Define umbilical cord prolapse.
Umbilical cord prolapse involves the umbilical cord descending ahead of the presenting part of the fetus
How common is umbilical cord prolapse?
1 in 500
What are the complications of untreated umbilical cord prolapse?
Compression or cord spasm (in cold or if touched)
–> fetal hypoxia –> irreversible damage or death
What are the risk factors for umbilical cord prolase?
Maternal:
- multiparity
- cephalopelvic disproportion
- AROM (50% occur with artifical rupture of membrances)
Fetal:
- prematurity
- twin pregnancy
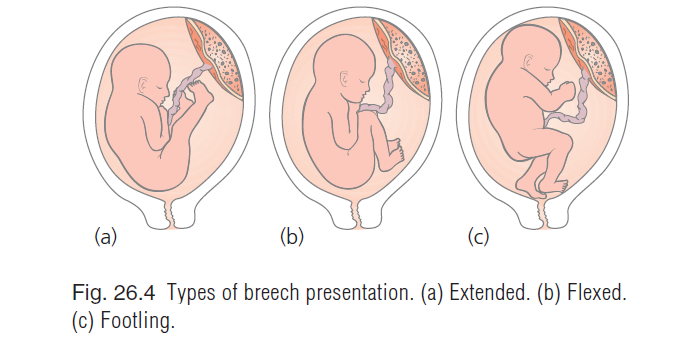
- abnormal presentations e.g. Breech, transverse lie
Uterine/placental:
- polyhydramnios
How is umbilical cord prolapse diagnosed?
Usually happens at AROM
FHR becomes abnormal
Cord is palpable vaginally, or is visible beyond the level of the introitus.
What is the management of umbilical cord prolapse?
Disgnose by speculum/digital examination and confirmation of fetal viability by auscultation of the fetal heart using CTG
Press emergency call button - senior help and prepare theatres
- The patient is asked to go on ‘all fours’ until preparations for an immediate caesarian section have been carried out
- The left lateral position is an alternative
- Retrofilling the bladder with 500-700ml of saline may be helpful as it gently elevates the presenting part
Tocolytics may be used to reduce uterine contractions
Delivery by emergency caesarean section
What can and what cannot be pushed back into the uterus in umbilical cord prolapse?
Presenting part of the fetus may be pushed back
The cord should not be handled but kept ward - should not be pushed back into the uterus
What should be done if the cord is past the level of the introitus?
Minimal handling + kept warm and moist
How common is morbidity and mortality of the fetus in umbilical cord prolapse?
Reported as high as 25–50% of cases
Which category of C section is done in umbilical cord prolapse?
Category 1 if pathological fetal heart pattern
OR category 2 if normal fetal heart pattern
Why has incidence of umbilical cord prolapse been reduced?
Reduced by the increase in caesarian sections being used in breech presentations
Give an example of a tocolytic which may be used in cord prolapse.
Terbutaline
Is vaginal delivery possible in cord prolapse?
Immediate caesarean section is normally used, but instrumental vaginal delivery is appropriate if the cervix is fully dilated and the head is low.


