Patterns of Lung Disease Flashcards
(25 cards)
Essential Anatomy
What is the elemental unit of lung function?
What does this unit include?
How does the centrilobular artery and bronchus appear on CT?
What is the basic unit of gas exchange? How many of these are in each SPL?
What collects at the periphery of each SPL?
What encases each SPL?
What does thickening of the interlobular septa represent?
How large is each SPL?
- The secondary pulmonary lobule (SPL) is the elemental unit of lung function.
- Each SPL contains a central artery (the aptly named centrilobular artery) and a central bronchus, each branching many times to ultimately produce acinar arteries and respiratory bronchioles.
- On CT, the centrilobular artery is often visible as a faint dot. The centrilobular bronchus is not normally visible.
- The acinus is the basic unit of gas exchange, containing several generations of branching respiratory bronchioles, alveolar ducts, and alveoli.
- There are generally 12 or fewer acini per secondary lobule.
- Pulmonary veins and lymphatics collect in the periphery of each SPL.
- Connective tissue, called interlobular septa, encases each SPL.
- Thickening of the interlobular septa can be seen on CT and suggests pathologic enlargement of either the venous or lymphatic spaces.
- Each SPL is between 1 and 2.5 cm in diameter.

Consolidation and Ground Glass
This is caused by what? What do these represent?
Which description is generally reserved for CT?
What do these findings imply? What two factors characterize these consolidation and ground glass?
- Consolidation and ground glass opacification are two very commonly seen patterns of lung disease caused by abnormal alveoli. The alveolar abnormality may represent either filling of the alveoli with fluid or incomplete alveolar aeration.
- Consolidation can be described on either a chest radiograph or CT, while ground glass is generally reserved for CT.
- Although consolidation often implies pneumonia, both consolidation and ground glass are nonspecific findings with a broad differential depending on chronicity (acute versus chronic) and distribution (focal versus patchy or diffuse).
Consolidation
Describe the alveolar schematic.
Histologically, what is consolidation due to? How is this commonly remembered as?
What do pulmonary vessels appear like in a consolidation? When do you see air bronchograms?
What does consolidation cause when structures are adjacent to it on radiography?
- Consolidation is histologically due to complete filling of affected alveoli with a liquidlike substance (commonly remembered as blood, pus, water, or cells)__.
- Pulmonary vessels are not visible through the consolidation on an unenhanced CT.
- Air bronchograms are often present if the airway is patent. An air bronchogram represents a lucent air-filled bronchus (or bronchiole) seen within a consolidation.
- Consolidation causes silhouetting of adjacent structures on conventional radiography.

DDx for Acute Consolidation
- Acute consolidation is most commonly due to pneumonia, but the differential includes:
- Pneumonia (by far the most common cause of acute consolidation).
- Pulmonary hemorrhage (primary pulmonary hemorrhage or aspiration of hemorrhage).
- Acute respiratory distress syndrome (ARDS), which is noncardiogenic pulmonary edema seen in critically ill patients and thought to be due to increased capillary permeability.
- Pulmonary edema may cause consolidation, although this is an uncommon manifestation.
DDx for Chronic Consolidation
Describe what each one is.
- The differential diagnosis of chronic consolidation includes:
- Bronchioloalveolar carcinoma mucinous subtype, a form of adenocarcinoma.
- Organizing pneumonia, which is a nonspecific response to injury characterized by granulation polyps which fill the distal airways, producing peripherally rounded and nodular consolidation.
- Chronic eosinophilic pneumonia, an inflammatory process characterized by eosinophils causing alveolar filling in an upper-lobe distribution.
Ground Glass Opacification
Describe the alveolar schematic
What is this due to histologically?
What appearance does this term describe?
How do pulmonary vessels appear? How about bronchioles?
- Ground glass opacification is histologically due to either partial filling of the alveoli (by blood, pus, water, or cells), alveolar wall thickening, or reduced aeration of alveoli (atelectasis).
- Ground glass is usually a term reserved for CT. CT shows a hazy, gauze-like opacity, through which pulmonary vessels are still visible.
- The term ground glass was originally described for unenhanced CT as enhanced vessels are visible in consolidation as well; however, in common practice, ground glass is used for any type of CT.
- As with consolidation, air bronchograms may be present.

DDx for Acute Ground Glass Opacification
Contrast to DDx for acute consolidation.
-
Acute ground glass opacification has a similar differential to acute consolidation since many of the entities that initially cause partial airspace filling can progress to completely fill the airspaces later in the disease. The differential of acute ground glass includes:
- Pneumonia. Unlike consolidation, ground glass is more commonly seen in atypical pneumonia such as viral or pneumocystis jiroveci pneumonia.
- Pulmonary hemorrhage.
- Acute respiratory distress syndrome (ARDS).
- Pulmonary edema, which is usually dependent.
DDx for Chronic Ground Glass Opacification
Describe each one too
- Chronic ground glass opacification has a similar but broader differential diagnosis compared to chronic consolidation. In addition to all of the entities which may cause chronic consolidation, the differential diagnosis of chronic ground glass also includes:
- Bronchioloalveolar carcinoma, which tends to be focal or multifocal.
- Organizing pneumonia, typically presenting as rounded, peripheral chronic consolidation.
- Chronic eosinophilic pneumonia, usually with an upper-lobe predominance.
- Idiopathic pneumonias, which are a diverse group of inflammatory responses to pulmonary injury.
- Hypersensitivity pneumonitis (HSP), especially the subacute phase. HSP is a type III hypersensitivity reaction to inhaled organic antigens. In the subacute phase there is ground glass, centrilobular nodules, and mosaic attenuation.
- Alveolar proteinosis, an idiopathic disease characterized by alveolar filling by a proteinaceous substance. The distribution is typically central, with sparing of the periphery.
DDx for Ground Glass in a Central Distribution
Include a description of the finding
- The differential diagnosis for ground glass in a central distribution includes:
- Pulmonary edema.
- Alveolar hemorrhage.
- Pneumocystititis jiroveci pneumonia.
- Alveolar proteinosis.
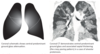
DDx for Peripheral Consolidation or Ground Glass
Compare and contrast pulmonary edema causing peripheral vs central lung parenchymal disease.
- The differential diagnosis for peripheral consolidation or ground glass includes:
- Organizing pneumonia.
- Chronic eosinophilic pneumonia, typically with an upper lobe predominance.
- Atypical or viral pneumonia.
- Pulmonary edema. Peripheral pulmonary edema tends to be noncardiogenic in etiology, such as edema triggered by drug reaction. Peripheral consolidation/ground glass is unusual for cardiogenic pulmonary edema.
Smooth Interlobular Septal Thickening

DDx for Crazy Paving
What in the world is crazy paving?!
What was this pattern initially described for? What is happening in this entity?
- Crazy paving describes interlobular septal thickening with superimposed ground glass opacification, which is thought to resemble the appearance of broken pieces of stone.
- Although nonspecific, this pattern was first described for alveolar proteinosis, where the ground glass opacification is caused by filling of alveoli by proteinaceous material and the interlobular septal thickening is caused by lymphatics taking up the same material.
- The differential diagnosis for crazy paving includes:
- Alveolar proteinosis.
- Lipoid pneumonia, which is an inflammatory pneumonia caused by a reaction to aspirated lipids.
- Organizing pneumonia.
- Pulmonary Hemorrhage.
- Acute respiratory distress syndrome.
- Pneumocystis jiroveci pneumonia.
-
Bronchioloalveolar carcinoma, mucinous subtype.
- MNEMONIC: ALOHA! (plus 2 more an infectious cause - PJP and a neoplasm (adenoCA)

Centrilobular Nodules
What do they represent?
Describe their schematic description.
What do they look like on CT? Size ranges?
What are the two general causes of centrilobular nodules?
- Centrilobular nodules represent opacification of the centrilobular bronchiole (or less commonly the centrilobular artery) at the center of each secondary pulmonary lobule.
- On CT, multiple small nodules are seen in the centers of secondary pulmonary lobules. Centrilobular nodules never extend to the pleural surface. The nodules may be solid or of ground glass attenuation, and range in size from tiny up to a centimeter.
- Centrilobular nodules may be caused by infectious or inflammatory conditions.

What are the infectious causes of centrilobular nodules?
Describe each entity.
- Infectious causes of centrilobular nodules include:
- Endobronchial spread of tuberculosis or atypical mycobacteria. Atypical mycobacteria are a diverse spectrum of acid-fast mycobacteria that do not cause tuberculosis. The typical pulmonary manifestation of atypical mycobacteria is a low-grade infection typically seen in elderly women, most commonly caused by mycobacterium avium-intracellulare.
- Bronchopneumonia, which is spread of infectious pneumonia via the airways.
- Atypical pneumonia, especially mycoplasma pneumonia.
What are the inflammatory causes of centrilobular nodule?
Describe each entity.
- The two most common inflammatory causes of centrilobular nodules include hypersensitivity pneumonitis (HSP) and respiratory bronchiolitis interstitial lung disease (RB-ILD), both exposure-related lung diseases. More prominent centrilobular nodules are suggestive of HSP.
- HSP is a type III hypersensitivity reaction to an inhaled organic antigen. The subacute phase of HSP is primarily characterized by centrilobular nodules.
- Hot tub lung is a hypersensitivity reaction to inhaled atypical mycobacteria, with similar imaging to HSP.
- RB-ILD is an inflammatory reaction to inhaled cigarette smoke-mediated by pigmented macrophages.
- Diffuse panbronchiolitis is a chronic inflammatory disorder characterized by lymphoid hyperplasia in the walls of the respiratory bronchioles resulting in bronchiolectasis. It typically affects patients of Asian descent.
- Silicosis, an inhalation lung disease that develops in response to inhaled silica particles, is characterized by upper lobe predominant centrilobular and perilymphatic nodules.
Perilymphatic Nodules
These follow the anatomic locations of pulmonary lymphatics. What locations can these be seen?
What is by far the most common cause of perilymphatic nodules? Does it have a typical distribution?
What is the DDx for perilymphatic nodules?
- Perilymphatic nodules follow the anatomic locations of pulmonary lymphatics, which can be seen in three locations in the lung:
- Subpleural.
- Peribronchovascular.
- Septal (within the interlobular septa separating the hexagonal secondary pulmonary lobules).
-
Sarcoidosis is by far the most common cause of perilymphatic nodules, typically with an upper-lobe distribution. The nodules may become confluent creating the galaxy sign. The differential of perilymphatic nodules includes:
- Sarcoidosis.
- Pneumoconioses (silicosis and coal workers pneumoconiosis) are reactions to inorganic dust inhalation. The imaging may look identical to sarcoidosis with perilymphatic nodules, but there is usually a history of exposure (e.g. a sandblaster who develops silicosis).
- Lymphangitic carcinomatosis.

DDx for Randomly Distributed Nodules
Describe schematic
These occur via what kind of spread?
What is PLHC? How do you tell between PLCH and the other causes of randomly distributed nodules?
- Randomly distributed nodules usually occur via hematogenous spread and have an angiocentric distribution. The differential of random nodules includes:
- Hematogenous metastases.
- Septic emboli. Embolic infection has a propensity to cavitate but early emboli may be irregular or solid.
- Pulmonary Langerhans’s cell histiocytosis (PLCH), a smoking-related lung disease that progresses from airway-associated and random nodules to irregular cysts. PLCH is usually distinguishable from other causes of random nodules due to the presence of cysts and non-angiocentric distribution.

What does “milliary” nodules mean?
What is the DDx for milliary nodules?
- A miliary pattern is innumerable tiny random nodules disseminated hematogenously, suggestive of the appearance of millet seeds.
- The differential of miliary nodules includes:
- Disseminated tuberculosis.
- Disseminated fungal infection.
- Disseminated hematogenous metastases.

What are Tree-in-bud nodules?
What do they represent? What are they due to?
What is the DDx for tree-in-bud nodularity?
- Tree-in-bud nodules are multiple small nodules connected to linear branching structures, which resembles a budding tree branch in springtime as seen on CT.
- The linear branching structures represent the impacted bronchioles, which are normally invisible on CT, and the nodules represent impacted terminal bronchioles.
- Tree-in-bud nodules are due to mucus, pus, or fluid impacting bronchioles and terminal bronchioles.
- Tree-in-bud nodules are almost always associated with small airways infection, such as endobronchial spread of tuberculosis.
- The differential of tree-in-bud nodules includes:
- Mycobacteria tuberculosis and atypical mycobacteria.
- Bacterial pneumonia.
- Aspiration pneumonia.
- Airway-invasive aspergillus. Aspergillus is an opportunistic fungus with several patterns of disease. The airway-invasive pattern is seen in immunocompromised patients and may present either as bronchopneumonia or small airways infection.

Solitary Cavitary Nodule/Mass
Describe their appearance.
What suggests a benign vs. malignant cavitary lesion?
What is the DDx for a solitary cavitary nodule/mass?
- A cavitary lesion has a thick, irregular wall, often with a solid mural component. Although the findings of benign and malignant cavitary nodules overlap, a maximum wall thickness of = 4 mm is usually benign and a wall thickness >15 mm is usually malignant. Spiculated margins also suggest malignancy.
- A solitary cavitary lesion is most likely cancer or infection.
- Primary bronchogenic carcinoma. While both squamous cell and adenocarcinoma can cavitate, squamous cell cavitates more frequently. Small cell carcinoma is never known to cavitate.
- Tuberculosis classically produces an upper-lobe cavitation.

Multiple Cavitary Lesions
How do these typically spread?
What is the DDx for multiple cavitary lesions?
What particular vasculitis and metastasis tend to cavitate?
- Multiple cavitary lesions are typically vascular or spread through the vascular system:
- Septic emboli.
- Vasculitis, including Wegener granulomatosis, which is especially prone to cavitate.
- Metastases, of which squamous cell carcinoma and uterine carcinosarcoma are known to cavitate.

What is a pulmonary cyst?
What is the DDx for multiple lung cysts? In general, what are cysts due to?
Describe each entity. . . in detail!
- A cyst is an air-containing lucency with a thin, nearly imperceptible wall. In general, cystic lung disease is usually due to a primary airway abnormality.
- The differential diagnosis for multiple lung cysts includes:
- Lymphangioleiomyomatosis (LAM), a diffuse cystic lung disease caused by smooth muscle proliferation of the distal airways. LAM causes uniformly distributed, thin-walled cysts in a diffuse distribution. It is classically associated with chylous effusion, as demonstrated in provided case.
- Emphysema, which tends to be upper-lobe predominant in a smoker.
- Pulmonary Langerhans cell histiocytosis, which features irregular cysts and nodules predominantly in the upper lungs.
- Diffuse cystic bronchiectasis. Bronchiectasis is dilation of the bronchioles. Although cystic fibrosis is the most common cause of bronchiectasis and has an upper-lobe predominance, congenital or post-infectious causes can have a diffuse or lower-lobe distribution.
- Pneumocystis jiroveci pneumonia, which features cysts in late-stage disease.
-
Lymphoid interstitial pneumonia - LIP, an exceptionally rare disease usually associated with Sjögren syndrome and characterized by alveolar distortion from lymphocytic infiltrate and multiple cysts.
- MNEMONIC: PPLLED

What is the DDx for a single pulmonary cyst?
Describe each one.
- Bulla. A bulla is an air-filled cyst measuring >1 cm. A giant bulla occupies at least 30% of the volume of the thorax.
- Bleb. A bleb is an air-filled cystic structure contiguous with the pleura measuring >1 cm. Rupture of a bleb is the most common cause of spontaneous pneumothorax.
- Pneumatocele, which is an air-filled space caused by prior lung trauma or infection.
What is the DDx for basal-predominant fibrotic change?
What is the most common cause?
Describe each one.
- Idiopathic pulmonary fibrosis (IPF), which is a clinical syndrome of progressive pulmonary fibrosis of unknown etiology and is most common cause of basilar fibrosis. It almost always features basilar honeycombing.
- End-stage asbestosis. Asbestosis is an asbestos-induced inflammatory process ultimately producing pulmonary fibrosis. Usually, other signs of asbestos exposure are present, such as pleural plaques.
-
Nonspecific interstitial pneumonia (NSIP), fibrotic form. NSIP is an idiopathic pneumonia. It is a lung response to injury commonly associated with collagen vascular disease and drug reaction.
- The two histologic subtypes are cellular and fibrotic forms, of which the latter may produce basal-predominant fibrosis. In contrast to IPF, honeycombing is usually absent.