17. Atopy, allergy and dth 1 Flashcards
(22 cards)
The early phase reaction
In allergic individuals, exposure to allergens leads to the rapid development of symptoms
develops within seconds or minutes of exposure and results from the binding of allergens to pre-formed IgE antibodies on the surface of mast cells and basophils
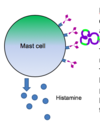
What happens after mast cell IgE ligation?
- IgE binds its specific allergen
- Cross-linking of IgE antibodies by allergen leads to clustering of FcεR1 receptors
- The intracellular portion of the receptor becomes phosphorylated
- The resulting intracellular cascade leads to cellular activation
- Mast cell ‘degranulates’ releasing histamine, tryptase and other pre-formed mediators
Leukotrienes
The leukotrienes produced have similar pharmacological effects to histamine
Phospholipase A2 leads to inflammation and mast cell activation
Pharmacological effects of mast cell mediators and leukotrienes
Skin: wheal and flare
Nose: discharge, sneezing etc
Eyes: conjunctivitis
Lung: wheeze
Examples of sources of allergens
- Pollens
- house dust mite faeces
- stinging insect venom
Allergens are almost always otherwise innocuous environmental proteins
Of the thousands of environmental proteins that we meet, only few hundred are recognised as allergens
General characteristric of allergens
Proteins (there are a few minor exceptions)
- Only protein can produce a T cell (and therefore B cell) response
Physical properties that favour transition across mucus membranes
- Need to cross mucus membranes to activate immunity.
- Typically soluble and low molecular weight
Biologically active, often enzymes
- Interesting, but ?important or coincidence
Have moderate homology with self-proteins
- Theory is that low homology with self-protein=wouldn’t bind to MHC; high homology=would be deleted during negative selection
Clinical allergy syndromes: anaphylaxis
‘Generalised allergic’ reaction
Systemic release of histamine causes generalised vasodilatation & fluid loss from circulation to tissues
- Cutaneous: hives, angioedema
- Gut histamine release: vomiting, diarrhoea
- Mucosal histamine release: laryngeal oedema, bronchoconstriction
- Circulation: vasodilatation, hypotension
Food, drugs and insect venom commonest triggers in UK
Cardinal features of anaphylaxis
typical symptoms
multi-system and dramatic
rapidly follows exposure to allergen and tends to improve fairly quickly thereafter
Clinical allergy syndromes: oral allergy syndrome
Most common type of food allergy amongst UK adults
IgE which is directed against pollen proteins cross-reacts with homologous proteins in plant-derived foods
Oral itching upon exposure to raw fruit, nuts and vegetables
In UK:
- Pollen = mainly birch
- Food = mainly Rosaceae fruits
Clinical allergy syndromes: airway disease
Rhinitis
- Sneezing, rhinorhoea, blockage due to a type 1 allergy
Lower airway obstruction
- Wheeze due to type 1 allergy
Allergens/ symptoms may be:
- Seasonal: pollens, moulds
- Episodic: occupational, animal dander
When symptoms are chronic, the inflammation becomes established and cannot be explained simply in terms of mast cell degranulation
The immunological tightrope
The immune system is constantly challenged with antigens & must somehow decide how to respond
- Self antigens vs non-self
- Dangerous infections vs commensal organisms
- Environmental allergens such as foods and pollens
Activation vs tolerance
Activation: Required for defence against infection and cancer
Tolerance: Required to prevent autoimmune and inflammatory diseases
Origins of allergic disease
Allergic or atopic march = progression of disease observed from infancy
Most children outgrow eczema and many food allergies; rhinitis/ asthma may or may not be outgrown
Allergic disease may however present de novo in adults

Chronic allergic inflammation: asthma
Patients with chronic asthma have on-going symptoms
Most patients are sensitised to a variety of airborne allergens
Biopsy shows inflammatory infiltrate and airway changes known as ‘re-modelling’ – thickened basement membrane and smooth muscle hyperplasia
The ‘early allergic reaction’ model does not provide a good explanation by itself
The late phase allergic reaction

- The early phase reaction to allergen is followed some hours later by a second ‘late phase reaction’
- Biopsy of the late phase shows infiltration with inflammatory cells – particularly CD4 T cells, eosinophils and mast cells; provides some insight into chronic allergic inflammation, and often used as an experimental model
T cell subsets

T cell subsets and Th2 hypothesis
Th2 responses to allergens have been consistently associated with allergic disease
- Biopsies of allergic inflammation are rich in T cells expressing Th2 cytokines
- T cells from allergic patients stimulated with allergen in the laboratory produce Th2 cytokines
Plenty of reasons to believe that Th2 responses may be important in allergy:
- IL-4 is required for B cell class switching to IgE
- IL-4 and IL-13 promote mucus hypersecretion
- IL-5 is required for eosinophil survival
- IL-9 recruits mast cells
Th2 interleukins and allergy
IL-4 is required for B cell class switching to IgE
IL-4 and IL-13 promote mucus hypersecretion
IL-5 is required for eosinophil survival
IL-9 recruits mast cells
Acute response in asthma
Inflammatory mediators cause increased mucus secretion and smooth muscle contraction leading to airway obstruction
Recruitment of cells from the circulation
Chronic allergic disease: asthma
Activated Th2 cells and other inflammatory cells accumulate
Th2 products lead to chronic disease
- IL4: mucus hypersecretion
- IL-13: bronchial hyper-responsiveness
- IL-5: eosinophil recruitment
- IL-9: mast cell recruitment
This model suggests a true role for T cells in chronic inflammation rather than just in causing IgE production
Potential factors in asthma aetiology: genetics
Childhood allergy is strongly predicted by presence of allergy in parents, but difficult to unpick relative contribution of environment
Numerous genetic risk factors identified, but none particularly compelling
Notable that the allergy epidemic has occurred too quickly to be explained entirely by genetics
Hygiene hypothesis
Low hygiene levels, high pathogen load, helminth infection proposed to:
- Skew immunity from Th2 to Th1
- Induce regulatory T cells
High hygiene levels, low pathogen load, absence of helminth infection proposed to:
- Skew immunity towards Th2
- Reduce production of regulatory T cells



