Pancreas Pathophys Flashcards
(55 cards)
chronic pancreatitis
- Chronic inflammatory changes that lead to:
- Parenchymal fibrosis
- Ductal dilation: dilation of the pancreatic ductal system
- Exocrine insufficiency
- Malabsorption
- Steatorrhea
- Clinically these patients may have malabsorption and steatorrhea because of exocrine insufficiency
- *You need to lose 95% of your pancreatic parenchyma in order to have steatorrhea and exocrine insufficiency, and clinically manifest this way.
- Endocrine insufficiency
- These patients can have endocrine insufficiency as well. They can develop diabetes.
- Pain
- Intermittent or long-lasting
One of the key characteristics that is frustrating for patients is pain which can be intermittent, or constant or remitting. It’s a very heterogenous presentation
treatment of gallstones
cholecystectomy
- For patients with gallstone disease as the etiology for pancreatitis (which is the #1 cause in the world and #2 in the USA), the definitive treatment is cholecystectomy (removal of the gallbladder)
- It is the definitive treatment but it is generally not the acute treatment for pancreatitis. When someone comes in with pancreatitis this is not the first thing you do, though it is the definitive treatment.
pancreatic cancer on the body and tail
- If you have cancer in the body or tail:
- It is a much less specific symptom complex. You have pain, weight loss, and it is diagnosed later so the tumors tend to be larger.
- There are a number of biochemical markers that are useful but not 100% specific or sensitive. The classic one is CA19-9, which can be elevated in pancreatic cancer. (But, not all cancers have elevated markers.)

pancreatic necrosis
- Somewhere over here (*) there is a transition
- This is an IV contrast study: the aorta is bright, meaning that this is an IV enhanced contrast study
- So, the head of the pancreas lights up well and the tail doesn’t. The tail part is necrotic. So that actually predicts mortality as well
- (So just be familiar with what the standard interstitial pancreatitis and the less common necrotic pancreatitis looks like)
chronic pancreatitis mechanism
- Mechanism
- Obstruction of pancreatic duct (pressure)
- The mechanism for this is really not clear. If you have obstruction of the pancreatic duct from strictures or fibrosis or stones (you can actually get stones in the pancreatic duct), maybe there is a pressure phenomenon that mediates the pain.
- Increased parenchymal pressure
- pH/ischemia
- Local ischemia and acidosis may be at play. This is very interesting but controversial
•
the misdirection of proenzymes
•There is a general category which includes the misdirection of proenzymes (zymogens). Instead of directing them to secretion, they are misdirected to lysosomes within the cell where they are prematurely activated to the active enzyme within the cell and lead to an autolytic destruction of the pancreas.

pancreatic pseudocyst
blood supply of the head and uncinate process of the pancreas?
celiac + SMA branches:

- The head and uncinate are supplied superiorly by branches of the celiac, which give rise to the GDA (gastroduodenal artery) and superior pancreatic branches
- The head and uncinate are supplied inferiorly from branches of the SMA to the inferior pancreatic vessels
most common type of pancreatic cancer?
exocrine
adenocarcinoma
gastrinoma
- The second most common type is the gastrinoma
- Gastrinoma is part of a syndrome called Zollinger-Ellison syndrome (ZES)
- These patients present with high levels of gastrin secretion and have peptic ulcers.
- Ulcers are very common and in gastrinoma, patients can have multiple ulcers (sometimes in unusual locations and very large).
- Surgery is recommended after localization is done with cross-sectional CT imaging
medication induced pancreatitis
There are direct toxic metabolic defects to the acinar cells directly from a variety of different medications. Classic ones you see on exams will be HIV medications (HAART: highly active anti-retroviral therapy), thiazides for BP patients, and a number of other meds causing this.
how does acute pancreatitis present?
- What is pancreatitis?
- Pancreatitis is inflammation of the pancreas
- How does it present?
- Typically it presents with abdominal pain that may radiate to the back as well
- Nausea, vomiting, and fever are very classic components of this disease entity
SIRS
I really want you to focus and think about pancreatitis as a systemic disease, and part of the systemic inflammatory response syndrome (SIRS)
- SIRS can be characterized by:
- Tachycardia (HR >90)
- Tachypnea (RR >20)
- Hypothermia or Hyperthermia (rectal temp <36C or >38C)
- And leukopenic or have leukocytosis (WBC <4k or >12k)
- Really think of it as a systemic disease!
insulinoma
- The most common type is the insulinoma
- Patients come in with a fasting hypoglycemia
- You treat them with glucose and they feel better
- They also have high insulin levels that can be detected on serology
- These patients can have insulinomas anywhere inside the pancreas, which can be benign or malignant
We usually recommend resection if possible
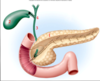
location of the pancreas
- The pancreas is posterior to the stomach, abutting the IVC and the aorta
- Again you can see the tail of the pancreas in the hilum of the spleen
- Going from right to left, the pancreas comes across the IVC and the aorta
- As you go out towards the tail of the pancreas, it abuts the splenic hilum

treatment of choledocholithiasis (CBD stones)
ERCP
treatment of acute pancreatitis
Treatment of pancreatitis
- If you take away nothing else from this talk, what I want to emphasize is that the treatment is supportive. Most of the time things will get better if you support the patient well.
- Supportive
- NPO: Initially try to rest the GI tract and pancreas.
- The patient becomes NPO (nil per os, meaning to withhold oral food and fluids)
- IVF/electrolyte replacement
- Aggressive fluid resuscitation and replacement of electrolytes as appropriate
- Analgesia
- These patients are in a lot of pain, so you want to control their pain.
- People don’t get addicted meds if you’re giving them pain meds for acute pancreatitis
- You want to aggressively treat their pain and give them electrolytes and fluids as appropriate
- Nutritional support
- In the acute setting and long-term setting, you want to give nutritional support.
ERCP
- ERCP (endoscopic retrograde cholangiopancreatography): relieves obstruction of bile duct from stones
- This procedure can also lead to pancreatitis sometimes
dorsal bud
•The dorsal pancreas eventually gives rise to the body and tail of the pancreas, and a small amount of the head.


Interstitial pancreatitis
- What does interstitial pancreatitis look like radiographically?
- This is a CT scan.
- G = gallbladder
- P = pancreas
- In this picture, the CT scan looks a little bit hazy.
- This is hazy because there is a lot of interstitial edema and stranding around the pancreas
- This is what pancreatitis looks like generally.
- There is a slightly more plump pancreas, with a hazy interstitial inflammation.
•
annular pancreas
Annular pancreas
- Much less common, 1 in 7000 people have a condition called annular pancreas
- “Annulus” means ring
- There is a failed complete rotation and fusion of the two dorsal and ventral buds
- If they don’t fuse properly, they can actually constrict the duodenum
- On the right, this is a figure of a barium study showing that there is a constriction at the duodenum (*)
- Above that proximally, there is dilation of the duodenum
- So, annular pancreas can lead to:
- Duodenal obstruction presenting with nausea and vomiting
- Pancreatitis
- And a lot of other situations
- This disease occurs in 1 in 7,000 people, more commonly in Down syndrome patients

venous drainage of body and tail of pancreas?
- The body and tail in an analogous way are drained by branches of the splenic vein
- The splenic vein runs from the spleen and joins with the SMV to form the portal vein
- (Essentially this is all you need to know about the venous drainage. There are a lot of vessels around, but if you know these few facts, you already know all you need to know about the arterial supply and venous drainage of the pancreas.)

main pancreatic duct
- The main pancreatic duct drains through the ampulla of Vater into the duodenum
- The main duct is also called the duct of Wirsung
intraductal papillary mucinous neoplasm
One variant of mucinous cystadenoma is IPMN (intraductal papillary mucinous neoplasm)
- It is usually within the pancreatic duct (hence, intraductal)
- It can either be in the main duct or in a branch
- It is mucinous, so it secretes the same mucin as in mucinous cystadenoma
- IPMN tends to be more common in men, whereas most cystic lesions then to be more female predominant
- IPMN is interesting because it involves the ductal structures
- If you put an endoscope down, you can see the ampulla Vater (1) and the duodenum (2)
- In this picture, the ampulla of Vater is very wide and it has a “fish-eye” deformity.
- This is the classic finding for IPMN and you can also see a mucinous gelatinous fluid secreting from the Ampulla of Vater into the duodenum
- If you look on CT (B) and MRI (C), you can see a dilated pancreatic duct



















