Cardiac Portion Flashcards
(235 cards)
myocardial ischemia
what is this and what is it caused by (3)? what determiens the severity? what are 3 contributatory factors? what how does it present as symptoms? what causes these symptoms in each?
temporary reduction of blood flow to an organ, potentially reversible, caused by mechanical, electrical, and valvular dysfunction
can be reversible or peremanent depending how long it has been happen for, can lead to infarction
this can cause angina when there is increased activity
Contributory factors: significant LVH, aortic stenosis, tachyarrythmias like afib/aflutter
symptomatic:
1. angina pectoris
1. O2 demand in the presence of fixed stenosis
- VASOSPAM and significant narrowing
1. prolonged decreaed O2=unstable angina or infarction
-acute thrombis likely present
sudden cardiac death in CHD
how soon does the pt die? what most likely causes it? when does this happen?
1. death within 1 hour after onset of symptoms usually within minutes
2. malignant arrhytmia commonly present
common presenting manifestation of CHD, frequent end point in patients with CHD propr to MI and imparied LV function
why are women often misdiagnosed when they have CHD? (3)
1. atypical symptoms: pain radiating to right arm, arm pain along
- many women produce false negative stress tests since single vessel disease more common
3. elderly or diabetic womeon complain of general malaise, loss of appetite, vague abdominal pain so if they have RF, GET EKG!!
stable angina pectoris
what does this pain feel like? is it reproducible? what are 3 things that make it better? what is the pattern? what are 6 things that can cause this? what are 4 things you might see to clue you into this?
chest discomfort described as
tightness, pressure, aching, choking that is often REPRODUCIBLE WITH ACTIVITY that resolve after cessation of activity, relaxation, or NTG
positive levine sign substernal to left sternum, with crescendo/decresendo pattern 1-5 mins, less likely to happen in AM (lower threshold)
can be brought on by: exertion, exercise, emotional stress,cold weather, cigarettes, sex
physical exam may be normal between episodes, may see xanthomas from hyperlidemia, AV nicking from HTN/DM, s4 gallop during angina, changes in BP
what are the 3 tests you can do to help identify stable pectoris for CAD? what do they show?
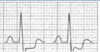
1. EKG:
normal between episodes
ST segment depression/T wave change during angina then normalize after angina passes
2. Stress EKG: most helpful non invasive tool
-increase workload with meds or exercise, compare resing and stress EKG for ischemia, may consider adding image to make it more specific, ability to detect dermines the amoutn of vessel involvment
3. coronary angiography- Gold standard for CAD
-tells which vessels are involved, degree of stenosis, and LV function
what is the drug you give for acute angina pectoris? or for prophylaxsis if the pt is going to be doing exercise?
sublingual NTG
reduces LV volume preload and decreasing O2 consumption
does this by causing venodilation, so that it decreases the amount of blood heading back to the heart, decreasing the volume and decreasing O2 demands
what are the 7 drugs you put someone on to help with chronic stable angina?
1. beta blockers ATENOLOL, METOROLOL: decreases HR, contractility, and BP improving exercise tolerance
*****REDUCE MORTALITY IN POST MI AND HF PATIENTS***
2. long acting nitrates isosorbide dinitrate
****DONT TAKE THIS WITH VIAGRA!!!!*****
****can develope nitrate tolerance so need to dose in intervals!!****
3. Non dihydropyridine calcium channel blockers dilate ARTERIES, decreasing afterload, decrease myocardial O2 consumption
4. dyhydropyridine calcium channel blockersamlodipine, nifedipine dilate ARTERIES, decrease afterload and myocardial O2 consumption
***best used in combination with a BB, reduce risk of HYPOTENSION**
5. diltiazem and verapamil used with nitrates, dilates arterioles decreasing afterload, decrease HR, and O2 consumption
***don’t use in HF patients!!***
6. ranolazine chronic angina that isn’t controled with the above
**increase QT interval, but won’t cause arrythmia**
7. antiplatelet drugs USED IN ALL PTS WITH CHD, PAD, AND CAROTID, DECREASES INCIDENCE OF CARDIAC DEATH AND MI, low dose asprin
what drug do you not want to use in CHD in a patient that has asthma/COPD because it can cause bronchospasm?
nonselective beta blockers
Use selective beta blocker!!
what two drugs decrease the mortality post MI and in HF patients?
Beta blockers
Atenolol and metoprolol
what 4 groups of patients with CHD qualitfy for revascularization?
1. patients with unacceptable symptoms controlled with meds
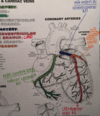
2. 3 vessel CAD with LV dysfunction OR left main coronary stenosis that compromises Left anterior descending (LAD) LEFT main artery consider CABG!!
3. patients post MI with ongoing ischemia
4. acute MI
when should percutaneous coronary revascularization/catherterization be used for CHD?
what are the rates of restenosis with angioplasty, stent, and drug eluting stent? what do you do to compensate for this?
angioplasty restenosis rate: 30-40%
angioplasty with stent placement: 15-20%
drug eluting stents restenosis: 5-8%
- single or 2 vessel disease
- 3 vessels disease in pt that doens’t qualify for operative
drug eluting stents helped decrease rates of restenosis a lot, however probles with late thrombosis so requires intense anti-platelet RX of ASA and clopidogrel
coronary artery bypass for CHD
what happens during this procedure? which two vessels are most commonly used? which one is the best one to use and why? what two factors increase mortality rates?
coronary arteries are bypassed using arteries or veins, low mortality if LV preserved
saphenous veins and mammary arteries most commonly used
internal mammary artery graft has highest patency rate over time**BEST OPTION WHEN POSSIBLE because arteries last longer than veins**
mortality increase with age and EF
coronary vasospasm
what can bring this on? what does the spasms cause? what will the pt feel and what will you see on the EKG? what can happen if this doesn’t resolve?
can be in normal cornary arteries or superimposed o atherosclerotic ones, the spasms cause the artery to close
often induced by cold, emotional stress, meds, and cocaine
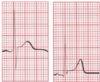
angina at rest with ST elevation
**can progress to MI if symptoms don’t resolve**
prinzmetals angina
what is this caused by? when do you get symptoms? who is it more common int? what does arteriography show? what are the two treatment options?
coronary ishchemia from vasospasms
symptoms at rest, usually in AM
women> men
ateriography shows normal looking arteries
Tx: nitrates and calcium channel blockers (dihyrdopyridines)
what percent of people with unstable angina remain unstable and need revascularization?
what percent improve medically? and what do you need to do before allowing them to leave?
20% will remain unstable and need revascularization
80% will get better clinicallly and need to get stress test once stable, if they produce a positive test then it might be an indication for revascularization
unstable angina
what is this? what are you at high risk for? how do you differentiate between this and a NSTEMI? what are the two presentations of this? what are two things you do to diagnose this? what are the two things you need to do for tx and the three drugs they need to be on?
angina at rest with minimal activity >10 minutes
GET VERY CLOSE TO HAVING A MI BUT DONT, RIGHT AT THE BRINK OF CELL NECROSIS BUT TISSUE HASN’T DIED YET, high risk for developing MI in following days/weeks so much treat aggressively and quickly
VERY SIMULAR TO NSTEMI, except in unstable angina negative cardiac markers
new onset: angina
accerating or cresendo angina in pt with previously stable angina (gets worse doing less activity)
DX:
NEGATIVE CARDIAC ENZYMES
EKG: ST depression, T wave inversion
Tx:
- HOSPITALIZE THEM!! BEDREST!!
- full anticoagulation and antiplatelet therapy
-HEPARIN +ASA+
prasurgrel/ticagrelor/clopidigrel OR glycoprotein IIb/IIIa
3. nitrates, Beta blockers, and Ca-blockers to decrease MVO2
what percent of people with unstable angina will have abnormal EKG?
50%
so worry about the 50% that have a normal one, still might need to work them up
since the pathology of unstable angina and NSTEMI are the same….what is the only thing that you use to tell them apart?
cardiac enzymes
ck-creatine kinase
MB
troponins
these indicate cell death and that the scale has tipped over the point of unstable angina and cell death is occuring, this is a myocardial infarction
non-stemi acute myocardial infarction
what is this caused by? what is this nickname for these? relate to morality? why must we treat aggressively? how do you differentiate between that and unstable angina?
infarcts caused by prolonged ischemia
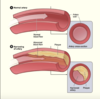
CAD to plaque rupture to platelets to clotting to thrombus
small infarcts that are unstable and could go on to cause a bigger infarct so that is why we treat aggressively
“incomplete infarcts” with lower initial mortality but high risk of re-infarction with HIGH MORTALITY
DX: like unstable angine with POSITIVE CARDIAC ENZYMES
acute myocardial infarction
STEMI
what is the cause of this? what does it lead to? what does patient complain of? what does this most likely occur? how does the patient appeare (3)? what often accompanies this? what are 6 signts of this? what are the 5 things you use to diagnose this?
prolonged ischemia resulting from inadequate tissue profusion leading to cell death and necrosis
total occulsion CAD to plaque to rupture to platelets to clotting, to occlusive thrombus
“elephant sitting on my chest and the worst pain I have felt in my life”
often early in the AM since coronary tone, SEVERE PAIN, anxious, diaphoretic, and distress, LV dysfunction
variable pulse and BP, S4 gallop, apical mitral regurgitation, cold, cyanotic, low CO, ST elevation
DX:
- Creatinine kinase (CK) ALWAYS ELEVATED!
check CK-MB, specific to damanged heart muscle
2. troponins cTnl represents muscle breakdown, sensitive to small infarcts
3. leukocytosis
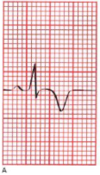
4. EKG ELEVATED ST
5. echo left ventricular function, identify mitral regurge
what are the treatments for a acute STEMI? (3)
1
1
2
1. percutaneous coronary intervention to reprofuse tissue (CATH)
- goal: open artery within 3 hours of onset of symptoms
goal: open atery within 90 mins presenting to hospital
***If within hour and a half of hospital that does this, consider transfer!!! Must also have CABG CAPABILITY****
2. thrombolytic (finbrinolytic) therapy: done if no access to cath lab, t-PA (altepase)
-done when ST elevation >1 mm in tow or more adjacent leads
50% reduction in mortality if given withint 1-3 hrs of symptoms
3. post thrombolytic management
a. ASA ongoing
b. heparin 24 hours
acute myocardial infarction
STEMI
what is the cause of this? what does it lead to? what does patient complain of? what does this most likely occur? how does the patient appeare (3)? what often accompanies this? what are 6 signts of this? what are the 5 things you use to diagnose this?
prolonged ischemia resulting from inadequate tissue profusion leading to cell death and necrosis
total occulsion CAD to plaque to rupture to platelets to clotting, to occlusive thrombus
“elephant sitting on my chest and the worst pain I have felt in my life”
often early in the AM since coronary tone, SEVERE PAIN, anxious, diaphoretic, and distress, LV dysfunction
variable pulse and BP, S4 gallop, apical mitral regurgitation, cold, cyanotic, low CO, ST elevation
DX:
- Creatinine kinase (CK) ALWAYS ELEVATED!
check CK-MB, specific to damanged heart muscle
2. troponins cTnl represents muscle breakdown, sensitive to small infarcts
3. leukocytosis
4. EKG ELEVATED ST
5. echo left ventricular function, identify mitral regurge
what are the treatments for a acute STEMI? (3)
1
1
2
1. percutaneous coronary intervention to reprofuse tissue (CATH)
- goal: open artery within 3 hours of onset of symptoms
goal: open atery within 90 mins presenting to hospital
***If within hour and a half of hospital that does this, consider transfer!!! Must also have CABG CAPABILITY****
2. thrombolytic (finbrinolytic) therapy: done if no access to cath lab, t-PA (altepase)
-done when ST elevation >1 mm in tow or more adjacent leads
50% reduction in mortality if given withint 1-3 hrs of symptoms
3. post thrombolytic management
a. ASA ongoing
b. heparin 24 hours
what are 3 drugs taht might be used to try to help in a actue MI early on pre hospital or in the ED?
- morphine sulfaste
- aspirin in ED
- nitro IV