Exam 5: Prosthetics PartFoot, Bilat, HighLE, UE ReadingGuide and Class discussion Flashcards
(73 cards)
What are 8 disarticulation/transection surgeries used in the foot?
- Forefoot
- Digit (metatarsophalangeal disarticulation of one digit)
- Ray (tarsometatarsal disarticulation of one ray)
- Transmetatarsal (cut through metatarsal bones)
- Midfoot
- Lisfranc (tarsometatarsal disarticulation)
- Chopart (midtarsal disarticulation)
- Hindfoot
- Syme’s (disarticulation of the talocrural joint; tarsotibial disarticulation)
- Two more that are similar to Syme’s functionally, but rarely used on adults:
- Pirogoff (wedging transection of the calcaneus, followed by bony fusion of the calcaneus and distal tibia with all other distal structures removed)
- Boyd (calcaneus remains largely intact rather than being wedged before arthrodesis with the tibia)
What are 3 forefoot amputations?
- Forefoot
- Digit (metatarsophalangeal disarticulation of one digit)
- Ray (tarsometatarsal disarticulation of one ray)
- Transmetatarsal (cut through metatarsal bones)
What are two midfoot amputations?
- Midfoot
- Lisfranc (tarsometatarsal disarticulation)
- Chopart (midtarsal disarticulation)
What are three hindfoot amputations?
- Hindfoot
- Syme’s (disarticulation of the talocrural joint; tarsotibial disarticulation)
- Two more that are similar to Syme’s functionally, but rarely used on adults:
- Pirogoff (wedging transection of the calcaneus, followed by bony fusion of the calcaneus and distal tibia with all other distal structures removed)
- Boyd (calcaneus remains largely intact rather than being wedged before arthrodesis with the tibia)
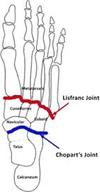
What is a Chopart amputation?
- A Midfoot amputation
- Disarticulation of the Talocalcaneonavicular joint (midtarsal disarticulation)
- Separates the talus and navicular as well as the calcaneus and cuboid.

What is a lisfranc amputation?
- A midfoot amputation
- Separates the three cuneiform bones and the cuboid bone from the five metatarsal bones (tarsometatarsal disarticulation)
What is a Transmetatarsal amputation?
- Forefoot amputation
- Cut through the metatarsals (metatarsal transection)

What is a ray resection?
- a forefoot amputation
- Removal of one Ray (tarsometatarsal disarticulation of one ray)

What is a digit amputation?
- A forefoot amputation
- Removal of one Digit (metatarsophalangeal disarticulation of one digit)

What is a Syme’s Amputation? (simple)
- A hindfoot amputation
- A disarticulation of the ankle
- Syme’s (disarticulation of the talocrural joint; tarsotibial disarticulation)
- Retains and re-attaches the heel pad

What are two hindfoot amputations besides the Syme’s and when are they used?
Two more that are similar to Syme’s functionally, but rarely used on adults because there is not enough room to put prosthetic foot under the residual limb):
- Pirogoff (wedging transection of the calcaneus, followed by bony fusion of the calcaneus and distal tibia with all other distal structures removed)
- Boyd (calcaneus remains largely intact rather than being wedged before arthrodesis with the tibia)
Sometimes used in children (I assume because RL side will not grow while soudn side continues to grow and there will be more room for a foot underneath the residual limb)

Describe a typical partial foot amputee who lost it due to vascular insufficinecy (4)
- Pt typically has vascular insufficiency (still)
- is usually between the ages of 60-70 years,
- has compromised proprioception and sensation, and has
- weak lower limb musculature.
Describe typical gait limitations for individuals with partial foot amputations, especially in the presence of vascular disease. (3 main with several sub-points)
- May be able to ambulate without a prosthesis
- Slow gait velocity, Inefficient, somewhat dysfunctional gait
- May compensate for unstable knees due to weak quads and impared prorprioseption by keeping knee extended during loading response.
- (bad b/c it causes extra force on joints)
- Has lost forefoot lever arm
- Abrupt unloading from premature toe break and forefoot collpase
- (short contralateral stride length)
- Higher pressure on residual foot
- Abrupt unloading from premature toe break and forefoot collpase
- May compensate for unstable knees due to weak quads and impared prorprioseption by keeping knee extended during loading response.
- Plantar Flexion contracture common
Describe typical gait limitations for individuals with partial foot amputations, especially in the presence of vascular disease:
- what are two things that contribute to Slow gait velocity, Inefficient, somewhat dysfunctional gait (and what are some consequences)?
- Slow gait velocity, Inefficient, somewhat dysfunctional gait
- May compensate for unstable knees due to weak quads and impared prorprioseption by keeping knee extended during loading response.
- (bad b/c it causes extra force on joints)
- Has lost forefoot lever arm
- Abrupt unloading from premature toe break and forefoot collpase
- (short contralateral stride length)
- Higher pressure on remaining residual foot
- Abrupt unloading from premature toe break and forefoot collpase
- May compensate for unstable knees due to weak quads and impared prorprioseption by keeping knee extended during loading response.
What is a bad thing that can happen if a partial foot amputee compensates for poor knee control by keepign knee extended during loading response?
- this sacrifices shock absorption at knee and hip, increasing the likelihood of cumulative joint trauma at hip and knee.
How is compromised forefoot support related to higher energy costs?
Compromised forefoot support increases center of gravity displacement. A penalty of higher energy cost results.
Explain the relationship between forefoot rocker and peak dorsiflexion in partial foot amputees and walking velocity
Walks with significantly slower velocity (Delay in forefoot rocker, delay in peak dorsiflexion)
Expalin why peak vertical GRF are higher for the sound limb in someone who has a partial foot amputation
There is an abrupt and prmature unloading of the amputated side during late stance and body-weight must transfer quickly to the sound side.
- Amputated side has
- premature toe break and forefoot collapse
- Fear, insecurity, and pain aggravated by increases pressure near the amputation site collectively create an abrupt transfer of weight to the sound side, thus increasing the magnitude of the initial vertical force peak.
**this also reduces the step length of the sound side
What is the relationship etween the plantar surface-area of the forefoot and the magnitude of pressure that is on the foot?
As plantar surface area of the supporting forefoot is reduced the magnitude of the pressure is increased.
What is the consequence of a plantarflexion contracture in someone with a partial foot amputation?
Pts with partial foot amputation frequently have plantar flexion contracture develop from muscle imbalance.
- any PF contracture, in turn, increases pressure at the distal residual limb during terminal stance, causing discomfort, pain, and risk of ulceration
What happens to a shoe if it is worn by a partial foot amputee without prosthetic replacement?
Shoes worn without prosthetic replacement of the missing forefoot quickly become disfigured (collapse at the toe break)
Name the areas of the residual foot most vunerable to tissue damage during walking. (f4)
- Distal end, first and fifth met heads
- navicular,
- malleoli
- tibial crest (front, shin-bone area I think)
Describe two actue prosthetic options for someone with a partial foot amputation? (not symes as far as I can tell)
Neuropathic walker developed at Rancho Los Amigos locks the ankle in custom molded, foam lined, thermoplastic AFO. Rocker bottom is contoured
- provides optimum protection for insensate foot
- Helps with first priority immediately after amputation: to protect the remaining tissue.
Custom shoe insert with in-depth or post op shoe for people with adequate protective sensation
What is the top priority just after a partial foot amputation is performed due to dysvascular issues?
first priority immediately after amputation: protect the remaining tissue.






