The Spinal Cord is a Cylindrical column of…
Millions of nerve cell bodies (grey mater)
Millions of neuronal axons (white mater) (ascending, descending or crossing from left go fight)
Start: end of the medulla in the brain
Ends as the conus medullaris (where its membranes tapers into a ligament - filum terminale)
Runs through successive vertebral foramina of most but not all vertebrae of the vertebral column (ends roughly about L2/L3)
It is shorter than the vertebral column it is found in.
How do dermatomyotomes develop?
In association with a specific neural level of the embryonic neural tube tissue.
The neural tube is the precursor of what will eventually become the adult spinal cord.
Dermatomyotomal tissue takes its neural supply with it irrespective of where it ends up in the adult body.
Differentiated skin and muscle units of a dermatomyotome always have a common source of nervous supply.
The adult nervous supply to the dermis and muscle of a dermatomyotome is a spinal segmental nerve.
Describe the Spinal Cord + Vertebral Column
Each vertebra of the vertebral column makes 1 vertebral segment.
Cord runs through vertebral foramina of spinal vertebrae.
The successive foramina of vertebrae form “the spinal canal”
The cord gives off a pair of nerves at each vertebral level (1L and 1R)
Spinal nerves leave the spinal canal via intervertebral foramina (1L and 1R)
The nerves of the cord are also known as segmental nerves.
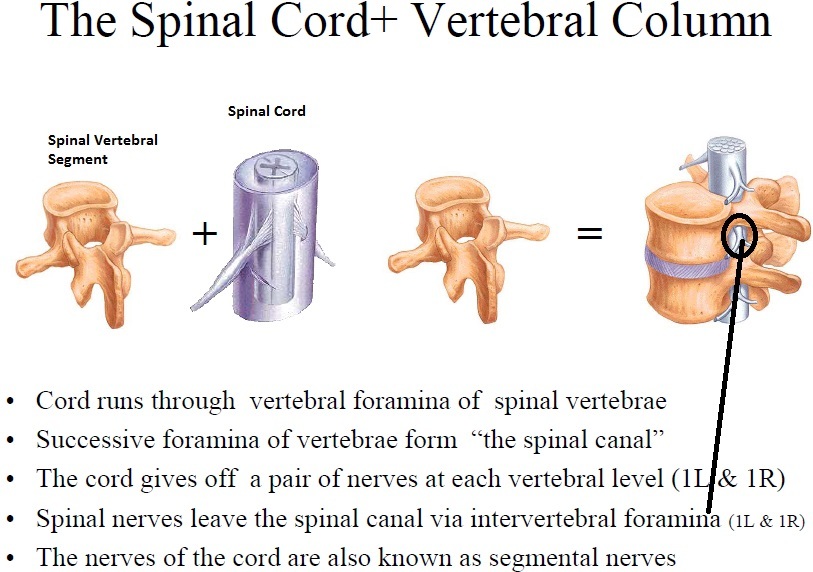
How do spinal nerves emerge from the vertebral column?
Most spinal nerves emerge inferiorly to their corresponding vertebral levels.
In the cervical cord, spinal nerves emerge SUPERIOR to their corresponding vertebral levels.
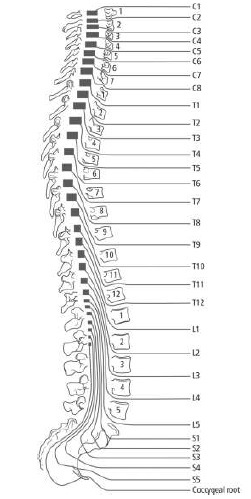
Describe the segmentation of the CNS
Each segment of nervous tissue has independence of connection (independent innervations) to the periphery.
Sensory nerves serve discrete territories of skin (sensations of the segment are fed through this route)
Motor nerves serve myotomal territories (motor instruction of the segment are mediated through the route)
Each segment has LEFT and RIGHT sides (symmetrical)
Each segment is known as a NEURAL LEVEL.
Discribe the distribution of neurones
The distribution of sensory and motoneurones varies - is not uniform - along the Rostro-caudal axis of the cord.
At each vertebral level the spinal cord gives out a pair of nerves (L and R)
Each of these nerves is known as a spinal segmental nerve.
A vertebral level is defined by the vertebral column.
A neuronal spinal level is defined by the spinal cord.
Segmental nerves are also known as Mixed Spinal Nerves
What does each Spinal Segment comprise of?
Dorsal roots (sensory/afferent)
Ventral roofs (efferent): motor roots only innervate skeletal muscle and autonomic roots innervate smooth muscle and glands.
As the mixed spinal nerve emerges through the intervertebral foramen, it divides into 2 branches (rami):
Dorsal or Posterior Ramus (small) –> the posterior ramus divides further into medial and lateral branches.
Anterior or Ventral Ramus (large) All rami contain all functional modalities for that segmental level.
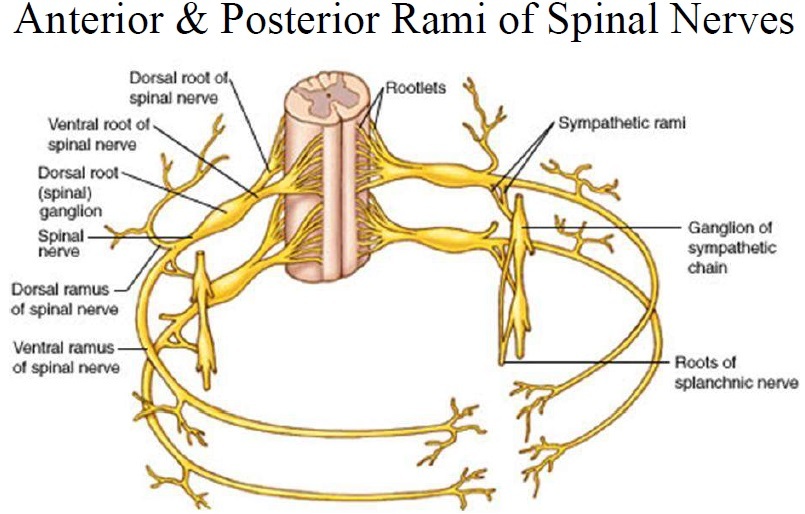
Describe the Nerve Supply to Upper Limb
It receives all its nerve supply from the spinal cord.
Most of its supply is derived from C5-T1.
The rest comes from the T2 roots. Spinal nerves (except T2) to the upper limb form a network of nerves: the Brachial Plexus.
Anterior divisions of the trunks supply anterior (flexor) compartments of the upper limb and posterior divisions of the trunks supply posterior (extensor) compartments.
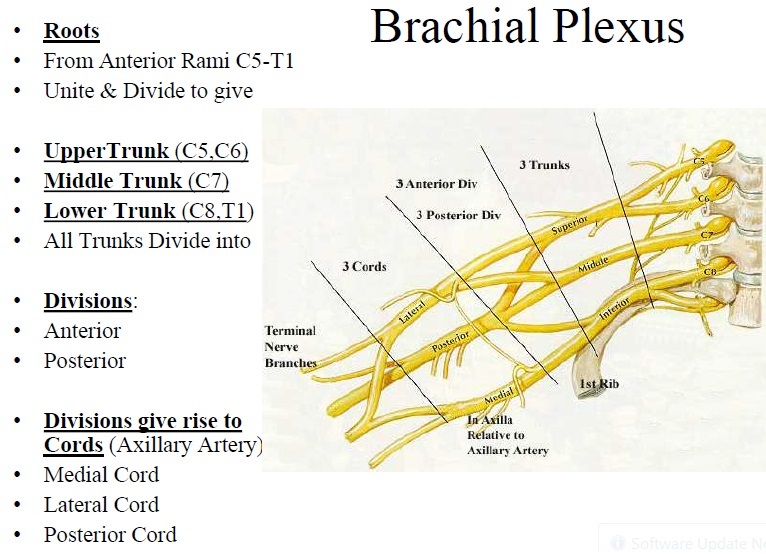
Apart from Radial, Median, Musculocutaneous, Axillary and Ulnar, what are the other nerves of the upper limb?
Lateral pectoral (C5, C6, C7)
Medial pectoral (C8, T1)
Upper subscapular (C5, C6)
Lower subscapular (C5, C6)
Dorsal scapular (C5)
Suprascapular (C5, C6)
Long thoracic (C5, C6, C7)
Describe the Nerve Supply to the Lower Limb
Supplies from the lumbar and sacral spinal segments (L1 to S4)
Spinal nerves to the Lower Limb originate from two separate networks for nerves:
The Lumbar Plexus (L1-L4 but not all of L4 - ~1/2)
The Sacral Plexus (L4 -S4)
Describe the Lumbar Plexus
Forms behind the psoas major muscle (abdominal muscle)
Nerves emerge either medial or lateral to borders of the psoas major muscle
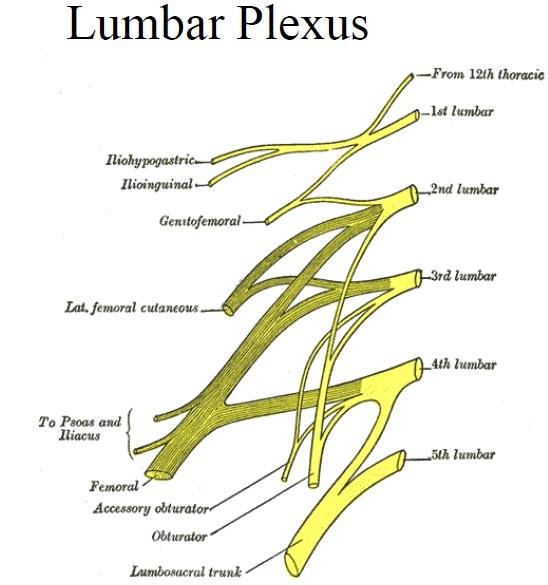
What are the Nerves of the Lumbar Plexus emerging lateral to psoas major?
The Femoral (L2-L4)
Iliohypogastric
Ilioinguinal
Lateral cutaneous nerve of the thigh
What are the nerves emerging medial to psoas major?
The obturator nerve
The lumbosacral trunk (part of lumbar plexus that joins to the sacral plexus)
What is the Sacral Plexus?
Composed of: Lumbosacral trunk (1/2 of L4 and all of L5) Sacral spinal segmental outflow (S1 - S4)
The Sacral plexus forms within the pelvic cavity. The plexus lies in relation to the piriformis.
The sacral plexus supplies: pelvic region, gluteal region, perineal region and the lower limb (via the Sciatic nerve)
What is a Dermatome?
An area of skin supplied by sensory nerve fibres from a single spinal nerve (neural level)
What does functional overlap between adjacent Dermatomes mean?
Some sections of skin are served by 2 successive spinal nerves.
Thus a typical dermatome sandwiched between others will be served by 3 successive sensory nerves
To produce a region of complete anaesthesia, at least 3 contiguous spinal nerves have to be sectioned.
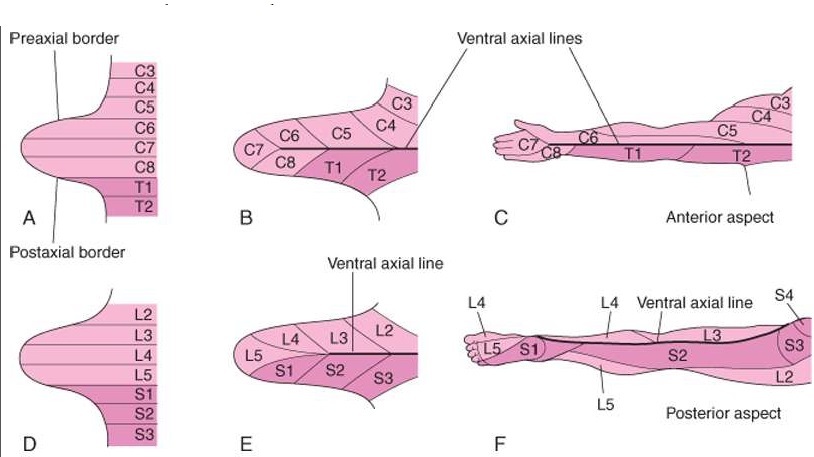
What does the axial lines of limbs mean?
The line of junction of two Dermatomes supplied from discontinuous spinal nerves is known as the axial line.
The limbs have anterior and posterior axial lines (pre and post axial borders)
The axial lines can be said to mark boundaries between the flexor and extensor compartment of the limb.
These borders are conveniently marked out by veins: Cephalic and Basilic; Great Saphenous and Small Saphenous
Describe the development of nerves
During development nerves grow into the developing limb buds.
As the limb bud increases in size, the nerves are ‘dragged’ along eith the structures they innervate thus eventually producing the adult pattern.
Each dermatome is named according to the spinal nerve which provides most of its spinal innervations.
There is considerable overlap between adjacent Dermatomes and thus section of a single dorsal spinal root does not usually lead to anaesthesia of the entire dermatome area.
The exception to this rule concerns skin areas that share a common boundary with the axial line. Here contiguous areas of skin are not innervated by adjacent spinal segments and there is no overlap across the axial line.
Describe the innervations to skeletal muscle
Can be described either at the level of a named nerve or in terms of spinal segments.
Most movements involve two spinal cord segments.
The muscles innervated by a single spinal nerve root is referred to as a myotome.
Each nerve root has many nerve cells.
Within a muscle, each axon innervates a variable number of muscle fibres.
The muscle fibres innervated by a single motor nerve fibre is called a motor unit.
The size of motor units varies considerably in different muscles.
In general terms, the smaller the muscle unit, the more precise movements it may perform.
Describe Motor Nerve innervation to the Upper Limb
Upper limb muscles usually receive motor fibres from several spinal segments or nerves. Thus, most muscles are made up of more than one myotome and multiple spinal segments are usually involved in producing the movement of the upper limb. The intrinsic muscles of the hand constitute a single myotome.
Give some examples of myotomes of the upper limb
Spinal nerves from segments C5 and C6 cause flexion at the elbow whereas spinal nerves from C7 and C8 cause extension at the elbow.
Weakness in one of those movements could indicate damage to the respective spinal nerves.
Describe the effects of lesions of the spinal nerves
Lesions of the spinal nerves close to the spinal cord cause loss of sensation in that dermatome and also loss of function in that myotome.
A more distal lesion (e.g. The axillary nerve in the axilla) cause loss of sensation in the peripheral nerve field (e.g. Axillary nerve would be the regimental badge areas); a lesion in the periphery can damage a peripheral nerve thus the patient would lose sensation and motor control beyond the point of the lesion to skin and muscle the fibres contained in the peripheral nerve innervate.
What is the Cutaneous Distribution of a Peripheral Nerve?
When nerve fibres leave the spinal cord, they travel through their spinal root and then often get redistributed via the nerve plexus (e.g. Brachial of lumbosacral plexus) and become peripheral nerves.
The CUTANEOUS DISTRIBUTION OF A PERIPHERAL NERVE is an area of skin this peripheral nerve innervates. It often has nerve fibres from several spinal roots. It is not a dermatome and should not be called as such. For example the axillary nerve innervated lateral shoulder and arm (regimental badge area)
Also known as a nerve territory


