In order for cells to survive, what must they do in regards to ECF? What is the control of this ECF/ H2O/ Na+ stores in the body?
- Cells need to maintain ECF within well defined limits.
- Gi tract will contribute to the amount of H20 in the body as well as Na+ ect. But kidneys are the main control center of water and salt maintenance.
What is the main control center of water and salt maintenance? What enables mammals to survive in variable conditions?
- kidneys are the main control center of water and salt maintenance.
- Kidneys enable mammals to survive in variable conditions.
Where is urine modified?
kidneys
What is the blood supply of the kidneys? Where does it come from?
Renal artery -> comes from the aorta
What are the functions of the kidneys?
- Filtration of blood
- Production of urine
- reabsorption of filtered substances adjusting salt and water excretion to maintain constant ECF volume and osmolality.
- Excretion of met wastes and xenobiotics
- Water/ acid-base
- production of glucose (gluconeogenesis)
- endocrine fxn
Will dialysis allow for all kidney functions to occur?
No, only allows for:
• Filtration of blood
• Production of urine
• reabsorption of filtered substances adjusting salt and water excretion to maintain constant ECF volume and osmolality.
What are some signs of kidney dysfunction in a 13 year old cat ?
- PU/PD, Vomiting (accumulation of urea/ substances that would be excreted by kidneys)
- Clinical exam: pale mm, both kidneys feel small upon palpation (decrease size with chronic disease) . Hematocrit 21% (decrease erythropoietin) , Creatinine 7.5.
- animal cannot concentrate urine
What is calcitriol?
Stimulated by PTH in response to hypocalcemia.
What is Renin?
Hormone activator, renal regulation of blood pressure, essential part of renin angiotensin aldosterone system (RAAS)
What is erythropoietin?
Hormone (glycoprotein, growth factor) essential for erythropoiesis.
How is calcitriol synthesized?
From food or the conversion of UV rays ( 7-dehydocholesterol. This is then converted to Vitamin D3 -> which is then converted by 25-hydroxylase in liver to 25(OH)-Vitamin D3 -> then 1-hydroxylase in kidney will convert 25(OH)-Vitamin D3 to 1,25(OH)20Vitamin D3 (Calcitriol)
What is a protein involved in calcium absorption that is synthesized from vitamin D?How is it synthesized/ how is calcium brought into cell and removed from cell?
• Calbindin is one of the proteins synthesized by Vitamin D
Vitamin D binds to receptor which then will go to nucleus. mRNA will leave nucleus to synthesize protein (i.e Calbindin). Calbindin will take the calcium from apical membrane and transfer it to basolateral membrane. We have calcium channels at the membrane. Stimulation of ATPase will pump calcium out into the blood.
What triggers renin?
• Renin is triggered by acute drop in plasma volume and blood pressure.
What does renin do?
• Renin is a hormone that will activate the angiotensinogen and will shorten (removing the last 4 AA) which will give you an angiotensin I.
◦ A converting enzyme (mainly found in lung) will then cut last 2 AA off, and will give you Angiotensin II. Angiotensin II has 8 AA.
What is erythropoietin? What can trigger it aside from low RBC?
- Erythropoietin is essential for new RBC formation.
- Can be triggered by high altitude.
How does erythropoietin influence RBC formation?what occurs if this synthesis does not
- Erythropoietin will go to the bone marrow and will find committed erythroid precursors which will mature and will end up making mature erythrocytes at the end.
- If that doesn’t work patients will develop anemia.
What are the main parts of the Kidney? What is the functional unit of the kidney?
Cortex and Medulla. functional unit is nephron
What can be found in the cortex? In the Medulla?
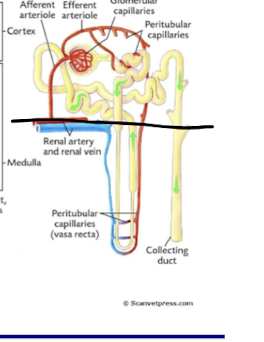
- Black line is approximate border of cortex and medulla. In the cortex you will find afferent and efferent arterioles, glomerular capillaries, peritubular capillaries, collecting ducts, ect Straight part of henlees loop is in the cortex, Straight ascending has partial in medulla and partial in the cortex.
- In medulla you will find peritubular capillaries collecting ducts. Thin segments of henlees loop are found in the medulla.
How many nephrons care found in the canine kidney? Feline? Cow?
Dogs: 400,000
Cats: 190,000
Cows: 4 million
Can nephrons be replaced?
no, only partially regenerated.
What are the 2 types of nephrons? Where are they found?
◦ Cortical nephrons: cortex, short loops of henlee, and are supplied by peritubular capillaries.
◦ Juxtamedullary nephrons: located near cortex/medulla junction, efferent arterioles give rise to long straight capillaries (vasa recta) that descend into renal medulla. Extremely long loops of henlee ( critical for urine concentration)
What are malphigahian bodies? what is it consisted of?
• Malpighian bodies: located in renal cortex, consists of glomerulus (capillaries) surrounded by bowmans capsule (double walled capsule)
What are the proximal tubules?
• Proximal tubule: longest part of nephron, consisting of a proximal and convoluted tubule and straight part
What is the loop of henlee?
• Loop of henlee: consists of thick descending limb ( extending into renal medulla), thin descending limb, thin ascending limb (only nephrons which have long loops( juxtamedullary nephrons)) and thick ascending limb (TAL, macula densa)











