Uro.... system Flashcards
Describe the general structure of the kidney.
What is its peritoneal relation?
Size and shape.?
retroperitoneal organ
- 120 - 200g
- 10 - 12cm long, 5-6cm wide, 4cm thick
2 different types of structures:
- urine formation: nephrons + uriniferous tubules
- urine collection: renal calyces + renal pelvis
What are the functions of the kidney?
-
homeostasis of bodily fluids (amount, osmolarity, pH, ion concentration)
∽ 180l primary urine filtered out of the blood/day -
excretion of metabolic end products (urine)
1.5 - 2l final urine formed/day - endocrine function (renin-angiotensin, vit D3, erythropoietin)
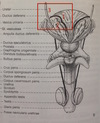
1 - 5

1) extremitas superior
2) extremitas inferior
3) hilum renale
4) sinus renalis
5) pyramidis renalis
6 - 10
Another name for #8.

6) capsula fibrosa
7) capsula adiposa
8) fascia renalis (= GEROTA)
9) medulla renalis
10) cortex renalis
11 - 13

11) papilla renalis
12) columna renalis
13) lobus renalis
What is a floating kidney?
What are other names?
loss of capsula adiposa → hypermobility of the kidney which descends into the pelvis
-
other names:
nephroptosis, nephroptosia, renal ptosis, renal descensus, renal prolapse
Which structures can be found in the cortex?
radii medullares (= medullary rays) = continuation of medullary substance
cortex corticis = contains radii medullares
labyrinthus corticis = area btw radii medullares
What are the projections of the kidney?
in fossa lumbalis
- right: Th12 → L3
- left: Th11 → L3
- hilum: L2
⇒ left kidney moves (2-3 cm) during deep inspiration
What are the boundaries of the kidney?
- laterally - medially
- cranially
- dorsally
laterally:
- 6) m. transversus abdominis
medially:
- 8) m. psoas major
cranially:
- diaphragm
- suprarenal gll.
dorsally:
- 7) m. quadratus lumborum
- n. subcostalis
- n. iliohypogastricus
- n. ilioinguinalis

What are the ventral boundaries of the kidney?
Differentiate btw right/left.
right:
- 1) right lobe of the liver
- 2) pars descendens duodeni
- 3) flexura coli dextra
- 4) loops of small intestine
left:
- 6) stomach
- 7) spleen
- 9) pancreas
- 10) flexura coli sinistra
- 11) radix mesocolica
- 12) loops of small intestine

What are the dorsal relations of the kidney clinically relevant?
contact to n. ilioinguinalis + n. iliohypogastricus explains why pain can spread up to the inguinal region in case of renal diseases
Explain the segmentation of the kidney.
5 segments
- segm. superius
- segm. anterius superius
- segm. anterius inferius
- segm. inferius
- segm. posterius
⇒ correspond to the arterial supply via a. renalis
What is the microscopic unit of the kidney?
Describe it.
nephron
- renal corpuscle
- glomerulus
forms together with renal tubule the uriniferous tubule
List some genetic abnormalities of the kidney.
- additional kidneys
- horseshoe kidney = fused kidneys
- renal aplasia = one kidney is missing
- renal hypoplasia = underdevelopment of one kidney
Explain the vasculature of the kidney
arterial supply:
- a. renalis dex./sin.
-
type I r. principalis ant./post.
* *type II** r. principalis ant./post./inf. - aa. interlobulares
- aa. arcuatae
- aa. corticales radiatae (= aa. interlobulares)
- arteriolae afferentes
drainage: beginning at glomerulus
- arteriolae efferentes
- vasa recta/peritubular cap.
- vv. corticales radiatae
- vv. arcuatae interlobulares
- vv. renales
- IVC
What are clinically important abberations of the renal vasculature?
- accessory renal aa.: persisting branches of aorta that didn’t redevelop during fetal dev., esp. important in case of surgeries
- abberant renal aa.: aa. don’t enter through hilum, but through sup./inf. pole
What is important abt v. renalis sin.?
Why is it clinically important?
3 tributaries:
- v. suprarenalis
- v. testicularis/ovarica
- v. phrenica inf.
⇒ cancer in the left renal v. can cause reflux into v. testicularis → dilation of scrotum (= varicocele)
What innervates the kidneys?
sympathetic innervation via plexus renalis
What are calices renalis?
Differentiate.
drain urine from papilla renalis into pelvis renalis
- major
- minor
What are the 2 shapes of the pelvis renalis?
type depends on calices renalis
volume: 3 - 8ml
- branching: minor calices open consistently into major which eventually open into pelvis renalis
- ampullary: minor and major calices open into pelvis renalis
What are the 2 ways for X-ray examinations to investigate the pelvis renalis?
- urogram: iodid containing contrast material injected intravenously, eventually excreted by kidney
- retrograde pyelogram: contrast material injected into ureters via a catheter
Which structures are connected by the ureter?
What are its 3 points of constriction?
pelvis renalis → urinary bladder
- exit from pelvis renalis
- crossing of a. iliaca communis/externa when entering the lesser pelvis
- wall of urinary bladder
Why are the points of constriction of the ureter clinically relevant?
⇒ renal colic = type of abdominal pain commonly caused by kidney stones, often wavelike in phases
What are the parts of the ureter?
- pars abdominalis in retroperitoneal space
- pars pelvica in lesser pelvis
- pars intramuralis in wall of urinary bladder