Development of the GI Tract Flashcards
(27 cards)
When does the GI tract development occur?
It occurs during the 3rd to 12th weeks embryonic age (5 to 14 weeks from LMP).
LMP meaning - last menstrual period.
What is the significance of the gut tube formation?
Organs and glands are produced by budding from the gut tube.
Why is folic acid important during the first trimester?
Folic acid helps with the fusion and closure of the spinal cord. It can significantly reduce the risk of neural tube defects (NTDs), such as spina bifida.
Spinal bifida meaning - It is when a baby’s spine and spinal cord don’t develop properly in the womb, causing a gap in the spine.
Describe primary germ formation.
- The primary germ layers are formed during the process of gastrulation.
- It starts to happen at the 3rd week (by week 10-12 the GI tract is almost fully formed).
- The embryo is a flat disc, comprised of two cell layers: epiblast and hypoblast.
- Epiblast cells in the mid-line of the embryo begin to ingress, starting from the caudal (tail) end; this is visible as the primitive streak.
- The ingressing cells differentiate into the mesoderm (that will become the surrounding muscles, connective tissue and mesenteries and blood vessels).
- The epiblast gives rise to the ectoderm (neural crest; it provides innervation to the gut, the enteric nervous system).
- The hypoblast (and epiblast) gives rise to the endoderm (with forms the epithelium and the gut tube and the glands). Most genetic abnormalities occur at this time.
Endoderm - Mesoderm - Ectoderm

Briefly describe the directions of the formation of the gut tube.
- The gut tube is formed by the folding of sheets of cells in two directions: -
- Folding towards the midline along the cranial-caudal axis.
- Folding towards the yolk sac at the cranial and caudal ends.
- The cloacal membrane is formed by ectoderm and ectoderm coming into contact with each other. It forms your urogenital sinus.
- Within the embryo, the cranial and caudal intestinal portals extend the tube towards the mouth and anus, delimited by the prochordal and cloacal plates.
- Bucco-pharyngeal membrane forms the mouth and the pharynx.
- Septum transversum forms the area where your diaphragm forms.
Urogenital sinus meaning - It is a part of the human body only present in the development of the urinary and reproductive organs. It is the ventral part of the cloaca, formed after the cloaca separates from the anal canal during the fourth to seventh weeks of development.

Describe the origin of the mesenteries.
- The mesentery is a contiguous set of tissues that attaches the intestines to the posterior abdominal wall in humans and is formed by the double fold of peritoneum. It helps in storing fat and allowing blood vessels, lymphatics, and nerves to supply the intestines, among other functions.
- The lateral plate mesoderm splits into parietal (somatic) and visceral (splanchnic) layers.
- The somatic layer depends on a continuous layer with mesoderm that covers the amnion (It forms the muscles).
- The splanchnic depends on a continuous layer that covers the yolk sac (It is the autonomic nervous system that goes in the gut).

What is the primary gut tube made up of?
It is made up of a sheet of endoderm, which makes the epithelia and glands. It is surrounded by mesoderm, which makes muscles and connective tissue (including mesentery).
What are the subdivisions of the primary gut tube, and where do their boundaries lie?
-
FOREGUT:
- Pharynx.
- Oesophagus.
- Stomach.
- Cranial half of duodenum.
- Ampulla of Vater (It is formed by the union of the pancreatic duct and the common bile duct).
-
MIDGUT:
- Caudal duodenum (From duodenal papilla).
- Jejunum.
- Ileum.
- Caecum.
- Appendix.
- Ascending colon.
- Proximal 2/3 of transverse colon.
-
HINDGUT:
- Distal 1/3 of transverse colon.
- Descending colon.
- Rectum.

What are the blood supplies to the different parts of the gut?
- The coeliac artery supplies the foregut.
- The superior mesenteric artery supplies the midgut.
- The inferior mesenteric artery supplies the hindgut.

What is the innervation of the gut?
- Sympathetic ganglia develop next to the major branches of the aorta.
- Post-ganglionic, sympathetic axons unnerved the same tissues that the arteries supply with blood.
- Celiac ganglion: foregut.
- Superior mesenteric ganglion: midgut.
- Inferior mesenteric ganglion: hindgut.

Describe the formation of the stomach.
- Stomach arises by expansion and rotation.
- During week 4 at the level where the stomach will form, the tube begins to dilate, forming an enlarged lumen.
- The stomach does a 90º clockwise turn about the cranio-caudal axis.
- The initial left side of the tube will form the greater curvature of the stomach and the initial right side of the tube will form the lesser curvature.
- Over time the The blood supplies is going to be gastric arteries.
- The vagus nerve is the main nerve to supply this part of GI tract.

What is the falciform ligament?
The falciform ligament is a ligament that attaches the liver to the anterior (ventral) body wall, and separates the liver into the left medial lobe and left lateral lobe.
What is the omentum?
- It is a fold of peritoneum connecting the stomach with other abdominal organs.
- It protects your bowl from getting infected.
- There are two:-
- The greater omentum - It extends from the greater curvature of the stomach, passing in front of the small intestines and doubles back to ascend to the transverse colon before reaching to the posterior abdominal wall.
- The lesser omentum - It is the double layer of peritoneum that extends from the liver to the lesser curvature of the stomach (hepatogastric ligament) and the first part of the duodenum.
- The epiploic foramen connects the greater and lesser omentum.

What fixes the mature gut in place?
Fusion of the mesentries with the posterior abdominal wall fixes the mature gut in place.
Describe pyloric stenosis.
- It is when there is a gastric outlet obstruction caused by smooth muscle hypertrophy (ie. the smooth muscle forming the pyloric sphincter overgrows).
- It can be spotted in newborns, as they will start projectile vomiting shortly after feeding (the vomit will NOT be bile-stained).

Describe the formation of the liver, budding from the gut tube.
- The hepatic diverticulum grows into the mesenchyme of the septum transversum.
- The cords of the hepatic endoderm, bile drainage ducts, and blood vessels proliferate, arranged as sinusoids.
- The lives exceeds the size of the septum transversum, and expands into the ventral mesentry.
- The remaining ventral mesentry gives rise to: -
- The falciform ligament between the liver and the body wall.
- The lesser omentum between the liver and stomach.
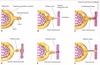
Describe the formation of the pancreas, budding from the gut tube.
- There are two pancreatic buds: -
- Dorsal, from the duodenal endoderm (induced by the notochord).
- Ventral, from the hepatic diverticulum (induced by the hepatic mesoderm).
- As the duodenum rotates, the dorsal and ventral buds meet and fuse.

Describe and annular pancreas.
An annular pancreas develops from a bi-lobed ventral bud that migrates in separate directions, coming around and fusing to constrict the duodenum.

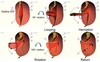
Describe the development of the intestines (midgut).
- The abdomen is too small to accommodate so the tube rotates 90º and elongates and comes out into the yolk sac (as there is not a lot of space).
- It then does a 180º rotation (this rotation helps start forming the large bowl as it comes back in).
- Around the 10-12 week the abdomen is bigger, and the intestines come back in (by this time you have the beginning of the small intestines startimg to form).
Describe an umbilical hernia.
- It is when the intestines return normally, but the rectus abdominis (abdominal muscle) fails to fuse around the umbilicus, leading to gut covered in skin.
- As the small intestines comes out into the yolk sac and then goes back in, its left some of the bowl in the area around the umbilicus.

Describe an omphalocele.
- It is the failure of the intestinal loops to return to the abdomen, so it ends up as a hernia covered in amnion.
- Its causes are unknown, but it is associated with maternal obesity, alcohol/ tobacco, SSRI (anti-depressants) use.
- These babies normally die.

Describe gastroschisis.
- It is a defect in the abdominal (belly) wall, a failure of the ventral body wall to fuse.
- This results in no covering of the gut as it sits outside the body.
- There is a marked association with young maternal age, low maternal BMI, and recreational drugs (especially cocaine).

Briefly, list and describe other possible congenital gut disorders.
- Persistence of the yolk duct (most common).
- Meckel’s diverticulum is a common intestinal abnormality that mimicks appendicitis (causing pain). It causes a slight bulge in the small intestine present at birth and a vestigial remnant of the omphalomesenteric duct (also called the vitelline duct or yolk stalk). It is present in 2-4% of the population and is usually asymptomatic.
- You can get ulcers.
- Volvulus means twisting and therefore an expansion.
- You can get diverticulum which is outpouching within it (so narrowing or it doesnt develop properly at all).
Describe Hirschsprung’s disease.
- It is where the person has an aganglionic megacolon.
- It primarily affects the hindgut.
- There is an absence of parasympathetic ganglia, caused by a lack of neural crest cells (precursors of enteric ganglion cells).
- Because of the failure of the development of enteric ganglia, there is a section of the gut that is completely absent of ganglia.
- This means that there is a dilatation of sections of the colon and the other parts are contracted, with a lack of tone and peristalsis, leading to profound constipation (as food cannot pass through the narrow contracted bits).