Jacewicz - ANS Flashcards
Where are the secondary neurons of the SYM system?
- Interomedialateral gray matter of the T1-L3 spinal cord
NE is the neurotransmitter at the NN endings of…?
Post-ganglionic SYM fibers
47 F with several week hx of difficulty swallowing, excess saliva, and hoarse voice. Prescribed only a drug for the excess saliva. Progresses to lightheadedness and syncope. Orthostatic hypotension. Dysarthric. Fasciculations of left tongue, and other left-sided neuro symptoms in arm.
What category of med did doc prescribe to reduce drooling? What add’l workup should have been requested at first presentation? What is anatomical dx?
- MED: cholinergic antagonist bc DEC activity of salivary glands via inferior and superior salivatory nuclei (CN 9 and 7)
- ADD’L WORKUP: CT of the head, MRI of the head (best option bc produces greatest resolution of head structures), ENT consult
- ANATOMICAL DX: lesion in left lower brain stem; fasciculations mean LMN lesion
1. Brain stem ependymoma in this case
67 M with left eyelid drooping slightly and left pupil smaller than right. Medial aspect of hand numb, and clumsiness controlling fingers of left hand. Slight flushing and dryness of left face compared to right. Lots of cigarette exposure and chronic cough.
What is your anatomic dx? What is the syndromic dx?
- ANATOMIC: C8-T1 left nerve root lesion
- SYNDROMIC: Horner’s syndrome
What are Argyll Robertson pupils?
- Bilateral small pupils that DEC in size on a near object (accommodate), but do NOT constrict when exposed to bright light
- This is a highly specific sign of neurosyphilis (and may also be a sign of diabetic neuropathy)
- Mechanism unclear, but due to damage to the pretectal nuclei in the midbrain
What is Adie pupil?
- Tonically dilated pupil that reacts slowly to light, but shows a more definite response to accommodation
- Caused by damage to peripheral pathways to the pupil (PARA neurons in the ciliary ganglion that cause pupillary constriction to bright light and with near vision)
1. Usually via viral/bacterial infection that damages postganglionic PARA nerves - NOTE: loss of pupillary light reflex when the rest of the ocular function is preserved is a warning sign for stroke/aneurysm
What is the key difference b/t somatic and ANS efferents?
- ANS is comprised of 2 efferent neurons: pregang and its fiber, and a postganglionic neurons and its fiber that innervates smooth muscle, cardiac muscle, or glands
1. Innervation of smooth muscle permits regulation of functions like BP and peristalsis
2. Innervation of glands regulates secretions from salivary lacrimal and other glands
3. Innervation of cardiac muscle controls heart rate and the force of heart muscle contraction - In the somatic motor system, however, 1 LMN sends its axon directly to innervate its target organ, the skeletal mm

What are the 3 divisions of the ANS and their pre- and postganglionic neurotransmitters?
- 1) SYM (thoracolumbar system): pre- is Ach, and postgang is NE
a. Exceptions: postgang of sweat glands and erector pili mm is Ach, and adrenal receives direct, preganglionic innervation with Ach - 2) PARA (craniosacral system): pre- and postgang NT is acetylcholine (Ach)
- 3) ENTERIC: variety of neurotransmitters + neuropeptides
How do the SYM and PARA affect the eyes, glands, heart, arterioles, lungs, and GI tract (table)?

How do the SYM and PARA affect the pancreas, liver, adrenal, ureter/bladder, and repro erectile tissue (table)?

Where does a secondary SYM neuron originate in the spinal cord? Describe its path to the paravertebral ganglion, and subsequent 3 potential paths.
- Secondary neuron originates in interomediolateral (lateral horn) zone of spinal cord gray matter
- Exits spinal cord via ventral root, travels through short segment of peripheral NN before entering white communicating ramus to gain access to paravertebral SYM chain ganglia
- Within paravertebral ganglia chain:
1. It may synapse immediately with a tertiary noradrenergic neuron, which sends its axon back to peripheral nerve via the gray communicating ramus
2. May travel rostral or caudal in the chain before synapsing on a tertiary noradrenergic neuron
3. May exit the chain to synapse in a more peripherally located prevertebral ganglion

What 5 nuclei are associated with the PARA system? Where are they located in the brainstem?
- MIDBRAIN:
1. Edinger- Westphal nucleus - PONS:
1. Superior salivatory nucleus: pontine tegmentum
2. Inferior salivatory nucleus: dorsal pons, near the medulla (just below SSN) - MIDDLE MEDULLA
1. Dorsal motor nucleus
2. Nucleus ambiguus

What are the 5 PARA system nuclei (and spinal cord location), and their functions?
- EDINGER-WESTPHAL: in midbrain, and send fibers via CN III to ciliary ganglion; controls pupil constriction
- SUPERIOR SALIVARY: in pontine tegmentum (floor), and sends projections via CN VII to the pterygopalatine ganglion that controls lacrimal gland & submandibular ganglion that controls secretion of the salivary glands
- INFERIOR SALIVARY: just below SSN in dorsal pons near medulla, and projects via CN IX to otic ganglion that controls parotid gland secretion
- DORSAL MOTOR and NUCLEUS AMBIGUUS: send projections via CN X to ganglia in their targeted organs, incl. heart and gut -> DEC HR, constrict bronchial tree, dilate intestinal blood vessels, and INC peristalsis
- PARA outflow from S2-S4 innervates descending and sigmoid colon, rectal and bladder sphincter muscles, the prostate, and other genital organs
- NOTE: long projection of preganglionic and relatively short projection of postganglionic NN to their targets (in contrast to SYM system)

Describe the organization of the enteric component of the ANS.
- Activity of intestines partially regulated by CNS via PARA and SYM innervation
- Gut also has separate set of local neurons that create two networks, and function mostly independent of central ANS:
1. Myenteric (Auerbach’s) plexus: regulates gut smooth mm and motility; b/t longitudinal and circular mm layers
2. Submucosal (Meissner’s) plexus: regulates glandular secretions and intestinal absorption; beneath circular mm layer - Many intestinal functions, like peristalsis and glandular secretions occur near normally in absense of input from the ANS
- NOTE: final common pathway of gut motility is through the enteric nervous system with Ach as the effector NT

What are the key concepts/differences b/t the PARA and SYM signaling systems?
What are the chief types of NN fibers used by both systems?
- PARA: 1o neuron in brainstem or lateral horn of S2-S4 with long axon; after ganglion cell is reached, short projection to target (ganglion cells in myenteric plexus in the gut)
1. Long pre, short post - SYM: all efferent, but afferent fibers run along with them; 1o cell bodies from lateral horn in T1-L2, then synapse pretty soon (in paravertebral ganglia)
1. Short pre, long post - NN fibers:
1. Preganglionic: Group B (lightly myelinated)
2. Postganglionic Group C (unmyelinated)
50-y/o heavy smoker who devos back pain and weight loss, then weakness in legs, and then inability to walk. Legs are flaccid, and there is a sensory level at L2. Huge mass in lower abdomen that is hard.
Dx? Will this affect his urinary continence? How?
- PMC coordinates micturition by INH ONUS nucleus in ventral horn (external, striated sphincter)
- Also INH T12-L1 SYM internal sphincter (only in men)
- Stimulates detrusor muscle via PARA to empty bladder
- This man will initially present with oliguria (complete urinary retention) b/c no PARA innervation to promote emptying; will require daily catheterization to empty the bladder
What is going on here? Describe the SYM innervation of the eye, and what types of lesions may cause this syndrome.

- HORNER’S SYNDROME: ptosis (drooping eyelid) and meiosis (constricted pupil) -> due to lesion of SYM fibers at any pt from hypothalamus to ciliary NN
1. Lesion is ipsilateral
2. If CENTRALLY placed (i.e., brainstem or spinal cord), you would expect loss of sweating (anhidrosis) over entire left side of body since all SYM function below the lesion would be lost
2. If lesion were PERIPHERAL, i.e., at T1-T2 NN root, or more distally placed, you would expect a loss of sweating only of left face, head, and neck - SYM: innervates dilator mm of iris and tarsal mm of the eyelid; 1o SYM neurons originate in hypothalamus, then pass through brainstem and spinal cord (green) to T1 level, and synapse in interomediolateral gray
1. Exit to eye at T1-T2, enter paravertebral ganglion w/synapse #2 in superior cervical ganglion
2. 3o (postganglionic ) neuron travels in carotid sheath, and enters SYM fibers in calvarium with carotid artery; travel along short/long ciliary NN to reach tarsal mm and dilators of iris

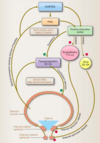
Briefly describe ANS control of CV function.

- BARORECEPTORS (mech pressure): in heart and major blood vessels, and provide info about BP to nucleus of solitary tract via CN IX and X
1. Sensory bipolar neurons conveying this info are in inferior ganglia of CN IX and X (red arrow); afferents travel in IX and X (image only shows X) - CHEMORECEPTORS: in carotid body, and provide info on conc of O2 and CO2 in blood to solitary nucleus via CN IX and X
1. Interneurons connect solitary nucleus to nuclues ambiguus and dorsal motor nucleus of vagus (X), which send efferent PARA fibers to heart
2. Solitary nucleus also connects to midbrain SYM neurons that send efferent fibers to the heart

Describe ANS bladder innervation and control.

- Voluntary (cortical) and involuntary (autonomic) control
- PAIN/TEMP: travel w/SYM and PARA fibers to spinal cord, cross midline, and travel w/spinothalamic tract
- FULLNESS: sensed by mechanoreceptors in bladder wall, transmitted to spinal cord via PARA fibers, and then on to thalamus/cortex via spinothalamic tracts
1. VERY FULL: mechanoreceptors in bladder trigone; travel to thalamus/cortex via post columns - DETRUSOR: PARA causes emptying, and SYM causes it to relax, allowing it to fill with urine
- INTERNAL URETHRAL SPHINCTER: only in males, and SYM causes contraction of sphincter mm, closure of urethra, and urine retention
- PMC (pontine micturition center):
1. To store urine, stimulates SYM relaxation of detrusor (way station for cortical voluntary control); stimulates SYM contraction of internal sphincter
2. To empty bladder, stimulates PARA contraction of detrusor, INH SYM relaxation of detrusor, INH SYM contraction of internal sphincter in males and INH voluntary control of external sphincter - NOTE: up to age 3, bladder empties by reflex (controlled by PMC), then medial surface of superior frontal gyrus develops voluntary control over PMC
Describe the autonomic and somatic control of sexual function (engorgement, ejaculation, orgasm).
- SOMATIC: pudendal N (S2-S4) innervates perineum, incl. genitalia -> sensory info from erogenous areas and voluntary motor info to pelvic floor mm (rhythmic contraction part of orgasm in M and F)
- VISCERAL: innervates blood vessels/glands -> erection, vaginal lubrication; emission, ejaculation in M
- ENGORGEMENT: penile erection psychogenic (SYM T12-L1) and usually INH by higher centers, or dependent on sensory input via pudendal N (S2-S4) to PARA (S2-S4) -> can lead to reflex erection independent of descending influences (PARA can also be activated by descending influences from cortical areas activated via o/erotic sensory influences)
1. F: vaginal lubrication, engorgement of erectile tissue mediated by autonomic fibers, mostly by an INC in PARA tone - EJACULATION: preceded by seminal emission phase in M, which incl. sperm transport, formation of seminal fluid, and closure of bladder neck to prevent retrograde ejaculation -> controlled by SYM (T12-L1)
1. Next stage is expulsion of sperm, which is mediated by PARA (S2-S4), and incl. contraction of seminal vesicles, prostate, and urethra
2. Rhythmic contraction of pelvic floor is mediated by the pudendal nerve (S2–S4, somatic) - ORGASM: triggered by interplay of sensory input and cortical arousal levels + neurotransmitter release

What are the signs/symptoms of autonomic dysfunction?
- Dry eyes (sicca), dry mouth
- Pupil dilation (mydriasis), pupil constriction (miosis), drooping eyelids (ptosis)
- Fainting (syncope), lightheadedness (near-syncope), esp. on arising from seated/lying position (orthostasis)
- Constipation, diarrhea
- Urinary incontinence, retention, incomplete bladder emptying
- Erectile dysfunction, DEC vaginal lubrication
- DEC/INC sweating
- Skin flushing, pallor, Raynaud’s


