\
Congenital abnormalities GIT
AtresiaDuplicationsFistula
Most common congenital is ______. Developmentally incomplete
Atresia
It rsults to mechanical obstruction due to replacement of noncanalized cord.
Esophageal atresia
Atresia most commonly occurs in the _______. It is usually assoc with a _____ connecting the upper and lower esophageal pouches to a bronchus or trachea.
Near tracheal BifucationFistula
Is less common than esophageal atresia but it frequently involves the duodenum and is characterized by a segment of bowel lacking a lumen.
Intestinal Atresia
It is an incomplete form of atresia in which the lumen is reduced in caliber as a result of fibrous thickening of the wall resulting in partial or complete obstruction.Most commonly affected is in the esophagus and small intestine.
Stenosis
The most common congenital intestinal atresia due to failure of the cloacal diaphragm to involute.
Imperforate anus
Are saccular or congenital cystic masses that contain redundant smooth muscle layers. May be present in the esophagus,intestines or colon.
Congenital duplication cyst
What is the tx of ménétrier dse
- Supportive 2. IV albumin 3. Parenteral nutritionSevere cases: gastrectomy
A disease caused by gastrin-secreting tumors, gastrinomas, that are most commonly found in the small intestine and pancreas.Px often present with duodenal ulcer and chronic diarrhea.Within the stomach the most remarkable feature is DOUBLING OXYNTIC MUCOSAL THICKNESS DUE TO A FIVEFOLD INCREASE IN PARIETAL CELLS
Zollinger Ellison Syndrome
Gastric polyps and tumors
- Inflammatory and hyperplastic polyps2. Fundic gland polyps3. Gastric adenoma4.gastric adenocarcinoma5. Lymphoma6. Carcinoid tumor7. Gastrointestinal stromal tumor
Nodules or masses that project above the level id the surrounding mucosa and are i.d in up to 5% of upper GI endoscopiesIt may develop as a result of epithelial or stromal cell hyperplasia, inflammation, ectopia or neoplasia.
Polyps
Approx 75% of all gastric polypsAre most common in indiv bet 50-60 yo.Polyps that usually develop in assoc with chronic gastritis, which initiates the injury and reactive hyperplasia that leads to polyp growth.In indiv with H.pylori, regresses after removal of insult.
Inflammatory and hyperplastic polyps
Occur sporadically and in indiv with FAP.Increased gastric secretion, in response to reduced gastric acidity, and the resulting glandular hyperplasia.5x more commom in women and an average of 50y0.May be asymptomatic or assoc with nausea, vomiting, or epigastric pain.Morphology:Occur in gastric body and fundusWell circumscribed lesions with smooth surfaceSingle or multipleCystically dilated irregular glands lined by flattened parietal and chief cellsInflammation is typically absent or minimal.
Fundic gland polyps
10% of all gastric polyps.Incidence increases progressively with age. Bet 50-603x more in malesLike fundic gland polyp it is assoc with FAPRisk of gastric ca is related to the size of lesion and is elev in leasion greater than 2cm in diameter
Gastric adenoma
Morphology:Usually solitary lesions less than 2cm in diameterMost commonly loc in the antrumMajority are composed of intestinal-type columnar epithelium.
Gastric adenoma
Is the most common malignancy in the stomach.90% of all gastric ca.Early symptoms resemble those of chronic gastritis, including,Dysphagia, dyspepsia, and nausea.Often discovered at advanced stages when symptoms such as wt loss, anorexia, altered bowel ha its, anemia a s hemorrhage trigger further diagnostic evaluation.It is. Ore common in lower socioeconomic status and in indiv with multifocal mucosal atrophy and intestinal metaplasia. PUD doesnt impart as risk factor except to those who had partial gastrectomy for PUD.Majority is not inherited.
Gastric adenocarcinoma
What is the pathogenesis in gastric adenocarcinoma?
Germline mutations in CDH1 which encodes E-cadherin , a protein that contributes to epithelial intercellular adhesion are associated with familial gastric ca of which is a diffuse type.
What is the pathogenesis of intestinal-type gastric ca?
Mutation in beta-catenin, a protein that binds to both E-cadherinand adenomatous polyposis coli ( APC ), as well as microsatellite instability and hypermethylationof several genes including TGF B RII, BAX, IGFR II and p16 /INK4.
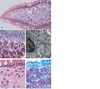
Morphology charac:Irreg enlargement of gastric rugae.Some areas appear polypoid.Enlarged rugae present in body and fundus except antrum( gen spared)Most characteristic feature: HYPERPLASIA OF FOVEOLAR MUCOUS CELLS.THe glands are elongated with CORK-SCREW appearance and cystic dilation is common.Inflammation is only modest although some cases show marked intraepithelial lymphocytosis.Diffuse or patchy glandular atrophy, evident as hypoplasia or parietal and chief cell is typical
Ménétrier dse
2 diseases associated in hypertrophic gastrophaties
- Ménétrier dis2. Zollinger ellison syndrome
Uncommon diseases charac by GIANT CEREBRIFORM ENLARGEMENT OF THE RUGAL FOLDS due to epithelial hyperplasia W/O inflammation.As expected they are linked to excessive GF release
HYPERTROPHIC GASTROPHATIES
Rare d/oCaused by x’ss secretion TGF-alphaCharac by: diffuse hyperplasia of foveolar epithelium of the. Body and fundus and hyperproteinemia due to protein losing enteropathySecondary symptom: wt loss, diRrhea, peripheral edema.Pathologic feature in children same in adult but pedia dse is self- lim and often follows respi infection.Risk of gastric adenocarcinoma is ⬆️ in adult.
Ménétrier dse
Intestinal obstruction occurs at any level but which is commonly affected and why?
Small intestine because of its narrow lumen