The Blood and Body Defences Flashcards
(31 cards)
Give examples of three major forms of myeloproliferative neoplasms
Polycythemia Vera = an excess of red blood cells in circulation
Essential Thrombocythemia = an excess of platelets
Idiopathic Myelofibrosis = Too few RBC, too many platelets and WBCs
What is Polycythemia?
An excess of RBC in circulation.
Clinical Signs: Breathing difficulties, dizziness, excessive bleeding, splenomegaly, headache, itchiness, red coloring (especially face), shortness of breath, symptoms of phlebitis
What is Primary Polycythemia?
Primarily familial and congenital polycythemia: due to enhanced responsiveness to EPO due to mutations in EPOR.
JACK2V617F
What is Polycythemia Rubra Vera (PV)?
Most commonly associated with JAK2V617F mutation; increased RBC, white blood cells & platelet production; may lead to myelofibrosis and acute leukemia.
What is Secondary Polycythemia?
Occurs due to conditions that promote RBC development:
- Hypoxia (due to COPD, kidney transplant - kidneys being a major source of EPO)
- EPO secreting tumours e.g. renal cell carcinoma, hepatocellular carcinoma
- Neonatal Polycythemia - seen in 1-5% of neonates, due to maternal DBC transfusion after intrauterine hypoxia.
What is Relative Polycythemia?
RBCs normal but reduced plasma volume; this is due to dehydration, severe vomiting.
What are the clinical signs of essential thrombocythemia?
- Frequently asymptomatic; hemorrhage or thrombosis; occasional progression to MF and leukemia.
What are the clinical signs of Idiopathic Myelofibrosis?
leukoerythroblastic blood picture, splenomegaly and bone marrow fibrosis, anaemia, thrombocythemia or thrombocytopenia and variable white cell counts; unusual progression to acte leukemia.

What is the JAK2 gene?
The JAK2 gene is a member of a family of four Janus Kinases, 1 2 and 3 and tyrosine kinase 2.
These are non-receptor kinases.

What does the V617F mutation do?
Mutation of the auto-inhibitory domain makes JAK2 constitutively active in the absence of ligand binding.

Describe Type I Hypersensitivity

Type 1 = basically allergies.
Can be minor (like hay fever) or major (anaphylaxis).
Fc receptors on mast cells can be detected by the IgE antibody. Mast cells have a lot of Fc receptors that recognise IgE molecules.
So when IgE binds to Fc receptor, it can cross link with other molecules. If this happen, binding is stronger, causing degranulation of mast cell.
But if this happens too much - in multiple cells, in multiple organs, resulting in the production of histamine and other inflammatory mediators, it can be life threatening. This is called a type 1 hypersensitivity response.
These massive allergic responses occur not first time of exposure but second time. Because second time round, your body has made very strong IgE responses against these molecules.
Individuals predisposed to genetically produce more IgE than required are termed atopic individuals.
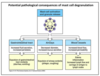
What are the pathological consequences of mast cell degranulation?
GI tract - increased fluid secretion, increased peristalsis = explosion of gastrointestinal tract contents.
Airways - decreased diameter, increased mucus secretion = explosion of airway contents (phlegm, coughing)
Blood Vessels = increased blood flow = increased permeability = edema, inflammation, increased lymph flow and carriage of antigen to lymph nodes.
What is Type II Hypersensitivity?
Type II Hypersensitivity is antibody and complement dependent mechanism of killing.
Uses IgG, complement, targeting cell surfaces.
- Antibody binds antigens on the surface of target cells.
- Fc receptors on NK cells recognise bound antibody.
- Crosslinking of Fc receptors signals the NK cell to kill the target cell.

What is Type III Hypersensitivity?
- Also IgG.
- Also involves complement and phagocytes.
- Soluble molecules are target of the antibodies.
- Another word for Type III Hypersensitivity = immune complex disease.

Explain the mechanism of Type III hypersensitivity
Mechanism
- Locally injected antigen to immune individual with IgG antibody.
- Local immune-complex
- Activation of complement releases inflammatory mediators, C5a, C3a and C4a. C5a also induces mast-cell degranulation.
- Local inflammation, movement of fluid and protein into tissue and blood vessel occlusion.

Explain Type III immune complex-mediated diseases (T3 hypersensitivity)
1) You have an environment with excess antigens and antibodies.
2) Formation of immune complexes with slight antigen excess.
3) Complement is activated by the immune complexes via the classical pathway. This causes basophils to degranulate, releasing mediators that increase vascular permeability
4) Complexes circulate and are trapped in the basement membrane of small blood vessels.
5) Activated complement attracts neutrophils and causes them to degranulate.
6) Neutrophils release enzymes for much of the tissue damage.
E.g. lupus, eczema

Explain Type IV (delayed) Hypersensitivity
- Antigen is introduced into subcutaneous into subcutaneous tissue and processed by local antigen-presenting cells.
- A th1 effector cell recognises antigen and released cytokines which act on vascular endothelium
- Recruitment of T cells, phagocytes, fluid and protein to site of antigen injection causes visible lesion
24-72 hours

In the context of chronic ganulomatous disease, explain primary immunodeficiency
- Basically its a primary phagocytic disease.
- Chronic granulomatous disease - x linked - mutations affecting phagocyte oxidase systems
Histopathology: presence of granulomas
Clincal Signs: impetigo, skin and rectal absecces,
What is chronic granulomatous disease

What drugs can be used to target immunity in therapeutic applications?

What is the phagocyte NADPH oxidase?
Under normal circumstances, the complex is latent in neutrophils and is activated to assemble in the membranes during respiratory burst.
NADPH oxidase generates superoxide by transferring electrons from NADPH inside the cell across the membrane and coupling these to molecular oxygen to produce superoxide anion, a reactive free-radical.
Superoxide can be produced in phagosomes, which contain ingested bacteria and fungi, or it can be produced outside of the cell. In a phagosome, superoxide can spontaneously form hydrogen peroxide that will undergo further reactions to generate reactive oxygen species (ROS).

What is the impact of HIV associated immunodeficiency?

How can naieve T cells differentiate?





