Multisystems II - First Aid Flashcards
(140 cards)
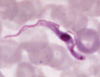
What stain would you use when looking for organisms like Borrelia, Trypanosomes, Rickettsiae, Chlamydia and Plasmodium?
Giemsa
A patient presents with an infected wound after abdominal surgery. The pus is very stinky. What type of antibiotic would be ineffective in treating this condition?
He likely has an anaerobic infection. Aminoglycosides require O2 to enter the bacteria and would be ineffective against anaerobes because they grow in oxygen poor environments.
What makes a bacteria an obligate anaerobe? List 3 bacteria that fall into this category.
The bacteria cannot use O2 as the final electron acceptor in the ETC. They lack catalase and cannot dispose of H2O2 produced in the presence of oxygen. They lack superoxide dismutase and accumulate reactive oxygen species in the presence of oxygen. Examples include clostridium, bacteroides and actinomyces.
Why is Rickettsiae an obligate intracellular bacteria?
It cannot make its own ATP
Why are asplenic patients at increased risk for meningococcal meningitis?
They cannot opsinize N. meningitides as well and the bacteria persist longer.
A patient presents with oral and facial abscesses that drain through the sinus tracts. Labs show gram positive filamentous anaerobic bacteria with sulfur granules. What is causing his condition? How do you treat him?

Actinomyces israelii. Treat with penicillin.
A sheep farmer presents with a black eschar on his arm with edema surrounding the lesion. Labs are shown below. What bacterial exotoxin is responsible for this lesion? What other presentations can be caused by this bacteria?

Edema factor from B. anthracis (boxcar-shaped gram + rod) is like adenylate cyclase, increases cAMP and causes fluid accumulation. In addition to cutaneous anthrax, inhalation of spores can cause pulmonary anthrax (fever, pulmonary hemorrhage, mediastinitis and shock) and GI anthrax (ulcers, regional, edema, hemorrhage, sepsis, 50% mortality)
A 10 year old boy presents with muscle spasticity and lock jaw a few weeks after stepping on a nail in the yard. What bacterial exotoxin is responsible for his symptoms?
Tetanospasmin from C. tetani prevents release of inhibitory neurotransmitters (GABA and glycine) from Renshaw cells in the spinal cord.
A 7 month old girl presents with flaccid paralysis after eating some honey with her sandwich. What bacterial exotoxin is responsible for her symptoms?
Botulinum toxin prevents release of excitatory neurotransmitters (ACh) from neuromuscular junctions.
A patient presents after being shot in the leg with bubbles forming around the wound. Labs show a double zone hemolytic pattern on blood agar. What bacterial exotoxin is responsible for his condition?
C. perfringes produces an alpha toxin which is a phospholipase (lecithinase) that degrades tissue and cell membranes.
A patient presents with fever, vomiting, desquamation of the skin, rash, hypotension and shock. Symptoms resolve after a tampon was removed that had been left in for a week. Staph aureus is cultured. What toxin was mediating his symptoms?
TSST-1. This locks the CD4 and MHC II receptors together, resulting in overproduction of IFN-gamma and IL2.
A patient presents with a skin rash. Streptococci are cultured after the patient died of septic shock. What toxin caused him to die?
Exotoxin A. This locks the CD4 and MHC II receptors together, resulting in overproduction of IFN-gamma and IL2.
A patient presents with a fever and neck stiffness. Physical exam reveals hypotension, edema and petechiae. CSF shows gram negative diplococci in pairs. How might a toxin be causing his symptoms?

Endotoxin activates macrophages and they secrete IL-1 (fever), TNF-alpha (hypotension, fever) and NO (hypotension). It activates complement and C3a (hypotension, edema) and C5a (PMN chemotaxis) are released. It activates tissue factor, the coagulation cascade and causes DIC.

Gram positive anaerobic spore-forming rods
Clostridium. Bacillus are gram positive AEROBIC spore forming rods
A patient who was admitted to the hospital for cardiac failure develops diarrhea and abdominal cramps. Pseudomembranes are seen on flexible sigmoidoscopy. Lab analysis shows a gram positive spore forming anaerobe. How should you treat him?
He has C. difficile colitis. The bacteria secrete toxin A (binds to brush border of gut) and toxin B (disrupts cytoskeleton via actin depolymerization). Treat with oral vancomycin or metronidazole.
A patient presents with a fever and neck stiffness. Physical exam reveals hypotension, edema and petechiae. At the end of the day he is dead and autopsy shows necrotic adrenal glands. What was likely causing his condition? How could he have been treated and how should you proceed form here?

N. meningitides causes meningococcemia, meningitis and Waterhouse-Friderichsen syndrome (when the adrenals are involved). He could have been treated with ceftriaxone or penicillin G early in the infection. Close contacts should be given prophylactic rifampin, ciprofloxacin or ceftriaxone.
3 types of spirochetes? What is the only type that can be visualized with dye?
Borrelia, Leptospira and Treponema: Only Borrelia can be visualized with Giemsa-Wright staining.
A 40 year old man returns from surfing in Hawaii with yellow skin, altered mental status, photophobia, conjunctival suffusion, anuria, fever and hemorrhage. Labs reveal anemia. What is likely causing his condition?
Water contaminated with animal urine can cause infection by leptospira interrogans. The symptoms this man is presenting with is classic of Weil’s disease.
A 29 year old woman presents with a flu-like illness and symptoms resolved after 10 days. 5 weeks later she returns with migratory polyarthritis, confusion, facial nerve palsy and polyneuropathy. ECG shows a right heart block. She says she enjoys hiking a lot. What is the likely cause of her condition? How do you treat it?
Lyme disease: B. burgdorferi is transmitted to humans by the tick I. scapularis from its natural reservoir in the mouse. Patients do not always notice a tick bite and do not always present with erythema migrans (below). Treat with doxycycline or ceftriaxone.

A patient with syphilis gets really bad flu symptoms after being treated with penicillin. What happened?
Jarisch-Herxheimer reaction: killed bacteria release a lot of pyrogens and induce an inflammatory response.
What other disease is transmitted by the same tick that transmits lyme disease? What would you expect to see on histology?
Anaplasma, on histology you would see berry-like inclusion bodies in granulocytes.
What zoonotic bacterial infection can cause bacillary angiomatosis in an immunocompromised patient?
Bartonella henselae (Cat Scratch Disease)
What zoonotic bacterial infection causes relapsing fever? Vector?
Borrelia recurrentis can continually vary its surface antigens. It is from louse.
What zoonotic bacterial infection causes undulant fever?
Brucella from unpasteurized dairy