Abdomen - Hernia Flashcards
(49 cards)
In a patient with an abdominal bulge, be able to determine whether a hernia is present and the type of hernia. In addition, be able to distinguish between abdominal wall hernias and diastasis recti.
- A ventral hernia is a defect in the abdominal wall fascia with protrusion of abdominal or preperitoneal contents.
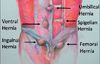
- Spontaneously occurring midline hernias: epigastric hernias (located between the xyphoid and umbilicus), umbilical hernias (located at the umbilicus), and hypogastric hernias (located below the umbilicus). Spigelian hernias occur off of midline and lateral to the rectus in the lower abdomen (between the iliac crest and 6 cm cephalad to the iliac crest).
- Incisional hernias occur at the location of prior surgical incisions.
- Diastasis recti is not a true hernia but rather stretching of the linea alba with bulging at the medial edge of the rectus muscle.

Be able to distinguish between indications for emergent and elective operative intervention for ventral hernias.
- Emergent:
- Acute incarceration w/ inability to reduce hernia
- Hernia content strangulation
- Bowel obstruction with signs of bowel ischemia
- Leakage of ascites through skin in pt w/ cirrhosis
- Elective:
- Pain or discomfort
- Hi risk for obsx: chronic incarcx, intermittent incarcx
- Interference with daily activities or quality of life
Identify contraindications to operative ventral hernia repair
- Relative contraindications:
- Obesity
- Active tobacco use
- Pregnancy
- Poor surgical candidate with multiple comorbidities
- Absolute contraindications
- Inability to withstand general anesthesia if required
In regards to hernias, be able to determine clinical factors that would favor laparoscopic versus open repair
Factors that favor laparoscopic repair are smaller defects, older age, and lack of need to reapproximate the linea alba.
Factors that favor open repair are larger defects, multiple prior operations with concern for dense adhesions not amenable to laparoscopic lysis of adhesions, and inability to tolerate pneumoperitoneum.
Name the layers of the abdominal wall
Encountered laterally from anterior to posterior:
- Skin
- Subcutaneous tissue
- Camper and Scarpa fasciae
- External oblique muscle
- Internal oblique muscle
- Transversus abdominis muscle and aponeurosis
- Transversalis fascia
- Preperitoneal fat
- Peritoneum
Describe the appropriate perioperative patient positioning, and prophylaxis in a patient undergoing ventral hernia repair (open or laparoscopic).
- Open procedure: supine with arms out.
- Laparoscopic procedure: supine with arms tucked.
- SCD stockings for VTE ppx w/ chemoproppx as indicated by patient/surgical risk factors.
- Appropriate abx within 1 hour of incision.
- Gram + coverage is sufficient for a clean case (ancef).
- If a longer duration case is anticipated or the operative field includes the space of Retzius (retropubic space), a Foley catheter should be placed.
To obtain informed consent, describe the relevant risks, benefits, and alternatives to operative intervention for ventral hernia repair.
- Risks: bleeding, wound infection, mesh infection if mesh is used, injury to surrounding structures including bowel, port site hernia if repaired laparoscopically, hernia recurrence, seroma, chronic or persistent pain, skin necrosis, and abdominal compartment syndrome.
- Benefits: fixing the hernia defect, decreasing risk of future incarceration or strangulation, and potential for decreased pain.
- Alternatives: abdominal binder or abdominal support.
Be able to discuss the recurrence rate of primary repair versus mesh repair for ventral hernias.
- Small primary (≤ 2-3 cm) w/ suture repair: 5% to 7%.
- Larger primary (> 2-3 cm) w/ suture repair: 10% and 50%.
-
Incisional hernias w/ suture repairs: 10% to 50%
- Recurrence decreases by > 50% w/ mesh.
- Risk factors for recurrence: smoking, obesity, DM, immunosuppression, malnutrition, corticosteroids, chemotherapy/radiation, and CTDs.
In a patient with an infected prosthetic mesh, be able to describe the criteria for operative intervention.
- Nonoperative management: antibiotics and local wound care.
- Mesh infections involving macroporous mesh made from polypropylene or polyester may be treated with local measures, mesh removal may be required.
- Nonoperative strategies unlikely to be successful in treating microporous or polytetrafluoroethylene (PTFE) prosthetic infections.
- Failure of nonoperative management is demonstrated by ongoing signs and symptoms of mesh infection.
In an open ventral hernia repair, decide on the material and location for mesh placement.
- Options: underlay (retrorectus, pre vs intraperitoneal), sublay, inlay (mesh placed as a bridge between the fascial edges), or onlay (mesh placed above the fascia).
- ideal: preperitoneal, sublay, fascia closed
- Intra-peritoneal mesh needs non-adhesive barrier
- Options: polyester, polypropylene, and PTFE vs biologic
- Prosthetics: macro- or micro-porous (macro resists infection)
- Biologic meshes can be cross-linked or non–cross-linked.
- Several synthetic absorbable meshes are now available
- Biologic and synthetic absorbable meshes: contaminated fields to decrease the risk of long-term mesh infections.
Describe the approaches to component separation to gain additional mobilization of the abdominal wall.
- Approaches to component separation: anterior release, posterior release, transversus abdominis release (TAR), separation of internal obl and transversus.
- Anterior release: creation of subcutaneous flaps, division of the external oblique aponeurosis lateral to the semilunar line, and development of the plane between the external oblique aponeurosis and the internal oblique muscle laterally. Mesh reinforcement can be placed in an underlay or overlay position.
- Posterior release: opening the retrorectus space medially and creating the posterior plane between the rectus muscle and the posterior rectus sheath. The posterior rectus sheath is incised again medial to the laterally perforating neurovascular bundles. The underlying transversus abdominis muscle can be divided (TAR), and dissection is carried laterally to mobilize the transversalis fascia and peritoneum off of the overlying muscle.

In a laparoscopic ventral hernia repair, describe the principles of port size and location of placement.
- Ports should be placed well laterally to the location of the hernia defect to allow appropriate working space and placement of mesh.
- Ports (5 mm) can be used for laparoscopic instruments and the tacking device. A 10- to 12-mm port is often needed for mesh insertion.
In a laparoscopic ventral hernia repair, decide on the appropriate mesh size and describe the appropriate sequence in mesh fixation to the anterior abdominal wall.
- Defect is measured intraperitoneally for most accuracy. Use spinal needles through the abd wall along defect edge w/ a ruler intra-abd.
- Mesh size: allow for a 3- to 5-cm overlap on all sides.
- Mesh orientation/fixation: transfascial sutures placed in the four quadrants of the mesh prior to insertion, or use a mesh deployment/positioning device.
- Mesh tacking: transfascial sutures brought through the abd wall, mesh tacked in at 1-cm intervals along the edge, then a second inner row of tacks is placed.
In a patient with an infected prosthetic mesh, be able to describe the key steps of the operative procedure.
- Incision and gaining access to the peritoneal cavity
- LoA: free intra-abdominal contents from mesh, gain working room laterally
- Removal of infected mesh and non-absorbable sutures
- Assessment of ability to close fascia or need for component release
- Closure of the abdominal wall with or without the aid of a biologic mesh
During an open ventral hernia repair, assess the tension on the abdominal wall
The ability to close the fascia can be assessed by grasping the fascial edges on each side with Kocher forceps and pulling the fascial edges to the midline.
Abdominal compartment syndrome is indicated by end-organ dysfunction, including impaired ventilation, cardiac output, and renal function. Intraoperatively, the risk of abdominal compartment syndrome may be indicated by increased peak ventilator pressures when closing the abdominal wall.
During ventral hernia repair in a contaminated field, describe the strategies of repair and expected outcomes.
- Repair of enterotomy includes primary repair for a smaller or single enterotomy or bowel resection with primary anastomosis for larger or multiple enterotomies.
- Strategies for abdominal wall closure include primary closure, placement of absorbable mesh, or placement of biologic mesh (NOT synthetic non-absorbable)
Describe potential complications after ventral hernia repair
- Complications include ileus, postoperative pain, sepsis, intestinal obstruction or fistualization, necrotizing soft tissue infection, seroma formation, hernia recurrence, and mesh infection.
- Recurrence rates range from 0% to 30% for prosthetic repairs.
- Factors that increase the risk of prosthetic mesh infections include presence of infection prior to surgery, skin ulceration over hernia, enterotomy during hernia repair, obesity, and incarcerated or obstructed bowel within the hernia.
Describe the spectrum of clinical manifestations of an infected prosthesis.
- Systemic: fevers, chills, leukocytosis, tachycardia, and hypotension.
- Sugrical site infection: erythema, purulent drainage, and chronic sinus tracts.
- Imaging and diagnostic findings: contrasted CT scan demonstrating fluid collection, with signs of infection including rim enhancement and gas, as well as positive culture from surgical site fluid collection in continuity with mesh.
- It is important to note that patients can develop postoperative seromas or fluid collections that are not infected, and both clinical examination findings and diagnostic maneuvers are required to differentiate between infected and noninfected fluid collections.
A 58-year-old chronic alcoholic has an umbilical hernia and ascites of recent onset. He has never been treated with diuretics or salt restriction. On examination, he has massive ascites with a large umbilical hernia, with thin skin at the apex. There is a slow ooze of clear, odorless fluid from the hernia. Therapy now should be:
Bedrest, IV abx, aggressive diuresis, hernia repair during this admission
- Leaking abdominal ascites is urgent and requires aggressive management.
- Admit pt: risk of bacterial peritonitis and/or hernia rupture.
- Repair in cirrhotics w/ uncontrolled ascites: high M/M - 8.3%, 16.6%
- Control the ascites prior to repair: diuresis, sodium, fluid restriction
- Bedrest: remove undue strain on the weak and leaking site
- Intravenous antibiotics: prevent bacterial peritonitis
- If operation must be undertaken emergently (true rupture), or diuretic therapy fails to control the ascites, combined umbilical herniorrhapy with a peritoneal-venous shunt can achieve a stable repair with relatively low morbidity.
Epidemiologic information about umbilical hernias: men vs women, incarceration, content, spontaneous closure, association w/ ascites
- Umbilical hernias are common - just as common if not more than incisional
- More common in women than men (3:1)
- Present more commonly with incarceration in men
- Content is usually pre-peritoneal fat or omentum.
- Spontaneous closure in children under 5 and pregnant patients.
- Persistent hernia beyond 5, sx hernias s/p delivery - repair
- Associated w/ ascites - repair for rupture, redness/ulceration of skin, incarceration.
- If a patient has ascites and a non-incarcerated hernia - address the ascites.
Describe rectus sheath anatomy in reference to the arcuate line
Above the arcuate line, the posterior rectus sheath is composed of the posterior lamella of the internal oblique aponeurosis with the transversus abdominis muscle and aponeurosis.
Below the arcuate line, there is no posterior sheath.
Describe the composition of the linea semilunaris and linea alba
The aponeurosis of the external oblique, internal oblique, and transversus abdominis fuse lateral to the rectus muscle to form the linea semilunaris and medial to the rectus muscle to form the linea alba.
Describe the relationship between the major muscles with their blood and nerve supplies.
- The nerves to the lateral muscles and rectus abdominis arise from the seventh through twelfth intercostal nerves and first and second lumbar nerves.
- Run in a plane between the internal oblique muscle and the transversus abdominis and pierce through the lateral rectus sheath.
- Blood supply to rectus muscles: superior epigastric artery, internal thoracic artery, inferior epigastric artery, lower intercostal arteries.
- Blood supply to lateral abdominal wall muscles: lower three to four intercostal arteries, the deep circumflex iliac artery, and the lumbar arteries.
Indications for surgery in a spigelian hernia
lower abdominal wall swelling, pain lateral to the rectus abdominis muscle, and small bowel obstruction