What all acyanotic defects not result in?
A lower than normal concentration of oxygen in the blood.
Describe the frequency and types of congenital malformation of the heart and great vessels
Congenital heart defects are common with an incidence of 6-8/1000 births.
Most common types are VSDs followed by ASDs.
Other ones include Transposition of the Great Vessels (Conotruncal Septum does not adopt spiral course) and Tetralogy of Fallot.
Discuss the Aetiology of Congenital Heart Defects
~20% Genetics (e.g. Down’s, Turner’s, Marfan’s syndromes)
Environmental - teratogenicity from drugs such as antidepressants, alcohol etc
Maternal infections (during first trimester) - Rubella, Toxoplasmosis etc
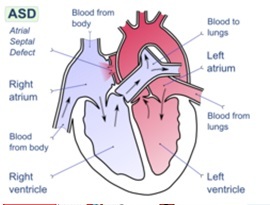
What is an Atrial Septal Defect?
An opening in the septum between the two atria which persists following birth.
Failure of the foramen ovale to close or an abnormal communication allows blood to continue to flow between the two atria postnatally.
Incidence of ~67 in 100,000 live births
What are the possible consequences of an Atrial Septal Defect?
Because left atrial pressure is normally higher than right atrial pressure, flow will mainly be from left to right and there is no mixing of deoxygenated blood with the oxygenated blood being pumped around the systemic circulation.
Therefore this is an ACYANOTIC LESION
What are the different types of Atrial Septal Defects?
Such defects can occur almost anywhere along the atrial septum but the most common site is at the foramen ovale (Ostium Secundum ASD). This defect arises from inadequate formation of the septum secundum, excessive resorption of the septum primum or a combination.
An Ostium Primum ASD occurs in the inferior portion of the septum, adjacent to the AV valves and is less common. This results from the failure of the septum primum to fuse with the endocardial cushions.
Describe a Sinus Venosus Defect
Closely related to ASDs but morphologically distinct.
This condition represents an “unroofing” defect with abscence of normal tissue between the right pulmonary vein (a) and the right atrium but is technically not a deficiency of the anatomic atrial septum (which is fully intact).
As sinus venosus defects are often large and result in flow from the right pulmonary veins and left atrium into the right atrium, the pathophysiology is similar to that of a true ASD.
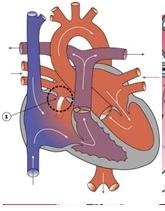
Is a Patent Foramen Ovale a true ASD?
No. The one-way valve, though not sealed, remains functionally closed.
PFOs may be present in ~20% of the population and are generally clinically silent since the higher LA pressure causes functional closure of the flap valve.
When may a PFO be clinically important/significant?
If RA pressure becomes elevated (e.g. In states of pulmonary hypertension or right heart failure) resulting in pathological right - to - left intra cardiac shunting. In that case deoxygenated blood passes directly into the arterial circulation
Also a PFO may be the route by which a venous embolism reaches the systemic circulation if pressure on the right side of the heart increases even transiently (paradoxical embolism). This occurs when thrombus in a systemic vein breaks loose, travels to the RA, passes across the PFO to the LA and then into the systemic arterial circulation.
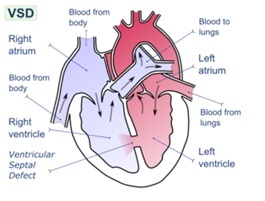
Describe a Ventricular Septal Defect
Abnormal opening in the interventricular septum. M
ost commonly occurs in the membranous portion of the septum (70%) but can occur at any point (Muscular 20%). Rare VSDs occur just below the aortic valve or adjacent to the AV valves.
Acyanotic defect
Most common congenital Heart defect
What are the consequences of a Ventricular Septal Defect?
Since left ventricular pressure is much higher than right, blood will flow from left to right.
The amount of flow depends on the size of the lesion.
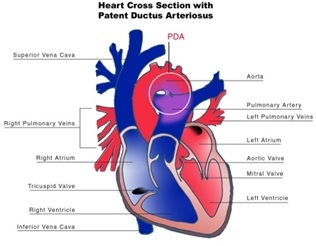
Describe a Patent Ductus Arteriosus
The DA exists in the fetus to shunt blood from the pulmonary artery to the aorta (bypassing the lungs).
This vessel should close shortly after birth as pressure in the pulmonary artery drops following perfusion of the lungs.
Failure to close leads to a PDA. Blood flow through a PDA will be from aorta to pulmonary artery after birth (high to low pressure)
A mechanical murmur is heard constantly throughout systole/diastole as pressure in the sorts is always greater than in the pulmonary artery. ACYANOTIC
Why may a Patent Ductus Arteriosus be clinically significant?
Although L to R shunting does not cause cyanosis, it can be problematic later on if untreated, with the extent of the problems depending on the degree of the shunting.
Chronic L to R shunting can lead to vascular remodelling of the pulmonary circulation and an increase in pulmonary resistance.
If the resistance of the pulmonary circulation increases beyond that of the systemic circulation, the shunt will reverse direction as pressures on the right side of the heart increase. (Eisenmerger syndrome)
What is Eisenmerger Syndrome?
The condition of severe pulmonary vascular obstruction that results from chronic left to right shunting through a congenital cardiac defect.
The elevated pulmonary vascular resistance causes reversal of the original shunt (to the right-to-left direction) and systemic cyanosis.
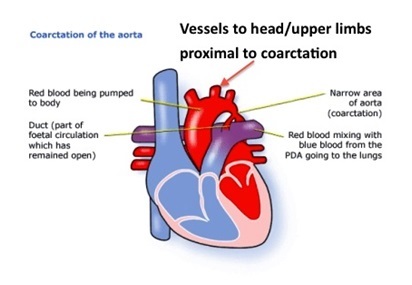
What is Coarction of the Aorta?
Narrowing of the aortic lumen in the region of the ligamentum arteriosum.
Narrowing of the aorta increases the afterload on the LV and can lead to LV hypertrophy.
Because the vessels in the head and upper limbs usually emerge proximal to the coarctation, the blood supply to these regions is not compromised. However blood flow to the rest of the body is reduced.
What does the extent of the symptoms of Coarctation of the Aorta depend on?
Depends on the severity of the coarctation. If very severe, an infant may present with symptoms of heart failure shortly after death.
In mild cases, the defect may be detected in adult life. Femoral pulses will be weak and delayed, with upper body tension.
What is Congenital Aortic Stenosis?
Most often caused by abnormal structural development of the valve leaflets.
Occurs in 5/10,000 bits.
The aortic valve usually has a bicuspid leaflet structure in congenital AS instead of the normal three-leaflet configuration, causing an eccentric stenotic opening through which blood is ejected. Most bicuspid aortic valves are non-obstructive at birth and therefore only rarely react in congenital AS.
What happens to the bicuspid aortic valves over many years?
Become progressively stenotic as the leaflets progressively fibrose and calcify.
Congenital AS represent a common cause of aortic stenosis (narrowing) in adults
What are the consequences of congenital aortic stenosis?
Because the valvular orifice is significantly narrowed, LV systolic pressure must increase to pump blood across the valve into the aorta.
In response to this increased pressure load, the LV hypertrophies.
The high-velocity jet of blood that passes through the stenotic valve may impact the proximal aortic wall and contribute to dilation of that vessel.
Describe Pulmonary Stenosis
Obstruction to right ventricular outflow may occur at the level of the pulmonic valve or in the pulmonary artery.
Valvular pulmonic stenosis is the most frequent form.
Consequence of pulmonic stenosis is impairment of right ventricular outflow which leads to increased RV pressure and hypertrophy.
Although mild pulmonic stenosis rarely progresses and is unlikely to affect RV function, untreated pulmonic stenosis typically results in findings of right sided heart failure.
What are the haemodynamic effects of a Left to Right Shunt?
Blood from the left side of the heart is returned to the lungs instead of going to the body.
Increased lung blood flow by itself is not damaging but increased pulmonary artery or pulmonary venous pressure is.
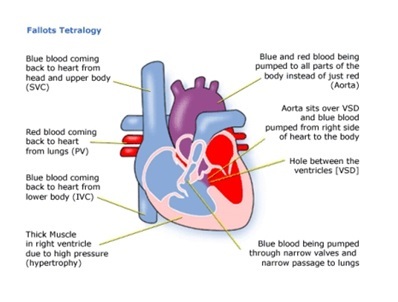
What is Tetralogy of Fallot?
Group of 4 lesions occurring together as a result of a single developmental defect which places the outflow portion of the interventricular septum too far in the anterior and cephalad directions
Four lesions: VSD, overriding aorta, a variable degree of pulmonary stenosis and right ventricular hypertrophy.
Most common form of cyanotic congenital heart disease after infancy, occurring in 5 of 10,000 live births and is often associated with other cardiac defects.
What are the consequences of Tetralogy of Fallot?
Pulmonary Stenosis causes persistence of the fetal RV hypertrophy as the RV must operate at a higher pressure to pump blood through the pulmonary artery.
The increased pressure on the right side of the heart along with VSD and the overriding aorta (receives blood from both ventricles) allow R to L shunting and mixing of deoxygenated blood with the oxygenated blood going to the systemic circulation, resulting in cyanosis.
What is the Natural History of Tetralogy of Fallot?
Present in infancy or early childhood with cyanosis or spells of cyanosis. Mild cases compatible with adulthood.
The magnitude of the shunt and level of severity depends on the severity of the pulmonary stenosis.









