14. Pharmacological aspects of immunology Flashcards
(35 cards)
NSAIDS examples
Aspirin Paracetamol Propionic acid derivatives - e.g. ibuprofen, naproxen Arylalkanoic acids – e. g indometacin, diclofenac Oxicams - e.g. piroxicam Fenamic acids - e.g. mefanamic acid Butazones - e.g. phenylbutazone Coxibs e.g. celecoxib
What do NSAIDS do?
All inhibit cyclo-oxygenase Three isoforms of cyclo-oxygenase COX-1 - Constitutive expression COX-2 – Induced in inflammation COX-3 – CNS only?
COX-1
Constitutive expression – all tissues Stomach, Kidney, Platelets, Vascular endothelium Inhibition → anti-platelet activity, side effects
COX-2
– Induced in inflammation (IL-1) Injury, infection, neoplasia Inhibition → analgesia and anti-inflammatory actions
COX-3
CNS only? Inhibited specifically by paracetamol → antipyretic and analgesic actions
Indications for NSAID therapy
Short-term management of pain (and fever) As mild analgesics (orally and topically) - mechanical pain of all types - minor trauma - headaches, dental pain - dysmenorrhoea As potent analgesics (orally, parenterally, rectally) - peri-operative pain - ureteric colic As anti-inflammatories (?) - gout - Inflammatory arthritis eg ankylosing spondylitis, rheumatoid arthritis
Aspirin
Use for pain and inflammation limited by: - GI toxicity - Tinnitus – mechanism obscure, usually reversible - Reye’s syndrome (fulminant hepatic failure in children) Anti-platelet effect - Prophylaxis of ischaemic heart disease - Treatment of acute MI
Non-NSAID antiplatelet drugs
Clopidogrel and dipyrimidole
Paracetamol
Doesn’t bind COX1 or 2. No significant anti-inflammatory action No significant GI toxicity Analgesic/ anti-pyretic Dangerous in overdose
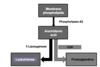
Paracetamol metabolism

Eicosanoid pathways

What is used to treat paracetamol poisoning?
N-acetylcystein / methionine (glutathione precursors) used in paracetamol poisoning
NSAID GI toxicity
In the GI tract prostaglandins E2 and I2
- Decrease acid production
- Increase mucus production
- Increase blood supply
NSAID inhibition in stomach and duodenum
- Irritation
- Ulcers (gastric 15-30%, duodenal 10%)
- Bleeding
Similar effect in the colon
- Colitis – esp with local preps e.g. rectal diclofenac
Things to ask about when prescribing NSAIDS
Upper GI bleeding
- Relative Risk 4.7 all users
- Azapropazone = 23.4
- Piroxicam = 18.0
- Small differences between others…
Biggest risk factor for GI bleed = previous GI bleed
Also
- Age
- Chronic disease (e.g.rheumatoid disease)
- Steroids
NSAID nephrotoxicity
Primarily related to changes in glomerular blood flow
- Decreased glomerular filtration rate
- Sodium retention
- Hyperkalaemia
- Papillary necrosis
Acute renal failure 0.5-1%
Avoid or dose adjust in renal failure
Avoid in patients likely to develop renal failure
Asthma and aspirin
About 10% of asthmatics experience bronchospasm following NSAID – perhaps because of arachidonic acid is shunted down the 5LPO pathway when COX is inhibited
Which NSAID? - non-selective NSAIDS

Preventing NSAID toxicity
Is an NSAID the answer (paracetamol, opioids?)
In terms of GI toxicity
Treatment with
- Gastroprotective drugs (misoprostil – PGE1 analogue, or proton pump inhibitor)
Avoid in renal failure, dose adjust if necessary
Selective COX-2 inhibitors
Selective inhibition of COX-2 in vitro and in vivo
Anti-inflammatory and analgesic in humans
Objective evidence of selectivity (GI, platelets) at > anti-inflammatory doses
The ‘coxibs’
- celecoxib
- etoricoxib
- rofecoxib
- valdecoxib
- etc
Efficacy of coxibs
Numerous clinical trial data
Comparable efficacy (not superior) to non-selective NSAIDs in
- Acute pain
- Dysmenorrhoea
- Inflammatory joint disease
GI side effects of coxibs
that rates of peptic ulceration and GI symptoms much lower with coxibs than NSAIDS but not lower than control
Do Coxibs increase risk of MI?
Cox-2 inhibitors – no activity as antithrombotics
Two studies published in 2005
↑ rates of MI in clinical trials of celecoxib and rofecoxib
Data not fully disclosed by companies?
Relative risk
- small (1.56 for celecoxib higher for others)
- acute (first three months)
Corticosteroid drugs
Cortisol (hydrocortisone) – predominant endogenous glucocorticoid
- Carbohydrate and protein metabolism
- Fluid and electrolyte balance (mineralocorticoid effects)
- Lipid metabolism
- Psychological effects
- Bone metabolism
- Profound modulator of immune response
How do steroids work?
Steroids reduce immune activation by crossing cell membrane
binding their receptors intracellularly
then entering nucleus altering gene expression in numerous cell types
including T cells, B cells and cells of the innate immune system.
Their onset of action is delayed and they must be taken regularly



