57/58: Surgical treatment of digital deformities - Feilmeier Flashcards
(36 cards)
MPJ anatomy review

flexor stabilization vs. flexor substitution vs. extensor substitution review
-
Flexor Stabilization
- Pronation
- Flexors fire earlier and stay contracted longer to stabilize
- “Excessive gripping”
- Most common
- Pronation
-
Flexor Substitution
- Flexors gain advantage over interossei
- Deep posterior and lateral muscles attempt to make up for weak gastro-soleal complex
- Least common
- Flexors gain advantage over interossei
-
Extensor Substitution
- Pes Cavus, Neuromuscular, Equinus
- Decrease/resolve with wt bearing initially
s/s hammertoe
- •Heloma durum (corn/callous)
- •Hyperkeratosis sub metatarsal head
- •Metatarsalgia
- •Subluxation, dislocation
- •May be flexible or rigid
MIPJ extension
PIPJ flexion
DIPJ extension
hammertoe
s/s claw toe
- Hyperkeratosis and metatarsalgia
- Subluxation, dislocation
- When condition is flexible, toes straighten on weightbearing but are contracted during swing phase
- Hyperkeratosis at distal tip of toe
MPJ extension
PIPJ flexion
DIPJ flexion
claw toe
s/s mallet toe
- Dystrophic nail
- Hyperkeratosis at distal tip of toe
DIPJ flexion
plantrflexed distal phalanx
mallet toe
describe adductovarus 5th toe

- Transverse and frontal plane deformity
- Associated with flexor stabilization
- Very common
- Can also have sagittal plane hammer/clawtoe of 5th
- Weak/ absent quadratus plantae?
- s/s heloma durum/molle, nail complaints
“curly toes”
clinodactyly
- Frontal and transverse planes
- Congenital
- Underlap near digits
- Flexion and varus rotation of DIPJ
- In severe cases the PIPJ is involved
- Usually bilateral
overlapping 2nd toe
- Plantar plate and tendons slip medially or laterally
- Plantar plate or collateral partial tear
- Sagittal and transverse deformity
floating vs. flail toe
(may be used interchangeably)
- floating toe
- Does not purchase ground
- Usually used to describe toe that is still primarily rectus in transverse plane
- Iatragenic: Weil osteotomy, Pin positioning
- Plantar Plate rupture: Predislocation syndrome
- Secondary to brachymetatarsia
- flail toe
- Does not purchase the ground- “floppy”
- Iatrogenic: Aggressive arthroplasty, 5th digit
why do you see nail changes with toe deformities?
nail hypertrophy (2nd toe first ususally) due to rubbing
lachman drawer test
- > 50% dorsal displacement of the base of the proximal phalanx on the head of the metatarsal is positive for plantar plate laxity/rupture
- Evaluates the structural integrity of the plantar plate
thompson and hamilton sign
- Pain with pure vertical force across the MPJ
- Palpable prominent base of proximal phalanx dorsally
- Sign of MPJ instability
kelikian push up test
- Load plantar forefoot- push up on metatarsal heads (simulate wt bearing)
- Watch what happens to the digits at MPJ, PIPJ
- Degree of fixed (structural) deformity is determined by the “push-up” test
- Determines what needs to be done and where
- Does MPJ need to be released?
- Soft tissue versus bone
describe retrograde buckling
- Results in continued stretch/strain to plantar plate
- Increased pressure to plantar metatarsal head
- Metatarsalgia
- Hyperkeratosis formation

crest pad
- For extensor substitution and claw toe deformities
- Takes pressure off of distal digits
- Does not straighten the toes

indications budin splint
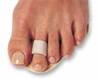
flexor stabilization and substitution
works best with flexible deformity
can also be used for pre-dislocation syndrome
will not work for extensor substitution
resection arthroplasty
Simply means joint work- make sure you specify if “resection”
contraindications to surgical correction of digital deformity
- Active soft tissue infection
- Impaired vascular status
- Impaired neurological status?
- Co-morbid medical conditions
- Cosmesis???
why should the 5th digit be corrected with arthroplasty over arthrodesis?
Due to the 5th digit and 5th MTPJ having its own axis of motion, resection arthroplasty is recommended over arthrodesis
most common way to fix a hammertoe
PIPJ fusion
- creates rigid lever arm
- contraction of flexor now works at MPJ (not at PIPJ) and at DPJ (–> malletoe)
benefits of arthrodesis of PIPJ
- Converts toe to rigid lever
- Done in patients whom intrinsic muscle function has been lost
- Provides stable lever arm
- Decrease risk of recurrence
- Transfers function of flexor to the MPJ






