Monday [abdomen muscles, intestine physiology, IBD, spinal curvatures] Flashcards
(100 cards)
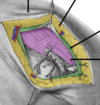
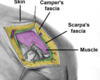
How is the abdominal superficial fascia divided?
Location - above umbilicus = single sheet connective tissue - below umbilicus = two layers; fatty superficial layer [Camper’s fascia] and the membranous deep layer [Scarpa’s fascia]
Where do the superficial nerves/vessels run?
Between these two layers of fascia
Annotate
What are the two main muscles of the anterolateral abdominal wall?
Flat muscles – three flat muscles, situated laterally on either side of the abdomen. Vertical muscles – two vertical muscles, situated near the mid-line of the body
How are the flat muscles strengthened?
Fibres run in different directions and cross each other to strengthen wall and to dercease chance of herniation.
What are the three flat muscles? [from superficial to deep]
External oblique Internal oblique Transverses abdominis
What do the aponeurosis of the flat muscles form in the midline?
linea alba (a fibrous structure that extends from the xiphoid process of the sternum to the pubic symphysis)
The way each flat muscle is arranged and the function of each
- EO = largest, runs inferomedially, contralateral rotation of the torso - IO = smaller and thinner, runs superomedially, bilateral contraction compress the abdomen, while unilateral contraction ipsilaterally rotates the torso - TA = deepest with transversely running fibres, compression of the abdominal contents
Annotate

image
What are the two vertical muscles anterolateral compartment abdomen? Bonus: what forms the six-pack?
Rectus abdominis [intersected by fibrous strips, known as tendinous intersections + linea alba = six pack]. Pyramidalis
Functions of the vertical muscles
rectus abdominis =As well as assisting the flat muscles in compressing the abdominal viscera, the rectus abdominis also stabilises the pelvis during walking, and depresses the ribs pyramidalis =This is a small triangular muscle, found superficially to the rectus abdominis. It is located inferiorly, with its base on the pubis bone, and the apex of the triangle attached to the linea alba. Tenses the linea alba.
What is the rectus sheath
The rectus sheath is formed by the aponeuroses of the three flat muscles and encloses the rectus abdominis and pyramidalis muscles. It has an anterior and posterior wall for most of its length: The anterior wall is formed by the aponeuroses of the external oblique, and of half of the internal oblique. The posterior wall is formed by the aponeuroses of half the internal oblique and of the transversus abdominis. Approximately midway between the umbilicus and the pubic symphysis, all the aponeuroses move to the anterior wall of the rectus sheath. At this point, there is no posterior wall to the sheath; the rectus abdominis is in direct contact with the transversalis fascia. The demarcation point where the posterior layer of the rectus sheath ends is the arcuate line
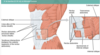
What are the horizontal/vertical planes o the surface of the abdomen?
Horizontal - Transpyloric plane – halfway between the jugular notch and the pubic symphysis, approximately the level of the L1 vertebrae. - Intertubercular plane – horizontal line that runs between the superior aspect of the right and left iliac crests Vertical - run from the middle of the clavicle to the mid-inguinal point (halfway between the anterior superior iliac spine of the pelvis and the pubic symphysis). These planes are the mid-clavicular lines
Annotate


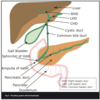
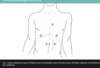
What is the midline, paramedian, Kocher and McBurney incision? When would you use these?
Midline = access abdominal cavity []linea alba poorly vascularised Paramedian = laterally to midline for structures like kidney/spleen/adrenals. Ligates muscles medially to incision = atrophy. Kocher = gain access gallbladder and/or biliary tree pathology McBurney = a McBurney is a called a ‘grid iron’ incision, because it consists of two perpendicular lines, splitting the fibres of the muscles without cutting them – this allows for excellent healing. McBurney incision is performed at McBurney’s point (1/3 of the distance between the ASIS and the umbilicus) and is used in an open appendicectomy
Annotate
What are the five muscles in the posterior abdominal wall?
Iliacus, psoas major, psoas minor, quadratus lumborum, diaphragm
Where is the quadratus and what is it’s function?
The quadratus lumborum muscle is located laterally in the posterior abdominal wall. It is a thick muscular sheet which is quadrilateral in shape. The muscle is positioned superficially to the psoas major. Actions: Extension and lateral flexion of the vertebral column. It also fixes the 12th rib during inspiration, so that the contraction of diaphragm is not wasted
Locatio and function of psoas major
The psoas major is located near the midline of the posterior abdominal wall, immediately lateral to the lumbar vertebrae. Actions: Flexion of the thigh at the hip and lateral flexion of the vertebral column
Location and function of the psoas minor, diaphragm and iliacus
The psoas minor muscle is only present in 60% of the population. It is located anterior to the psoas major. Actions: Flexion of the vertebral column The iliacus muscle is a fan-shaped muscle that is situated inferiorly on the posterior abdominal wall. It combines with the psoas major to form the iliopsoas – the major flexor of the thigh. Actions: Flexion and lateral rotation of the thigh at the hip joint The posterior aspect of the diaphragm is considered to be part of the posterior abdominal wall. It is described in detail here.
what is psoas sign?
The psoas sign is a medical sign that indicates irritation to the iliopsoas group of muscles. The sign is elicited by flexion of the thigh at the hip. The test is positive if the patient reports lower abdominal pain. A right sided psoas sign is an indication of appendicitis. As the iliopsoas contracts, it comes into contact with the inflamed appendix, producing pain.
Annotate


Bonus: describe the fascia of the posterior abdomen
Fascia of the Posterior Abdominal Wall A layer of fascia (sheet of connective tissue) lies between the parietal peritoneum and the muscles of the posterior abdominal wall. This fascia is continuous with the transversalis fascia of the anterolateral abdominal wall. Whilst the fascia is one continuous sheet, it is anatomically correct to name the fascia according to the structure it overlies. Psoas Fascia The psoas fascia covers the psoas major muscle. It is attached to the lumbar vertebrae medially, continuous with the thoracolumbar fascia laterally and continuous with the iliac fascia inferiorly Thoracolumbar fascia The thoracolumbar fascia consists of the three layers; posterior, middle and anterior. Muscles are enclosed between these layers: Quadratus lumborum – between the anterior and middle layers. Deep back muscles – between the middle and posterior layers. The posterior layer extends between the 12th rib and the iliac crest posteriorly. Laterally the fascia meets the internal oblique and transversus abdominis muscles, but not the external oblique. As it forms these attachments it covers the latissimus dorsi. The anterior layer attaches to the anterior aspect of the transverse processes of the lumbar vertebrae, the 12th rib and the iliac crest. Laterally the fascia is continuous with the aponeurotic origin of the transversus abdominis muscle. Superiorly the fascia thickens to become the lateral arcuate ligament, which joins the iliolumbar ligaments inferiorly.
annotate fascia