Airway Pharmacology Flashcards
(18 cards)
What aspects of acute airway pathology can and cannot be treated with drugs?
-
Can be treated:-
- Contraction of smooth muscle.
- Excess mucus secretion.
- Oedema / swelling.
- irritation of sensory neurons (cough).
-
Cannot be treated:-
- Cause of inflammation.
- Airway / lung remodeling.
- Tissue damage.
How can we treat airway smooth muscle contraction?
- We can do that through bronchodilators (a drug that relaxes bronchial muscle resulting in expansion of the bronchial air passages).
- Some examples would be:
-
β-2 adrenergic receptor agonists :-
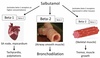
- Short-acting (SABA) - e.g. salbutamol. [They are the first inhalers given to asthma patients for an acute asthma attack].
- Long-acting (LABA) - e.g. salmeterol. [They are used in people with chronic asthma. They take it every day on a regular basis so that their muscles relax throughout the day].
- Ultra long-lasting (ultra-LABA) - eg. indacaterol. [They are used in people with chronic asthma. They take it every day on a regular basis so that their muscles relax throughout the day].
- Long-acting muscarinic receptor antagonists - e.g. tiotropium. [They are used as a second line of therapy for asthma and first line of therapy for COPD].
- Phosphodiesterase inhibitors - e.g. theophylline. [They arent used alot anymore as they have a relatively narrow therapeutic window. The diferenece between the dose for a good effect and a bad effect is relatively small so it can be unsafe. They arent as effective as β-2 adrenergic receptor agonists].
-
β-2 adrenergic receptor agonists :-
How do bronchodilators generally act?
- Bronchodilator drugs act by binding to a specific receptor or enzyme expressed by the airway smooth muscle cell and inducing an intracellular change which interrupts the contractile process (thereby causing relaxation of the smooth muscle).
- By relaxing the muscle, we increase the luminal area, thus decreasing resistance and increasing flow.

How do inflammatory mediators induce airway smooth muscle cell (ASMC) contraction?
- There are various contractile receptors present in the smooth muscle membrane that bind to different contractile mediators (e.g. prostaglandins, acetylcholine, etc.) and activate the receptors.
- This activates the Gq pathway.
- Within the cell there is an organ called the sarcoplasmic reticulum (SR) that stores calcium.
- When this pathway is activated, it results in Ca2+ being able to leave the SR into the cytosol. This increase the Ca2+ mobilisation and sensitivity.
- The Ca2+ binds to calmodulin and activates myosin light chain kinase. This initiates muscle contraction.

How does β-2 adrenergic receptor activation act to induce ASMC relaxation?
- The β-2 agonist (e.g. salbutamol) binds to the β-2 adrenoreceptors in the membrane of the smooth muscles. The β-2 adrenoreceptors are coupled to Gs subunit.
- The activation of the β-2 adrenoreceptors also activates the Gs subunit and causes in increase in the activation of Adenylyl Cyclase, an enzyme that catalyses the conversion of ATP to cAMP.
- The resulting increase in cAMP, in turn, activates Protein Kinase A, which phosphorylates multiple intracellular targets, ultimately decreasing intracellular calcium levels, inducing smooth muscle relaxtion.

How do long-acting muscarinic antagonists act to relax the ASMCs?
- Rather than activating a receptor and causing a relaxation to occur these drugs work by inhibiting a particular contractile mediator pathway.
- The action of LAMAs on airway involves blocking acetylcholine receptors present on ASMC cell membrane.
- Acetylcholine is a mediator and neurotransmitter that binds to M3 (muscarinic) receptors expressed in the membrane of ASMC and induces contraction.
- Therefore blockade of this receptor reduces the level of contraction in situations where acetylcholine plays a prominent role in inducing ASMC contraction.
- For this reason they are less effective as bronchodilators in asthma therapy, where acetylcholine typically has a more minor role in ASM contraction.

How do phosphodiesterase inhibitors act to relax the ASMCs?
- Inhibition of phosphodiesterase reduces the breakdown of cAMP to AMP.
- The resulting increase in cAMP, in turn, activates Protein Kinase A, which phosphorylates multiple intracellular targets, ultimately decreasing calcium levels, inducing relaxation.
What are some steps in the inflammatory process which could potentially be targeted with drugs to reduce inflammation?
- Proliferation of the immune cells.
- Antibody production.
- Antibody-crosslinking and degranulation.
- Inflammatory mediator-receptor binding.
- Tissue infiltration from the bloodstream (adhesion molecule expression).
- Chemotaxis.
- Cytokine-receptor binding.
- Cytokine production and release.
- Apoptosis.

What are the different classes of drugs, what disease do they help treat and what is the mechanism of their action?
mAb - monoclonal antibodies.

Why are corticosteroids used and what are their different types?
Corticosteroids are used as preventer medication to reduce airway inflammation. There are two main different types :-
-
Inhaled corticosteroids.
- Fluticasone.
- Budesonide.
- Beclometasone.
-
Oral/systemic steroids.
- Prednisone.
- Dexamethasone.
If inhaled corticosteriods are not helping the individual to relieve their symptoms thats when oral/systemic steroids are taken. The dosage is bigger but at the same time there may be greater adverse effects (as the streroid is able to reach more tissues in the body).
What are the effect of corticosteroids (such as glucocorticoids) on various immune and structural cells to reduce inflammation?

What is the mechanism of action of corticosteroids to reduce inflammation?
- They are used against asthma.
- They achieve their anti-inflammatory effect by binding to glucocorticoid receptors present within the cytosol of immune and structural cells (steroids are able to diffuse through cell membranes as they are lipid soluble).
- The bound drug-receptor complex then migrates to the nucleus of the cell, where it binds to DNA and modulates transcription.
- This has the knock-on effect of changing protein expression.
- By acting in this way, corticosteroids are able to increase pro-inflammatory mediators and decrease anti-inflammatory mediator expression in a wide variety of cell types, therefore shifting the balance and reducing the overall level of inflammation.

What considerations need to be made when using drugs to treat patients?
-
Drug efficacy.
- Increase the quality of life (by reducing the severity of their symptoms).
- Increasing their life expectancy.
-
Adverse effects.
- Decrease the quality of life (by increasing their risk of developing other diseases).
- Economic costs.
Why are drugs used in asthma typically administered by a metered-dose inhaler?
- In order to try and reduce the extent and likelihood of adverse effects in respiratory diseases, many drugs are delivered by inhalation via a metered-dose inhaler.
- This has the advantage that the drug is applied directly to the target tissue (the airways/lungs) and so the greatest dose will be present at the site of action (and, in theory, the dose reaching the other tissues will be much lower and less likely to produce adverse effects).
- It is also much quicker in the event of rescue/reliever doses.

List some side effects of β-2 agonist (salbutamol).
List some side effects that long-term/ high-dose corticosteroid administration is associated with.
- Growth retardation - stunted growth.
- Skin ulcers.
- Candidiasis (infection with candida) - is a fungal infection caused by yeasts.
- Hypercortisolism - Excess levels of cortisol in the blood. can lead to Cushing syndrome where there is significant weight gain particularly on the back and face.
- Depression.
- Osteoporosis - A disease of bone in which the bones become extremely porous and are subject to fracture.
How do you decide on a therapeutic strategy (ie. what drugs to use, when and in what order)?
- You must ensure that the acute risks are managed.
- Drugs with greater general efficacy are used first.
- Drugs with a lower risk of adverse effects are used first.
- Drugs with a broader mechanism of action are used first.
- Cheaper drugs are used before more expensive drugs.
- Fewer drugs are used before multiple drugs.
- You would combine drugs if they decrease the risk of adverse effects.
What is the difference between asthma pharmacotherapy and COPD therapy?
- Asthma pharmacotherapy is administered in a stepwise manner, with you moving up a step to improve control as needed, and moving down as many steps as possible to maintain minimal control.
- COPD therapy is administered in a progressive (in one direction) stepwise manner, with you moving up/ along as the symptoms and dyspnoea worsens.



