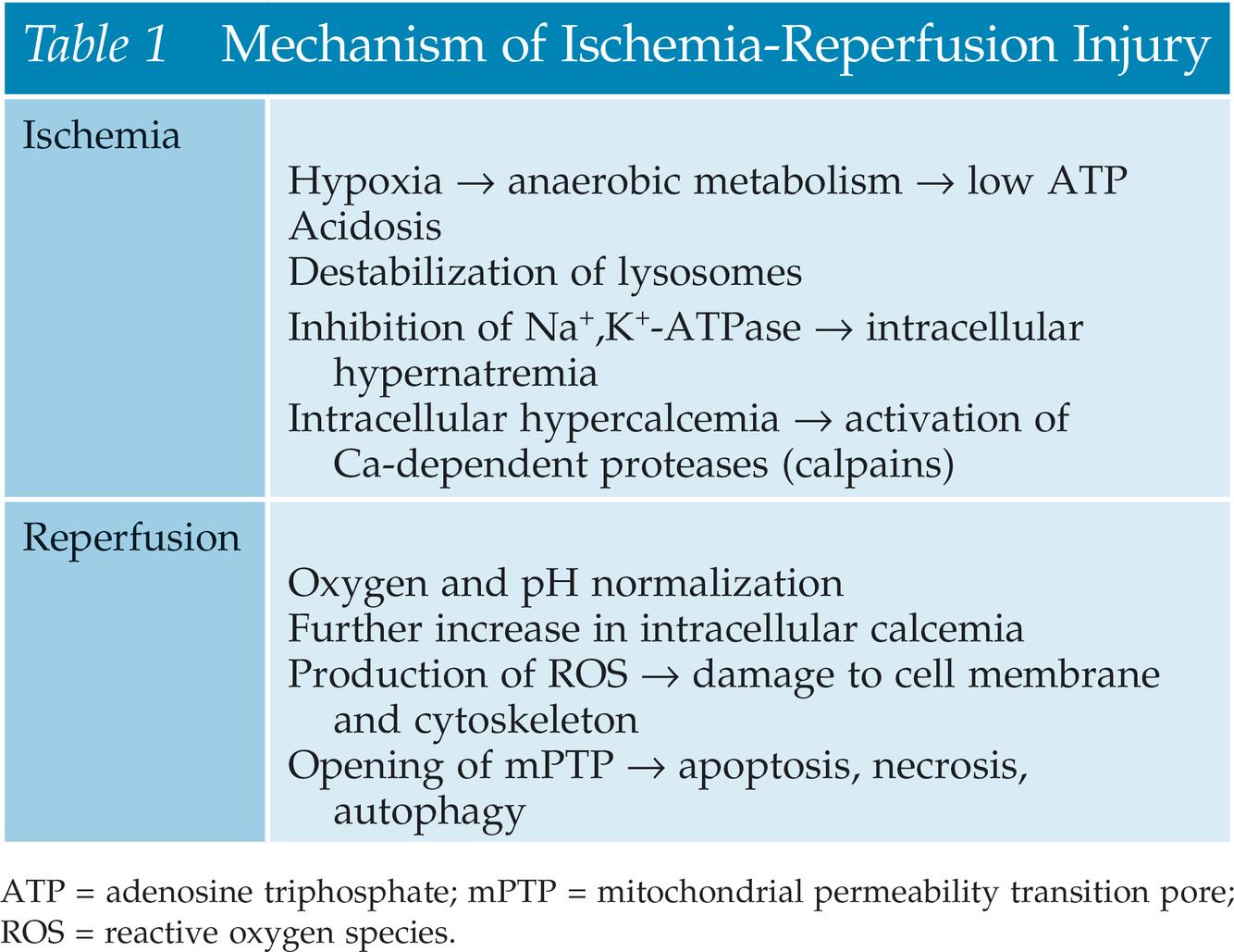
Is ischemia-reperfusion injury worse in deceased or living donor transplants? Why?
deceased, brain death is associated with upregulation and activation of the complement cascade as well as generalized ischemia 2/2 activation of the sympathetic system in its attempt to increase cerebral perfusion pressure
What are some ways that the donor graft can be damaged during harvesting?
- warm ischemia time (after vessel clamping)
- cold ischemia time (after refrigeration)
- manipulation of the graft
Why are HLA proteins central in the discussion of alloantigens when speaking of transplant rejection?
they are highly polymorphic, widely expressed, and capable of eliciting a uniquely large polyclonal T cell response
Describe class 1 HLAs
- expressed by most of the nucleated cells
- can only be recognized by CD8 coreceptors
- present intracellular peptides (including viruses/bacteria)
Describe class II HLAs
- present extracellular antigens to T cells
- are present on APCs
- recognized only by CD4 coreceptors
What other alloantigens in the immune system (other than HLA) can cause rejection despite identical HLA complex genes?
minor histocompatibility antigens
Know this schematic: APC and T cell interaction and the anti-rejection med targets
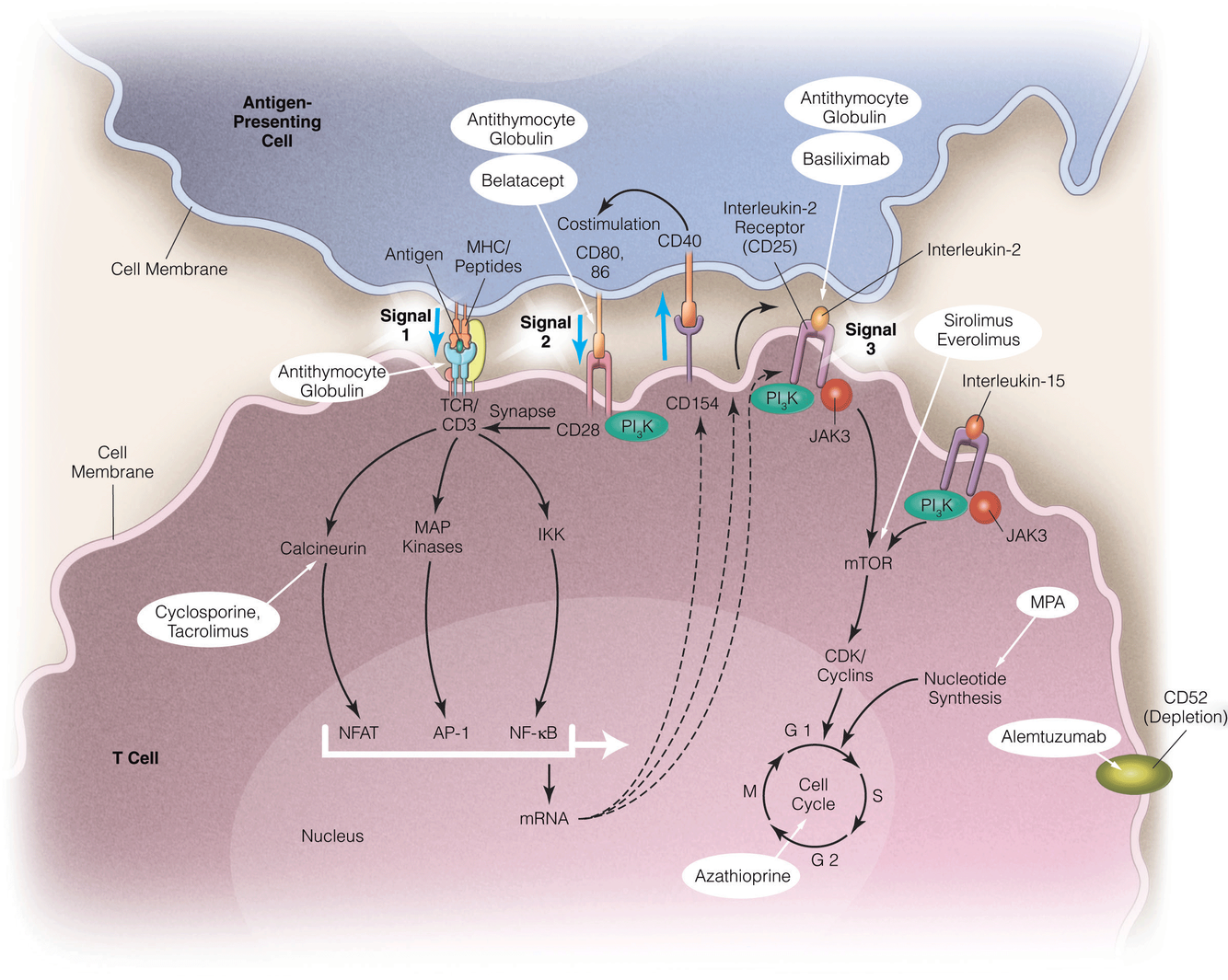
What are the different categories of methods of presentation of APVs to recipient T cells?
direct, indirect, semi-direct
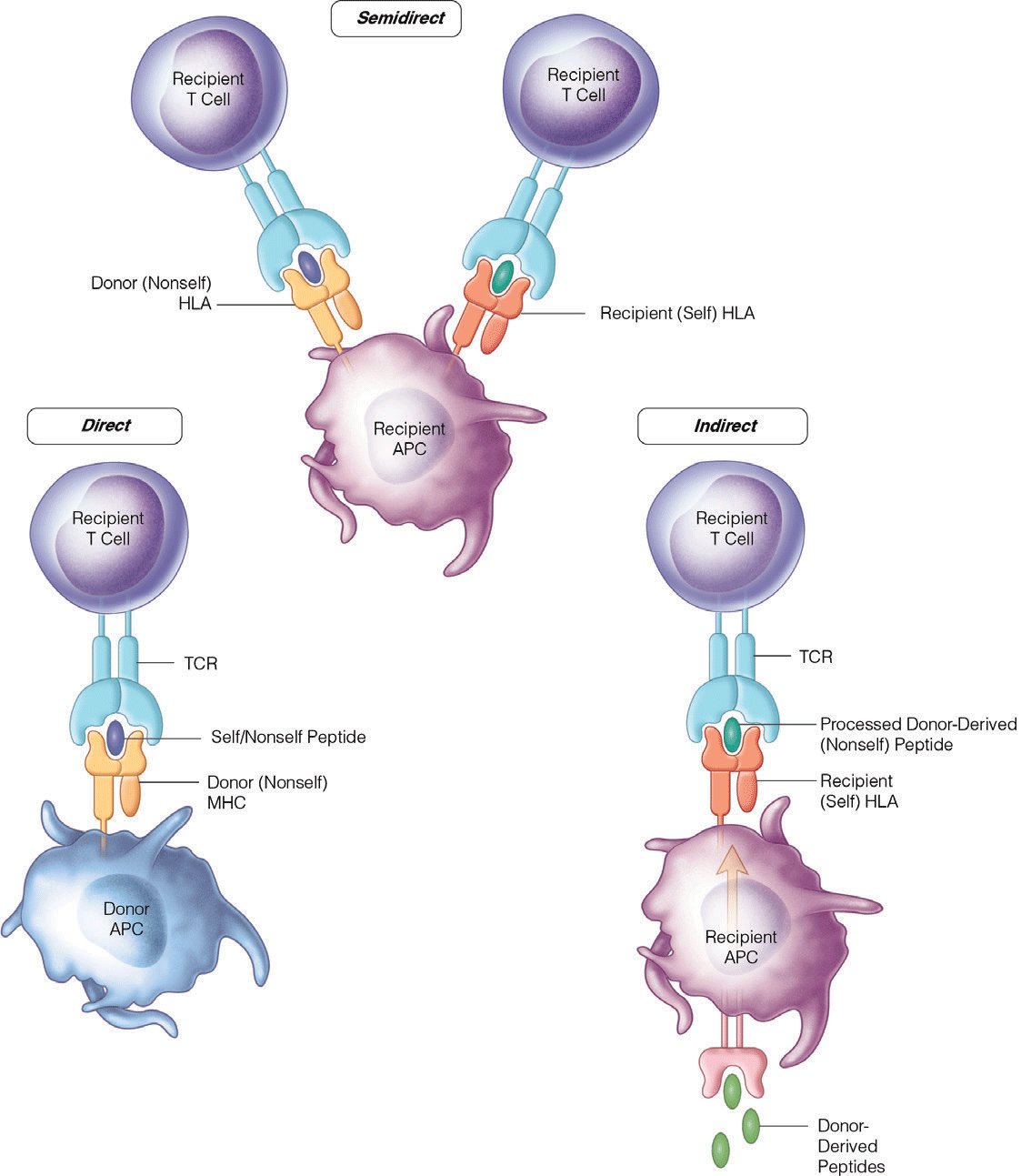
What major cell line makes up adaptive immunity? How do they contribute to rejection?
T cells
- defined broadly by surface markers CD4 or CD8
- T helper 1s (CD4) produce IL-2, which proliferates CD8 Ts
- T helper 2s produce other ILs, active B cells and eos
- CD8 Ts can directly induce allograft cell death
- T(reg) cells can suppress other T activation
- Memory Ts produce cytokines faster
What major cells are present in innate immunity? What are their functions?

What is the leading cause of death in patients under the age of 45?
trauma
What is the number one cause of death in the first hour of trauma?
hemorrhage
- nearly 40% of trauma deaths are 2/2 hemorrhage
- In the Prospective, Observational, Multicenter, Major Trauma Transfusion (PROMMTT) study the median time to hemorrhagic death was only 2.6 hours.
What should the pre-hospital fluid resuscitation be like for penetrating trauma patients?
Patients with penetrating injuries, who received very little fluid resuscitation until they reached the operating room (OR) had a higher rate of survival than patients who were resuscitated in the prehospital phase and in the trauma bay.6 Additionally, they had fewer complications and shorter lengths of stay.
What is the pre-hospital recommendation on tourniquet use?
all law enforcement, fire, and emergency medical services, and concerned citizens be supplied with and trained on how to apply tourniquets
low rate of complications, but attention must be paid to tourniquet time
How do you assess airway in trauma patients?
- ask their name
- assume spine instability until exam done
- can do chin lift/jaw thrust while maintaining inline stability
- maintain stability while intubating
Describe the use of medication in RSI?
- no bag-mask (inc risk of aspiration)
- administer rapid induction agent, then NMB, then ETT
- best meds are fastest w/ short duration w/o HDS fx
- ex: etomidate 2-3 mg, succ 100 mg vs roc 70 mg, ETT
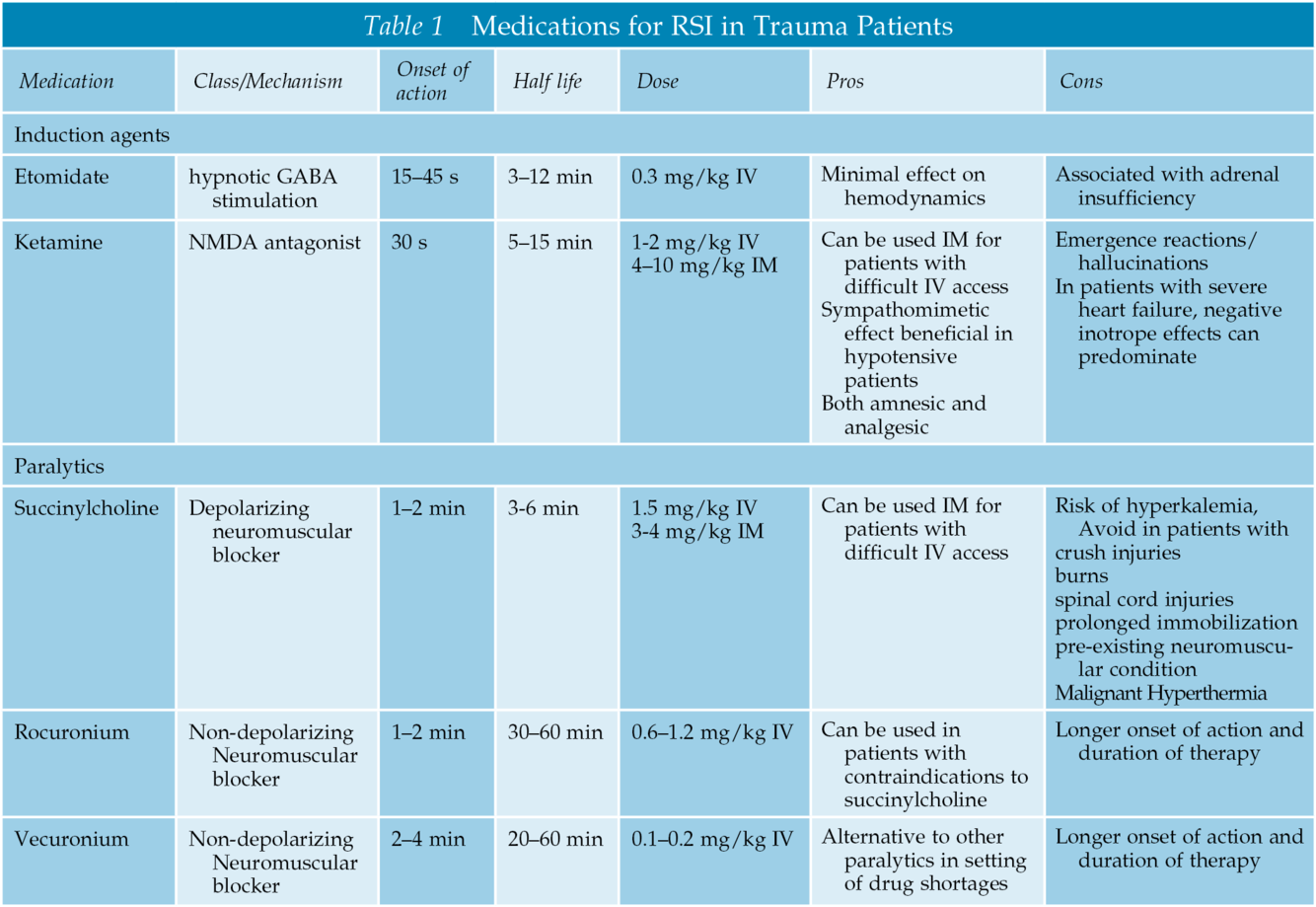
How do you manage a difficult airway in the trauma bay?
- be prepared and well stocked
- anticipate in head, neck, face trauma
- stock: suction x2, oropharyngeal airway, nasal cannula, laryngoscopes, multiple ETT sizes 5-8, LMA, bougie, tape, cricothyroidotomy kit
- prep for surgical airway if difficulty intubating and oxygenating
How do you perform a cricothyroidotomy?
- as long as you can mask, you can re-attempt ETT
- longitudinal incision at cricothyroid membrane
- incise membrane transversely
- spread membrane
- small ETT (5 or 6) should be placed through the incision
- ensure location in trach w/ ET CO2, ensure not mainstem w/ BL breath sounds
- secure the tube in place w/ tape and note the level of insertion at teeth
- look for your tube in CXR
How do you assess breathing in a trauma patient?
- look: symmetrical chest rise, gross trauma
- listen: bilateral breath sounds
- feel: crepitus
Diagnose tension pneumothorax?
- clinical
- absent breath sounds on one lung
- tracheal deviation
- hypotension
- no need for XR to confirm before management
How do you manage tension PTX?
- needle decompression vs tube thoracostomy depending on skill and staff
- needle: 2nd intercostal space at mid-clavicular line, convert to tube thoracostomy for definitive mgmt
- tube: 4-5th intercostal space at mid-axillary line, place posteriorly and superiorly
- do not place chest tubes through existing wound
How do you assess circulation in the trauma patient?
- check pulses in all extremities
- measure blood pressure
- obtain access
- manage hemorrhage






