LEC-8 Reflexes Flashcards
Innate (Primitive) Reflexes - later suppressed by frontal lobes
- Glabellar: after repeated taps on forehead, the person should blink once - Snout: tapping a baby’s closed lips near the midline should cause the lips to pucker/purse - Rooting: Within the first 2 weeks of life, baby will turn their head in little circles towards a direction if their cheek or mouth is stroked - Palmomental: stroking a certain part of the palm of the hand should elicit movement of a chin muscle - Grasp: place something on the palm of the baby’s hand, the baby will curl its fingers around the object and pull in
Developmental Reflexes
- Moro: (Newborn - 7 mo) when startled, baby spreads out its arms and legs as if trying to “grasp” something (newborn - 7 mo) - Tonic Neck: (Newborn - 7 mo) When baby’s head is bent to one side, the arm on the same side as their face straightens and the other arm bends (like “I’m a little teapot”) - Crossed adductor: (Newborn - 7 mo) Tapping patellar tendon elicits both an extension of the knee and a slight adduction of the thigh - Neck Righting: (by 10 months) When the baby’s head passively turns to one direction while lying supine, they try to ‘roll over’ so that their face and chest are on the same plane - Supporting reaction: (by 10 monhs) when lifted in the air while upright, the baby will extend their legs and wiggle them around - Landau: (by 10 months) when held up on their stomach, babies will straighten their legs and head as if they were swimming - Parachute: (by 12 months) when rotating the child from upright to ‘face-first’ position (making the child think they’re falling), the baby holds out their arms as if to ‘break’ the fall
Gegenhalen
Intrinsic resistance of a person to passive movement (i.e. one person tries to lift another person’s hand) - indicative of frontal lobe damage and dementia
Brainstem Reflexes
Corneal: blink upon poking cornea Pupillary Light: pupils contract in response to light Gag: gag in response to ‘tickling’ of back of throat
Corneal Reflex
Afferent Cranial Nerve: Trigeminal (CN5) Efferent Cranial Nerve: Facial (CN7)
Pupillary Light Reflex:
Afferent Cranial Nerve: Optic (CN2) Efferent Cranial Nerve: Oculomotor (CN3)
Gag Reflex
Afferent Cranial Nerve: Glossopharyngeal (CN9) Efferent Cranial Nerve: Vagus (CN10)
Myotatic Reflex
Patellar Tendon jerk
Sensory Fibers from Muscle
Ia: Primary Spindle endings, for muscle length/rate of change of length (12-20 um myelinated) Ib: Golgi tendon organs, for muscle tension (12-20 um myelinated) II: Secondary spindle/non-spindle endings, for muscle length and deep pressure (6-12 um myelinated) III: Free nerve endings, for pain, temperature, and chemical stimuli (2-6 um myelinated) IV: Free nerve endings, for pain, temperature, and chemical stimuli (0.5-2 um nonmyelinated)
Upper Motor Neuron Syndrome
Weakness, spasticity and increased muscle tone, hyperactive myotatic reflexes, loss of cutaneous reflexes
Lower Motor Neuron Syndrome
Weakness, flaccidity and decreased muscle tone, hypoactive myotatic reflexes, loss of cutaneous reflexes
Superficial Reflexes
Abdominal: when skin over abdomen is lightly stimulated, abdominal muscles contract (bellybutton moves towards direction of stimulation) Cremasteric: when inguinal canal is stimulated, the ipsilateral testicle rises into the pelvis Hoffman: tapping fingernail elicits flexion of thumb of same hand Plantar: stroking the sole (plantar) of the foot from lateral side to across the ball of the foot causes flexion of foot
Urogenital Reflex
Anal wink: stimulation around the anus leads to puckering of anus Bulbocavernosus (bulbospongiosus) reflex: squeezing the glans of the penis/clitoris causes the anal sphincter to tighten
Cutaneous Dermatome Innervations
C4: Clavicle C5: Lateral Upper Arm C6: Thumb and lateral forearm C7: Middle finger C8: Pinky finger T4: Nipple T10: Umbilicus L4 & L5: Calf L5: Big toe S1: Little toe S3-5: Perineum L1-L2: Cremaster
Congenital Spinal Cord Disorders
Pathophysiology: Failure of neural tube closure, especially around lumbosacral region Disease: Spina Bifida Occulta Disease: Myelomingocele Disease: Meningocele Risk Factors: Anti-epileptic drugs (valproate), folate deficiency, diabetes, obesity, elevated body temperature
Syringomyelia
Disease type: congenital or acquired (trauma, neoplasm) Pathophysiology: presence of a syrinx in the middle of the spinal cord, obstructing sensory pathways Presentation: loss of pain and temperature sensation across entire arm and upper chest (a “cape-like pattern”)

Friedrich’s Ataxia
Disease type: Autosomal recessive hereditary spinal cord disorder Pathophysiology: Reduced levels and loss of function of frataxin, a mitochondrial matrix protein that protects against Fe overload Onset: usually 10 yrs or younger Presentation: Ataxia, loss of proprioception, optic atrophy, kyphoscoliosis, cardiomyopathy, diabetes mellitus

Adrenomyeloneuropathy
Disease type: X-linked recessive hereditary spinal cord disorder Pathophysiology: Abnormal peroxisomal fatty acid beta oxidation, causing VL chain FA’s to accumulate in oligodendrocytes, Schwann cells, adrenal cortex, & Leydig cells (testicular) Presentation: if in boys 10 or younger, cerebral form (progressive CNS degeneration), if in young adult males, myelopathy with progressive paraparesis Treatment: “Lorenzo’s Oil” or bone marrow transplant

Hereditary Spastic Paraparesis
Disease type: Hereditary (X-linked, autosomal dominant or recessive) spinal cord disorder Presentation: Progressive UMN symptoms, bladder dysfunction, variable impaired vibration sensation

Neoplastic Spinal Cord Disorders
Intramedullary: astrocytoma, ependymoma Extramedullary, extradural: meningioma, schwanomma
Epidural Abscess
Disease type: Infectious Spinal Cord Disease Presentation: rapidly progressive myelopathy, tenderness to percussion

Syphilis - Tabes Dorsalis
Disease type: Infectious spinal cord disease Presentation: Paraparesis with steppage gait, hyporeflexia with Babinski sign
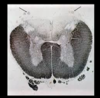
HIV Spongiform myelopathy
Disease: Infectious spinal cord disease

Subacute Combined degeneration
Pathophysiology: B12 or Cu deficiency Presentation: peripheral neuropathy, LE weakness with UMN signs, associated anemia (B12 also shows cognitive dysfunction)






