Inspiratory reserve + Tidal volume=
Expiratory reserve volume + Residual volume=
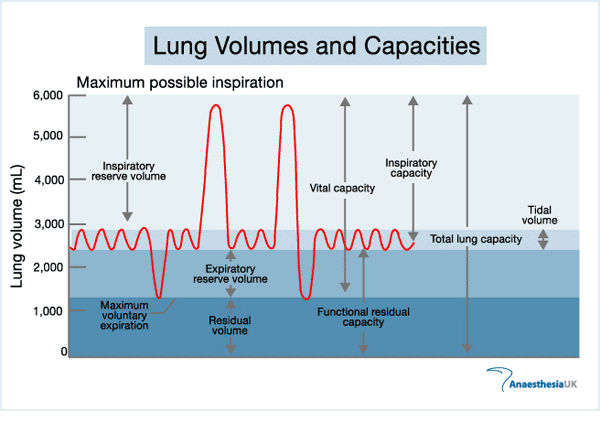
Inspiratory reserve + Tidal volume= Inspiratory capacity
Expiratory reserve volume + Residual volume= Functional residual capacity
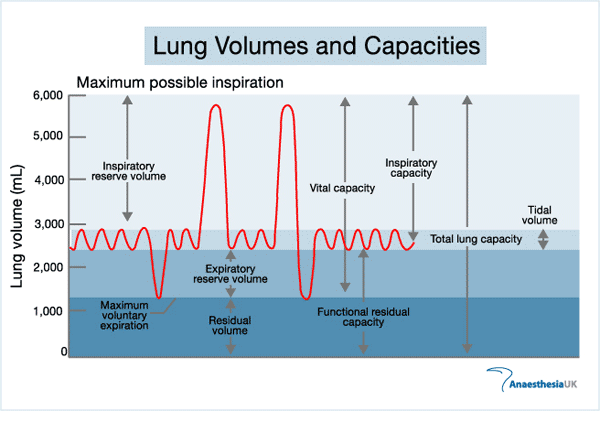
Tidal volume + Inspiratory reserve volume + Expiratory reserve volume =
Tidal volume + Inspiratory reserve volume + Expiratory reserve volume = Vital capacity
Atmospheric pressure =
Plural pressure at rest =
zero
negative
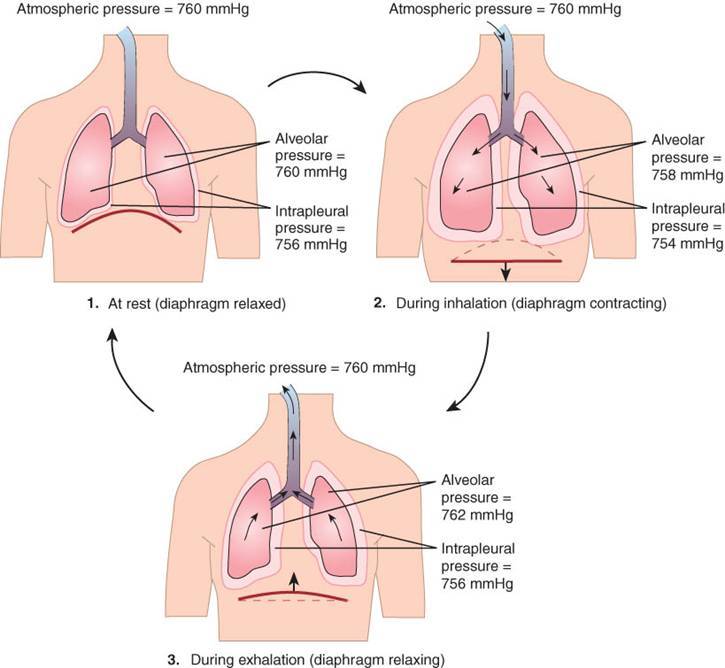
Define Transpulmonary pressure: Ptp
Palv-Ppl
What happens during inspiration in the lungs?
Hint: start with muscles cnx and how that changes volumes and pressures
Diaphragm and intercostals cnx–> thorax EXpands–> Ppl becomes more Subatmospheric (more negative)–> will cause INCREASE of Transpulmonary pressure –> Lungs expand–> Palv becomes subatmospheric–> air into alveoli
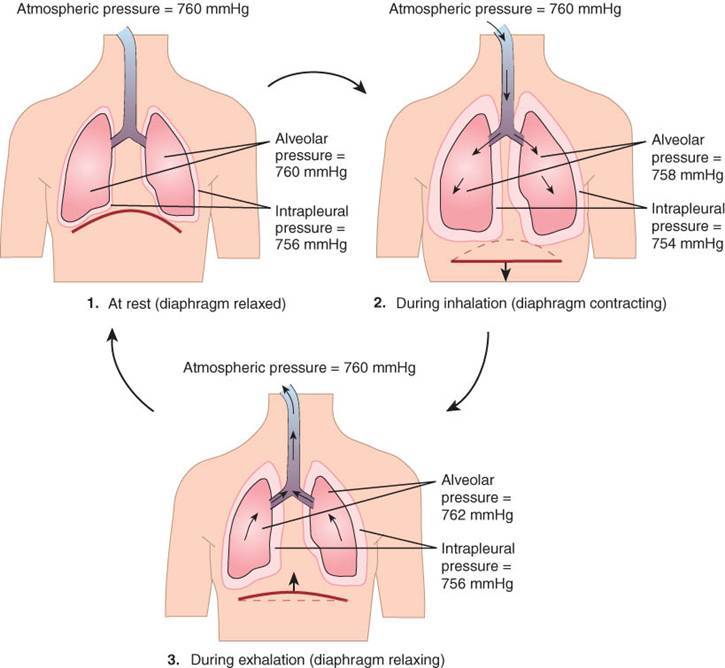
We must genenerate a ____ pressure in the alveoli to get air to rush in
Negative pressure (does this after lungs expand)
What determines airflow, particularly during expiration?
Flow =
Palv-Patm /airway resistance
Thus RESISTANCE big determining factor and changes across lengthand diamter of airway
What can you deduce from this graph about the size of bronhci and the resistance?
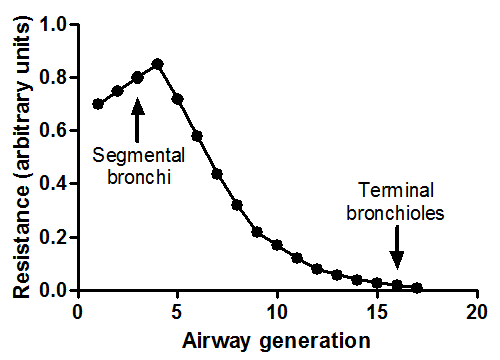
Key is HIGH resistance in the medium sized bronchi around 5-10 generations; less of a total cross sectional area. As we get to higher generations, resistance much lower
At low lung volumes, airway resistance is ______
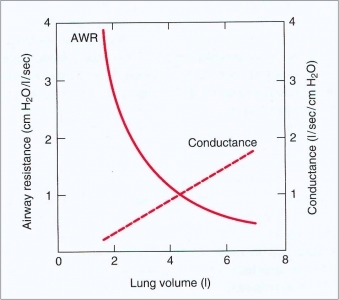
HIGH, increasing lung volume increases x-section and decreases resistance.
Resistance and xsection have inverse relationship
The tip of this curve is what:
What is it defined by?
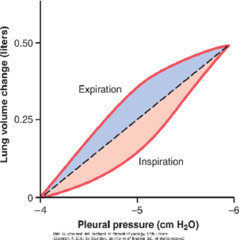
Point of zero airflow
Ptp = Ppl
When looking at this graph, what does the slope represent?
Ptp =
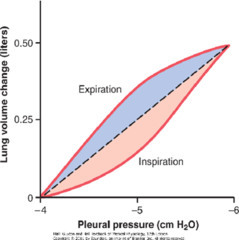
Compliance
Ptp = Palv = Ppl
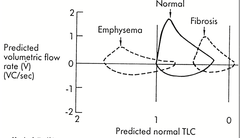
What do we see in emphysema and fibrosis in a Vital capacity vs pressure graph?
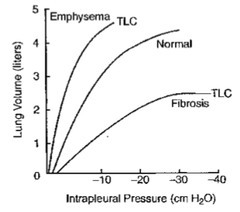
Empysema requires less pressure generated to get to TLC
In fibrosis, you need a larger change in pressure to generate change in volume
Why do lines A, B and C meet at around 4 liters of expired air?
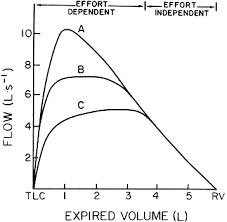
Past a certain point, expiration is effort independent, doesn’t matter how hard you blow out.
What is the pattern of the pressure in the alveoli as it moves towards bronchus?
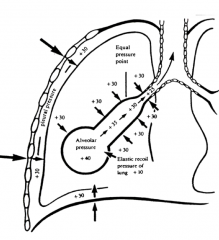
We see pressure inside alveoli dissipates
starts at +40 while the pressure exerted against it is +30…
as we get closer to bronchus, pressure decreases and is more likely to collapse
Indications for PFTs
Indications for PFTs
• Diagnostic: Symptoms, signs, abnormal lab tests
• Assess the effects of diseases and therapies
• Screening: Smokers, occupational exposures, preoperative risk, disability, prognosis
START WITH SPIROMETRY
You’re on rotations and your attending calls you over and shows you a spirometry and asks you a dx… what’s your repsonse?
tell her you need the pt history as well.. can’t dx with spirometry alone!
What is going on in the Volume Time curve
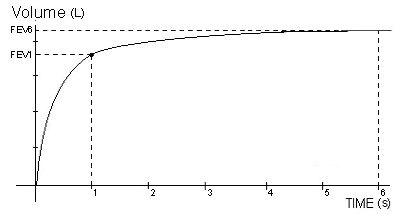
Just showing us that the peak is air you are expiring. You reach a peak after 1 sec and slowly decreases after that. Most people reach residual volume at 6 seconds
Any structures that are affecting airflow inside the chest or intra-thoracic will affect _____
Structures outiside the chest (extra-thoracic) will affect _____
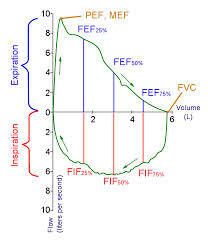
expiration
inspiration
At ____the inspiratory and expiratory flow rates should be about the same
50% vital capacity
Focusing on the expiratory phase (part on top) how is obstructive disease different then normal?
Restrictive?
Obstructive has a scalloped expiratory flow… result of air trapping. You can’t blow air out as fast.
Restrictive: you cannot bring in as much air, no issue on expiration
Which image shows fixed upper airway obstruction with flow limitation and flattening of both the inspiratory and expiratory limbs of the flow-volume loop.
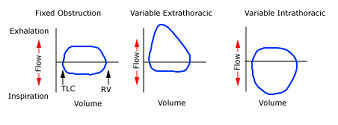
One on far left
Could patient with COPD have a loop pattern like the one of the far left?
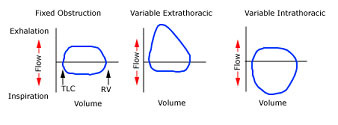
The diagram shows fixed upper airway obstruction as flow is limited in both inspiration and expiration.
This immediately rules out intrathoracic pathology – COPD and pulmonary fibrosis.
panel shows dynamic (or variable, nonfixed) extrathoracic obstruction with flow limitation and flattening of the inspiratory limb of the loop.
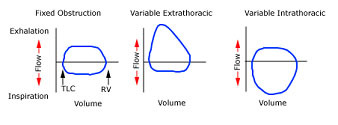
Middle loop = Vairable extrathoracic issue





