Nursing is one of the most rapidly evolving professions in the medical field. Over the past 50 years, the practice has evolved almost beyond recognition. Changes in healthcare have shifted the entire practice of medicine, and nursing is no exception.
At Brainscape, we're passionate about technology that helps medical students and clinical professionals learn information faster. As a result, we have become involved in conversations about how the nursing profession has evolved, as well as how it is forecast to change in the future.
In this article, we synthesize some of our observations of how nursing has changed over the past 50 years.
Changes In Nursing Over The Last 50 Years
Technology
Changes in technology are a huge driver of changes in the nursing profession. Huge shifts in how patient records are maintained, how medications are tracked and ordered, and how care is passed from one provider to another are causing ripple impacts throughout the medical field. Right now, there is a generational divide between people who embrace this new technology and those who don’t. Some older nurses are uncomfortable with new technology for various reasons, and this tendency is slowing down the adoption of these new methods.
“The healthcare system isn’t doing a great job at figuring out how to nurture those people along,” said one of the young nurses we spoke with.
Of course, there are all the changes in equipment as well. Fifty years ago, syringes were reusable and made of glass that was sterilized with fire between uses. Nurses often used whetstones to sharpen syringes between uses. IV bags didn’t exist, but IV bottles did, and they were made of glass, too. Modern medicine is a throwaway culture, based on disposable syringes, gloves, and items of all sorts. In fact, it has become a major source of pollution.
More Independence And Training
Fifty years ago, many nurses lived at the hospital where they worked and received training. In fact, I come from a three-generation line of nurses, and my grandmother lived in the nurses' dormitories at Tacoma General Hospital in Washington State for a time. For decades, nurses were trained on the job, like in any other trade.
Nursing has traditionally been a woman’s role, and that stereotype is still true: more than 85% of nurses in the United States are female. Fifty years ago, nurses were expected to stand at attention when a doctor entered the room (and to wear the traditional uniform of skirt, stockings, and cap).
Nowadays, things have changed. Nurses are given much more autonomy, and while a nurse’s ability to practice medicine varies from state to state, nurses have more mobility than ever before. This changing role has also resulted from nurses being trained to a higher level of care than ever before. There is also more specialization in nursing than before, allowing students to follow paths in diabetes, pharmacology, and more.
The Rise Of Nurse Practitioners
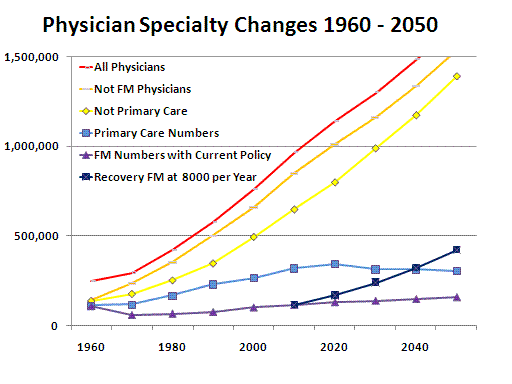
Nurse practitioners present a newer aspect of nursing. The category was largely created in the 1960s as a response to a shortage of doctors, especially in rural and poor communities that didn’t have the financial resources or population to support a doctor. In 18 states, nurse practitioners can work as independent primary care providers with their own practices, which is a huge change in role from the traditional view of nurses as merely doctors’ assistants. In 32 states, nurse practitioners are still required to work with a physician, but this requirement is shifting.
Right now, the United States has an aging population that is going to need a lot of healthcare resources. We also have a dwindling number of primary-care doctors (as most are going into specialties where they can make more money). Because of this, more and more nurse practitioners are providing primary care services. Many healthcare advocates believe that this trend should be encouraged to alleviate shortages in primary-care providers.
The Structure Of Medicine
Over the past 20 years, there has been a broad movement towards conglomerations of hospitals and healthcare systems, and away from smaller clinics and healthcare facilities. This makes sharing of records and coordination of care easier than ever before. But some believe this model is leading to increasing homogenization of healthcare and loss of community-based health systems.
Many hospitals are moving towards “process improvement,” a system modeled after assembly line production processes that are meant to slash waste and improve efficiency. Largely driven by profit motives and increasing competition in the healthcare sector, this poses a challenge to the traditional role of nurses as caregivers, not simply technicians. Standardization of care can eliminate human error, but it can also prevent individualized care plans that take into account the qualitative factors based on relationship and community that play a crucial role in health outcomes.
The Development Of Apps
A final change that we want to highlight is the rise of apps related to nursing. Over the past decade, mobile technology has transformed how nurses study, communicate, and deliver care. Smartphones and tablets have become essential tools in the clinical environment, not just for communication, but also for patient monitoring, data management, and professional development.
Clinical apps now help nurses access drug databases, interpret lab results, and check compatibility between medications in seconds — tasks that once required bulky reference books or consultation with pharmacists. Apps such as Epocrates, Medscape, and Nursing Central have become staples for quick, evidence-based decision-making at the bedside.
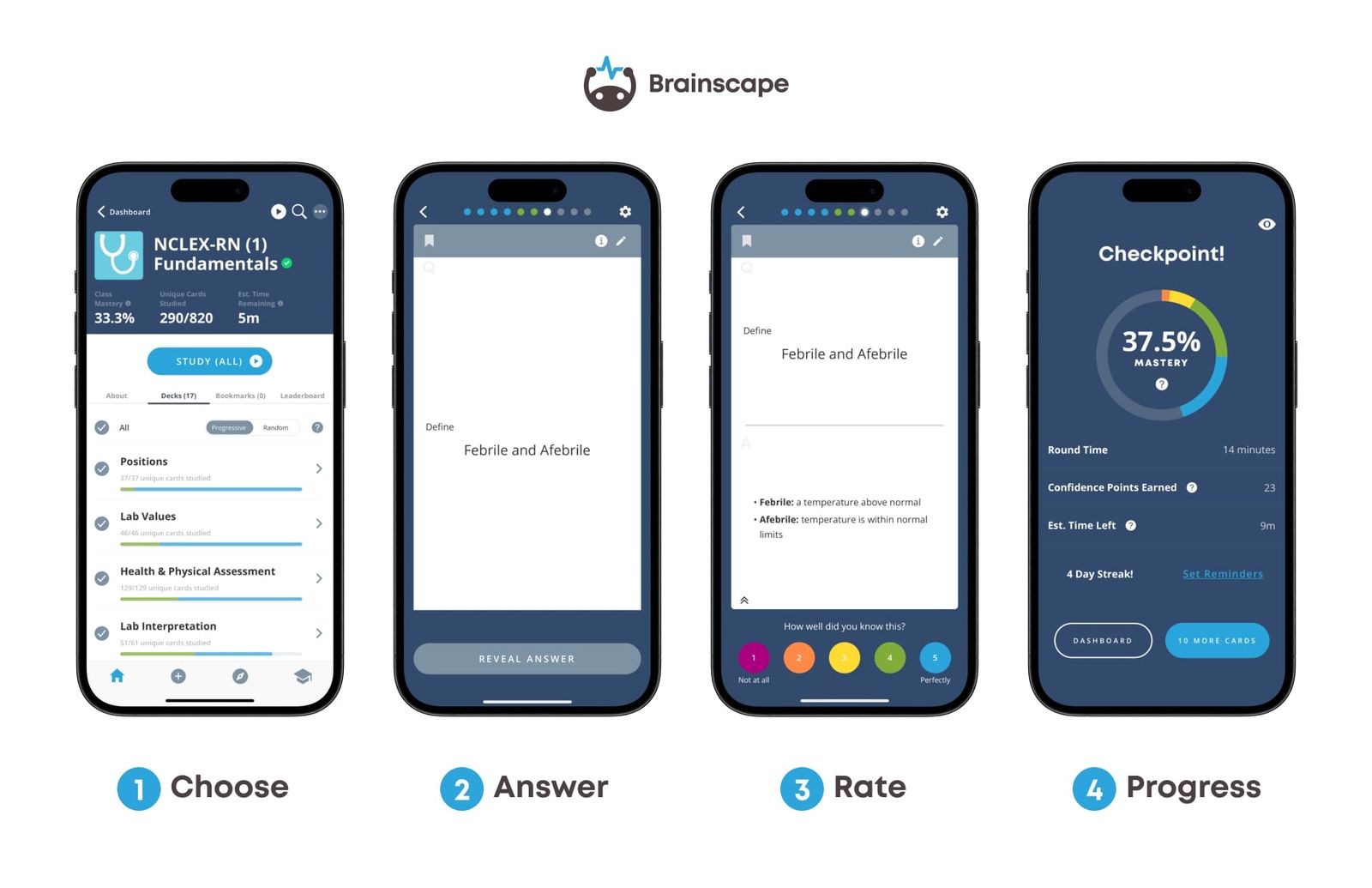
Education apps have also revolutionized nursing. Digital flashcard platforms such as Anki or Brainscape allow nursing students and practitioners to memorize pharmacology, anatomy, and clinical procedures far more efficiently by using learning science techniques like spaced repetition and active recall. These tools make it easier to retain key information long term, reducing the need for last-minute cramming before exams or licensing tests like the NCLEX, and improving the efficiency with which clinicians meet targets for patients.
New Field, New Tools
The role of the nurse has come a long way, from sharpening syringes over open flames to prescribing medications as independent healthcare providers. As the field continues to evolve, so too must the ways we prepare for it.
Whether you’re just starting your nursing journey or leveling up your credentials, embracing modern tools like flashcards can help you stay ahead in a fast-changing profession. In today’s world of tech-driven care and rising patient demands, the smartest nurses are more than compassionate: they’re prepared.
Additional Reading
- How to study medications for the NCLEX
- The best way to use NCLEX practice questions
- Does it matter which nursing school you attend?
**NCLEX-RN® is a registered trademark of the National Council of State Boards of Nursing (NCSBN), which neither sponsors nor endorses this product.
References
Bureau, U. C. (2025, September 23). Older population and aging. Census.gov. https://www.census.gov/topics/population/older-aging.html
Guo, Z. (2022). Environmental pollution of medical waste and new Medical Plastic Waste Treatment Technology. Highlights in Science, Engineering and Technology, 26, 72–79. https://doi.org/10.54097/hset.v26i.3647
Kang, S. H. (2016). Spaced repetition promotes efficient and effective learning. Policy Insights from the Behavioral and Brain Sciences, 3(1), 12–19. https://doi.org/10.1177/2372732215624708
Kerfoot, B. P., Turchin, A., Breydo, E., Gagnon, D., & Conlin, P. R. (2014). An online spaced-education game among clinicians improves their patients’ time to blood pressure control. Circulation: Cardiovascular Quality and Outcomes, 7(3), 468–474. https://doi.org/10.1161/circoutcomes.113.000814
Munday, R. (2024, March 28). Male nurse statistics: A look at the numbers. Nursejournal.org. https://nursejournal.org/articles/male-nurse-statistics/
