Exam VI - Mycoses & Parasitology Flashcards
(18 cards)
Fungal Structure
Cell wall composed of chitin and glucan Ergosterol instead of cholesterol These are potential targets because they are hard to treat since they are eukaryotic like we are = not many anti-fungals on the market
Morphology of Fungi Form
Yeasts: usually unicellular, reproduce via budding creating pseudohyphae and via binary fission Ex. Candida albicans
Morphology of Mold Form
Multicellular have hyphae, which altogether create mycellium Ex. Aspergillus fumigatus
Dimorphism
Some fungi have both yeast and mold forms: thermally dimorphic 37° C (human body temp): yeast form
25° C (room temp): mold form
“yeast in the beast, mold in the cold”
they switch between these forms depending on the environment
Mycoses: Classification by Location
Superficial – infect skin, hair, and nails
Cutaneous – keratinized layer of skin, hair, and nails caused by dermatophytes; itchy scaling of skin with ring like patches Systemic – goes throughout the body; kidney, lung, brain, etc.; thermally dimorphic
Opportunistic – candida albicans because we have it all the time, but when the balance in the body is disrupted it causes infection; immunocompromised AND healthy individuals
Systemic Mycoses
Thermally dimorphic with ability to cause infections in both healthy and immunocompromised Respiratory infections Capable of disseminating to the rest of the body “endemic” geographic regions
Blastomyces dermatitidis
Coccidiodes immitis
Histoplasma capsulatum
Paracoccidiodes brasiliensis
**The signs and symptoms of these fungi are essentially the same, but the location of the fungi, morphology, etc. will help you ID the exact culprit
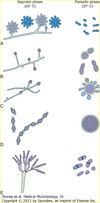
Saprobic and Parasitic Phases of Endemic Dimorphic Fungi
A: Histoplasma capsulatum
B: Blastomyces dermatitidis
C: Paracoccidioides brasiliensis
D: Coccidioides immitis
* All types of Systemic Mycoses
Blastomyces dermatitidis
Systemic Mycoses
Transmission: inhalation of conidia
Soil and leaf litter
Conversion from conidia (infectious form) to yeast (parasitic form) in the lungs
Endemic areas: Southeastern U.S. Ohio-Mississippi River Valleys, Great Lakes region
“broad based budding yeast”
Don’t know you inhaled it, and once in the lungs they will sense the temp change and morph into the yeast form
As it buds off, the base (parent cell) is broader than the daughter cell
Infection: lower respiratory tract
Asymptomatic
Acute onset flu like symptoms: myalgia, chills, malaise, fever
More severe: pneumonia like, high fever, non-productive cough, infiltrates on X-ray – throughout both lungs
Coccidiodes immitis
Systemic Mycoses respiratory infection
Transmission: inhalation of conidia
Found in the soil of the desert Southwest U.S., California, Mexico, Central & South America
Spherule = the name for the yeast form of coccidiodes immitis
Takes hours (12-24) to change between mold and yeast forms
Infection is asymptomatic
Self limiting flulike illness: fever, chest pain, cough, and weight loss
Can progress and disseminate to other parts of the body - dangerous
Histoplasma capsulatum
Systemic Mycoses: Spelunker’s lung
H. capsulatum is found throughout the world and is endemic in certain areas of the United States including states bordering the Ohio River Valley and the lower Mississippi River.
Positive histoplasmin skin tests occur in as many as 80% of the people living in areas where H. capsulatum is common.
Grows in soil and material contaminated with bat or bird droppings.
Spores become airborne when contaminated soil is disturbed.
Transmission: inhalation of conidia
Symptoms: acute primary histoplasmosis, asymptomatic, acute symptomatic primary histoplasmosis; largely dependant on # of spores inhaled
Fever, headache, cough, chills, chest pain, weight loss and sweats
TB vs. Spelunker’s Lung: TB has bloody sputum
Paracoccidioides brasiliensis
Systemic Mycoses
Transmission: inhalation of conidia
Found in soil in Central and South America
Asymptomatic infection common in children
Microscopy: yeast form with many cells budding off called the“Pilot’s wheel”
Symptomatic infection in males 30-50 years of age
Persistent cough with sputum, chest pain, fever, weight loss,
Can disseminate to mucosal surfaces, causing lesions of the mouth, nose & GI tract and can go dormant until reactivation
Tissue Tropism of Parasites
CNS: amebae, malaria, Toxoplasma, trypanosomes
Urogenital Tract: trichomonas
Skin: Leishmania
Blood: malaria and trypanosomes
Liver: entamoeba and Leishmania
Intestine: giardia, Cryptosporidium, Entamoeba, Cyclspora, and microsporidia
Modes of Transmission
Intermediate Host- accidental ingestion of larvae
Fecal/Oral Route: accidental ingestion of larvae from feces of infected host
Active Skin Penetration: larval stages invade through skin
Injection via Insect: larval stages develop to infectivity in insect intermediate host
Giardia lamblia
Protozoa with 2 stages
- Cysts (resistant stage)- usually in water typically shed in stools; Infective stage spread by fecal-oral route
- Trophozoites (active stage) – causes problems in GI tract such as cramps and diarrhea; live in the intestine
Streams, lakes, wild and domestic animals
Contaminated water, fruits and vegetables
Resistant to chlorination
Transmission: ingestion (10-25 cysts)
Gastric acid causes change from cyst to trophozoite
Trophozoite attaches to intestinal villi causing localized tissue damage
Incubation: 1-4 weeks, average 10 days
Symptoms: acute, onset of foul smelling, watery diarrhea, cramps, flatulence, and steatorrhea lasting 10-14 days
Diagnosis: microscopy of stool sample, 1/day for 3 days
Naegleria fowleri
Protozoa: amoeba
Soil at the bottom of lakes
Seasonal: summer, warmer temperatures
Transmission: contact with nasal mucosa
Swimming, water skiing, immersed in water
Invades nasal mucosa, travels to the brain - causes death most of the time, therefore not a successful parasite
Netty pot cases
Primary Amebic Meningoencephalitis (PAM)
Intense frontal headache, sore throat, fever, altered sense of taste and smell, nuchal rigidity - this is usually indicative of meningitis
Death: 4-5 days
Diagnosis: CSF sample will contain ameba and red blood cells
Life Cycle: cyst (found in environment), trophozoite, flagellated form, promitosis back into trophozoite (infectious form) to penetrate the nasal muscae and travels to CSF and brain tissue
Helminths
parasitic worms
1. Flatworms: Tapeworms: cestodes and Flukes: trematodes
2.Roundworms: nematodes
Most common helminth: It has no geography preference = pinworms; infects mostly children
Enterobius vermicularis
Pinworms
Ingestion of eggs, which migrate to large intestine
Mature into adults (2-6 weeks)
Females lay thousands of eggs in the perianal folds
Symptoms: pruritus, loss of sleep, fatigue
Life Cycle: eggs on perianal folds, embryonated eggs ingested by human, larvae hatch in small intestine, adults in lumen of cecum, gravid females migrates to perianal folds at night to lay eggs
Children, day cares, schools
Scotch tape test on anus
Treat entire family as a precaution
Dracunculus medinensis
Nematode (roundworm) in Asia & Africa
Ingestion of intermediate host: copepod (type of cyclops)
Worm larvae released in the stomach, which penetrate through GI walls and migrate to extremities (ams and legs) to cause tissue damage
Forms a vesicle on the skin (1yr after exposure)
Ulcerates (blister), female worm is exposed
Upon contact with water, larvae are released
Ingested by copepods
Animals can also be reservoirs
Life Cycle: larva escapes from skin lesion, ingested in cyclops in the water, goes through 2nd and 3rd larval stages, human ingested cyclops, penetrates intestinal wall, females travel to extremities and lay eggs (dx stage)


