MSK Flashcards
(58 cards)
Physiology of the Physis
What is the other common name for physis?
How many histological zones are in the physis?
What is the zone closest to the metaphysis called? What happens there?
What does that lead to?
Difference between adult and pediatric injuries?
- The physis, commonly known as the growth plate, consists of four histological zones of cartilage arranged in layers.
- The zone closest to the metaphysis is the zone of provisional calcification, composed of chondrocytes that undergo apoptosis after preparing the matrix for calcification.
- New bone subsequently forms along the scaffolding formed by these chondrocytes, leading to longitudinal growth.
- The unfused physis is the weakest part of the developing skeleton. An injury that can
cause a ligament sprain in an adult may result in physeal fracture in a child.
Salter-Harris Classification
What is it based on?
Which classes have a greater chance of growth disturbance?
Mnemonic?
- The Salter-Harris - SH system classifies Salter-Harris fractures based on the involvement of physis and adjacent epiphysis and metaphysis.
- In general, the higher the classification, the greater the chance of growth disturbance.
- MNEMONIC: SALRT (picture the distal tibia physis)
- Slip
- Above
- Lower
- Through
- Ruined or Rammed

Salter-Harris Type I Injury
Radiographic appearance?
Examples?
- Type I: Injury limited to the physis.
- SH I injuries are often radiographically occult if the epiphysis is not displaced. The physis may be asymmetrically widened. In the absence of physeal widening, the diagnosis of a SH I injury can be suggested based on soft-tissue swelling around the physis.
- Examples: slipped capital femoral epiphysis and gymnast’s wrist (physeal widening caused by chronic stress on the wrist, which may mimic rickets).
Salter-Harris Type II Injury
Describe this injury and mnemonic
- Type II: Fracture extends to metaphysis.
- Mnemonic: Above the distal tibial physis.

Salter-Harris Type III Injury
Describe this injury.
Provide an example.
Mnemonic?
- Type III: Fracture extends to epiphysis.
- Example: Juvenile tillaux fracture, a distal tibial epiphyseal fracture.
- Mnemonic: Lower (picture the distal tibial physis, which is also the example above!)
Salter-Harris Type IV Injury
Describe this fracture.
Provide example.
Mnemonic?
- Type IV: Fracture goes through metaphysis, physis, and epiphysis.
- Example: triplane fracture, comprised of 3 fractures of the distal tibia: oblique fracture through the metaphysis, a vertical fracture through the epiphysis, and horizontal fracture through the physis.
- Mnemonic: Through (picture distal tibial physis fracture, which is also the example above!)

Salter-Harris Type V Injury
Describe this injury.
Mnemonic?
- Type V: Physis is crushed.
- Mnemonic: SALTR (picture distal tibial physis fx)
- Slip
- Above
- Lower
- Through
- Ruined or Rammed
Pediatric Ossification Centers
What are they and in what order do they ossify?
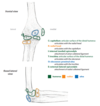
- Six separate ossification centers, each appearing at different stages of development, make the evaluation of the pediatric elbow challenging. However, the cartilaginous ossification centers always ossify in the same order, which can be remembered with the mnemonic CRITOE:
- Capitellum (typically ossifies between 6 months and 1 year of age).
- Radial head.
- Internal (medial) epicondyle.
- Trochlea.
- Olecranon.
- External (lateral) epicondyle (typically ossifies between 10 and 14 years of age).
What is pathognomonic for an elbow fracture, even if no fracture is visible?
- An elbow effusion, as evidenced by displacement of the anterior and/or posterior fat pads (posterior more sensitive), is pathognomonic of a fracture, even if no fracture is visible.

How do you evaluate elbow alignment?
Describe the two lines used to evaluate elbow alignment and what does abormal measurements in these two lines specifically suggest?
- The elbow alignment is evaluated with the anterior humeral and radiocapitellar lines.
- Anterior humeral line: drawn along the anterior humeral cortex, the anterior humeral line should pass through the middle of the ossified capitellum on the lateral view. If abnormal this suggests supracondylar fracture.
- Radiocapitellar line: drawn through the radial shaft, the radiocapitellar line should pass through the capitellum on all views. If abnormal, suggests elbow dislocation.

What is the most common pediatric elbow fracture?
Second most common?
What is the most common adult elbow fracture?
- Supracondylar fracture is the most common pediatric elbow fracture.
- Lateral condyle fracture is the second most common fracture.
- In contrast, the most common adult elbow fracture is of the radial head.
Toddler’s Fracture?
What is it? Mechanism of injury?
Radiographic appearance?
Nondisplaced fractures of what other bones may appear similar?
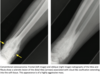
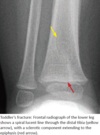
- Toddler’s fracture is a nondisplaced spiral fracture through the tibial** **metadiaphysis, caused by a rotational force to the leg.
- Toddler’s fracture may be clinically difficult to diagnose.
- Radiograph shows a hairline spiral lucency through the distal tibia.
- Nondisplaced fractures of the cuboid and calcaneus may appear similar, with a faint sclerotic band sometimes the only sign of a fracture.
Buckle Fractures
What are they?
Subtle imaging appearance?
How should the cortex normally appear?
- Buckle fractures are unique to the pediatric skeleton, representing a buckling of cortex rather than a true break.
- Buckle fractures can be subtle on imaging and sometimes are only detected by careful inspection of the cortex. Normally, the cortex should be so smooth that a virtual marble can roll down the cortex without bouncing off. Any focal cortical irregularity in a child should raise concern for a buckle fracture.

Pelvic Apophyseal Avulsion Injuries
What is an apophysis?
How many pelvic apophyses are there? how about proximal femoral apophysis?
When do they ossify and when do they fuse?
Why are they susceptible to avulsion? These injuries are most commonly seen in what population and why?
What do acute injuries look like? How about subacute?
Contrast lesser trochanter fractures in adolescents vs adults.
What are all the apophysis and what muscle insert and originate from each one?
- An apophysis is a growth plate that does not contribute to longitudinal growth.
- There are five pelvic apophyses and two proximal femoral apophyses, which arise in puberty and fuse by the third decade. The apophyses are the weakest link of the myotendinous unit. Pelvic apophyses close relatively late in skeletal development and are therefore susceptible to avulsion. Apophyseal avulsion fractures occur most commonly in athletic adolescents, who have strong muscles and open apophyses.
- Acute injuries appear as an avulsed bone fragment. Subacute avulsions are more complex appearing, as the donor site may undergo mixed lytic and sclerotic change in an attempted reparative response.
- Avulsion injuries may be subtle as they are Salter-Harris I equivalent fractures. There is often minimal or no displacement of the otherwise normal-appearing apophyseal ossification.
- Although a lesser trochanter avulsion may occur in an athletic adolescent due to avulsion of the iliopsoas insertion, in an adult a lesser trochanteric fracture is suspicious for a pathologic fracture.

Overview of Imaging for Child Abuse
If there is clinical or radiographic concern for child abuse what imaging needs to be done?
Bone scintigraphy is more sensitive for what type of fractures? What are the shortcomings of bone scintigraphy?
How do you estimate the age of fractures?
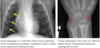
- If there is a clinical or radiographic concern for child abuse, a complete skeletal survey using high-resolution bone technique (for children under 2 years of age) should be performed, including frontal views of all long bones, rib views with obliques, skull, pelvis, hands/feet, and entire spine. The images are reviewed by the radiologist while the child is still in the department.
- Bone scintigraphy is more sensitive for posterior rib fractures, but has higher radiation dose than radiography, is insensitive for skull fractures, and cannot evaluate fracture morphology for age__.
- The age of fractures is estimated by the presence of callus formation. In general, a fracture is less than two weeks old if there is no callus, and at least one week old if there is callus.
- These estimates are rough guidelines. A younger child will form callus and heal more quickly.
What are the highly specific fractures for non-accidental trauma?
Are they the most common fractures?
- These fractures are highly specific for child abuse but are not always seen. If any of heset fractures are seen, immediate concern must be raised for child abuse.
-
Classic metaphyseal lesion (also called metaphyseal corner fracture or bucket handle fracture) is highly specific for abuse, and is a circumferential fracture through the peripheral spongiosa bone of the distal metaphysis, most commonly around the knee or ankle. A classic metaphyseal lesion is thought to be due to violent shaking.
- The classic metaphyseal lesion typically heals quickly (within 10 days without callus formation, so prompt radiography is essential for diagnosis.
-
Posterior rib fractures are also highly specific for abuse but may be very difficult to diagnose when acute. A repeat chest radiograph with bone technique can be performed in the acute setting, or follow-up radiograph after one week to view interval callus formation.
- Unlike in adults, rib fractures are not typically seen after CPR in children. In the rare case of rib fractures from CPR, fractures tend to be anterior and lateral, not posterior.
- Scapula fracture.
- Sternum fracture.
- Spinous process fracture.
-
Classic metaphyseal lesion (also called metaphyseal corner fracture or bucket handle fracture) is highly specific for abuse, and is a circumferential fracture through the peripheral spongiosa bone of the distal metaphysis, most commonly around the knee or ankle. A classic metaphyseal lesion is thought to be due to violent shaking.
What are the suspicious (but no highly specific) fractures that suggest non-accidental trauma?
- These fractures should raise suspicion for child abuse, but are not highly specific.
- More than one fracture.
- Fracture out of proportion to the history.
- Digital fracture in infants.
- Long bone fracture in non-ambulatory child.
- Complex skull fracture.
What are the nonspecific (but frequently seen) fractures suggestive of non-accidental trauma?
- These fractures are commonly seen, both in the settng of child abuse and accidental trauma, but are not specific for child abuse when seen in isolation.
- Linear skull fracture.
- Long bone fracture in an ambulatory child.
Overview of Skeletal Dysplasia
What are bone dysplasias?
What are several terms used to describe abnormal limb growth?
- Bone dysplasias are characterized by impairment of normal growth of bone yielding an abnormal skeleton. The impairment can involve growth slowing down, speeding up, or can cause the bones to grow in an unusual manner.
- Several terms used to describe abnormal limb growth include:
- Rhizomelia: Proximal limb shortening (e.g., humerus is too short).
- Mesomelia: middle limb shortening (e.g., radius is too short).
- Acromelia: distal limb shortening (e.g., hand or wrist is too short).
- Micromelia: Entire limb is shortened.
- Amelia: Limb is absent.
Achondroplasia
What is it?
Affected individuals have what kind of intelligence?
What are the key radiographic findings?
- Achondroplasia is the most common cause of dwarfism.
- Affected individuals have normal intelligence.
- Key radiographic findings include the abnormal morphology of the lumbosacral spine and pelvis:
- Narrowing of interpedicular distances in the lower spine causes spinal stenosis that is compensated for by a characteristic lumbar lordosis as the child learns to walk.
- Posterior scalloping of vertebral bodies.
- Characteristic tombstone iliac wings.
- Flat acetabula, with short femoral necks.
- Other findings include frontal bossing of the skull.

Thanatophoic Dysplasia
What is it?
Inheritance pattern?
Key radiographic findings?
- Thanatophoric is most common lethal skeletal dysplasia.
- It is inherited in an autosomal dominant manner.
- Key radiographic findings are focused on the vertebral bodies and femur:
- Flattening of vertebral bodies (platyspondyly), causing H-shaped vertebral bodies with diffuse narrowing of interpedicular distance.
- Curved telephone receiver femurs.
Osteogenesis Imperfecta
What is it? Which subtype is lethal?
Key radiographic findings?
DDx for multiple fxs?
Contrast DDx to OI
- Osteogenesis imperfecta (OI) represents a varied spectrum of disorders due to abnormal type I collagen.
- OI type II is lethal.
- Key radiographic findings include multiple fractures in the ribs (causing characteristic accordion ribs), vertebral bodies, and long bones. Additional findings include:
- Bowed long bones.
- Osteopenia.
- Wormian bones in the skull, which are secondary to non-coalesced ossification centers in the skull.
- The differential diagnosis for multiple fractures includes OI, rickets and child abuse. of these three, OI is the only entity to cause antenatal fractures.
- With rickets, one would not expect antenatal injury. Fractures and osteopenia may be present.
- With child abuse, one would not expect osteopenia or antenatal injury. Fractures may be present.
Asphyxiating thoracic dystrophy (Jeune syndrome)
What is it? What happens to the lungs?
In addition to main finding, what other bony findings are seen?
- Asphyxiating thoracic dystrophy is an autosomal recessive disorder of a congenitally small thorax causing respiratory distress.
- In addition to the small thorax and associated pulmonary dysplasia, bony findings include:
- Short ribs that are bulbous anteriorly.
- High-riding handlebar clavicle.
- Trident acetabulum.
Cleidocranial Dysostosis
What is it?
Affected patients have what kind of intelligence?
What is this strongly associated with?
Wormian bones are seen in what other entities?
Additional radiographic findings?
- Cleidocranial dysostosis is a skeletal dysplasia characterized primarily by abnormalities in the clavicles.
- Affected patients are of normal intelligence but tend to be short.
- The key radiographic finding is complete or partial absence of the clavicles.
- Cleidocranial dysostosis is strongly associated with wormian bones in the skull.
- Wormian bones are nonspecific, and are also seen in hypothyroidism, osteogenesis imperfecta, healing rickets, and down syndrome.
- Additional radiographic findings of cleidocranial dysostosis include:
- Delayed ossification of the skull (neonatal).
- Widened pubic symphysis (typically not seen until later in life).