How does the composition of breast change with aging and how is this related to imaging and ease of diagnosis?
- Young women = ↑ fibrous interlobular stroma which appears radiodense or white on imaging; makes diagnosing tougher.
- Older women have ↑ adipose tissue, which appears more radiolucent and helps with the interpretation of images
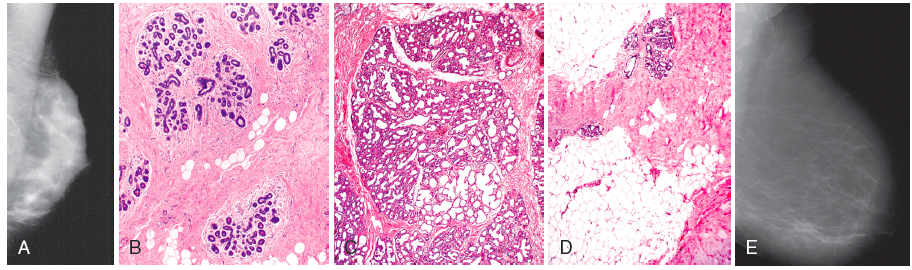
What 2 lesions of the breast arise in the intralobular stroma?
- Fibroadenoma
- Phyllodes tumor
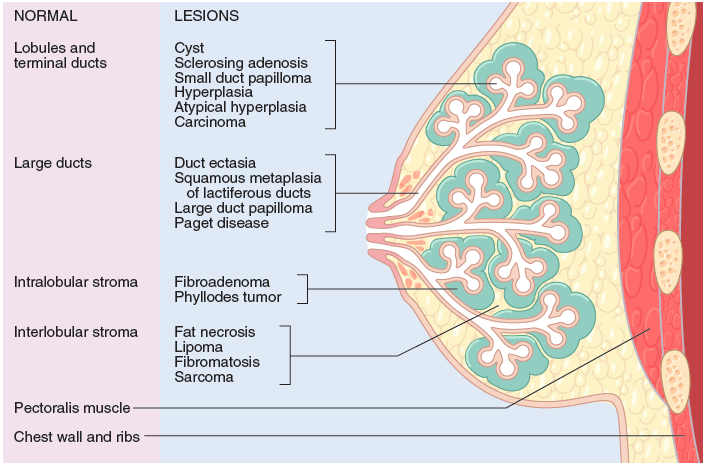
What 4 lesions can arise in the interlobular stroma of the breast?
- Fat necrosis
- Lipoma
- Fibromatosis
- Sarcoma
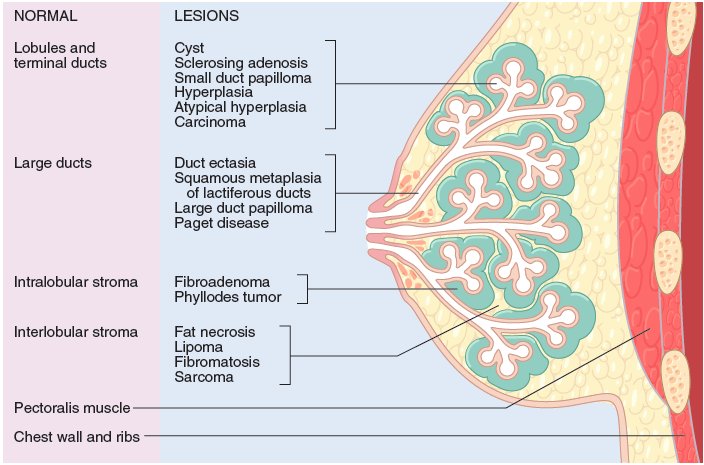
What 4 lesions can arise in the large ducts of the breast?
- Duct ectasia
- Squamous metaplasia of lactiferous ducts
- Large duct papilloma
- Paget disease
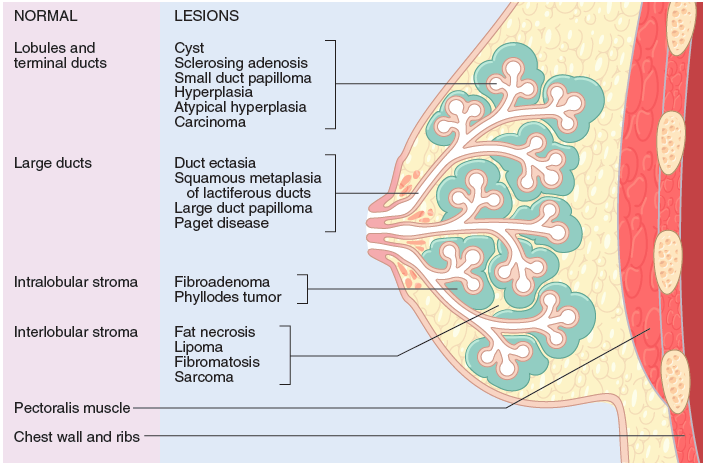
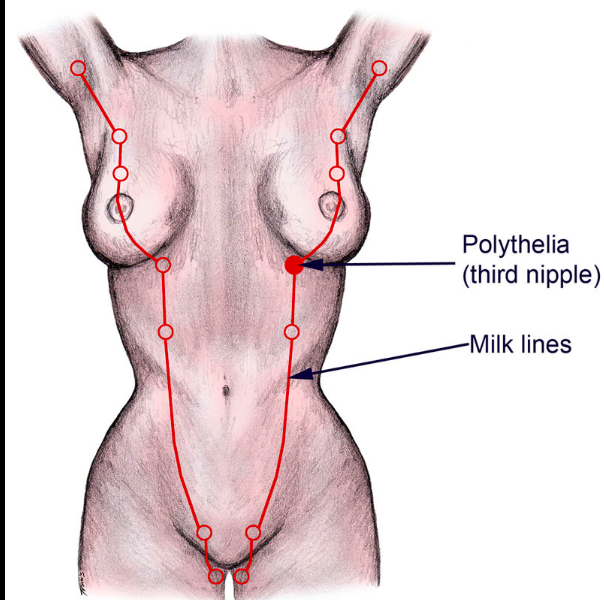
What are milk line remnants and how do they most commonly come to attention clinically?
- Supernumerary nipples or breast, anywhere from axilla –> perineum
- Present as painful PRE-menstrual enlargements
What is the clinical significance of accessory axillary breast tissue; managed how clinically?
- Potential site for malignancy or other lesions
- Prophylactic mastectomies ↓ risk, but do NOT completely eliminate
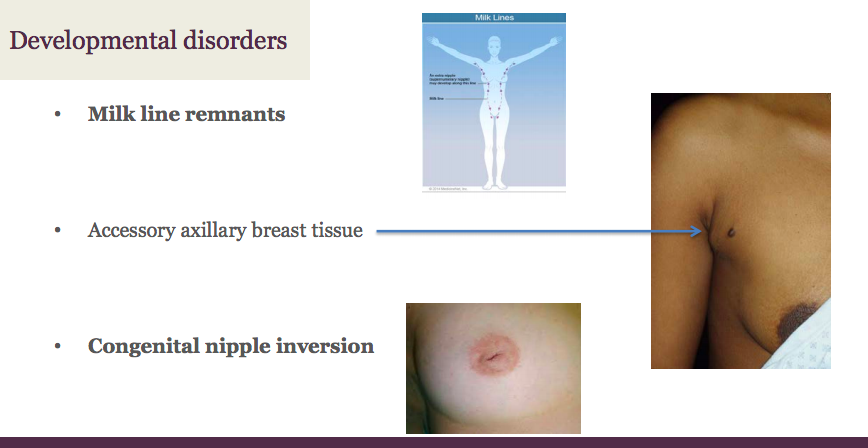
Why is acquired nipple inversion of greater concern than congenital?
May indicate presence of an invasive cancer or an inflammatory nipple disease
Palpable masses of the breast are most commonly due to what 3 etiologies?
- Cysts
- Fibroadenomas
- Invasive carcinoma

In what setting is nipple discharge most worrisome?
When spontaneous and unilateral; especially >60 y/o
What is the most common cause of bloody or serous discharge from th nipple?
Large duct papilloma
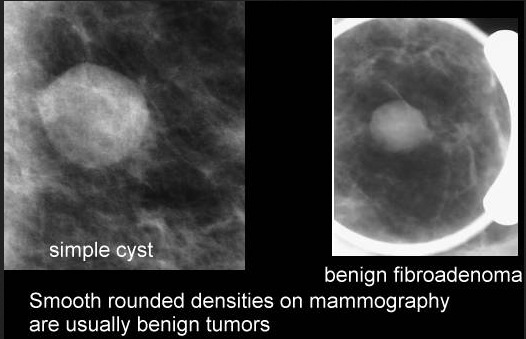
What characteristics of a density detected on mammogram is associated with benign vs. malignant lesions?
- Benign = rounded densities
- Malignant = irregular masses
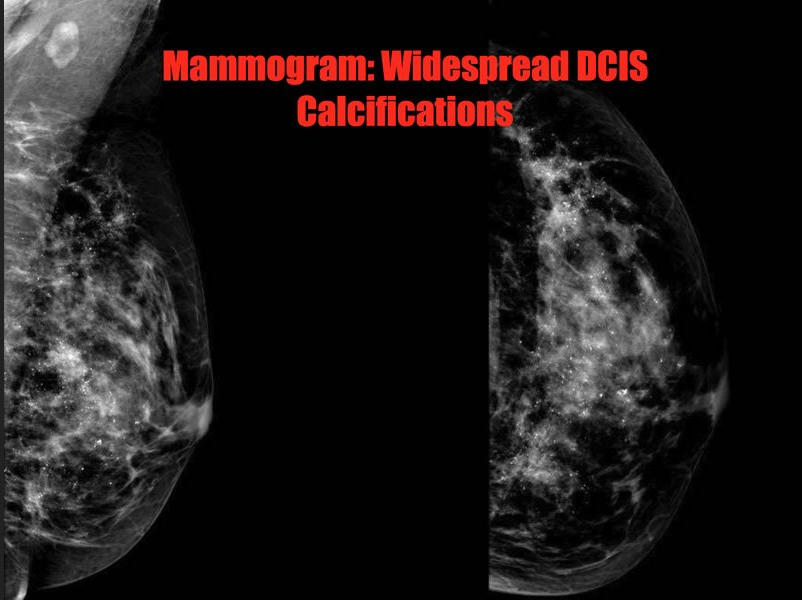
How is DCIS most commonly seen on mammograms?
Calcifications –> small, irregular, numerous and clustered
When does acute mastitis typically occur and what are the signs/sx’s?
- Typically during 1st month of breastfeeding
- Breast is erythematous and painful, and fever is common
Squamous metaplsia of lactiferous ducts (aka recurrent subareolar abscess, periductal mastitis, and Zuska) disease commonly presents with what signs and sx’s?
- Painful erythematous subareolar mass
- Inverted nipple
Risk factors for squamous metaplsia of lactiferous ducts (aka recurrent subareolar abscess, periductal mastitis, and Zuska) include?
- Smoking
- Vitamin A deficiency
What are the key morphological features of squamous metaplsia of lactiferous ducts (aka recurrent subareolar abscess, periductal mastitis, and Zuska)?
- Keratinizing squamous metaplasia of nipple ducts
- Intense chronic granulomatous inflammation
What are the distinguishing features, signs and sx’s of duct ectasia?
- Palpable periareolar mass w/ thick, white nipple secretions and occasionally skin retractionb
- NO pain or erythema!
Duct ectasia most commonly occurs in which age group and what is a risk factor?
- Women 40-60 y/o
- Usually multiparous (birthed more than one child)
In duct ectasia the ectatic ducts are filled with inspissated secretions and numerous what?
Lipid-laden macrophages
What is the common clinical presentation of fat necrosis of the breast and what is a risk factor?
- Painless, palpable mass + skin thickening or retraction
- May also have mammographic densities or calcifications
- 50% of women have hx of breast trauma or prior surgery
How does lymphocytic mastopathy (aka sclerosing lymphocytic lobulitis) most commonly present; associated with what underlying disorders?
- Single or multiple HARD palpable masses or mammographic densities
- Most common in women w/ T1DM or autoimmune thyroid disease
- Autoimmune basis
What are the 3 principal morphological changes associated with nonproliferative breast changes (fibrocystic change)?
- Cysts
- Fibrosis
- Adenosis
How can a FNA of a cyst associated with nonproliferative breast changes help confirm the diagnosis?
Dissapearance of the mass after FNA of its contents
The nonproliferative breast change, adenosis, is defined as what; and is a normal feature seen in which women?
- ↑ in the number of acini per lobule
- Normal feature of pregnancy










































