Jacewicz - Meninges, BBB, Ventricles Flashcards
(33 cards)
Anterior neuropore failed to close in a fetus. What region is most likely to be maldeveloped?
- Cerebral cortex
- Baby could end up with prosencephaly

What cell type are dorsal root ganglion and the enteric nervous system derived from?
Neural crest cells
Fetal head with brain with thin cortex, single enlarged ventricle, and fused thalami. Which developmental region of the brain is most likely abnormal in the fetus?
Prosencephalon
Fetus at 18 weeks gestation with diminished movement of lower extremities. What abnormality is most likely?
Spina bifida
Successful migration of developing neurons to their final resting place is dependent on…?
Radial glia
What is Arnold-Chiari?
- Herniation of the cerebellar tonsils
- Can lose CSF flow, leading to hydrocephalus, but this is uncommon —> usually an incidental finding on MRI
What is communicating hydrocephalus?
- Damage to arachnoid granulations: can be caused by bacterial meningitis via inflammatory damage
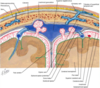
What is this top arrow pointing to? What N passes through here, and what is its function?

- Optic canal: CN II (optic N)
- Carries visual info from retina of the eye back to the brain, allowing for vision
What is this bottom arrow pointing to? What N passes through here, and what is its function?

- Superior orbital fissure: CN III (occulomotor), CN IV (trochlear), V1 (ophthalmic of CN V), CN VI (abducens)
- CN III: controls orbital mm of the eye (except supraoptic and lateral rectus), and carries fascicle of NN that constrict the pupil
- CN IV: controls supraoptic mm of the eye
- CN VI: controls lateral rectus mm of the eye
- V1: transmits sensory info from ipsilateral forehead and scalp to brainstem
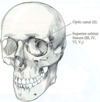
Identify/name the bony openings through which the cranial nerves exit the skull.

- Cribiform plate: olfactory bulb fibers pass through here to reach nasal epithelium; trauma may shear these fibers to produce anosmia
- Optic canal: optic nerve (CN II)
- Superior orbital fissure: CN III, IV, VI, and V1
- Foramen rotundum: V2 (maxillary branch)
- Foramen ovale: V3 (mandibular branch)
- Foramen spinosum: middle meningeal artery
-
Internal auditory canal/meatus: CN VII (facial) and CN VIII (vestibulocochlear)
1. Facial exits via stylomastoid foramen
2. CN VIII leaves via external auditory meatus -
Jugular foramen: CN IX (glossopharyngeal), X (vagus), XI (spinal accessory)
1. Spinal branches of CN XI pass rostrally through foramen magnum, join cranial branches, and exit via the jugular foramen - Hypoglossal canal: CN XII (hypoglossal)

Identify the indicated landmarks, and the things that pass through them.

- Foramen ovale: V3 of trigeminal N
- Foramen spinosum: middle meningeal artery
-
Carotid foramen: internal carotid artery enters here, passes through bony canal, and enters calvarium through carotid canal
1. Note: foramen lacerum is blocked by connective tissue - Stylomastoid foramen: CN VII, which entered via internal auditory canal
- External auditory meatus: CN VIII, which also entered via internal auditory canal
- Jugular foramen: CN IX, X, XI (spinal branches of CN XI enter calvarium via foramen magnum)
- Hypoglossal canal: CN XII

Identify the indicated anatomical features.
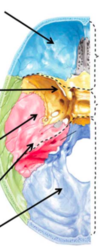
- Anterior fossa, sphenoid bone, middle fossa, petrous bone, and posterior fossa
- NOTE: lesser wing of sphenoid and petrous ridge of temporal bone create bony prominences against which brain can rub and be injured if accelerated or decelerated quickly through head trauma
What are the meninges? What is their purpose?
- PURPOSE: protect brain from injury via mech support and bathe it in fluid to buffer against chem/mech forces
- PIA MATER: thin layer of cells tightly approximated to brain surface
- ARACHNOID: somewhat thicker than pia
- DURA: meningeal layer (closest to brain) and periosteal layer (outer layer just beneath periosteum); these 2 layers separate in midline and at lateral aspects of brain to create superior sagittal/lateral sinuses

What three spaces are associated with the meninges?
- Two “potential” spaces: 1) epidural, and 2) subdural
1. Under normal circumstances, these do not exist; head trauma and o/conditions may cause bleed into epidural space (usually arterial: middle meningeal aa) or subdural space (usually venous: bridging vv) -
Subarachnoid space is a true space lined by arachnoid above and pia mater below -> contains most of the CSF that bates the brain
1. Large blood vessels, aa, and vv at base of and surrounding the brain lie in this space -> rupture of any of these vessels leads to subarachnoid hemorrhage

How do the meninges change/stay the same from brain to spinal cord?

- The 3 meningeal layers for the brain are continuous with similar membranes surrounding the spinal cord
- Dura and arachnoid continue out into peripheral NN too, forming epineurium and perineurium, respectively
- NOTE: dural membrane surrounding the spinal cord is comprised of only a single layer in contrast to the double layer covering the brain

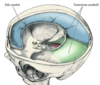
What are these structures?

- FALX CEREBRI: formed by meningeal layers
- TENTORIUM CEREBELLI: also formed by meningeal layers, and supports cerebral hemispheres, separating them from the underlying cerebellar hemispheres in the posterior fossa
1. Separates the supratentorial compartment from the infratentorial compartment
Describe the extracranial arterial supply to the brain.
- Brain served by 2 major pairs of aa: R and L internal carotid and R and L vertebral
- R and L COMMON CAROTID AA bifurcate in neck below angle of jaw into ECA/ICA
1. ECA supplies face, scalp, meninges
2. ICA: ascend through carotid canal, enter cranial vault by cavernous sinus, and make hairpin turn backwards and continue as middle cerebral artery (MCA) and anterior cerebral artery (ACA); ophthalmic artery branches off near apex of hairpin turn and is first branch of the ICA - R and L VERTEBRAL AA originate from subclavian aa, and enter vertebral foramen bilaterally at C6 level, traveling up through these foramen and entering calvaria through foramen magnum
1. The 2 vertebral aa join at junction of the medulla and pons to form the basilar artery or BA

What is this vessel? What happens if it ruptures?
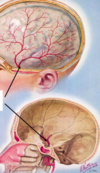
- MIDDLE MENINGEAL ARTERY: branches off external carotid
- Close approximation to inner aspect of skull, so outline created by grooves in inner table of the skull bone where the middle meningeal artery travels
- Head trauma w/skull fracture across regions of MMA can rupture it, causing bleeding into epidural space -> neurological/neurosurgical emergency w/death in a few hours if undiagnosed and untreated
Identify the indicated anatomical features.
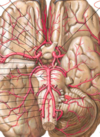
- Ventral aspect of the brain, and the aa that comprise the Circle of Willis, the structure that provides potential for collateral blood flow if one or more of the 4 major aa supplying the brain is obstructed/occluded
1. Comprised of PCA connected to ICA via post communicating aa; anterior segment of ACA, called A1, and anterior communicating artery complete the circle - O/important aa here incl. basilar artery, superior cerebellar artery, middle cerebral artery, lateral striate arteries, the vertebral arteries, the superior, anterior inferior and posterior inferior cerebellar arteries

Describe the arterial supply of the lateral/sagittal brain.
- These all branch off the internal carotid artery (ICA)
- PCA
- MCA
- ACA

Describe the venous drainage of the brain (image).
- NOTE: cavernous sinus, straight sinus, superior sagittal sinus, great cerebral vein, inferior sagittal sinus, and transverse sinuses
1. All of these drain into the internal jugular (anterior) and occipital veins (posterior) - Occlusion of any of the major venous sinuses may cause seizures, tissue injury, and blockage of CSF circulation

Briefly describe the ventricles of the brain (anatomically) and their connections.
- Note the physical relationships b/t components of the lateral ventricle with the frontal, parietal, occipital, and temporal lobes of the brain
- Communication b/t lateral ventricles with midline third ventricle through the interventricular foramen of Monro
- Communication b/t third and fourth ventricles via the cerebral aqueduct of Sylvius also known as the Sylvian aqueduct

Compare the composition of CSF and blood plasma (table).
- CSF protein is roughly 1/100th the conc of protein in blood
- CSF glucose roughly 2/3rds that of blood, and it takes about 2 hours for CSF to equilibrate w/peripheral blood glu -> important in a brittle diabetic, whose blood sugars may fluctuate markedly during the day

Describe CSF circulation. What happens if it is blocked by somethiing like a tumor?
- CSF is created in choroid plexus by specialized epi cells that line and partly fill lateral, 3rd, 4th ventricles
- CSF escapes lateral ventricles into 3rd ventricle via foramen of Monro, enters 4th ventricle via aqueduct of Sylvius, leaves 4th ventricle via foramina of Magendie and Luschka
- In subarachnoid space, some CSF circulates around spinal cord (10% reabsorbed at egress pt of nerve roots)
1. Bulk travels up through opening in tentorium cerebelli and circulates over/around brain - 90% reabsorbed into venous sinuses via arachnoid granulations (outpouchings of arachnoid that protrude into lg venous sinuses)
- CSF is made at a rate of ~ 20 ml/hr (about 500ml/d)
- BLOCKAGE: CSF outflow paths can be blocked by tumor or blood clot b/t lateral and 3rd ventricles, 3rd and 4th ventricles, and at foramen magnum, causing intraventricular CSF to build up with raised intracranial pressure and hydrocephalus
1. Hydrocephalus caused by physical blockage of ventricular system = obstructive hydrocephalus