GI Part I (Pre-Midterm) Flashcards
(87 cards)
Your favorite snack while hiking is trail mix. This mix contains salty peanuts, sweet dried fruit and chocolate bits. You can enjoy the various flavors in this snack because the neuroepithelial cells in the taste bud:
Choices:
- have five receptor genes and each one encodes receptors for sweet, sour, bitter, salt and umami.
- extend their axons directly to the ventral posteromedial nucleus in the thalamus.
- synapse with pseudounipolar neurons in the facial nerve, glossopharyngeal or vagus nerves.
- phagocytose bits of ingested food for processing in secondary lysosomes.
- exchange ions between cells via gap junctions and therefore respond as a syncytium.
- synapse with pseudounipolar neurons in the facial nerve, glossopharyngeal or vagus
Explanation:
- Have five receptor genes and each one encodes receptors for sweet, sour, bitter, salt and umami. is incorrect because salt and sour tastes are activated by ion channels, not receptors.
- Extend their axons directly to the ventral posteromedial nucleus in the thalamus. is incorrect because the neuroepithelial cells do not extend into the CNS like olfactory cells do.
- Exchange ions between cells via gap junctions and therefore respond as a syncytium. is incorrect because the cells respond individually, not as a syncytium.
Which ionic component of saliva is most likely to be higher in saliva than in its concentration in plasma when saliva is secreted at low rates (resting state)?
- Sodium (Na)
- Potassium (K)
- Chloride (Cl)
- Potassium (K)
Explanation:
Na and Cl are absorbed, but K is secreted into saliva.
When you smell freshly baked “Mom’s apple pie” which ions increase in concentration in your saliva?
- *Choices:**
1. Na and Cl
2. Na and K
3. K and Cl
- Na and Cl
Explanation:
At high flow rates the duct cells can’t reabsorb the Na and Cl fast enough to recover all of the ions from the
flow.
In an unfortunate surgical mishap, the vagal innervation of a patient’s lower esophageal sphincter is severed. The effect on esophageal function will be:
- *Choices:**
1. minimal because the vagus plays no role in esophageal function.
2. to disrupt control of the initiation of swallowing because the resting tone of the esophagus will be lost.
3. to induce gastric reflux since the resting tone of the lower esophageal sphincter will be lost.
4. to disrupt passage of food into the stomach because LES relaxation will be compromised.
5. rapid atrophy of the muscles of the lower one-third of the esophagus, resulting in decreased ability to protect the esophagus from stomach acid.
- to disrupt passage of food into the stomach because LES relaxation will be compromised.
Explanation:
LES relaxation is induced by activation of the vagus nerve, therefore loss of vagus innervation disrupts the ability to pass food into the stomach.
Where does the main pancreatic duct enter into the duodenum?
- *Choices:**
1. Ampulla of Vater
2. Ileocecal valve
3. Ligament of Trietz
4. Pyloric sphincter
- Ampulla of Vater

Thrombotic occlusion of the superior mesenteric artery would lead to infarction of which of the following GI organs?
Choices:
- Esophagus
- Large Intestine
- Liver
- Pancreas
- Small intestine
- Stomach
- Small Intestine
NOTE: After discussing it w/ Dr. Grahame, the colon could/would also be affected. The small intestine would be completely destroyed, though, so you can argue that it’s the “more correct” answer. That being said, Dr. Grahame said the question was unfair, so it will be removed/changed. (Our percentage breakdown on QStream also shows that most of us picked either small or large intestine.)
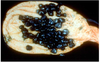
A 72-year-old male with a 5-decade history of smoking and chronic alcoholism has lost 15 kg over the past 3 months. Following a biopsy, an upper esophageal mass is resected and sent to pathology for examination.
Which one of the following clinical findings is most likely to be associated with the lesion shown above?
Choices:
- 30% 5-year survival
- Gastroesophageal reflux
- Progressive dysphagia
- Celiac lymph node metastases
- Past Epstein Barr virus infection

- Progressive dysphagia.
Explanation:
The pictures show a moderately to well differentiated squamous cell carcinoma. Esophageal carcinomas typically manifest with progressive dysphagia, initially with solids, then liquids; the correct choice is
- Progressive dysphagia. Additional clinical manifestations include odynophagia,, weight loss, hemorrhage following rupture, and pneumonias from aspiration or bronchoesophageal fistulas. The extensive infiltration of the wall is an adverse prognostic feature; the overall 5-year survival is 9%.
- An upper esophagus squamous cell carcinoma would most probably metastasize to cervical lymph nodes, mid-esophagus neoplasms to mediastinal, paratracheal or peribronchial lymph nodes, and those involving lower esophagus tend to involve gastric and celiac nodes. Plummer-Vinson syndrome, human papillomavirus infections, smoking and alcoholism are some risk factors or associations described in the literature.
Which one of the following is the most likely cause of adenocarcinoma of the esophagus?
Choices:
- Acid reflux
- Alcohol
- Human papilloma virus
- Lye ingestion
- Smoking
- Acid Reflux
Explanation:
Acid reflux is associated with gastric metaplasia which is considered precancerous and may lead to
adenocarcinoma of the esophagus. The other risk factors listed are associated with squamous carcinoma.
The condition that occurs lateral to the umbilicus, in which there is a failure of the abdominal wall to completely form, leaving portions of the viscera fully exposed to the amniotic fluid, is called
Choices:
- Gastroschisis
- Hirschprung disease
- Intussusception
- Meckel diverticulum
- Omphalocele
- Volvulus
- Gastroschisis
Explanation:
- Hirschprung’s disease (also known as congenital aganglionic megacolon) is caused by the incomplete migration of neurons derived from the primitive neural crest down the GI tract. The result is the absence ofganglion cells in distal regions such as the anal sphincter, compromising the ability to pass stool.
- Intussusception is the “telescope-like” invagination of a segment of intestine into the adjoining intestinal lumen.
- Meckel diverticulum is the most frequent congenital malformation of the GI tract. Essentially, it is a pouch-like structure located on the wall of the distal illium (~40-60 cm from the ileocecal valve) formed as a vestigial remnant of the omphalomesenteric duct (also called the vitelline duct or yolk stalk).
- Volvulus is a complete twisting of a loop of intestine around its mesenteric site of attachment.
- Omphalocele is the condition where there is failure of the intestinal loops to return to the abdomen during development. The viscera remain covered by the thin peritoneum-amnion membranes.
With respect to esophageal atresia (EA) and tracheoesophageal fistula (TEF), which one of the following conditions is least likely to require immediate surgical intervention?
Choices:
- TEF without EA
- EA without TEF
- EA with TEF to proximal esophagus
- EA with TEF to distal esophagus
- EA with TEF to both proximal and distal esophagus
- TEF without EA
Explanation:
Anything with EA needs to be corrected ASAP because there is no patent esophagus. If there is a EA with TEF, food and water (i.e., formula/milk) will have to enter the respiratory tract if it will ever make it to the stomach. IF there is no TEF but there is EA, then there’s no way of even getting into the stomach.
In the case of TEF without EA there are the expected separate paths to the stomach and to the lungs, but there’s also an additional connection. It will probably still need surgical intervention, but at least the child can breathe and eat.
http://2.bp.blogspot.com/_kE4lQ4oqHVc/S9BbqM53c1I/AAAAAAAAB4g/fwX2gTAQc7s/s1600/tea.gif
Explanation and link provided by 2LT Rayad Barakat USU Class of 2018.
The development of the gastrointestinal tract requires an epithelial-mesenchymal interaction for tube patterning into the different components. Which one of the following transcription factors is expressed in the endoderm and up-regulates expression of factors in the mesoderm (such as the HOX genes)?
Choices:
- NKX2.5 (NK2 homeobox 5)
- PAX2 (paired box gene 2)
- PITX2 (paired-like homeodomain 2)
- SHH (Sonic hedgehog)
- WT1 (Wilms tumor 1)
- SHH (Sonic hedgehog)
Explanation:
- NKX2.5 is responsible for the induction of the heart-forming region, is expressed in mesoderm and induced by endoderm (p169 Langman’s text). Mutations of NKX2.5 may produce atrial septal defects (ASDs) and other cardiac abnormalities.
- PAX2 is expressed in the metanephric mesenchyme and causes the mesenchyme to epithelialize during the development of the collecting ducts of the kidney. Mutations in the PAX2 gene may cause renal coloboma syndrome.
- PITX2 is involved in cardiac looping and is expressed in the lateral plate mesoderm of the left side. Mutations in the PITX2 homeobox gene are known to cause Axenfeld-Rieger syndrome (ARS).
- WT1 is expressed in the metanephric blastema and regulates the production of factors that stimulate growth and branching of the uteric buds. Mutations in WT1 may cause Wilms’ tumor.
Which of the following substances are the cells surrounding the asterisk most likely secreting?
Choices:
- Enzymes
- Ghrelin
- Mucus
- Serotonin
- Sodium

- Mucus
Explanation:
- Cells that compose the bulk of the acini are pyramidal or flask shaped (like an Erlenmeyer flask). The lumen of an acinus is quite small and usually difficult to see in the light microscope. Mucus-secreting cells are lightly stained with flattened nuclei pushed to the bottom of the cells. Their secretory products are Mucins, proteins that are heavily glycosylated and poor staining.
- Serous secreting acinar cells contain secretory granules that are often visible in the light microscope. Examples of serous secreting cells are visible above. They are frequently secreting Enzymes, such as in the pancreas. Cells actively involved in ion pumping (e.g. Sodium) often have regularly arranged mitochondria, e.g, striated ducts.
- Cells secreting Ghrelin and Serotonin would also have secretory granules that will stain with eosin but these cells tend to be found as singles or small groups in the GI tract.
The asterisk is in the lumen of a structure. This structure is most likely a/an
Choices:
- Excretory duct
- Intercalated duct
- Mucus-secreting acinus
- Serous acinus
- Striated duct

- Striated duct
Explanation:
- Examination of the indicated structure shows that the cells that make up the wall of the structure are regular cuboidal in shape. This suggests that we may be looking at a duct of some kind. In comparison, the cells that compose the bulk of the acini are pyramidal or flask shaped (like an Erlenmeyer flask). The lumen of an acinus is quite small and usually difficult to see in the light microscope.
- Mucus-secreting cells would be lightly stained with flattened nuclei pushed to the bottom of the cells. Serous secreting acinar cells contain visible secretory granules and some signs of this can be seen in the cells located at either sides of the indicated structure.
- If the structure is not part of the acinar component of the gland, then the choices are of various ducts. Excretory ducts are very large and generally have stratified layers of cells. This structure has a simple epithelium (one layer of nuclei). The lumen is about equivalent to the height of a cell, too large for a typical intercalated duct and there is evidence of lines radiating from the apical to basal aspect of the cells. These are the staining patterns of mitochondria that give the striated appearance of “striated ducts”.
Dental infections have been linked to an increased risk for all of the following conditions/diseases EXCEPT:
Choices:
- Asthma
- Cardiovascular disease
- Diabetes
- Endocarditis
- Pre-term low birth weight infants
- Asthma
Explanation:
- Dental infections are associated with an increased risk of each of the above except asthma.
- The correlation with cardiovascular disease is significant, however, a direct cause and effect relation has not yet been proven.
Which of the following recommendations applies to pregnant patients who seek dental care during pregnancy?
Choices:
- No dental treatment during pregnancy because it increases the risk for miscarriage.
- Treat acute periodontal problems during pregnancy to reduce risk for pre-term delivery.
- Do not debride (scale and root plane) until the 2nd trimester.
- Provide emergency dental care only.
- Treat acute periodontal problems during pregnancy to reduce risk for pre-term delivery.
Explanation:
Acute periodontal problems should be treated during pregnancy to reduce the risk for pre-term delivery.
The surface monolayer of chylomicrons consists mainly of phosphodiglycerides such as a lecithin and which one of the following?
Choices:
- Bile salts
- Cholesterol
- Cholesterol esters
- Monoglycerides (e.g., lysolecithin)
- Ttriglycerides
- Cholesterol
Explanation:
To be in the surface monolayer, a molecule must be amphipathic. Cholesterol is not only amphipathic, but the steroid nucleus also packs tightly between the fatty acyl chains of the phospholipids. Cholesterol esters and triglycerides are too nonpolar to be part of the surface layer and therefore migrate to the core of the lipoprotein particle. Bile salts and monoglycerides are detergents. In high concentrations they would simply emulsify any lipid structure. The physiological concentration of monoglycerides is therefore kept very low. Bile salts are not found in plasma or lymph, where lipoproteins are present, and therefore are not incorporated into the structures.
All of the following are significant products of pancreatic amylase action on amylopectin EXCEPT which one?
Choices:
- Glucose
- Maltose
- Maltotriose
- Isomaltose
- Alpha-dextrins
- Glucose
Explanation:
In the small intestine, pancreatic amylase continues the process of starch digestion started in the mouth by salivary amylase (but, that was largely interupted by denaturing effects of acid in the stomach). Products of pancreatic amylase are the disaccharide maltose, the trisaccharide maltotriose, the alpha 1,6-linked disaccharide isomaltose, and oligosaccharides known as limit dextrins that are usually 4-9 glucosyl residues long. Alpha dextrins are the shortened oligosaccharide products of alpha amylase action. Amylase does not release free glucose.
Reduced activity of which one of the following enzymes would have the most deleterious effect on protein digestion?
Choices:
- Chymotrypsin
- Elastase
- Pepsin
- Carboxypeptidase
- Enteropeptidase
- Enteropeptidase
Explanation:
The pancreas secretes digestive enzymes mainly as inactive zymogens or proenzymes that require proteolytic cleavage to become active. Enteropeptidase (often termed enterokinase, which is actually a misnomer because no ATP is involved) is secreted by the brush border cells in the intestine, and its job is to get the ball rolling. It cleaves trypsinogen to form trypsin, which in turn “autoactivates” more molecules of trypsin. Once activated, trypsin becomes a very important player in the whole process; it not only acts by itself directly on dietary proteins in the gut, but also plays a central role in converting various other pancreatic zymogens into their active forms.
Amino acids and glucose in the lumen of the small intestine are taken up by intestinal absorptive cells mainly by which kind of transport mechanism?
Choices:
- Primary-active, using ATP driven pumps
- Secondary-active, using Na+ driven symporters
- Secondary-active, using K+ driven antiporters
- Passive-facilitated, using substrate selective transport proteins
- Passive-facilitated, using non selective, ungated channels
- Passive-facilitated, using substrate selective voltage gated channels
- Secondary-active, using Na+ driven symporters
Explanation:
Recall that the kidney uses a similar symport system that recovers glucose by co-transport with sodium.
Which one of the following organisms is most often the causative agent of “hand, foot, and mouth disease?”
Choices:
- Candida albicans
- Coagulase-negative Staphylococci
- Coxsackievirus
- HSV-1
- HSV-2
- Coxsackievirus

The enzyme urease is encoded by Helicobacter pylori and is required for colonization and survival in the stomach. The reaction that is catalyzed by this enzyme results in the production of which one of the following?
Choices:
- Ammonia
- Carbon monoxide
- Hydrogen peroxide
- Oxygen
- Urea
- Ammonia
Explanation:
Urease catalyzes the reaction:
urea + H2O -> CO2 + 2NH3
The ammonia produced acts as a base to neutralize stomach acid in the microenvironment of the bacterium, which depends on urease for survival.
A 42-year-old female is admitted to the intensive care unit following a motor vehicle accident. On physical examination she exhibits decerebrate posture, papilledema, absent response to pain and unilateral, dilated and unreactive right pupil. On the second day she becomes hypotensive; endoscopic evaluation discloses gastric and duodenal ulcers. Which one of the following alternatives is correct, regarding the lesions developed on the second day?
Choices:
- Probably caused by vagal nuclei stimulation.
- Rare with intracranial diseases.
- Perforation is unexpected.
- Gastric obstruction probable if patient survives.
- Associated with intractable vomiting.
- Probably caused by vagal nuclei stimulation
Explanation:
The clinical scenario describes acute gastric and duodenal ulceration arising in patients with intracranial disease (Cushing ulcers). Cushing ulcers are considered to arise from gastric acid hypersecretion caused by direct stimulation of the vagal nuclei, The correct answer is: Probably caused by vagal nuclei stimulation. Cushing ulcers are common in patients with severe intracranial diseases and carry a high incidence of perforation. Obstruction, associated with intractable vomiting if total, is associated typically with chronic ulcers.
A 57-year-old male has worsening midepigastric pain and 8 kg weight loss over the last 6 months. Stool samples reveal occult blood, there is conjunctival pallor on physical examination. Upper gastrointestinal radiographic series show an ulcerated lesion involving the gastric antrum. The mass is resected; the pathology is attached.
Which one of the following alternatives regarding the epidemiology or pathogenesis of this entity is correct, based on the clinicopathologic features of this case?
Choices:
- Strongly associated with peptic ulcer disease.
- Association to familial adenomatous polyposis (FAP) proves the preeminent role of genetic changes in its pathogenesis.
- Associated with Barret esophagus.
- Increased second-generation Japanese inmigrant incidence.
- Decreasing USA overall incidence.

- Decreasing USA overall incidence.
Explanation:
Gastric cancer, more specifically intestinal-type adenocarcinoma, is the diagnosis of this case. The overall incidence is decreasing in the United States, although those neoplasms arising in the gastric cardia are becoming more frequent due to their association with Barrett esophagus.
The correct answer is: Decreasing USA overall incidence. Gastric cancer is more common in patients with multifocal mucosal atrophy and intestinal metaplasia, not in individuals with peptic ulcer disease (PUD). Partial gastrectomy for PUD imparts a slightly increased risk. Japanese patients with FAP have an increased incidence of intestinal-type adenocarcinomas; this incidence is not as elevated for individuals with FAP residing in low-risk areas, thus supporting the importance of environmental factors. By their second generation, migrant populations from high to low incidence countries have the incidences of the countries of destination.
A 62-year-old male with Addison disease (primary chronic adrenocortical insufficiency) has progressive memory loss and moderate personality changes over the past 11 months. Physical examination reveals a smooth and beefy-red tongue, numbness, loss of vibration sense and conjunctival pallor. Endoscopy shows diffuse loss of rugal folds over the body and fundus, the antrum is spared. Which of the following pathology findings is most likely to be associated with this disease?
Choices:
- Antibodies to Helicobacter pylori
- Hyperplastic gastric polyps
- Decreased gastrin
- Gastric neuroendocrine cell hyperplasia
- Neutrophils within gastric lamina propria
- Gastric neuroendocrine cell hyperplasia
Explanation:
The clinical findings of Addison disease, neurologic/behavioral changes, glossitis, conjunctival pallor (probable anemia), in conjunction with the endoscopic changes are consistent with autoimmune gastritis. Well-developed autoimmune gastritis presents as diffuse atrophy of the body and fundus, with sparing or only mild involvement of the antrum. The antral neuroendocrine cell hyperplasia is a physiologic response to decreased acid production (damage of acid-producing oxyntic body and fundus mucosa). Neuroendocrine cell hyperplasia is responsible for increased gastrin secretion. Antibodies to parietal cells and intrinsic factor are also associated with pernicious anemia, which in turn is associated with megaloblastic anemia and neurologic/behavioral changes. Antibodies to Helicobacter pylori, hyperplastic gastric polyps, normal to decreased gastrin and antral location (occasionally involving body and fundus) are characteristics of
Helicobacter pylori chronic gastritis.