Inflammation Flashcards
(46 cards)
What is the ‘Triple Therapy’ for RA?
A treatment with 3 csDMARDS
Methotrexate, Sulfasalazine and Hydroxychloroquine
What are Matrix Metalloproteinases (MMPs)?
Enzymes that break down collagen
Active at neutral pHs, and require Zn2+
Activated by the removal of propeptides by other proteases
Can be inhibited by Tissue Inhibitors of Metallo-Proteinases (TIMPs)

What are the main ‘risk’ genes for RA?
Genes in the MHC region
Eg, HLA-DRB1
Explain the Reactive Oxygen Species pathway

What is LAD-1?
An adhesion deficincy
Leukocytes do not adhere to extracellular material or endothelium
Leukocytes deficient in the B2 integrin
What is Rheumatoid Arthritis?
The persistant joint inflammation (of synovium) of at least 3 joint areas
Early morning stiffness of at least 30 min duration
1% of people in the UK have RA

What are Anti-Citrullinated Protein Antibodies (ACPA)?
These are highly specific for RA
Can be found in the body up to 14yrs before the onset of RA symptoms
Can predict erosive and progressive disease
What is the main active ingrediant in Sulfasalazine?
Sulfinpyradone
What is Leflunomide?
A new DMARD
Inhibits dihydro-oroate dehydrogenase –> used in the ynthesis of pyrimidines

Explain Prostanoid receptors
PGE2 (prostaglandins)–> EP1 - 4 Act on very specific GPCRs on target cells
PGI2 (prostacyclin) –> IP
Thromboxane receptor = TP
PGD2 –> DP1 + 2
What are the effect of RONS?
Activation of inflammatory gene transcription
Amino acid modifications
DNA damage –> cell apoptosis
What is the EP3 receptor?
A prostaglandin receptor
Activates leukocytes and mast cells
Promotes oedema formation
What are Chemokines?
Chemotactic Cytokines
Produced in responce to bacteria, TNF and IL-1
Act on GPCRs
2 Types
CXC –> Neutrophil attractants
CC

What are eicosanoids?
Oxidation products of 20carbon long fatty acids
Primerily from Arachidonic Acid
Main type is prostaglandins
What are chemotaxins?
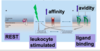
Molecules that attract and activate leukocytes (increasing integrin avidity and affinity)
2 types…
Non Selective
Selective = Chemokines
Explain how low dose aspirin is beneficial……and how therefore taking a COX-2 selective NSAID can have adverse effects
Aspirin is selective to COX-1, and so prevents (pro-thrombotic) thromboxane from platelets, which will decrease the chances of clotting)
This is effective as platelets cannot remake proteins as they have no nucleus, so this effect occurs for a period of time. Also the endothelial produced PGI2 is unaffected
However, when a COX-2 inhibitor is used, PGI2 production stops, and so clotting becomes much more common, as the pro-thrombotic thromboxane is still present (as COX-1 isn’t inhibited)

What are the key indications of poor outcome in RA?
Genetics –> eg, the HLA-DRB1 genotype present
Lab Results –> RF or ACPA presence…..high CRP level
Clinical Assessment –> Many active joints and poor scores
Low educational / social-economical circumstances
What is Rheumatoid Factor?
Antibodies that bind to the Fc domain of IgG
What are the 2 neuropeptides that can positively feedback on histamine release and oedema formation?
NKA (Neurokinin A)
CGRP

Explain which each of the 3 selectins are
L - Expressed on inactivated leukocytes
This causes leukocyte activation, which increases avidity (stickability)
There is rapid shredding of the selectin by proteolytic cleavage (shedase)
P - Expressed on platelets and endothelium
Start in granules, and are rapidly translocated to the cell surface upon activation
E - Endothelial expression is induced by cytokines or LPS
Required ‘de novo’ synthesis –> made on demand –> so takes time (hours)
Their expression is inhibited by glucocorticoids
What is Rituximab?
A B cell depleting monoclonal anti-CD20 antibody

What are the 5 cardinal signs of inflammation?
Heat
Redness
Swelling
Pain
Loss of Function

What is the enzyme that primarily controls steroid biosynthesis?
HMG-CoA Reductase
Produces mevalonic acid
What are the 3 things that plasma proteases are used to create, in reference to inflammation
Kinins (Bradykinin) –> Increases permeability/vasodialtion and pain
Complement –> Activates leukocytes, mast cell degranulation, and bacterial lysis and opsonisation
Clotting Cascade –> Amplifies the kinin and complement pathways
Also causes thrombosis and platelet activation