Advanced GI, Liver Disease and Advanced Neurology Flashcards
(27 cards)
Where is the most common place for a tablet to get stuck?
The Vuleculinc Space (behind the epiglottis)
Briefly explain the FOUR stages of swallowing
Oral Preparatory –> Senses stimulated by sight and smell, producing saliva. This is where chewing occurs and the bolus is formed
Oral Stage –> When the tongue propels the bolus towards the back of the throat. The soft pallate shuts off the nose
Pharyngeal Stage –> ‘Wave like movement that occurs when swallowing’ The airway closes and throat muscles contract to send the bolus into the oesophagus
Oesophageal Stage –> The time in which the bolus enters the oesophagus until in enters the stomach. Lasts between 8-20 seconds

What is the neuronal control of swallowing?
Sensory stimulation of receptors are sent to the ‘swallow centre’ in the medulla via afferent fibres….as well as recieving input from supramedullary structures
Information is then sent back to the muscles via the efferent fibres
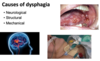
What are the THREE possible causes of Dysphagia?
Neurological –> Eg, strokes, MS, MND and Dementia
Structural –> Tumour of the neck, strictures, mouth ulcers and scarcopenic muscles changes (during natural ageing)
Mechanical –> Trachostomy tube in place, denture problems, infections (eg, thrush), learning disabilites and epilepsy
What are the 5 different types of Enteral tubes that can be put in?
Nasogastric –> Wide bore (cant be used for feeding) or fine bore. These are short term tubes and can be blocked easily
Post-Pyloric –> Through the nose, stomach, pyloric sphincter and small bowel. Used for patients with impaired gastric emptying (normally in ICU). These are very difficult to put in
Gastrostromy (PEG/RIG) –> Endoscope (or barium) into the stomach to allow a hole to be punched through and the tube placed. Can be used for overnight feeding and is more discrete, however more care is needed
Jejunostomy –> Surgically inserted into the jejunum (part of the small intestine) to prevent TPN use, but very easy to block and patients feel very bloated
Gastrojejunostomy –> A PEG tube is inserted into the jejenum. Easier to place than a jejunostomy, but still hard and can be blocked easily

What is Liver Cirrhosis?
Functional hepatocytes become non-functional stellate cells that make collagen
What are the 5 main LFTs?
Alanine Transaminase (ALT) –> Liver specific!
Aspartate Transaminase (AST) –> Found in the liver, heart, skeletal muscle pancreas and muscle (so not very specific)
Both released from heaptocytes when damaged however
Alkaline Phosphatase (ALP) –> Indicates biliary tract involvement….also found in the liver, bone, intestine and placenta
Gamma-Glutamyl Transferase (GGT) –> Increased by enzyme induction (eg, alcohol and cancers). Also found all over the body
Billirubin –> Indicates billary tract involvement. A product of RBC breakdown that is conjugated, beocming water-soluble and excreted via the bile into the intestines and urine. Will cause yellow skin

In Chronic Liver Disease, what effect is there on Albumin levels?
And what effect will this have on specific drugs?
Lower concentration
So higher free drug concentration of highly bound drugs like phenytoin
In liver impairment, what ADME effects are there?
Absorption –> Decreased hepatic blood flow, so decreased first pass effect (increased dose of normal drugs, less for pro-drugs)
Distribution –> Increased V of water soluble drugs due to ascites, so increased concentrations
Low albumin will cause an increase active drug for highly bound drugs
Metabolism –> Accumulation of drug (especially pro-drugs) due to decreased enzymatic activity
Elimination –> Cholestasis causes a decrease in elimination of drugs via the bile, causing reduced enterohepatic circulation
What effect does alcohol have on the liver?
An increase in fat production (steatosis), potentially causing fatty liver disease
Then causes destruction of hepatocytes by neutrophillic infiltration

Why should tramadol be avoided in Liver Cirrhosis?
Half life doubles
Lowers the seziure threshold
What are the TWO types of Stroke?
Ischemic Stroke –> A clot in the brain
Becomes a TIA if symptoms present for less than 24hrs
Haemorrhagic Stroke –> Bleed in the brain

Explain what Thrombolysis is and what a Thrombectomy is
Thrombolysis –> Dissolving the plot using Alteplase (t-PA) a clot busting drug that breaks down plasminogen to plasmin. Should be done ASAP and regardless of if thrombectomy occurs or not
Thrombectomy –> A thin tube is inserted into a vein (via the groin) and into the brain that grabs the clot
The procedure must be done within 6 hours of the stroke occuring

What are the TWO types of Haemorrhagic Stroke?
And what are their treatments?
Subarachnoid (SAH) –> Surgical intervention needed, and often nimodipine
Intracranial (ICH) –> Symptomatically managed… so BP below 160mmHg within 6 hours and 140mmHg for 7 days

What are the THREE types of MS?
And how is the condition managed?
Relapsing-remitting
Primary progressive
Progressive relapsing
Sympomatically managed to prevent spasms, fatigue, actue flares and disease progression

If the gut is affected by a disease, nutritionally what is likely to occur?
Digestion and absorption will change
Pain may also present due to the large nerve supply
Can cause incontinence due to the gut pushing things further down the colon
What is the ERAS Protocol in terms of nutrition and surgery?
Enhanced Recovery After Surgery (ERAS)
Where glucose is taken just before surgery to prevent insulin resistance (speeding up gut recovery)
Avoid prolonged fasting pre-op also
What type of liquids will somebody with a stoma require?
And why?
Isotonic!
This is because normal liquids (hypotonic) cause sodium to be pulled into the small intestine (and so draw water with it), causing dehydration
What is PERT?
(In terms of nutrition)
Parcreatic Enzyme Replacement Therapy (PERT) such as Creon and Nutrizym
This should be titrated to demand, with yellow/oily stools suggesting that they are being underdosed
What are the 4 main complications that can occur due to enteral feeding?
Diarrhoea
N+V
Aspiration
Metabolic
What is the basic reason for why psychosis occurs?
Increased dopamine levels in the mesolimbic pathway
What is Clozapine?
Drug used for when anti-psychotics just don’t work
Licenced for ‘Treatment resistent schizophrenia’
Major burden = side effects

What is a major interaction with clozapine?
Smoking!!
If a patient stops smoking on treatment then dose reviews will be needed
Why is anticoagulation contraindicated in haemorrhagic strokes?
As it is a bleed on the brain….so you don’t want to thin the blood any more!
If it present then you may need to use reversal agents


