Carcinoma of the prostate Flashcards
(18 cards)
Carcinoma of the prostate
- Most common cancer in men
- 10% cancer mortality in men
- Increasing incidence as more men getting checked
- Hormonal factors important
- Extremely variable
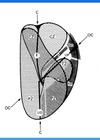
What are the prostatic Zones?
- Transition Zone (TZ): around urethra, site of BPH (benign prostatic hyperplasia), some carcinomas occur
- Peripheral one (PZ): atrophy, most carcinomas occur here
Incidence of prostatic cancer
- Incidental tumours: all pops have a high incidence, increases with age
- Clinically important tumours: marked variation- 20x higher in black amaericans than japan, changes with migration.
Factors contributing to prostatic carcinomas
Genetic Factors: familial incidence (high in black-americans)
Environmental: diet
What’s the issue with prostatic cancers clinical features?
That there are none (not specific ones anyway). Obstructive symptoms too late.
Only way to find is examination: firm area/nodule (finger on prostate)
How do we get a diagnosis with no symptoms?
PSA: protein specific antigen in the serum poor sensitivity/specificity
MRI
Biopsy
Macroscopic appearance of prostate cancer
Can be really hard to spot, as it is sneaky and just infiltrates, doesn’t change mass/size

Whats in this picture

Top: normal glandular prostate (higgildy piggildy with dark basal cells)
Bottom: adenocarcinoma, no basal cells
Grading of prostatic cancer.
“Gleason grading”: unique to prostatic
Patterns 1-5, add two most common patterns to get the score eg
“Gleasons score 7 (3 + 4)”

What are each leavel of gleason grading ?
1: not even cancer, proliferating condition
2: too regular, also not cancerous
3: lowest you can use for cancers, starting to become irregular
4: glands start to fuse together, no individual glands
5: diffusely infiltrating single cells or glands, necrosis in the middle
Issues with gleasons grading
Scores of 2-5 no longer used, lowest score is 6 (which then gets percieved as middle of the range by those that don’t know better).
Group scores lumped together even though prognosis may be different eg 7 could be (4 + 3) or (3 + 4)
New proposal for gleasons grading
Ensures “GI 6” is now the lowest grade
a 7 (3 + 4) is lower then a 7 (4 + 3)

Progression of prostatic cancer
Local spread: extraprostatic fat, seminal vesicles, other pelvic V. BAD!!!
Lymph nodes(uncommon): pelvic, aortic, can block off ureters
Distant metastasis: often to vertebrae
**the further out of the prostate → the higher the stage → the worse the prognosis

Prostatic Nerves
Main nerves run between prostate and rectum. These can be the way the cancer of the prostate goes out. These supply penis and can be damaged during prostate removal → further issues
TNM staging: T2, T3, T4
T2: in prostate
T3: out of prostate
T4: into rectum or bladder
3 categories of management
Small Low grade tumours: no treatment (active surveillance)
Significant Tumours: radical treatment
Advanced tumours: palliative treatment
What is meant by “radical treatment”
Radical prostatectomy: whole prostate + seminal vesicles removed
Radical radiotherapy: into prostatic bed
Palliation treatment includes
Anti-androgen treatment: castration or antiandrogen drugs
Palliative radiotherapy: local or metastases


