Lecture #35 - Ant pit hormones (thyroid) and parathyroid gland Flashcards
(27 cards)
Anterior Pit Hormones
- What’re the three axis?
- In GHRH…..
- Yeah, just read it
- Ditto
- HPG, HPT and HPA axis that’re regulated at heirarchal level*
- In GHRH - the -ve feedback isn’t a hormone that’s in the name (unlike prolactin) - it’s IGF-1 released by liver (IGF-1 is -ve feedback regulator and it -ve hypothalamus and +ve SS neurons)*
- SS important metabolism bs both (SS and TRH) are involved in metabolism*
- Prolactin - two sets of neurons are going to activate anterior pituitary to secrete prolactin –> -ve feedback regulatory and increase stimulation of dopamine neuron which stops prolactin…..strong -ve feedback for most of our lives; don’t need prolactin - only for milk production*

Appreciate
So thyroid stays regulated else increase or decrease is bad —-> they needa stay in defined range

Thyroid gland
- Location?
- What’re the hormones made and secreted?
- Location: just below the larynx, on the anterior and lateral surfaces of the trachea
- Hormones made and secreted:
- Thyroid hormone - basal metabolic rate/metabolism
- Calcitonin - calcium homeostasis (not regulated in that HP axis)

Thyroid gland: structure
- What is it composed of?
- Each follicle is surrounded by what?
- Thyroid gland - composed of small spherical sacs or follicles
- Each follicle is surrounded by follicular cells.

Thyroid gland: cell types (2) and what do they make?
. Follicular cells make thyrogloublin and secrete it into the follicle (thyroglobulin is a precursor…… these are produced when thyroglobulin’s tyrosine residues are combined with iodine and the protein is subsequently cleaved.)
-
Parafollicular cells or C cells - lie in clusters between the follicles and make the hormone calcitonin (cells on the outside)
- Blood vessel essential for thyroid hormone synthesis bc need supply of Iodine - comes through follicle; binds to thyroidglobulin protein which is your thyroid hormone and then secreted straight into blood vessel and into stream
- Same with calcitonin; when need it, it can get secreted straight into bloodstream

Thyroid hormone synthesis
TGB - protein structure has T4 and T3 within it (subunits which are active thyroid hormones)
TGB = thyroglobulin; these protein-iodine precursors of thyroid hormones
TGB protein can only be stored in the follicle if it gets iodized and to do that, it needs constant supply of iodine.
Iodine gets pumped into follicle and reacts with tyrosine residue in the TGB protein and iodizes that protein thereby stabalising it (thus can be stored)

Thyroid Hormone Secretion (4)
- Iodised TGB moves into the follicular cells.
- Thyroid hormones are released from the iodised TGB.
- Thyroid hormones have two forms: T3 - the active form, T4 - the more plentiful form.
- T3 and T4 secreted into blood (bc lipid), travel bound to a carrier protein (thyroid-binding globulin) to target cells
Therefore:
Iodine is a necessary part of our diet (required for the production of thyroid hormone).

Effects of thyroid hormone (2)
- Metabolism
- Growth - has development effects
- Acts via nuclear receptors that alter the transcription of gene - thyroid enters cell and binds to transcription factor and etc (lecture #1)
Effects of thyroid hormone: metabolism
(4)
- Increased body heat production (increased oxygen consumption and ATP hydrolysis)
- Stimulate fat mobilisation and oxidation of fatty acids in many tissues. Decreased triglyceride and cholesterol levels - so have more feuls to create energy
- Stimulate carbohydrate metabolism, enhance insulin- dependent entry of glucose into cells, increase gluconeogenesis and glycogenolysis - so more glucose
- Sets the basal metabolic rate
- Increase proteolysis; predominantly from muscle - breakdown proteins to get aa’ for glucose production (for skeletal)
-Increase thyroid = increase BMR
Effects of thyroid hormone - BMR
(1)
BMR is the body’s rate of energy expenditure under basal conditions (person is awake, at physical and mental rest, lying down, no muscle movement, at a comfortable temperature and is fasted 12-18 h).
- As you can see, liver uses 29% of basal metabolic energy
- Food digestion increases metabolic rate by 8%

Effects of thyroid hormone - growth (3)
- Normal growth in _____?
- Growth retardation in what? Called what?
- Essential for?
- Normal growth in children
- Growth retardation in thyroid deficiency (cretinism) esp in young kids
- Essential for development of fetal and neonatal brain (CNS) - nervous system also affected
-Make sure you have iodine in diet to prevent this. If low TH at brith - have TH treatment (give to kids) first few days of birth else mentally retarted for life
Endocrine disorders associated with thyroid hormone (5)
- Name
2,3,4,5,6 - effects
- Not enough thyroid hormone (hyposecretion) (adults: myxedema)
2, Low metabolic rate
- Weight gain (not using that energy in body)
- Cold intolerant (thyroid affects heat levels)
- Lethargic (no energy production)
- Slow heart rate

Too much thyroid hormone
- Name?
2,3,4,5,6,7 - effects
- Hypersecretion - Graves Disease
- High metabolic rate
- Weight loss
- Heat intolerant
- Nervousness
- Increased heart rate
- Tissue swelling

Endocrine disorder - Thyroid hornome = ____?
- What is it?
- Can occur if?
Goitre (thyoid gland grows outta control)
- Goitre is enlargement of the thyroid gland
- Can occur if diet lacking in iodine

Iodine Deficiency Disorder (Simple Goitre)
- What’s iodine deficiency?
- What happens to TRH and TSH?
- Without iodine, what can’t be made?
- Thyroid gland enlarges with….?
- Iodine deficiency: thyroid gland is healthy but unable to make enough thyroid hormone (TH). Lack of negative feedback.
- When stored TH is depleted, TRH and TSH secretion increase to stimulate the thyroid gland to make more TH.
- Without Iodine, TH cannot be made
- Thyroid gland enlarges with continual thyroid hormone (T , T ) stimulation by TSH (loss of negative feedback control as there is an inadequate concentration of iodine to make TH).

Thyroid gland: calcitonin
- What makes this?
- What is this hormone involved in?
- Parafollicular cells or C cells - lie in clusters between the follicles and make the hormone calcitonin
- Calcitonin is involved in controlling calcium levels.
* -Not regulated by hypo/pit*
* -calcium lvls in blood regulated by this*
* -sensors on C cells that respind to how much calcium in blood stream (thus blood vessels) and react appropriately*

Controls blood calcium lvls
(2)
– 1% Ca2+ in blood and tissues
• Plasma [9.2-10.4 mg/dL]
– 99% calcium is stored in bones
Calcitonin acts on cells (OB and OC) to regulate amount of Ca++
Bones - very dynamic -
Where does our calcium come from?
- Secreting as much as we should be taking in - calcium deficiency if don’t take in as much as going out
- If Ca++ too much for us then urinary tract
- Hydroxyapaptite: one molcule has 10 atoms of Ca++ so good storage (it’s a mineral)

Appreciate

Calcitonin
- Important effect in who?
- Weak effect in who?
- Calcotonin deficiency is……?
• Children- important effect
– osteoclasts liberate 5g of calcium from bone into the blood each day.
- Adults Weak effect in most adults where osteoclasts liberate only 0.8g of calcium into blood.
- Calcitonin deficiency is not known to cause any adult disease
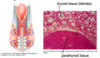
Parathyroid glands
- Secrete what?
- Essential for?
- Secrete PTH (parathyroid hormone)
- PTH is essential for life bc controls Ca2+ lvl in body (not jsust used for bone but also other reactions e.g. heart contraction)
* If thyroid gland gone (due to e.g. disease), then must take in thyroid hormone instead*
Appreciate
-Decrease in blood calcium - PTH secreted so need to increase Ca++
10 Ca : 1 Hydroxy
so increase OC activity
- increase lvl of Ca++ (and stops secretion of Ca++)
- Hydroxy has phosphate so if no phosphate then can’t make hydroxy so calcium afffected

Calcium regulation: PTH and Calcutonin (opposite effects)
PTH increases OC and calcotonin increases OB
- Both have…..?
- Both act on….?
- Together they….?
- PTH and calcitonin have opposite effects on blood calcium concentration.
- Both act on bone (have receptors on bone cells) to increase bone breakdown (PTH) or decrease bone breakdown (calcitonin).
- Together they maintain calcium homeostasis.
NOTE: NOT CONTROLLED BY HYPO (BOTH AREN’T)

What happens when blood Ca2+ are low? (4)
- Hypocalcemia
- Increased excitability of the nervous system
- Leads to of muscle tremors, spasms or
cramps (tetany)
- Begins as plasma Ca2+ concentration falls to 6 mg/dL (cricical cramps under 6)
- At 4 mg/dL muscles of the larynx contract tightly (laryngospasm), which can shut off air flow and cause suffocaBon



