Thrombosis Flashcards
(16 cards)
Why does coagulation occur (as in, what is its purpose)?
- Coagulation prevents blood loss.
- Inflammation activates coagulation and coagulation promotes inflammation.
- Coagulation is an immunological response.
What is the response to tissue damage inflammation?
- Primary haemostasis is the aggregation of platelets
- Secondary haemostasis is the conversion of fibrinogen to fibrin mesh by thrombin which is a protease.
- Thrombin is itself converted from prothrombin which is the culmination (end point) of a cascade of similar activation step.
- Anticoagulants prevent thrombosis.
- Fibrinolysis reverses thrombosis.

Describe both arterial and venous thrombosis.
-
ARTERIAL THOMBOSIS: -
- they mostly result from an atheroma rupture or damage to the endothelium (eg. MI, stroke)
- it is a platelet-rich, ‘white’ thrombosis; it’s mostly primary haemostasis
- it may block downstream arteries
-
VENOUS THROMBOSIS: -
- it often results from stasis (period of inactivity) or a hyper-coagulant state (eg. DVT/ deep vein thrombosis)
- it is a platelet-poor, ‘red’ thrombus; it is mostly secondary haemostasis
- it may move to the lungs
What is the coagulation vs fibrinolysis balance?
- If there is damage to endothelium, things such as tissue factor (TF) are exposed to the blood and can start coagulation.
- Tissue factor will initiate clotting
- Von Willebrand factor (VWF) activates platelets
-
Mechanisms to stop clot formation
- Anti thrombin and heparan inhibit clotting
- Prostaglandins inhibit platelets
- Nitric oxide inhibits platelets
-
When a clot forms there are also mechanisms
- we have a tPA (tissue Plasminogen Activator) that converts plasminogen into plasmin which caused fibrinolysis to create D dimers

What is Virchow’s Triad, and what are its three components?
- It describes the three categories that are thought to contribute to thrombosis.
- These three categories are: -
- STASIS: static blood lacks kinetic energy and tends to clot
- HYPER-COAGULANT STATE: eg. infection, hereditary, drugs (eg. HRT/hormone replacement therapy)
- ENDOTHELIAL DAMAGE: eg. surgery or cannula
How are the valves involves in stasis?
Blood tends to eddy (a circular movement of water causing a small whirlpool) around the valves, increasing the risk of stasis.

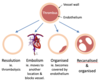
What are the four possible fates of a thrombus?
- RESOLUTION: where the fibrinolytic system destroys the whole clot over time
- EMBOLISM: where the thrombus dislodges and goes to the heart/lungs, causing death
- ORGANISED: where the endothelial cells just grow over the clot; this makes the person more prone to having another one due to the narrower vein
- RECANALISED AND ORGANISED: where the thrombus is so big you can’t grow over it, but you can grow through it
What is the difference between a proximal DVT and a distal DVT?
- With a proximal DVT (above the knee), there is a higher risk of a pulmonary embolism and post-thrombotic syndrome (When its blocking the vessel and not dislodging causing pain, swelling, and sometimes ulcers) as the vessels are relatively larger.
- With a distal DVT (lower leg), it rarely causes a pulmonary embolism or post-thrombotic syndrome as the vessels are relatively small.
What is the fate of venous thrombosis?
-
Small venous thrombolus- may be asymptomatic
- Slight VQ mismatch/small infarct zone
-
Large venous thrombolus- can cause rapid death
- Saddle embolism can block both pulmonary arteries
- Saddle pulmonary embolism commonly refers to a large pulmonary embolism that straddles the bifurcation of the pulmonary trunk, extending into the left and right pulmonary arteries.
- Saddle embolism can block both pulmonary arteries
What does a platelet release when it has been activated?
- Upon exposure of the sub endothelial cells, the von Williebrand factor on the sub endothelial cells will bind the platelets and cause the platelets to become activated.
- The circulating von Williwbrand factors may bind to exposed subendothelial cells.
- So there will be a whole lot of activated platelets with von Williebrand factor all at the site of tissue damage.
- The activated platelet releases thromboxane A2 (TxA2) and adenosine diphosphate (ADP); these induce receptors (GPIIb/IIIa) for fibrinogen.
- These bind to receptors on adjacent platelets and increase expression of the glycoprotein complex GPIIb/IIIa.
- These factors behave in a paracrine (relating to or denoting a hormone which has effect only in the vicinity of the gland secreting it) and autocrine (denoting or relating to a cell-produced substance that has an effect on the cell by which it is secreted) fashion.
- Fibrinogen acts as a tether, holding platelets together (this is not blood coagulation).
- Once you have a clump of platelets they form a negatively charged phospholipid surface which is required for coagulation.
- Coagulation involves the conversion of fibrinogen to fibrin and then crosslinking of the fibrin clot.
What are the three coagulation pathways?
- Common pathway
- Extrainsic pathway - the most important in vivo.
- Intrinsic pathway - forms the basis of laboratory tests of coagulation.
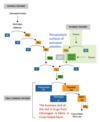
Describe the common pathway.
The common pathway pathway reactions run at a trickle and are easily overpowered by inihibitors.
- Factor IXa activates Factor X by proteolysis to create Factor Xa.
- Factor Xa (FXa) cleaves prothrombin to form thrombin (FIIa).
- Thrombin (FIIa) is a protease that cleaves fibrinogen into fibrin. Fibrinogen is a large molecule that’s present in plasma - once cleaved, it becomes insoluble fibrin.
- Fibrinogen also promotes blood clotting by forming bridges between, and activating, blood platelets through binding to their GpIIb/IIIa surface membrane fibrinogen receptor.
- Thrombin cleaves Factors V and VIII to give FVa and FVIIIa. This is known as amplification, as FVIIIa and FVa amplify the existing reactions, making them harder to overpower.
- FVa and FVIIIa together with the plasma Ca2+ form the: -
- Tenase complex - FVIIIa + FIXa = FXa
- Prothrombinase complex - FVa + FXa = thrombin
- These complexes assemble on the charged phospholipid surfaces in the activated platelets.
- Once enough thrombin has been generated, XIII is activated, which crosslinks the fibrin fibres into a solid clot.

Describe the prothrombinase complex.
- The negative surface of the activated platelet causes Ca2+, prothrombin and Factor Xa and Va to bind.
- This makes the prothrombinase complex.
- Factor Xa is bound to negatively charged phospholipids via GLA domain. In order to make GLA domain you need vitamin K. Activating factor X leads to cleavage of prothrombin to thrombin.
- Forming these GLA domains is Vitamin K dependent and can be inhibited by warfarin (rat poison).

Describe the extrinsic pathway.
- Trauma can lead to blood being exposed to tissue factor (TF) which is under the endothelial cells. TF is a receptor for factor VIIa, also bound to a negatively charged surface of platelet phospholipids along with calcium.
- Once activated, VIIa activates Xa and the common pathways begins.
- Major one happening in vivo.
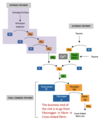
Describe the intrinsic pathway.
- Activated when you put blood on a charged surface such as glass
- Defects in the factors of the extrinsic pathway have for larger physiological effects than mutations in the enzymes of the intrinsic pathway.
How do you get rid of a clot once you heal?
- Fibrinolysis by tissue plasminogen activator (tPA)
- Thrombolytic agents can be used to treat strokes and myocardial infarctions
- tPA converts plasminogen into plasmin. Plasmin causes fibrinolysis of the clot into D dimers.
- Fibrinolysis by antithrombin
- Expressed by endothelial cells
- Inhibits a lot of enzymes in the coagulation cascade such as Thrombin and factor VII.
- Heparan binds to the enzyme inhibitor antithrombin III (AT), causing a conformational change that results in its activation. Activated AT, inactivates thrombin, factor Xa and other proteases.
- Expressed by endothelial cells


