S3) Anatomy of the Abdomen Flashcards
(50 cards)
State the structure and functions of the mucosal epithelial layer

- Structure: selectively permeable barrier
- Function: promote absorption, produce hormones and mucus, facilitate transport and digestion of food
State the structure and function of the mucosal lamina propria
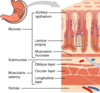
- Structure: lots of lymphoid nodules and macrophages
- Function: produce antibodies (mainly IgA)
State the structure and functions of the muscularis mucosae

- Structure: layers of smooth muscle orientated in different directions
- Function:
I. Keeps epithelium in contact with gut contents
II. Keeps crypt contents dynamic
Describe the structure of the submucosa of the gut

- Contains dense connective tissue, blood vessels, glands, lymphoid tissue
- Contains submucosal plexus (Meissner’s)
Describe the contents of the inner circular muscle layer

Contains myenteric (Auerbach’s) plexus
Describe the structure of the serosa in the gut

- Continuous with mesenteries
- Contains blood and lymph vessels and adipose tissue
What kind of epithelia is found in the gut?
- Stratified squamous (oesophagus and distal anus)
- Simple columnar (everything else)
What is an enterocyte?
An enterocyte is a simple columnar epithelial cell that absorbs nutrients

The enterocyte is the most predominant cell in the small intestine and lumen.
Describe it structure
- Consists of apical and basolateral membranes
- Blood vessels/lymphatics lie immediately below cell
How are enterocytes adapted for their absorbative function?
Microvilli (collectively termed brush border)

Where are goblet cells found?
- Scattered in between enterocytes
- Increase in number from duodenum to colon

Describe the structure of the goblet cell
- Narrow base (mucus compresses nucleus to its base)
- Larger apical size

Goblet cells secrete mucus.
What are the three main functions of mucus?
Protects epithelia from:
- Friction (acts as lubricant)
- Chemical damage (acidic environment)
- Bacterial inflammation (forms physical barrier)
Where are gastric surface mucous cells found?
Gastric surface mucous cells line gastric mucosa/gastric pits

What do gastric surface mucous cells do?
Secrete mucus/HCO3 that forms barrier to stomach acid
How is the gut tube adapted for the increased surface area required for absorption?
- Permanent folds
- Villi
- Microvilli
Why does the stomach form temporary folds?

- The stomach needs to be easily expandable
- Temporary folds form called rugae
Crypts are found in the small intestine and colon.
What type of cells do they contain?
Contain specialised cells:
- Stem cells
- Paneth cells
- Enteroendocrine cells
What are stem cells?
Stem cells are cells that reside in crypts that constantly divide to replace epithelia

Where are paneth cells found and what do they do?
- Location: base of crypts
- Function: secrete antibacterial proteins to protect stem cells

How can paneth cells be identified?
Paneth cells contain vesicles which stain red

Where are enteroendocrine cells found and what do they do?
- Location: deeper in crypts and gastric glands
- Function: secrete hormones that control the function of the gut e.g gastrin, CCK, secretin
Briefly, identify states where crypts are affected by inflammatory bowel disease
- Crypt alteration
- Cryptitis – inflammation of wall
- Crypt abscess – neutrophils in lumen
Describe the organisation of glandular tissue in the gut
- Organised secretory cells – acini and tubules
- Connected to a duct
















