How long after fertilization does a fertilized oocyte resume meiosis?
What does it do with the 2nd polar body?
How long after fertilizatoin does the first mitotic division occur?
Generally, what must a zygot do in order to avoid expellation with menses?
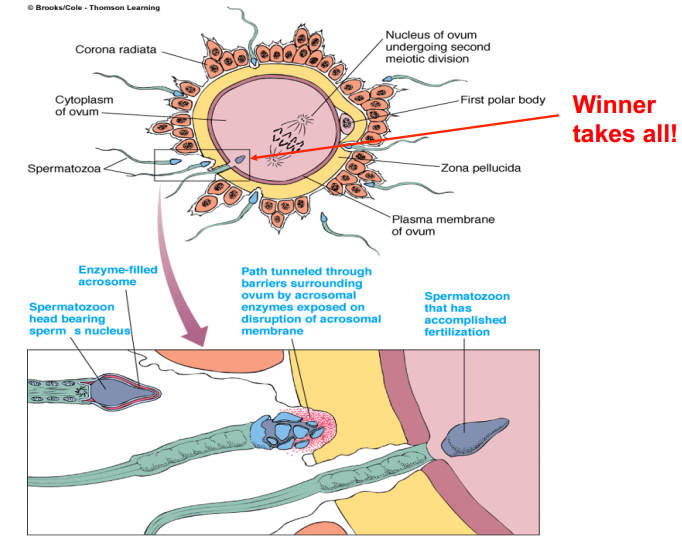
Fertilization of ovum
A. Sperm deposited in vagina must travel to oviduct to meet the egg that has been released from the ovary
B. Enzymes from acrosome of sperm enable entry of the sperm into the cytoplas
C. Ovum responds with reaction that prevents entry of subsequent sperm
D. 2-3 hours after fertilization the ovum resumes meiosis (which was arrested at ovulation); sheds 2nd polar body ensuring diploidy of the zygote
E. Within 18-21 hours the first mitotic division occurs
F. Zygote must signal its presence to avoid being expelled with menses
How long does a fertilized ovum remain in the oviduct prior to implantation?
What process does the fertilized ovum begin to undergo?
What is transport of the fertilized ovum into the uterus dependent upon?
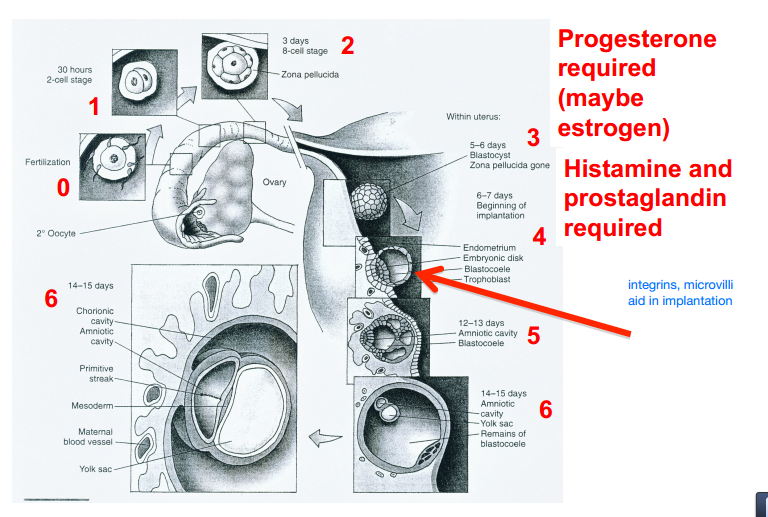
Growth within oviduct and transport to uterus
A. Fertilized ovum remains in oviduct for 3-5 days before implantation in uterus
B. Repeated cell division occurs but with no appreciable increase in size
C. At 4-8 cell stage, morula is formed
D. At 32-64 cell stage the morula becomes a blastocyst
E. Transport of the morula to the uterus is dependent on ciliary motion of cells lining the oviduct
Upon reaching the uterus, the blastocyst implants into the uterine wall.
What process does the uterine stroma undergo in response to implantation? What is the function of this process?
What hormones/chemicals are required for this process?
Implantation
A. Upon reaching the uterus, the blastocyst attaches to the wall
B. The uterine stroma reacts to blastocyst attachment by undergoing a processing of decidualization that prepares the endometrial component of the placenta
- This process is dependent on both histamine and prostaglandins
C. The process of implantation requires that the uterus be primed by progesterone; estrogen may also be required
What does maternal recongnition of pregnancy refer to?
What hormone requires this recognition?
What cells secrete this hormone?
What receptor does this hormone bind to?
What inhibits the release of this hormone?
What is the biological response of this hormone?
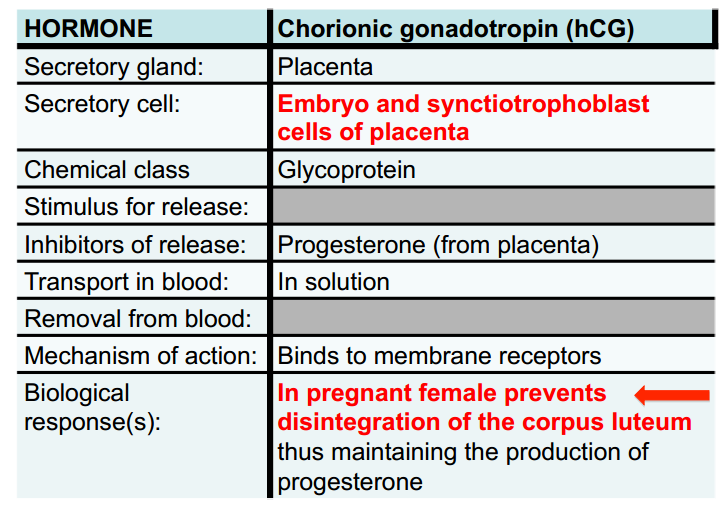
Maternal recognition of pregnancy
A. Refers to the maintenance of the corpus luteum in response to a hormone secreted by the conceptus, human chorionic gondotrophin (hCG)
B. Produced by the syncytiotrophoblast of the implanting blastocyst and diffuses into maternal circulation
C. Binds to LH receptors in ovary and maintains the corpus luteum
D. Thus, hormone production by corpus luteum is maintained
What hormone is hCG very similar to?
When do hCG levels peak? Why do hCG levels decrease after this point in time?
Human chorionic gonadotropin (hCG )
- Is required early in pregnancy
a. Detectable within 9 days of conception (and hence can be used as a pregnancy test)
b. Reaches high concentration within a month and peaks at 15 weeks - Produced by the syncytiotrophoblast cells in blastocyst (early) and then the placenta
- Is a glycoprotein whose alpha unit is identical to that of LH (and TSH and FSH) and a beta unit that is virtually the same as LH
- Consequently, hCG has essentially the same biological activity as LH (maintains the function of the corpus luteum—production of estrogen and progesterone—until the placenta takes over that function).
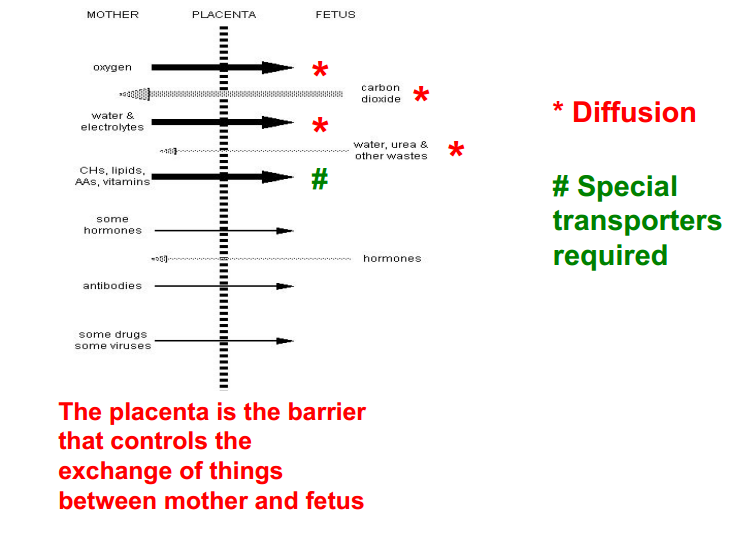
In attached figure, note that hCG levels decrease after progesterone begins being synthesized by the placenta. hCG is no longer needed at such high levels after the corpus luteum involutes and progesterone production is taken over by the placenta.
What structure within the placenta contains fetal blood vessels that penetrate into the wall of the uterus near maternal blood vessels?
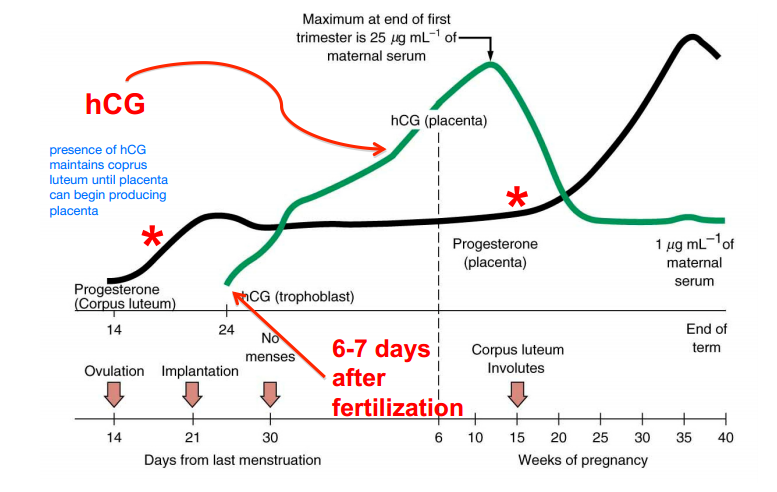
Structure of the placenta
- 3 cm thick and 15-20 cm in diameter
- villi of chorionic syncytiotrophoblast containing fetal blood vessels penetrate deeply into the wall of the uterus in proximity to maternal blood vessels
- this fetal-maternal vascular arrangement is grouped into lobules of which there about 200 in the placenta
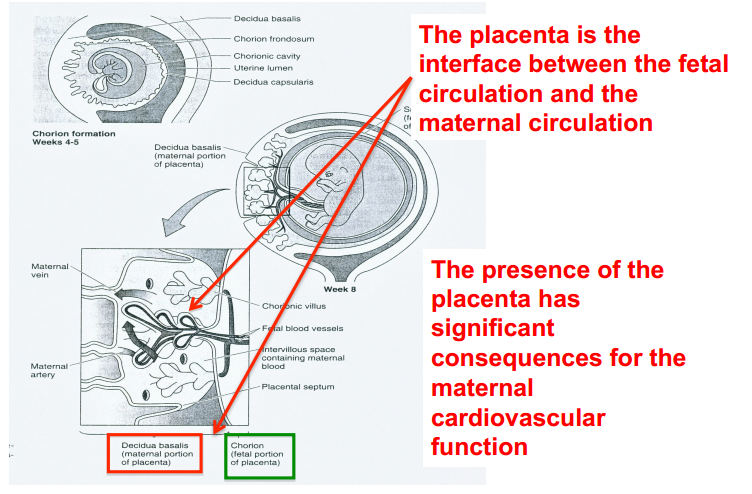
By what mechanisms do exchange of nutrients, oxygen, and fetal waste products occur in the placenta?
Functions of the placenta
- Circulation of maternal and fetal blood within the placenta is established within three weeks of conception
- Exchange of nutrients, oxygen and fetal waste products takes place between the fetal and the maternal circulation here
a. Maternal and fetal circulations are separated by many cells, and simple diffusion is only significant for low molecular weight molecules (blood gases, sodium, water, urea etc.)
b. Special transport mechanisms are present to move larger molecules such as sugars, amino acids, nucleotides, vitamins and plasma proteins
What change occurs to cardiac output during pregnancy?
Why is blood flow velocity low at the placental interface?
Maternal cardiac output is increased because of the extra perfusion “load” represented by the growing fetus
a. Blood flow velocity at placental interface is low to facilitate exchange between mother and fetus, and to prevent the early conceptus from being “dislodged” by the mechanical consequences of arterial pulsations
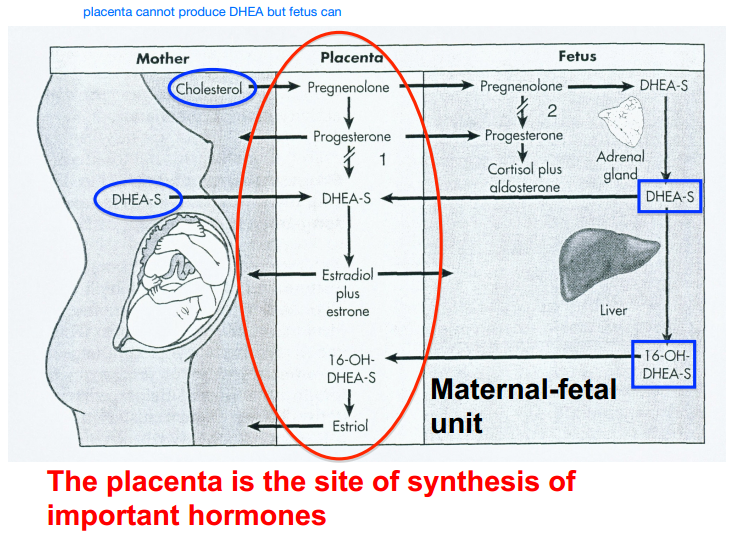
T or F: The maternal-fetal unit (mother + placenta + fetus) is an endocrine organ whose hormones play an essential role in the pregnancy and the development of the fetus.
True.
How do progesterone hormone levels change during pregnancy?
What are the effects of progesterone during pregnancy?
Progesterone
- Is required throughout pregnancy and is secreted at an increasing rate until delivery.
a. Initially the increase is due to secretion by the corpus luteum stimulated by hCG
b. Later progesterone is synthesized by placenta using maternal cholesterol as the precursor
c. Has a number of effects:
i. Reduces uterine muscle activity
ii. Maintains the endometrium
iii. Maintains the cervix in a firm state
iv. Increases maternal appetite and promotes the deposition of fat)
v. Increases maternal alveolar ventilation to a significant extent, probably due to direct stimulation of the medullary respiratory control centers by progesterone (and possibly estrogen)
What initially produces estrogen during pregnancy?
By week 4-5, what synthesizes estrogen? From what precursor?
What are 3 effects of estrogen on the uterus?
Estrogen
- Also increases in concentration throughout pregnancy, initially due to increased secretion by the corpus luteum stimulated by hCG
- By the 4-5 week of pregnancy the placenta is synthesizing all of the estrogen needed from maternal and fetal DHEA
- Has a number of effects on the uterus, preparing it for delivery:
a. increases actin and myosin in uterine smooth muscle cells
b. increases the number of gap junctions between uterine muscle cells
c. increases receptors for oxytocin on uterine muscle cells
Parturition, or birth, requires both _____ of the cervix and coordinated _____ of the uterus.
Parturition, or birth, requires both relaxation (softening) of the cervix (so the birth canal can open) and coordinated contraction of the uterus (to push the fetus through the birth canal).
What are the effects of prostaglandins and oxytocin on uterine smooth muscle?
The myometrium consists of non-striated (smooth) muscle cells
- Cells are linked by gap junctions forming a functional syncetium
- Uterine muscle contractions are dependent on extracellular Ca+2
- Prostaglandins increase the concentration of intracellular Ca+2
- Oxytocin increases the rate of Ca influx and lowers the excitation threshold of the muscle
- During pregnancy the cells hyperthropy from 50μ to 500μ
What is the effect of prostaglandins on the cervix?
What synthesizes prostaglandins during pregnancy?
What hormone stimulates prostaglandin release?
The cervix functions to retain the fetus within the uterus
- Prostaglandins E and F increase the compliance of the cervix
- PGE and PGF are synthesized by the endometrium, myometrium, cervix and placenta
- PGs are released by estrogen
Explain how the onset of parturition is triggered by a CRH clock.
What are the effects of cortisol on the fetus?
The onset of parturition is triggered by a CRH “clock”
a. The increase in CRH causes an increase in estrogen from the placenta
b. CRH acts on the fetal pituitary causing secretion of ACTH
c. ACTH acts on the fetal adrenal cortex to stimulate the secretion of androgens
d. The androgens are converted by the placenta to estrogen
e. The fetal adrenal cortex also secretes cortisol with promotes the maturity of the fetal lungs (ability to breath air), increases liver glycogen levels, increases gluconeogenesis, increases intestinal transport and digestion, and stimulates closure of the ductus arteriosus
f. The increased estrogen:
i. Promotes an increased number of gap junctions between myometrial cells, making it possible for the uterus to generate coordinated contractions
ii. Increases prostaglandin production and results in softening (relaxation) of the cervix
iii. Increases the number of oxytocin receptors in the myometrium
iv. Thus the myometrium becomes more responsive to oxytocin
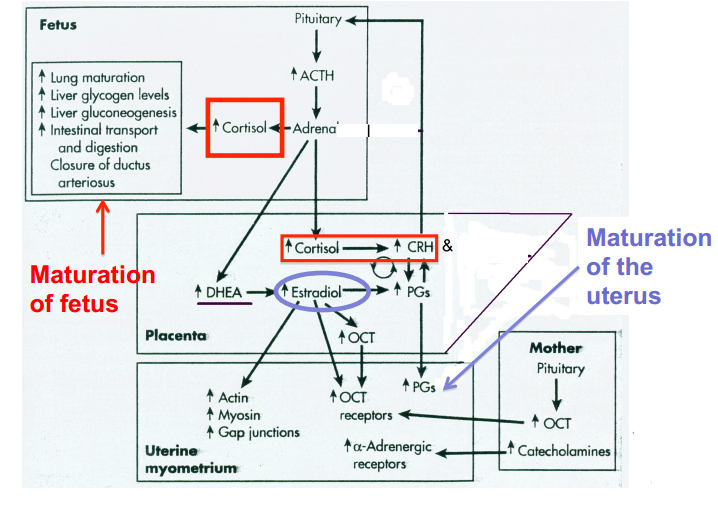
How do CRH levels not cause parturition early in pregnancy (before the fetus is ready for birth)?
A binding protein synthesized by the placenta keeps CRH levels low. When the levels of this protein decreases CRH levels rise and cause the effects discussed.
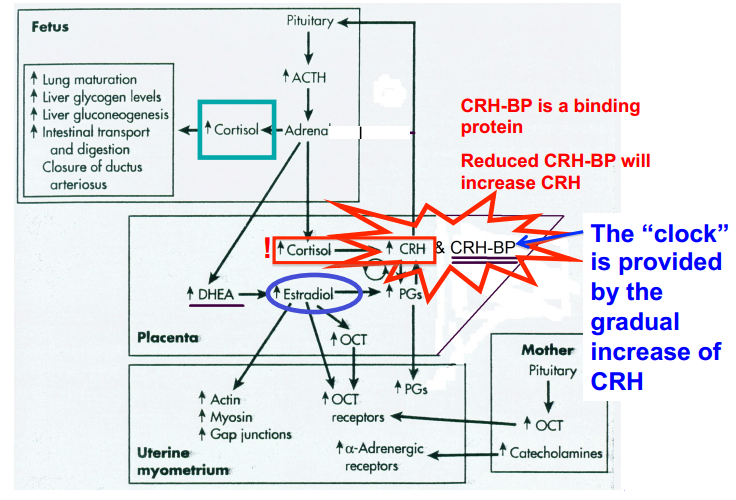
Explain the positive feedback loops involved in parturition.
The progression of parturition
a. The changes outlined previously result in increase uterine contraction
b. This moves the fetus down the uterus and results in push on the cervix
c. A neuroedocrine reflex is then triggered that results in release of oxytocin
d. The increased oxytocin stimulates additional uterine contractions (positive feedback)
e. The increased oxytocin also stimulates increased prostaglandin production which also increases uterine contraction (an additional positive feedback).
f. Cycles terminate when fetus is expelled (delivered) and stimulation of cervix stops
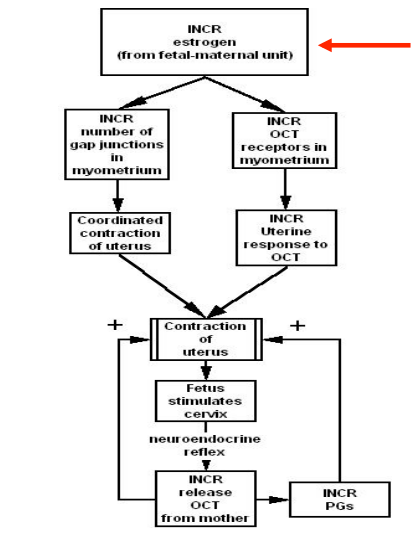
What cells surround alveolar cells in the mammary gland?
What hormones lead to increased alveoli in mammary glands during puberty?
Generally, what occurs to the mammary glands during pregnancy?
Mammary gland secretion of milk
- Mammary gland comprised of 15-20 lobes each of which consists of lobules interconnected by areolar tissue and ducts
- The lobules consist of alveoli from which emerge lactiferous ducts
- Lactiferous ducts converge on lactiform sinuses that serve as small reservoirs
- The sinuses narrow in diameter as they run up through the papilla
- The alveoli contain the milk secreting cells
- Beneath the alveolar cells are myoepithelial cells that form a contractile basket around each alveolus
- At birth the mammary gland consists almost entirely of lactiferous ducts with few, if any, alveoli
- At puberty, increase in estrogen and progesterone lead to appearance of alveoli
- During pregnancy the ductal-lobular-alveolar system undergoes hypertrophy
What hormones must decrease in concentration for lactation to occur?
What hormones are required for milk production and release? What cells do they act on?
What is the effect of suckling on lactation?
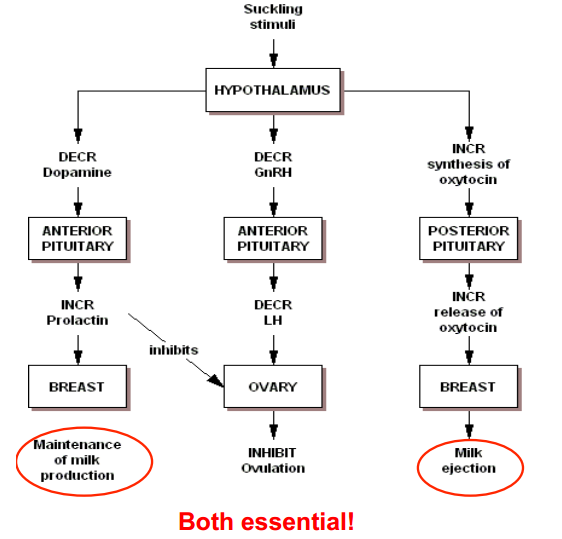
Control of milk secretion and release
- Requires the disappearance of estrogen and progesterone from the maternal circulation(occurs within one week of birth)
- Prolactin increases through pregnancy until term and remains at an elevated level throughout lactation
- If there is no suckling, scant milk secretion will continue for 3-4 weeks because of the elevated prolactin level
- When suckling does occur there are bursts of prolactin secretion
- This is a neuroendocrine reflex
- OCT is required for milk release (acts on myoepithelial cells). PRL stimulates milk production by alveoli.
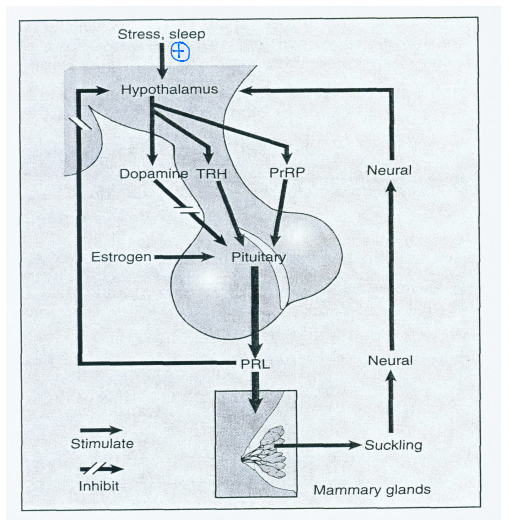
What hormones are affected by suckling? What are the results of changing these hormone levels?