Pulmonary Infections including Immunocompromised Flashcards
(34 cards)
What are the clinical classifications of PNA?
- Community acquired PNA (CAP)
- Hospital acquired PNA (HAP)
- Health care associated PNA (HCAP)
- Ventilator associated PNA (VAP)
- PNA in the immunocompromised
What is the MCC of CAP?
What are the etiologies of atypical pneumonia? Who do they affect? How can mycoplasma appear?
What pneumonic etiology is seen in elderly smokers? Radiographic appearance?
What pneumonic etiology is seen in alcoholics and aspirators? Radiographic appearance?
- S. pneumoniae is the most common cause of community-acquired pneumonia.
- Atypical pneumonia, including mycoplasma, viral, and chlamydia, typically infects young and otherwise healthy patients.
- Mycoplasma has a varied appearance and can produce consolidation, areas of ground-glass attenuation, centrilobular nodules, and tree-in-bud nodules.
-
Legionella most commonly occurs in elderly smokers. Infections tend to be severe.
- Peripheral consolidation often progresses to lobar and multifocal pneumonia.
- Infection by Klebsiella and other gram-negatives occurs in alcoholics and aspirators.
- Klebsiella classically leads to voluminous infl__ammatory exudates causing the bulging fissure sign.
What are the radiographic patterns of penumonia?
- Lobar PNA
- Lobular (bronchopneumonia)
- Interstitial PNA
- Round PNA
What is the most common presentation of CAP?
What is the most common etiology?
What remains patent and this leads to what?
- Lobar pneumonia is consolidation of a single lobe.
- It is usually bacterial in origin and is the most common presentation of community acquired pneumonia.
- The larger bronchi remain patent, causing air bronchograms.
How does lobular (broncho)pneumonia manifest?
What is the most common etiology?
- Lobular pneumonia manifests as patchy consolidation with poorly defined airspace opacities, usually involving several lobes, and most commonly due to Staph aureus.
How does interstitial PNA occur?
Appearance?
Etiologies?
- Interstitial pneumonia is caused by inflammatory cells located predominantly in the interstitial tissue of the alveolar septa causing diffuse or patchy ground-glass opacification.
- It can be caused by viral pneumonia, mycoplasma, chlamydia, or pneumocystis.
What is a round pneumonia?
Most common etiology?
Why do they occur?
- Round pneumonia is an infectious mass-like opacity seen only in children.
- Most commonly due to streptococcus pneumoniae.
- Infection remains somewhat confined due to incomplete formation of pores of kohn.
What are the complications of PNA?
- pulmonary abscess
- pulmonary gangrene
- empyema
- pneuomatocele
- bronchopleural fistula
- empyema necessitans
What are the etiologies for pulmonary abscess?
What is almost always present?
Radiographic appearance on frontal and lateral views?
- Pulmonary abscess is necrosis of the lung parenchyma typically due to staphylococcus aureus, pseudomonas, or anaerobic bacteria.
- An air-fuidlevel is almost always present.
- An abscess is usually spherical, with equal dimensions on frontal and lateral views.
What is pulmonary gangrene?
- Pulmonary gangrene is a very rare complication of pneumonia where there is extensive necrosis or sloughing of a pulmonary segment or lobe. Pulmonary gangrene is a severe manifestation of a pulmonary abscess.
What is an empyema?
What are the stages in the development of an empyema? Treatment of each stage?
Is a pleural effusion associated with pneumonia always considered an empyema? Why not?
Appearance? Contrast this to abscess.
What is a radiographic sign for empyema? A similar finding can be seen in what entities (diagram)?
- Empyema is infection within the pleural space.
- There are three stages in the development of an empyema:
- Free-flowing exudative effusion: Can be treated with needle aspiration or simple drain.
- Development of fibrous strands: Requires large-bore chest tube and fibrinolytic therapy.
- The fluid becomes solid and jelly-like: Usually requires surgery.
- Although pneumonia is often associated with a parapneumonic effusion, most pleural effusions associated with pneumonia are not empyema but are instead a sterile effusion caused by increased capillary permeability.
- An empyema conforms to the shape of the pleural space, causing a longer air-fuidlevel on the lateral radiograph. This is in contrast to an abscess, which typically is spherical and has the same dimensions on the frontal and lateral radiographs.
- The split pleura sign describes enhancing parietal and visceral pleura of an empyema seen on a contrast-enhanced study.

What is a pneumatocele?
Etiologies?
Prognosis?
- A pneumatocele is a thin-walled, gas-filled cyst that may be post-traumatic or develop as a sequela of pneumonia, typically from staphylococcus aureus or pneumocystis.
- Pneumatoceles almost always resolve.
What is a bronchopleural fistula?
What is caused by? MCC? Other etiologies?
Imaging?
Treatment?
- Bronchopleural fistula (BPF) is an abnormal communication between the airway and the pleural space. It is caused by rupture of the visceral pleura. By far the most common cause of BPF is surgery; however, other etiologies include lung abscess, empyema, and trauma.
- On imaging, new or increasing gas is present in a pleural effusion. A connection between the bronchial tree and the pleura is not always apparent but is helpful when seen.
- The treatment of BPF is controversial and highly individualized.
What is empyema necessitans?
Most commonly due to?
Other causative organisms?
- Empyema necessitans is extension of an empyema to the chest wall, most commonly secondary to tuberculosis. Other causative organisms include Nocardia and Actinomyces.

Tuberculosis Overview
Where is this more of a problem? Who gets it in the US?
Initial TB exposure leads to what two clinical outcomes?
What is “reactivation TB”?
- Tuberculosis - TB, caused by Mycobacterium tuberculosis, remains an important disease despite remarkable progress in public health and antituberculous therapy over the past century. Tuberculosis remains a significant problem in developing countries. In the United States, TB is seen primarily in the immigrant population and immunocompromised individuals.
- Initial exposure to TB can lead to two clinical outcomes:
- Contained disease (90%) results in calcified granulomas and/or calcified hilar lymph nodes. In a patient with normal immunity, the tuberculous bacilli are sequestered with a caseating granulomatous response.
- Primary tuberculosis results when the host cannot contain the organism. Primary tuberculosis is seen more commonly in children and immunocompromised patients.
- Reactivation (post-primary) TB is reactivation of a previously latent infection.
What is primary TB? What parts of the pulmonary system may be involved?
What percent of patients infected with primary TB have no radiographic changes?
What are the imaging manifestations of primary TB? Most typical lobe involvement?
Classic imaging findings? Describe them.
Cavitation?
Adenopathy? Features?

- Primary tuberculosis represents infection from the first exposure to TB. Primary TB may involve the pulmonary parenchyma, the airways, and the pleura.
- As many as 15% of patients infected with primary TB have no radiographic changes and the imaging appearance of primary tuberculosis is nonspecific.
- The four imaging manifestations of primary TB (of which any, none, or all may be present) are ill-defined consolidation, pleural effusion, lymphadenopathy, and miliary disease.
- Primary TB may occur in any lobe, but the most typical locations are the lower lobes or right middle lobe. It can be difficult to distinguish between primary and postprimary TB, and in clinical practice, the treatment (antituberculous therapy) is the same.
- Classic imaging findings are not always seen, but include:
- Ghon focus: Initial focus of parenchymal infection, usually located in the upper part of the lower lobe or the lower part of the upper lobe.
- Ranke complex: Ghon focus and lymphadenopathy.
- Cavitation is rare in primary TB, in contrast to reactivation TB.
- Adenopathy is common in primary TB, typically featuring central low-attenuation and peripheral enhancement, especially in children. In contrast, post-primary TB does not feature prominent adenopathy.
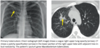
What is reactivation TB? What is it also called?
Who does it occur in?
Clinical manifestations?
What areas of the lung does it most commonly occur?
In an immunocompetent patient, what are the imaging hallmarks?
What suggests active endobronchial spread?
How about in an immunosuppressed patient?
What is a tuberculoma?
- Reactivation TB, also called post-primary TB, usually occurs in adolescents and adults and is caused by reactivation of a dormant infection acquired earlier in life. Clinical manifestations of reactivation TB include a chronic cough, low-grade fever, hemoptysis, and night sweats.
- Reactivation TB most commonly occurs in the upper lobe apical and posterior segments.
- In an immunocompetent patient, the imaging hallmarks of reactivation TB are upper lobe predominant disease with cavitation and lack of adenopathy. Focal upper lobe consolidation and endobronchial spread are common. Although not specific to TB, tree-in-bud nodules suggest active endobronchial spread.
- In an immunosuppressed patient (ie HIV), low-attenuation adenopathy is a typical additional finding, similar to the adenopathy seen in primary TB. L_ow-density lymph nodes may mimic immune reconstitution syndrome in HIV patients._
- A tuberculoma is a well-defined rounded opacity usually in the upper lobes.
What is the imaging appearance of healed TB?
What does a calcified granulma represent?
- Healed TB is evident on radiography as apical scarring, usually with upper lobe volume loss and superior hilar retraction.
- Calcified granulomas may be present as well, which indicate containment of the initial infection by a delayed hypersensitivity response.

What is miliary TB?
Does it occur in primary or post-primary TB?
- Miliary tuberculosis is a diffuse random distribution of tiny nodules seen in hematogenously disseminated TB.
- Miliary TB can occur in primary or reactivation TB.

Atypical Mycobacteria Infection
What is the classic presentation? What is the classic name for this presentation?
What are the most common organisms?
Classic radiographic findings?
- The classic presentation of atypical mycobacteria is an elderly woman with a cough, low-grade fever, and weight loss called Lady Windermere syndrome.
- Mycobacterium avium intracellulare and M. kansasii are the two most common organisms.
- Classic radiographic findings are bronchiectasis and tree-in-bud nodules, most common in the right middle lobe or lingula.

What is “Hot-tub” lung?
Typical patient population?
Imaging appearance?
- “Hot-tub” lung is a hypersensitivity pneumonitis in response to atypical mycobacteria, which are often found in hot tubs.
- There is no active infection and the typical patient is otherwise healthy.
- Imaging is similar to other causes of hypersensitivity pneumonitis, featuring centrilobular nodules.
Most patients infected with endemic fungi have what clinical outcome?
- Endemic fungi can cause community-acquired pneumonia in normal individuals, with each subtype having a specific geographic distribution. Most infected patients are asymptomatic.
Histoplasma Capsulatum
Where is this localized and in what specific vector?
What is the most common sequela of infection? Less common radiologic manifestation?
Chronic infection mimics what entity and what does this look like?
What is a rare complication of Histoplasma infection?
- Histoplasma capsulatum is localized to the Ohio and Mississippi valleys, in soil contaminated with bat or bird guano.
- The most common sequela of infection is a calcified granuloma. A less common radiologic manifestation is a pulmonary nodule (histoplasmoma), which can mimic a neoplasm.
- Chronic infection can mimic reactivation TB with upper lobe fibrocavitary consolidation.
-
Fibrosing mediastinitis is a rare complication of Histoplasma infection of mediastinal lymph nodes leading to pulmonary venous obstruction, bronchial stenosis, and pulmonary artery stenosis. Affected lymph nodes tend to calcify.
- Mnemmonic: Hisoplasma CAPsulatum can put a “cap in the mediastinum”.
Where is Coccidioides immitis found?
Radiologic appearances?
- Coccidioides immitis is found in the southwestern US and has a variety of radiologic appearances, including multifocal consolidation, multiple pulmonary nodules, and miliary nodules.







